Updated 5 May 2022. View update notification.
This is the most up-to-date version of the Anaphylaxis Wallchart (v2).
Clinical features
Any acute onset of hypotension or bronchospasm or upper airway obstruction where anaphylaxis is considered possible, even if typical skin features are not present
OR
Any acute onset illness with typical skin features (urticarial rash or erythema/flushing, and/or angioedema)
PLUS
Involvement of respiratory, cardiovascular, or persistent severe gastrointestinal symptoms
1 Immediate action
- Call for assistance.
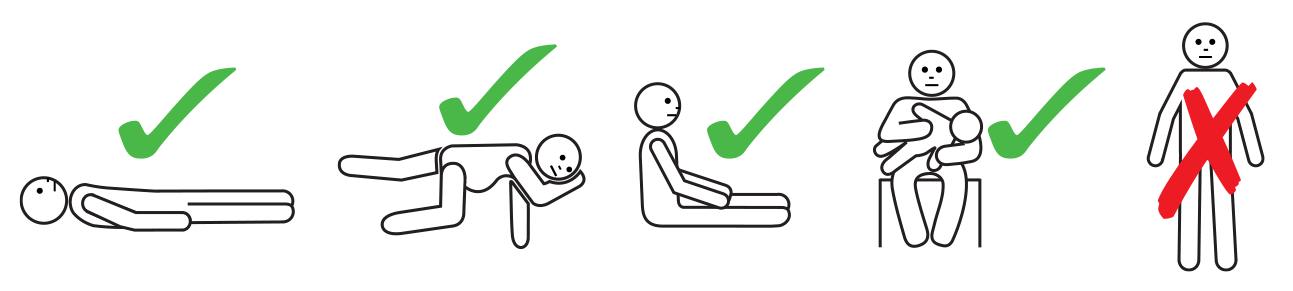
- Lay patient flat – do not allow them to stand or walk.
If breathing is difficult, allow the patient to sit with legs outstretched.
Hold young children flat, not upright.
2 Give INTRAMUSCULAR ADRENALINE (EPINEPHRINE) into mid-lateral thigh without delay
Adrenaline dose chart (1:1000 ampoules containing 1 mg adrenaline per 1 mL)
| Age (years) | Weight (kg) | Adrenaline volume 1:1000 |
|---|---|---|
| <1 | 5–10 | 0.05–0.1 mL |
| 1–2 | 10 | 0.1 mL |
| 2–3 | 15 | 0.15 mL |
| 4–6 | 20 | 0.2 mL |
| 7–10 | 30 | 0.3 mL |
| 10–12 | 40 | 0.4 mL |
| >12 and adult | >50 | 0.5 mL |
Repeat adrenaline every 5 minutes as needed.
If multiple doses are required, consider adrenaline infusion if skills and equipment available (see Step 5).
Autoinjector |
|---|
An adrenaline autoinjector, e.g. EpiPen or Anapen, may be used instead of an adrenaline ampoule and syringe.
Instructions are on device labels and ASCIA Action Plans. |
Remove allergen (if still present): flick out insect stings, freeze ticks with liquid nitrogen or ether-containing spray (if available) and allow to drop off.
ALWAYS give adrenaline FIRST, then asthma reliever puffer, if someone with known asthma and allergy to food, insects or medicine has SUDDEN BREATHING DIFFICULTY (including wheeze, persistent cough or hoarse voice) even if there are no skin symptoms.
3 Call ambulance to transport patient to hospital
4 Supportive management
When skills and equipment are available:
- monitor pulse, blood pressure, respiratory rate, pulse oximetry
- give oxygen and airway support if needed
- obtain intravenous access in adults and hypotensive children
- if hypotensive, give intravenous normal saline (20 mL/kg rapidly) and consider additional wide-bore intravenous access.
5 Additional measures
Adrenaline (epinephrine) infusion
If inadequate response or deterioration, start an intravenous adrenaline infusion as follows:
Give only in liaison with an appropriate specialist. Phone ………………………………………………
- Mix 1 mL of 1:1000 adrenaline in 1000 mL of normal saline
- Start infusion at 5 mL/kg/hour (0.1 microgram/kg/min)
- Titrate rate according to response
- Monitor continuously
If adrenaline (epinephrine) infusion is ineffective or unavailable, also consider:
For upper airway obstruction
- nebulised adrenaline (5 mL, i.e. 5 ampoules of 1:1000)
- intubation if skills and equipment are available
For persistent hypotension/shock
- give normal saline (maximum 50 mL/kg in the first 30 min)
- in patients with cardiogenic shock (especially if taking beta blockers) consider an intravenous glucagon bolus of 1–2 mg in adults (in children: 20–30 micrograms/kg up to 1 mg). This may be repeated or followed by an infusion of 1–2 mg/hour in adults
- in adults, selective vasoconstrictors metaraminol (2–10 mg) or argipressin (vasopressin) (10–40 units) only after advice from an appropriate specialist
For persistent wheeze
- bronchodilators: salbutamol 8–12 puffs of 100 micrograms using a spacer or 5 mg salbutamol by nebuliser
- oral prednisolone 1 mg/kg (maximum 50 mg) or intravenous hydrocortisone 5 mg/kg (maximum 200 mg)
6 Observation
Prolonged and biphasic reactions may occur.
Observe the patient for at least 4 hours after last dose of adrenaline.
Observe longer (overnight) if the patient:
- had a severe reaction (hypotension or hypoxia), or
- required repeated doses of adrenaline, or
- has a history of asthma or protracted anaphylaxis, or
- has other concomitant illness, or
- lives alone or is remote from medical care, or
- has known systemic mastocytosis.
Document food, medicine, sting/bite exposure in the 2–4 hours before anaphylaxis.
7 Follow-up treatment
Corticosteroids
The role of corticosteroids is unknown. It is reasonable to prescribe a 2-day course of oral steroid (e.g. prednisolone 1 mg/kg, maximum 50 mg daily) to reduce the risk of symptom recurrence after a severe reaction or a reaction with marked or persistent wheeze. Corticosteroids should only be administered after adrenaline and resuscitation.
Adrenaline (epinephrine) autoinjector
Prescribe an autoinjector, pending specialist review. Train the patient in autoinjector use and give them an ASCIA Action Plan for Anaphylaxis.
Allergy specialist
Refer patients with anaphylaxis for review.
Antihistamines
Antihistamines have no role in treating respiratory or cardiovascular symptoms of anaphylaxis. Oral non-sedating antihistamines treat itch and urticaria. Injectable promethazine should NOT be used in anaphylactic shock as it can worsen hypotension.
Endorsed by the Australasian College for Emergency Medicine, the Australasian Society of Clinical and Experimental Pharmacologists and Toxicologists, the Australasian Society of Clinical Immunology and Allergy (ASCIA), the Australian College of Rural and Remote Medicine, the Australian Dental Association, the Internal Medicine Society of Australia and New Zealand, the Royal Australasian College of Physicians, and the Royal Australian and New Zealand College of Radiologists.
This Anaphylaxis Wallchart has been officially recognised as an Accepted Clinical Resource by the Royal Australian College of General Practitioners.
Australian Prescriber welcomes Feedback




