What is in this leaflet
This leaflet answers some common questions about this medicine. It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you taking this medicine against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What this medicine is used for
Olmesartan is used to treat high blood pressure which is sometimes called hypertension.
Everyone has blood pressure. This pressure helps push blood all around your body. Your blood pressure changes at different times of the day, depending on how busy or worried you are. You have hypertension (high blood pressure) when your blood pressure stays higher than is needed, even when you are calm and relaxed.
There are usually no symptoms of hypertension. The only way of knowing that you have hypertension is to have your blood pressure checked on a regular basis. If high blood pressure is not treated it can lead to serious health problems, including stroke, heart disease and kidney failure.
Olmesartan belongs to a group of medicines known as angiotensin-II receptor antagonists. Angiotensin-II is a substance produced in the body which causes blood vessels to tighten. Olmesartan blocks the action of angiotensin-II and therefore relaxes your blood vessels. This helps lower your blood pressure.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another reason.
This medicine is not addictive.
This medicine is available only with a doctor's prescription.
The safety and effectiveness of this medicine in children aged less than 1 year has not been established.
Before you take this medicine
When you must not take it
Do not take this medicine if you have an allergy to:
- any medicine containing olmesartan
- any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin
Do not take this medicine if you are pregnant. It may affect your developing baby if you take it during pregnancy.
Do not breastfeed if you are taking this medicine. Olmesartan may pass into breast milk and there is a possibility that your baby may be affected.
Do not take this medicine if you have of the following medical conditions:
- serious problems with your kidneys
- serious problems with your liver
- you have diabetes and are taking a medicine called aliskiren to reduce blood pressure
Do not take this medicine after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking this medicine, talk to your doctor.
Before you start to take it
Tell your doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any of the following medical conditions:
- kidney problems
- liver problems
- heart problems
- excessive vomiting or diarrhoea recently
- high levels of potassium in your blood
- problems with your adrenal glands (small glands above the kidneys)
Tell your doctor if you are pregnant or plan to become pregnant or are breastfeeding. Your doctor can discuss with you the risks and benefits involved.
Tell your doctor if you are following a very low salt diet.
If you have not told your doctor about any of the above, tell them before you start taking this medicine.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and olmesartan may interfere with each other. These include:
- other medicines used to treat high blood pressure
- other diuretics, also known as fluid or water tablets
- non-steroidal anti-inflammatory drugs (NSAIDs) or COX-2 inhibitors, medicines used to relieve pain, swelling and other symptoms of inflammation, including arthritis
- potassium supplements, potassium-sparing agents or potassium-containing salt substitutes
- other medicines that may increase serum potassium (e.g. trimethoprim containing products)
- lithium, a medicine used to treat mood swings and some types of depression.
- any medicines that contain aliskiren
- any medicines that contain colesevelam
These medicines may be affected by olmesartan or may affect how well it works. You may need different amounts of your medicine, or you may need to take different medicines.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while taking this medicine.
How to take this medicine
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
If you do not understand the directions, ask your doctor or pharmacist for help.
How much to take
Adults:
The usual starting dose of olmesartan is 20 mg once daily.
The dose may need to be increased to 40 mg once a day if necessary.
For children 6-18 years (weighing 35 kg or more):
The usual dose is 20 mg once daily.
For children 6-18 years (weighing less than 35 kg):
The usual dose is 10 mg once daily.
APO-Olmesartan tablets cannot be divided to accommodate 10 mg dosing. Olmesartan 10 mg tablets are available from alternative brands when the 10 mg strength is required.
For children 1-5 years (weighing 5 kg or more)
The dose will vary depending on your child's weight.
How to take it
Swallow the tablets whole with a full glass of water.
Do not chew the tablets.
When to take it
Take your medicine at about the same time each day. Taking it at the same time each day will have the best effect. It will also help you remember when to take it.
It does not matter if you take this medicine before or after food.
How long to take it for
Continue taking your medicine for as long as your doctor tells you.
This medicine helps to control your condition but does not cure it. It is important to keep taking your medicine even if you feel well.
If you forget to take it
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Otherwise, take it as soon as you remember and then go back to taking your medicine as you would normally.
Do not take a double dose to make up for the dose that you missed. This may increase the chance of you getting an unwanted side effect.
If you are not sure what to do, ask your doctor or pharmacist.
If you have trouble remembering to take your medicine, ask your pharmacist for some hints.
If you take too much (overdose)
Immediately telephone your doctor or the Poisons Information Centre (telephone 13 11 26) for advice or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have taken too much of this medicine. Do this even if there are no signs of discomfort or poisoning.
You may need urgent medical attention.
If you take too much olmesartan, you may feel light-headed, dizzy or you may faint. You may also have a fast heartbeat.
While you are taking this medicine
Things you must do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking this medicine.
Tell any other doctors, dentists, and pharmacists who treat you that you are taking this medicine.
If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine. It may affect other medicines used during surgery.
If you become pregnant or start to breastfeed while taking this medicine, tell your doctor immediately.
If you are about to have any blood tests, tell your doctor that you are taking this medicine. It may interfere with the results of some tests.
Keep all your doctor's appointments so that your progress can be checked. Your doctor may occasionally do a blood test to check your potassium levels and see how your kidneys are working, and to prevent unwanted side effects.
Have your blood pressure checked when your doctor says, to make sure this medicine is working.
Make sure you drink enough water during exercise and hot weather when you are taking this medicine, especially if you sweat a lot. If you do not drink enough water while taking olmesartan, you may feel faint, light-headed or sick. This is because your blood pressure is dropping suddenly. If you continue to feel unwell, tell your doctor.
If you have excess vomiting and/or diarrhoea while taking this medicine, tell your doctor. You may lose too much water and salt and your blood pressure may drop too much.
If you feel light-headed or dizzy after taking your first dose of this medicine, or when your dose is increased, tell your doctor immediately.
Things you must not do
Do not take this medicine to treat any other complaints unless your doctor tells you to.
Do not give your medicine to anyone else, even if they have the same condition as you.
Do not stop taking your medicine or lower the dosage without checking with your doctor.
Things to be careful of
If you feel light-headed, dizzy or faint when getting out of bed or standing up, get up slowly. Standing up slowly, especially when you get up from bed or chairs, will help your body get used to the change in position and blood pressure. If this problem continues or gets worse, talk to your doctor.
Be careful driving or operating machinery until you know how this medicine affects you. As with other medicines in this class, olmesartan may cause dizziness, light-headedness or tiredness in some people. Make sure you know how you react to olmesartan before you drive a car, operate machinery, or do anything else that could be dangerous if you are dizzy or light-headed. If this occurs do not drive. If you drink alcohol, dizziness or light-headedness may be worse.
Things that would be helpful for your blood pressure
Some self-help measures suggested below may help your condition. Talk to your doctor or pharmacist about these measures and for more information.
- Alcohol - your doctor may advise you to limit your alcohol intake.
- Weight - your doctor may suggest losing some weight to help lower your blood pressure and help lessen the amount of work your heart has to do. Some people may need a dietician's help to lose weight.
- Diet - eat a healthy diet which includes plenty of fresh vegetables, fruit, bread, cereals and fish.
Also eat less fat and sugar (especially saturated fat) which includes sausages, fatty meats, full cream dairy products, biscuits, cakes, pastries, chocolates, chips and coconut. Monounsaturated and polyunsaturated fats from olive oil, canola oil, avocado and nuts are beneficial in small quantities. - Salt - your doctor may advise you to watch the amount of salt in your diet. To reduce your salt intake you should avoid using salt in cooking or at the table and avoid cooked or processed foods containing high sodium (salt) levels.
- Exercise - regular exercise, maintained over the long term, helps to reduce blood pressure and helps get the heart fitter. Regular exercise also improves your blood cholesterol levels, helps reduce your weight and stress levels, and improves your sleep, mood and ability to concentrate. However, it is important not to overdo it. Walking is good exercise, but try to find a route that is reasonably flat. Before starting any exercise, ask your doctor about the best kind of programme for you.
- Smoking - your doctor may advise you to stop smoking or at least cut down. There are enormous benefits to be gained from giving up smoking. There are many professionals, organisations and strategies to help you quit. Ask your doctor or pharmacist for further information and advice.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking this medicine.
Olmesartan helps most people with high blood pressure, but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects.
If you are over 65 years of age you may have an increased chance of getting side effects.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor or pharmacist if you notice any of the following and they worry you:
- feeling light-headed, dizzy or faint
- cough
- headache
- flushing
- feeling sick (nausea) or vomiting
- stomach pain
- diarrhoea
- an uncomfortable feeling in the stomach
- unusual tiredness or weakness, fatigue
- 'flu-like' symptoms
- runny or blocked nose, or sneezing
- bronchitis
- sore throat and discomfort when swallowing (pharyngitis)
- swelling of the hands, feet or ankles
- back pain
- urinary tract infection.
These are common side effects. They are generally mild.
Tell your doctor as soon as possible if you notice any of the following.
- skin rash or itchiness
- aching, tender or weak muscles not caused by exercise
- painful joints
- fast heart beat
- shortness of breath or tightness in the chest
- swelling of the hands, feet or ankles
- symptoms that may indicate high potassium levels in the blood, such as nausea, diarrhoea, muscle weakness, change in heart rhythm
These may be serious side effects. You may need medical attention.
If any of the following happen, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- chest pain
- symptoms of an allergic reaction including cough, shortness of breath, wheezing or difficulty breathing; swelling of the face, lips, tongue, throat or other parts of the body; rash, itching or hives on the skin
The above list includes very serious side effects. You may need urgent medical attention or hospitalisation.
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Other side effects not listed above may also occur in some people.
Some of these side effects, for example changes to levels in the blood or blood cell count, can only be found when your doctor does tests from time to time to check your progress.
Storage and disposal
Storage
Keep your tablets in their original packaging until it is time to take them. If you take the tablets out of the pack, they will not keep well.
Keep your tablets in a cool dry place where the temperature stays below 25°C.
Do not store this medicine or any other medicine in the bathroom or near a sink. Do not leave it on a window sill or in the car.
Heat and dampness can destroy some medicines.
can destroy some medicines.
Keep this medicine where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop taking this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Product description
What it looks like
20 mg tablets:
Yellow film coated, round, biconvex tablets debossed with '323' on one side and 'L' on other side. AUST R 221052.
40 mg tablets:
Yellow film coated, oval shape, biconvex tablets debossed with 'L324' on one side and plain on other side. AUST R 221063.
Available in blister packs of 30 tablets.
Ingredients
This medicine contains 20 or 40 mg of olmesartan as the active ingredient.
This medicine also contains the following:
- lactose monohydrate
- microcrystalline cellulose
- low-substituted hydroxypropylcellulose
- hydroxypropylcellulose
- magnesium stearate
- Opadry Yellow 03F82788
This medicine contains sugars as lactose.
This medicine does not contain sucrose, tartrazine or any other azo dyes.
Sponsor
Apotex Pty Ltd
16 Giffnock Avenue
Macquarie Park NSW 2113
Tel: (02) 8877 8333
Web: www1.apotex.com/au
APO and APOTEX are registered trademarks of Apotex Inc.
This leaflet was last updated in November 2022.
Published by MIMS March 2024



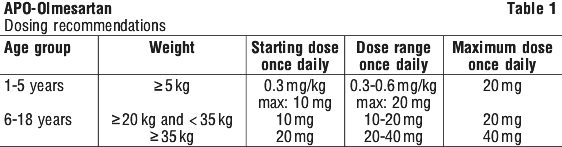 For children who cannot swallow tablets, the equivalent dose may be given as an extemporaneous suspension. This brand of product has not been approved for use as an extemporaneous suspension. An alternative brand approved for use to compound an extemporaneous suspension is to be used if treatment is required in the suspension form.
For children who cannot swallow tablets, the equivalent dose may be given as an extemporaneous suspension. This brand of product has not been approved for use as an extemporaneous suspension. An alternative brand approved for use to compound an extemporaneous suspension is to be used if treatment is required in the suspension form.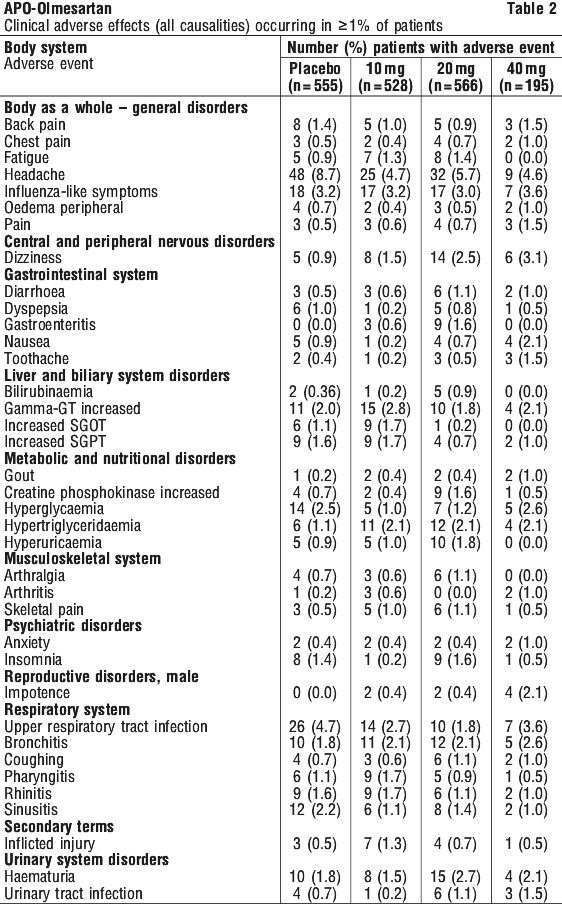 Other adverse events of potential clinical relevance reported in the clinical trials are listed below. Adverse events reported across all clinical trials with olmesartan medoxomil (including trials with active as well as placebo control), irrespective of causality or incidence relative to placebo, included those events listed below.
Other adverse events of potential clinical relevance reported in the clinical trials are listed below. Adverse events reported across all clinical trials with olmesartan medoxomil (including trials with active as well as placebo control), irrespective of causality or incidence relative to placebo, included those events listed below.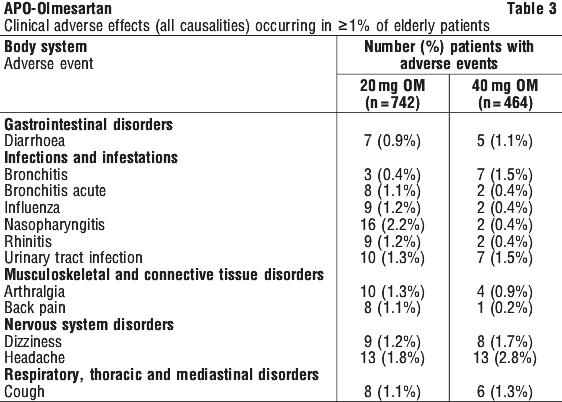 The most common adverse events considered to be treatment related in elderly patients were headache (1.5%) and dizziness (1.1%) on 40 mg olmesartan medoxomil.
The most common adverse events considered to be treatment related in elderly patients were headache (1.5%) and dizziness (1.1%) on 40 mg olmesartan medoxomil.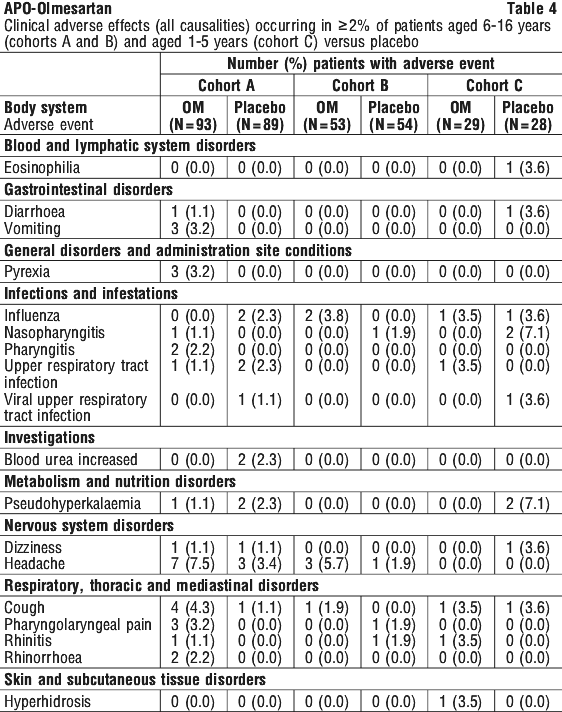
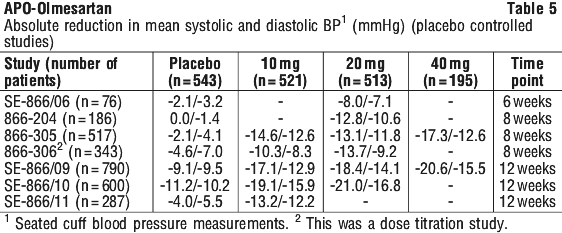 Data above from seven placebo-controlled studies also confirm that the blood pressure lowering effect was maintained throughout the 24-hour period with olmesartan medoxomil once daily, with trough-to-peak ratios for systolic and diastolic response between 60 and 80%.
Data above from seven placebo-controlled studies also confirm that the blood pressure lowering effect was maintained throughout the 24-hour period with olmesartan medoxomil once daily, with trough-to-peak ratios for systolic and diastolic response between 60 and 80%. The blood pressure lowering effect of olmesartan medoxomil, with and without hydrochlorothiazide, was maintained in patients treated for up to 1-year. There was no evidence of tachyphylaxis during long-term treatment with olmesartan medoxomil or rebound effect following abrupt withdrawal of olmesartan medoxomil after 1-year of treatment.
The blood pressure lowering effect of olmesartan medoxomil, with and without hydrochlorothiazide, was maintained in patients treated for up to 1-year. There was no evidence of tachyphylaxis during long-term treatment with olmesartan medoxomil or rebound effect following abrupt withdrawal of olmesartan medoxomil after 1-year of treatment.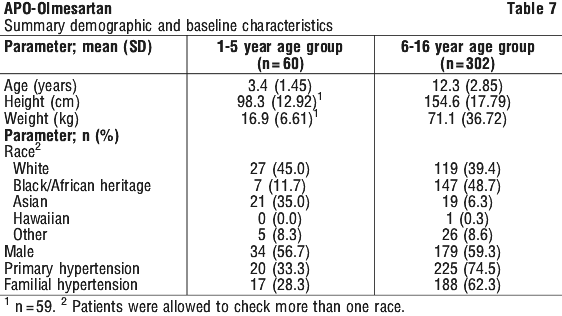 The study included three periods: a 3 week double-blind, randomised, dose-response period for patients aged 6-16 years or, for patients aged 1-5 years, an open-label dose period; up to 2 week double-blind, randomised, placebo-controlled withdrawal period; and a 46 week open-label safety and efficacy period. The primary endpoints were the dose response in systolic blood pressure or in diastolic blood pressure for subjects 6 to 16 years of age at the end of this period. This study was not a clinical outcome study.
The study included three periods: a 3 week double-blind, randomised, dose-response period for patients aged 6-16 years or, for patients aged 1-5 years, an open-label dose period; up to 2 week double-blind, randomised, placebo-controlled withdrawal period; and a 46 week open-label safety and efficacy period. The primary endpoints were the dose response in systolic blood pressure or in diastolic blood pressure for subjects 6 to 16 years of age at the end of this period. This study was not a clinical outcome study.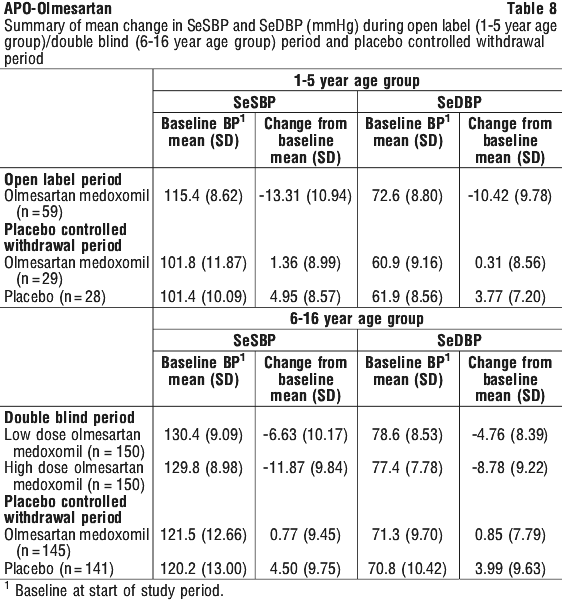 At the end of the open-label efficacy and safety period, compared to baseline, the mean systolic and diastolic blood pressure were reduced at all visits for all patient age groups. However data in children 1-5 years are limited due to small numbers of patients enrolled in the clinical studies. Overall the clinical trials were unable to demonstrate that olmesartan medoxomil was significantly better than placebo in reducing blood pressure in children 1-5 years of age.
At the end of the open-label efficacy and safety period, compared to baseline, the mean systolic and diastolic blood pressure were reduced at all visits for all patient age groups. However data in children 1-5 years are limited due to small numbers of patients enrolled in the clinical studies. Overall the clinical trials were unable to demonstrate that olmesartan medoxomil was significantly better than placebo in reducing blood pressure in children 1-5 years of age.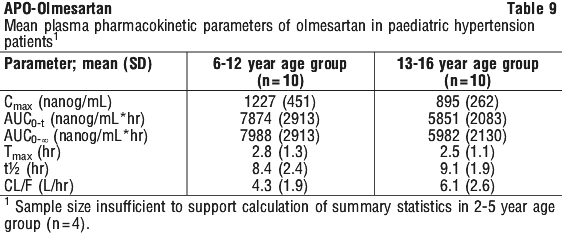
 Olmesartan medoxomil is described chemically as 2,3-dihydroxy-2-butenyl 4-(1-hydroxy-1-methylethyl)-2-propyl-1-[p-(o-1H-tetrazol-5-ylphenyl)benzyl] imidazole-5-carboxylate, cyclic 2,3-carbonate.
Olmesartan medoxomil is described chemically as 2,3-dihydroxy-2-butenyl 4-(1-hydroxy-1-methylethyl)-2-propyl-1-[p-(o-1H-tetrazol-5-ylphenyl)benzyl] imidazole-5-carboxylate, cyclic 2,3-carbonate.