Introduction
The inhibition of prostaglandin synthesis by aspirin and other non-steroidal anti-inflammatory drugs (NSAIDs) was first described over 20 years ago.1 The NSAIDs are now one of the most commonly used medications worldwide, with annual sales in the order of US$13 billion. These drugs are frequently used for the management of musculoskeletal diseases and for other causes of acute and chronic pain. Despite their clear efficacy in the management of inflammation, NSAIDs are a significant cause of adverse events, particularly gastrointestinal ulceration2 and altered renal function.
The enzyme responsible for prostaglandin synthesis is cyclo-oxygenase (COX). Following the observation that dexamethasone inhibits the increase in COX activity induced in macrophages, but has no effect on basal production of prostaglandins, it was proposed that there were two enzymes, COX-1 and COX-2.3 The COX-1 enzyme seems to have primarily a 'housekeeping' role, subserving normal physiological function in the gut and kidney and being involved with platelet activation. The COX-2 enzyme is induced during inflammation and tissue repair and also has significant physiological roles to play in reproduction and in renal function (Fig. 1). The molecular function and protein structures of the COX isoforms were rapidly identified. This led to the development of a number of selective COX-2 inhibitors. These drugs should provide the same efficacy as the non-selective NSAIDs with fewer gastrointestinal adverse reactions.
There is a huge potential market for these drugs. In the first few months following its launch in the USA sales of one COX-2 inhibitor exceeded those of sildenafil.
|
Fig. 1
Cyclo-oxygenase enzymes.
COX-1 is involved in normal physiological functions including the production of protective prostaglandins in the stomach. COX-2 is induced by inflammation.
Both enzymes are inhibited by non-steroidal anti-inflammatory drugs (NSAIDs). COX-2 inhibitors have little effect on COX-1 activity and so do not inhibit prostaglandin synthesis. 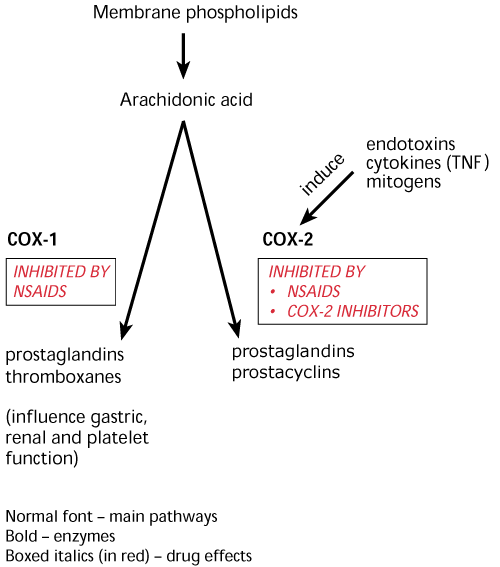
|
|
Fig. 2
Selectivity of COX-2 inhibitors and non-steroidal anti-inflammatory drugs5 given as log inhibitory concentration (IC80) ratio. The '0' line indicates equipotency.
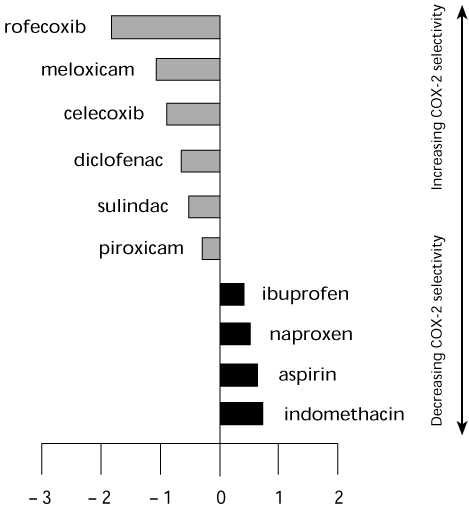 Log [IC80 ratio (William Harvey Human Modified Whole Blood Assay (WHMA) COX-2/COX-1)]
|
Assessment of COX-2 selectivity
There is a wide variety of assays to assess COX-1 and COX-2 selectivity.4 This has led to confusion in the reporting of the relative effects of some of the new selective inhibitors depending on which assay system is used. The Human Whole Blood Assay is probably the best available currently to assess inhibition of COX-1 and COX-2.
This assay has recently been modified slightly as the William Harvey Human Modified Whole Blood Assay (WHMA). A wide range of COX-2/COX-1 ratios has been reported for currently available and experimental NSAIDs.5 These data are summarised in Fig. 2 with rofecoxib being greater than 50-fold COX-2 selective, and celecoxib being 5-to-50 fold COX-2 selective. Diclofenac, sulindac and piroxicam have less than 5-fold COX-2 selectivity.
Measuring COX inhibition in gastric mucosa by using gastric biopsies may also provide important additional information. Although these investigations may define COX selectivity, they do not necessarily imply that COX-2 selective drugs will have improved safety profiles - this can only be shown by randomised controlled clinical trials.
Clinical studies
When comparing the adverse effects of COX-2 inhibitors with those of NSAIDs appropriate doses must be used. It is essential to compare doses which have similar efficacy.
Although the new COX-2 inhibitors had significantly lower incidences of gastric injury in the short term, 12-month anti-inflammatory and gastrointestinal outcome studies against standard NSAIDs are required to fully assess their efficacy and adverse effects.
Celecoxib
In single dose studies celecoxib (100 mg and 400 mg) was superior to placebo and as effective as aspirin (650 mg) in relieving the pain of dental extraction. Phase II and III studies of up to six months in doses of 100-400 mg/day for osteoarthritis and 200-800 mg/day for rheumatoid arthritis showed equivalence to naproxen 1 g daily or diclofenac 150 mg daily in terms of efficacy. In normal volunteers, endoscopic studies with celecoxib 100 mg or 200 mg twice daily for seven days revealed levels of gastric mucosal injury similar to those of placebo. Larger three6 or six-month studies showed the incidence of ulcers was similar to placebo and significantly reduced compared to naproxen and diclofenac.
Rofecoxib
Rofecoxib has a long half-life and is suitable for once-daily dosing in osteoarthritis and rheumatoid arthritis. A single dose of 50 mg is superior to placebo and equivalent to ibuprofen 400 mg or naproxen 550 mg for relieving acute pain after dental extraction. Gastric mucosal injury at seven days is similar to placebo, but less than ibuprofen 2.4 g daily or aspirin 2.6 g daily. A recent analysis of eight double-blind randomised controlled trials, including two one-year efficacy studies versus diclofenac 150 mg daily, in over 5000 osteoarthritis patients has reported a significantly lower 12-month cumulative incidence of perforations, ulcers and upper gastrointestinal tract bleeding with rofecoxib than with other NSAIDs (1.3% versus 1.8%).7
Future directions
Significant interest has now been shown in the role that inflammation (driven by COX-2) plays in conditions such as Alzheimer's disease and colonic carcinoma.8 COX-2 is certainly induced around the inflammatory plaques seen widely throughout the central nervous system in Alzheimer's disease, and COX-2 expression is upregulated dramatically in colonic carcinoma. Epidemiological data support the argument that patients taking NSAIDs have a lower incidence and a slower rate of progression of Alzheimer's disease. NSAIDs also reduce the growth rate of colonic polyps in humans9 and the incidence of colonic tumours in animals.
The selective COX-2 inhibitors seem to have similar effects, increasing blood pressure and reducing renal function, as the non-selective COX inhibitors. Selective COX-2 inhibitors should not be given to people with aspirin sensitivity as there are no published studies to show that this is safe for these patients. Although there is some theoretical concern relating to the potential for an increased risk of thrombosis with COX-2 inhibitors this does not seem to have been borne out by studies to date. Larger and longer-term studies are however required to answer these and other issues such as whether or not ulcer healing might be impaired by a selective COX-2 inhibitor. Since these drugs have the potential for widespread use in the community it is important that cost-effectiveness studies are carried out, although it would seem that the selective COX-2 inhibitors may be cost-effective for those patients at high risk of ulcer complications.10
Conclusion
The efficacy of the new drugs is not greater than that of the NSAIDs. However, if the current large outcome studies of celecoxib and rofecoxib confirm the reduced gastrointestinal toxicity then these drugs will increase the options for the treatment of arthritis.