What is in this leaflet
Read this leaflet carefully before you start to use Ciloxan Eye Drops.
This leaflet answers some common questions about Ciloxan Eye Drops. It does not contain all of the available information. It does not take the place of talking to your doctor or pharmacist.
The information in this leaflet was last updated on the date listed on the final page. More recent information on the medicine may be available.
You should ensure that you speak to your pharmacist or doctor to obtain the most up to date information on the medicine.
You can also download the most up to date leaflet from www.novartis.com.au
The updates may contain important information about the medicine and its use of which you should be aware.
All medicines have risks and benefits. Your doctor has weighed the expected benefits of you using Ciloxan Eye Drops against the risks this medicine could have for you.
The information in this leaflet applies to Ciloxan only. This information does not apply to similar products, even if they contain the same ingredients.
If you have any concerns about using this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine.
You may need to read it again.
What Ciloxan is used for
Ciloxan Eye Drops are used to treat certain types of eye infections caused by bacteria. Your doctor will usually prescribe this medicine to treat a type of eye infection called bacterial conjunctivitis or an infected ulcer of the cornea.
Ciloxan Eye Drops contain the active ingredient ciprofloxacin hydrochloride. Ciprofloxacin hydrochloride is a "fluoroquinolone" antibiotic. This antibiotic works by killing the bacteria that are causing your infection.
Ciloxan Eye Drops are only available on a doctor's prescription.
Your doctor may have prescribed Ciloxan for another reason.
Ask your doctor if you have any questions about why Ciloxan has been prescribed for you.
Use in children
Do not use Ciloxan Eye Drops in children under 12 months of age. The safety and effectiveness of Ciloxan Eye Drops has not been established in children below the age of 12 months including neonates (the newborn).
Before you use Ciloxan
When you must not use it
Do not use Ciloxan Eye Drops if you have an allergy to:
- Ciprofloxacin
- Any other "quinolone" antibiotics e.g. nalidixic acid
- Any of the other ingredients in Ciloxan Eye Drops that are listed under "Product description".
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
Do not put the eye drops into your eye(s) while you are wearing soft contact lenses. The preservative in Ciloxan Eye Drops, benzalkonium chloride may be deposited in soft contact lenses. Ciloxan Eye Drops may cause irritation or discolour soft contact lenses.
Wearing contact lenses is not recommended while you are using Ciloxan Eye Drops as you are being treated for an eye infection.
Do not use this medicine after the expiry date printed on the pack or bottle or if the seal around the pack is broken or shows signs of tampering. If it is has expired or is damaged, return it to your pharmacist for disposal.
If you use this medicine after the expiry date has passed, it may not work.
If this medicine has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start using Ciloxan Eye Drops, talk to your doctor.
Before you start to use it
Tell your doctor if you have had an allergy to any other medicines or any other substances, such as foods, preservatives or dyes.
Tell your doctor if you are pregnant or plan to become pregnant. Your doctor will discuss the possible risks and benefits of using Ciloxan during pregnancy.
Tell your doctor if you are breastfeeding. Your doctor will discuss the possible risks and benefits of using Ciloxan when you are breastfeeding.
If you have not told your doctor about any of the above, tell him/ her before you use Ciloxan Eye Drops.
Taking or using other medicines
Tell your doctor or pharmacist if you are taking or using any other medicines, including other eye drops or ointments, and any other medicines that you buy without a prescription from a pharmacy, supermarket or health food shop. Some medicines and ciprofloxacin may interfere with each other.
Tell your doctor if you are taking any of the following:
- medicines to thin your blood e.g. warfarin
- medicines to prevent tissue rejection e.g. cyclosporin
- theophylline for asthma or breathing problems
- caffeine for the treatment of migraines.
Your doctor and pharmacist will have more information on medicines to be careful with or avoid while using this medicine.
How to use Ciloxan
Carefully follow all directions given to you by your doctor and pharmacist. They may differ from the information contained in this leaflet.
If you are being changed from one medicine to another, follow your doctor's instructions carefully as to when to stop the medicine and when to start the new eye drops.
If you do not understand the instructions on the carton / bottle, ask your doctor or pharmacist for help.
How much to use
The usual dose to treat corneal ulcers is:
Day 1
- 2 drops in the affected eye(s) every 15 minutes for the first 6 hours.
- 2 drops in the affected eye(s) every 30 minutes for the remainder of the first day.
Day 2
- 2 drops in the affected eye(s) every 60 minutes.
Days 3 to 14
- 2 drops in the affected eye(s) every 4 hours.
Your doctor may continue your treatment with Ciloxan Eye Drops until the surface of your eye (cornea) is completely healed.
The usual dose to treat bacterial conjunctivitis is:
Days 1 and 2
- One drop in the affected eye(s) every 2 hours while you are awake.
Days 3 to 7
- 1 drop in the affected eye(s) every 4 hours while you are awake.
Your doctor will tell you how many drops you need to use each day.
These dosing instructions will be printed on the label by your pharmacist.
How to use it
It is important to use Ciloxan exactly as your doctor or pharmacist has told you. If you use the drops less often than your doctor has advised your medicine may not work as well and your eye problem may not improve. If you use the drops more often than your doctor has advised your eye problem may not improve any faster and this may increase the incidence of side effects.
If you are wearing soft contact lenses, remove them before putting the drops in your eye.
Follow these steps to use the Eye Drops:
- Wash your hands thoroughly with soap and water.
- Immediately before using a bottle for the first time, break the safety seal around the neck area and throw the loose plastic ring away.
- Shake the bottle.
- Remove the cap from the bottle.
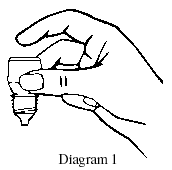
- Hold the bottle upside down in one hand between your thumb and middle finger (see Diagram 1).
- While tilting your head back, gently pull down the lower eyelid of your eye to form a pouch/pocket.
- Place the tip of the bottle close to your eye. Do not let it touch your eye.
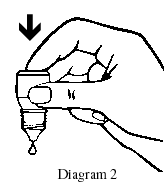
- Release one drop into the pouch/pocket formed between your eye and eyelid by gently tapping or pressing the base of the bottle with your forefinger (see Diagrams 2 and 3).

- Close your eye. Do not blink or rub your eye.
- While your eye is closed, place your index finger against the inside corner of your eye and press against your nose for about two minutes. This will help to stop the medicine from draining through the tear duct to the nose and throat, from where it can be absorbed into other parts of your body. This will also reduce the unpleasant taste sensation that some people experience when using these drops.
- If necessary, repeat the above steps for the other eye.
- Your eyelids can only hold less than one drop at a time, so it is normal for a small amount of the eye drop to spill onto your cheek. You should wipe away any spillage with a tissue.
- Replace the cap on the bottle, closing it tightly.
- Wash your hands again with soap and water to remove any residue.
You may feel a slight burning sensation in the eye shortly after using Ciloxan Eye Drops. If this persists, or is very uncomfortable, contact your doctor or pharmacist.
Be careful not to touch the dropper tip against your eye, eyelid or anything else. This will help to prevent your eye drops becoming dirty or contaminated.
After using Ciloxan Eye Drops wait at least 5 minutes before putting any other eye drops in your eye(s).
When to use it
Use Ciloxan Eye Drops every day, at about the same times each day unless your doctor tells you otherwise. Using your eye drops at the same times each day will help treat your eye infection.
It will also help you remember when to use the eye drops.
How long to use it
Continue using your medicine for as long as your doctor tells you.
As Ciloxan Eye Drops start to kill the bacteria that are causing the infection in your eye(s) you will start to feel better. However, it is very important that you continue to use Ciloxan Eye Drops for the full treatment period advised by your doctor to ensure that the infection does not return.
If you are unsure about when to stop using Ciloxan Eye Drops you should talk to your doctor or pharmacist.
If you forget to use it
If you forget to use Ciloxan Eye Drops you should put the drops that you missed in as soon as you remember and then go back to using them as recommended by your doctor.
If it is almost time for your next dose, skip the dose that you have missed and continue to use them as recommended.
Do not use double the amount to make up for the dose that you missed. Using multiple doses may cause unwanted side effects.
If you are not sure whether to skip the dose, talk to your doctor or pharmacist.
If you are having trouble remembering to use the medicine, ask your pharmacist for some hints.
If you use too much (overdose)
If you accidentally put too many drops in your eye(s), immediately rinse your eye(s) with warm water.
If you think that you or anyone else may have swallowed any or all of the contents of a bottle of Ciloxan, immediately telephone your doctor or the Poisons Information Centre on 13 11 26 for advice, or go to Accident and Emergency at your nearest hospital. Do this even if there are no signs of discomfort or poisoning.
While you are using Ciloxan
Things you must do
Tell your doctor if, for any reason, you have not used Ciloxan Eye Drops exactly as prescribed. Otherwise your doctor may think that the eye drops were not effective and change the treatment unnecessarily.
If you become pregnant while you are using this medicine, tell your doctor immediately.
Tell all the doctors, dentists and pharmacists who are treating you that you are using Ciloxan.
If you are about to be started on any new medicine, remind your doctor or pharmacist that you are using Ciloxan Eye Drops.
Things you must not do
Do not use Ciloxan Eye Drops to treat other complaints unless your doctor tells you to.
Do not give this medicine to anyone else, even if they appear to have the same condition as you.
Do not stop using Ciloxan Eye Drops or lower the dose without first asking your doctor.
Do not let children handle Ciloxan Eye Drops.
Things to be careful of
Be careful driving or operating machinery until you know how Ciloxan Eye Drops affect you and your vision. As with any eye medicines, temporary blurred vision or other visual disturbances may affect the ability to drive or use machinery in some people. If blurred vision occurs when you use your drops, wait until your vision is clear before driving or operating machinery.
Side Effects
Tell your doctor as soon as possible if you do not feel well while you are using Ciloxan Eye Drops.
This medicine helps most people with an eye infection but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects.
Do not be alarmed by the following list of possible side effects. You may not experience any of them.
Most side effects from Ciloxan Eye Drops occur in, or around, the eye.
These include:
- Redness, itching, irritation, pain, swelling or discomfort in or around the eye(s) and/or eyelids
- A white precipitate in the eye(s) or crusting on the eyelid(s)
- Excess tear production or discharge from the eye(s)
- Dry eye(s)
- Staining, swelling or irregular appearance of the front of the eye(s) (cornea)
- Flaking skin of the eyelids
- A numb sensation in or around the eye(s)
- Tired eyes
- Allergic reactions
- A feeling that something is in your eye(s)
- Decreased or blurred vision
- Double vision
- Sensitivity to light.
These are the most common side effects of your medicine. They are usually mild and short lived.
Occasionally some people notice unwanted effects in the rest of their body as a result of using Ciloxan Eye Drops.
These effects may include:
- Bad taste in the mouth following the use of Ciloxan Eye Drops
- Nausea
- Diarrhoea or abdominal pain
- Headache
- Dizziness
- Ear pain
- Increased drainage from the sinuses
- Skin inflammation.
If you are over 65 years of age and taking inflammatory inhibiting medicines similar to cortisone, you have a higher risk of getting tendon problems during treatment with Ciloxan Eye Drops. If this occurs, stop treatment and immediately consult your doctor.
If any of the following happen, stop using the Ciloxan Eye Drops and tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- skin rash
- swelling of face, hands or feet
- wheezing, difficulty in breathing
- shortness of breath
- severe and sudden onset of pinkish, itchy swellings on the skin, also called hives or nettlerash.
These hypersensitivity reactions can be very serious side effects. You may need urgent medical attention or hospitalisation. These side effects are very rare.
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Other side effects not listed above may also occur in some people.
After using Ciloxan
Store Ciloxan Eye Drops in a cool dry place, where the temperature stays below 25°C. Do not refrigerate or freeze. Protect from light.
Do not store Ciloxan Eye Drops or any other medicine in the car, the bathroom or any other warm, damp place. Heat and dampness can destroy some medicines.
Do not leave the top off the bottle for any length of time, to avoid contaminating the eye drops.
Keep it out of the sight and reach of children. A locked cupboard at least one-and-half metres above the ground is a good place to store medicines.
Disposal
Write the date on the bottle when you open the eye drops and throw out any remaining solution after four weeks. Eye drops contain a preservative which helps prevent germs growing in the solution for the first four weeks after opening the bottle. After this time there is a greater risk that the drops may become contaminated and cause an eye infection. A new bottle should then be used.
If your doctor tells you to stop using Ciloxan Eye Drops or they have passed their expiry date, ask your pharmacist what to do with the remaining solution.
Product description
What it looks like
Ciloxan Eye Drops are a sterile liquid supplied in a pack containing a 5mL dropper bottle with a screw cap.
Tamper evidence is provided with a safety seal around the neck area of the bottle.
Ingredients
The active ingredient in Ciloxan Eye Drops is ciprofloxacin (base) 3mg in 1 mL.
Ciloxan Eye Drops also contain:
- Benzalkonium chloride (0.06mg/mL) as a preservative)
- Sodium acetate
- Acetic acid
- Mannitol
- Disodium edetate
- Purified water
- Hydrochloric acid and/or sodium hydroxide to adjust pH.
Supplier
This product is supplied in Australia by:
Novartis Pharmaceuticals Australia Pty Limited
ABN 18 004 244 160
54 Waterloo Road
Macquarie Park NSW 2113
Telephone: 1800 671 203
Web Site: www.novartis.com.au
Australian registration number
AUST R No. 42899
Date of preparation
This leaflet was prepared in October 2023.
© Novartis Pharmaceuticals Australia Pty Limited 2022
® Registered trademark
Internal document code:
(cix_eye261023c) based on PI (cix_eye261023i)
Published by MIMS December 2023

 Uncommon ophthalmic events (occurring in less than 1% and greater than 0.1% of patients) included lid margin crusting, crystals/scales, dryness/dry eye, discharge, corneal staining, keratopathy/keratitis, tearing, photophobia, pain, vision decrease, chemosis, corneal infiltrates, inflammation, blurred vision, corneal toxicity, allergy, intolerance, lid oedema, heavy sensation, swelling, conjunctival reaction, numbing sensation, conjunctivitis, punctate epithelial erosion and progression of infiltrate.
Uncommon ophthalmic events (occurring in less than 1% and greater than 0.1% of patients) included lid margin crusting, crystals/scales, dryness/dry eye, discharge, corneal staining, keratopathy/keratitis, tearing, photophobia, pain, vision decrease, chemosis, corneal infiltrates, inflammation, blurred vision, corneal toxicity, allergy, intolerance, lid oedema, heavy sensation, swelling, conjunctival reaction, numbing sensation, conjunctivitis, punctate epithelial erosion and progression of infiltrate. Chemical name: the monohydrochloride monohydrate salt of 1-cyclopropyl-6-fluoro- 1,4-dihydro-4-oxo- 7-piperazin-1- ylquinoline- 3-carboxylic acid.
Chemical name: the monohydrochloride monohydrate salt of 1-cyclopropyl-6-fluoro- 1,4-dihydro-4-oxo- 7-piperazin-1- ylquinoline- 3-carboxylic acid.