1 Name of Medicine
Fosfomycin trometamol.
2 Qualitative and Quantitative Composition
One sachet of Cipla Fosfomycin granules for oral solution contains 5.631 g of fosfomycin trometamol equivalent to 3.0 g fosfomycin.
Fosfomycin trometamol is a white or almost white hygroscopic powder. It is very soluble in water, slightly soluble in methanol and ethanol (96%) and practically insoluble in acetone.
Excipient with known effect.
One sachet of Cipla Fosfomycin granules for oral solution contains 2.213 g of sugar (sucrose). For the full list of excipients, see Section 6.1 List of Excipients.3 Pharmaceutical Form
Cipla Fosfomycin contains 3 g fosfomycin (as fosfomycin trometamol), presented as white to off-white powder for oral solution in single use sachet.
4.1 Therapeutic Indications
Cipla Fosfomycin is indicated only for the treatment of acute uncomplicated lower urinary tract infections (acute cystitis) in females above 12 years of age caused by the following susceptible pathogens: Escherichia coli, or Enterococcus faecalis.
Cipla Fosfomycin is not indicated for the treatment of pyelonephritis or perinephric abscess or where resistance is likely (previous treatment failure, infection due to non-susceptible organism).
Appropriate culture and susceptibility studies should be performed to identify the causative organism(s) and determine its (their) susceptibility to Cipla Fosfomycin. However, therapy may be initiated before results of these tests are known; once results become available, appropriate therapy should be continued. Consideration should be given to the relevant clinical guidelines on the appropriate use of antibacterial agents.
4.2 Dose and Method of Administration
Dosage.
The recommended dose for the treatment of an acute uncomplicated lower urinary tract infection (UTI) is a single Cipla Fosfomycin sachet in women above 12 years of age.
Paediatric population.
The safety and efficacy of fosfomycin in children below 12 years has not been established. No data are available.
Renal impairment.
Use of fosfomycin is not recommended in patients with severe renal impairment (creatinine clearance < 10 mL/min, see Section 5.2 Pharmacokinetic Properties).
Method of administration.
Cipla Fosfomycin is for oral administration.
It should be taken on an empty stomach or about 2-3 hours after meals, preferably before bedtime and after emptying the bladder.
The dose should be dissolved into a glass of cold water (do not use hot water) and taken immediately after its preparation.4.3 Contraindications
Hypersensitivity to fosfomycin trometamol or to any of the excipients (see Section 6.1 List of Excipients).
4.4 Special Warnings and Precautions for Use
General.
Do not use more than one single dose of Cipla Fosfomycin to treat a single episode of acute uncomplicated lower UTI. Repeated daily doses of fosfomycin in an acute UTI did not improve the clinical success or microbiological eradication rates compared to single dose therapy but did increase the incidence of adverse events.
Gender.
The three pivotal trials MON-US-01, MON-US-02 and MON-US-03 were conducted in female patients only. However, there is extensive early clinical trial and post-marketing experience in males. There do not appear to be any gender-associated differences in the safety profile of fosfomycin.
Efficacy data in male patients with UTI is limited so Cipla Fosfomycin is not recommended in males.
Hypersensitivity.
Hypersensitivity reactions, including anaphylaxis and anaphylactic shock, may occur during fosfomycin treatment and may be life-threatening (see Section 4.8 Adverse Effects (Undesirable Effects)). If such reaction occurs, fosfomycin should never be re-administrated and an adequate medical treatment is required.
Antibiotic-associated diarrhoea.
Antibiotic-associated diarrhoea has been reported with use of nearly all antibacterial agents, including fosfomycin. Diarrhoea may range in severity from mild to fatal colitis but is usually self-limited in duration and resolves spontaneously (see Section 4.8 Adverse Effects (Undesirable Effects)). Diarrhoea, particularly if severe, persistent and/or bloody, during or after treatment with Cipla Fosfomycin (including several weeks after treatment), may be symptomatic of Clostridium difficile-associated disease (CDAD). It is therefore important to consider this diagnosis in patients who develop serious diarrhoea during or after treatment with Cipla Fosfomycin. If CDAD is suspected or confirmed, appropriate treatment should be initiated without delay.
Food.
Food may delay the absorption of the active ingredient of Cipla Fosfomycin, with consequent slight decrease in peak plasma levels and urinary concentrations. It is therefore preferable to take the medicine on an empty stomach or about 2-3 hours after meals.
Use in hepatic impairment.
See Section 5.2 Pharmacokinetic Properties, Special populations.
Use in renal impairment.
In consideration of the safety profile of the drug and of single dose treatment, in patients with mild to moderate renal impairment (defined as creatinine clearance > 10 mL/min) it is not necessary to adjust the dose but these patients have to be carefully monitored.
Due to reduced excretion of drug and limited data, fosfomycin trometamol is contraindicated in severe renal failure (creatinine clearance < 10 mL/min), haemodialysis, peritoneal dialysis and haemofiltration.
Also see Section 4.2 Dose and Method of Administration; Section 5.2 Pharmacokinetic Properties, Special populations.
Use in the elderly.
Fosfomycin may be given in the elderly. In elderly patients with good renal function, pharmacokinetics, efficacy and safety appear similar to younger adults. For elderly patients with age-related or other renal insufficiency, see Section 5.2 Pharmacokinetic Properties, Special populations.
Paediatric use.
Experience in children with fosfomycin is limited. The product is not recommended for children below the age of 12.
Effects on laboratory tests.
In post-marketing surveillance, three cases of increased INR (prothrombin time) and two cases of decreased INR (prothrombin time) were reported. No further clinical information is available regarding these patients. As fosfomycin does not bind to plasma proteins and does not undergo metabolism, an interaction with anticoagulant drugs of the coumarin type such as warfarin is not anticipated, although fosfomycin has not been studied in patients taking anticoagulants. Recommend monitoring of coagulation in patients receiving coumarins.
Sugar (sucrose) content.
Cipla Fosfomycin contains sucrose. Its use is not recommended in patients with hereditary problems of fructose intolerance, glucose-galactose malabsorption or sucrase-isomaltase insufficiency.4.5 Interactions with Other Medicines and Other Forms of Interactions
Concomitant administration of metoclopramide has been shown to lower serum and urinary concentrations of fosfomycin and should be avoided.
Other drugs that increase gastrointestinal motility may produce similar effects.
Cimetidine does not alter the pharmacokinetics of fosfomycin.
Interaction studies with metoclopramide and cimetidine have only been performed in healthy adult volunteers aged 20 years and over. No other drugs have been studied for potential interactions with fosfomycin. No drug interaction studies have been performed in humans aged less than 20 years.
Concomitant usage with urinary alkalinisers is not recommended. Fosfomycin is most bactericidal at typical urinary pH. Also, potential for resistance development appears less at acidic pH.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
Fosfomycin had no effect on fertility in male and female rats at doses up to 1000 mg/kg/day (3-times the clinical dose relative to body surface area). No data are available in humans.
(Category B2)
Fosfomycin was not found to be teratogenic in rats and rabbits when tested at doses of up to 1000 mg/kg/day and 500 mg/kg/day, respectively (3- and 3.8-times the clinical dose relative to body surface area, respectively). Fetoxicity was observed in rabbits at doses ≥ 1000 mg/kg/day, which was secondary to maternotoxicity (maternal deaths and body weight losses). No adverse findings were reported in peri-postnatal studies in rats treated at up to 1000 mg/kg/day (3-times the clinical dose relative to body surface area).
In early clinical trials and in the post-marketing period, at least 1552 pregnant human patients are known to have received fosfomycin during pregnancy, usually a 3 g single oral dose. Only limited data on the safety of fosfomycin treatment during the first trimester of pregnancy (n = 152) are available.
There is no evidence based on review of human data that fosfomycin is associated with adverse foetal or maternal outcomes or teratogenicity. At the present time, single-dose antibacterial treatments are not considered suitable to treat UTIs in pregnant women (also see Section 5.2 Pharmacokinetic Properties, Special populations).
Fosfomycin is excreted in breast milk.
Cipla Fosfomycin therapy should therefore not be used in breastfeeding mothers unless the potential benefit outweighs the potential risks.4.7 Effects on Ability to Drive and Use Machines
No specific studies have been performed but patients should be informed that dizziness has been reported. This may influence some patients' ability to drive and use machines.
4.8 Adverse Effects (Undesirable Effects)
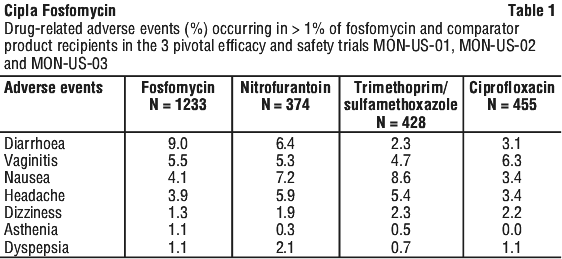
The majority of clinical trials have been conducted in adult or adolescent females aged 12 years or above. The most common adverse reactions following the single 3 g dose of fosfomycin trometamol involved the gastrointestinal tract, mainly diarrhoea. These events were usually self-limited in duration and resolve spontaneously. Table 1 lists drug-related adverse events which occurred in 1% or more of fosfomycin recipients in the three pivotal trials.
 The following list displays adverse drug reactions that have been reported with the use of fosfomycin from either clinical-trial or post-marketing experiences.
The following list displays adverse drug reactions that have been reported with the use of fosfomycin from either clinical-trial or post-marketing experiences.
The displayed frequency categories use the following convention:
Very common (≥ 1/10); common (≥ 1/100 to < 1/10); uncommon (≥ 1/1,000 to < 1/100); rare (≥ 1/10,000 to < 1/1,000); very rare (< 1/10,000), not known (cannot be estimated from the available data).
Infections and infestations.
Common: vulvovaginitis.
Immune system disorders.
Not known: anaphylactic reactions including anaphylactic shock, hypersensitivity.
Nervous systems disorders.
Common: headache, dizziness.
Gastrointestinal disorders.
Common: diarrhoea, nausea, dyspepsia, abdominal pain.
Uncommon: vomiting, anorexia, dry mouth, flatulence.
Not known: antibiotic-associated colitis (see Section 4.4 Special Warnings and Precautions for Use, Antibiotic-associated diarrhoea).
Skin and subcutaneous tissue disorders.
Uncommon: rash, urticaria, pruritus.
Not known: angioedema.
One patient in a pivotal trial developed unilateral optic neuritis, considered possibly related to fosfomycin therapy.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at http://www.tga.gov.au/reporting-problems.4.9 Overdose
In acute toxicity studies a single oral dose of 5000 mg/kg was well tolerated both in mice and rats and a single dose of 2000 mg/kg did not produce changes in rabbits and dogs.
Repeated dose studies by oral route showed that the no-effect dose was between 100 and 200 mg/kg after 4 weeks of treatment in dogs and rats, respectively.
Signs and symptoms.
Experience regarding the overdose of oral fosfomycin is limited. Cases of hypotonia, somnolence, electrolytes disturbances, thrombocytopenia and hypoprothrombinemia have been reported with parenteral use of fosfomycin.
Recommended treatment.
In the event of overdose, the patient must be monitored (particularly for plasma/serum electrolyte levels), and treatment should be symptomatic and supportive. Rehydration is recommended to promote urinary elimination of the active substance. Fosfomycin is effectively cleared from the body by haemodialysis with a mean elimination half-life of approximately 4 hours.
For information on the management of overdose, contact the Poisons Information Centre on 131126 (Australia).5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
Fosfomycin inhibits the first stage of bacterial wall synthesis. It inhibits the phosphoenolpyruvate transferase enzyme, thereby irreversibly blocking the condensation of uridine diphosphate-N-acetylglucosamine with p-enolpyruvate.
Fosfomycin is actively transported into the bacterial cell via two different transport systems (the sn-glycerol-3-phosphate and hexose-6 transport systems). Fosfomycin has a mainly bactericidal action. It can also reduce bacterial adhesion to bladder mucosa, which can be a predisposing factor for recurring infections. As this mechanism of action is unique to fosfomycin cross-resistance is not expected with other antibiotics.
Microbiology.
The activity of fosfomycin against E. coli isolates causing uncomplicated UTIs in females greater than 12 years of age in Australia were tested by the European Committee on Antimicrobial Susceptibility Testing (EUCAST) disk diffusion method. Isolates determined to be resistant by disk diffusion were retested by agar dilution susceptibility testing using EUCAST methodology. Based upon Table 2's breakpoints the local susceptibility data from these studies conducted in 2019 and 2020 determined that 99.3% (n=1033 isolates tested) and 99.6% (n=1023 isolates tested) were fosfomycin susceptible.
Activity in vitro.
Bacterial species commonly susceptible to fosfomycin using European Committee on Antimicrobial Susceptibility Testing (EUCAST) or Clinical and Laboratory Standard Institute (CLSI) susceptibility testing guidelines: Escherichia coli, Enterococcus faecalis.
Oral fosfomycin is not recommended in the treatment of the following bacterial species which do not have EUCAST or CLSI susceptibility testing guidelines: Staphylococcus saprophyticus, Pseudomonas aeruginosa, Enterococcus faecium, Staphylococcus aureus, Acinetobacter spp., Stenotrophomonas maltophilia, Bacteroides spp., Enterobacterales (other than E. coli), and other anaerobic bacteria.
Resistance.
Main mechanism of resistance is a chromosomal mutation causing an alteration of the bacterial fosfomycin transport systems. Plasmid-encoded mechanisms of resistance to fosfomycin have also been documented.
 Based on EUCAST criteria, fosfomycin trometamol single 3 g oral dose is calibrated for the treatment of acute uncomplicated UTI caused by Escherichia coli. The minimum inhibitory concentration (MIC) breakpoints are ≤ 8 (less than or equal to) mg/L (S) and > 8 mg/L (R). EUCAST disk diffusion zone diameter breakpoints for E. coli only are ≥ 24 mm (S) and < 24 mm (R). All methods require glucose-6-phosphate supplementation.
Based on EUCAST criteria, fosfomycin trometamol single 3 g oral dose is calibrated for the treatment of acute uncomplicated UTI caused by Escherichia coli. The minimum inhibitory concentration (MIC) breakpoints are ≤ 8 (less than or equal to) mg/L (S) and > 8 mg/L (R). EUCAST disk diffusion zone diameter breakpoints for E. coli only are ≥ 24 mm (S) and < 24 mm (R). All methods require glucose-6-phosphate supplementation.
There are no published EUCAST breakpoints for fosfomycin trometamol single 3 g oral dose for other urinary pathogens, such as Enterobacterales other than E. coli, Pseudomonas spp., Staphylococcus saprophyticus, or Enterococcus spp.
Based on CLSI criteria, only E. coli and Enterococcus faecalis from urinary tract isolates are calibrated. MIC breakpoints for both are ≤ 64 mg/L (S), 128 mg/L (intermediate [I]), and ≥ 256 mg/L (R). Disk and agar dilution MIC methods are approved provided there is supplemental glucose-6-phosphate. CLSI does not recommend broth dilution fosfomycin susceptibility testing.
There are no CLSI guidelines for any other bacteria apart from E. coli and Enterococcus faecalis.
Clinical efficacy against specific pathogens.
The prevalence of acquired resistance may vary geographically and with time for selected species and local information on resistance is desirable.
Oral fosfomycin should be used where there is resistance to other suitable antibiotics, including trimethoprim, cephalexin and amoxycillin/clavulanic acid.
Pharmacokinetic (PK)/pharmacodynamic (PD) relationship.
Limited data indicate that fosfomycin most likely acts in a concentration-dependent manner. There are no known PK/PD breakpoints for fosfomycin.
Clinical trials.
In three phase 3 prospective parallel multi-centre double-blind double-dummy randomised trials of acute uncomplicated UTI performed in the 1990s, a single 3 g oral dose of fosfomycin was compared to three other oral antibiotics (see Table 3). The study population consisted of female patients with symptoms and signs of acute lower UTI of less than 4 days duration, no manifestations of upper tract infection (e.g. flank pain, chills, fever), no history of recurrent UTIs (20% of patients in the clinical studies had a prior episode of acute uncomplicated lower UTI within the preceding year), no known structural abnormalities, no clinical or laboratory evidence of hepatic dysfunction, and no known or suspected CNS disorders, such as epilepsy, or other factors which would predispose to seizures. In the first two studies (MON-US-01 comparator arm ciprofloxacin and MON-US-02 comparator arm trimethoprim/sulphamethoxazole), adult females aged 18 years and older were enrolled and patients with renal dysfunction (defined as serum creatinine clearance < 30 mL/min) were excluded. In the third study (MON-US-03, nitrofurantoin comparator), females aged 12 years and older were enrolled and patients with severe renal dysfunction (defined as serum creatinine clearance < 60 mL/min) were excluded. In all three studies, pregnancy, immunosuppression and neutropenia were exclusion criteria.
In these studies, the following clinical success (resolution of symptoms) and microbiologic eradication rates were obtained (Table 3):
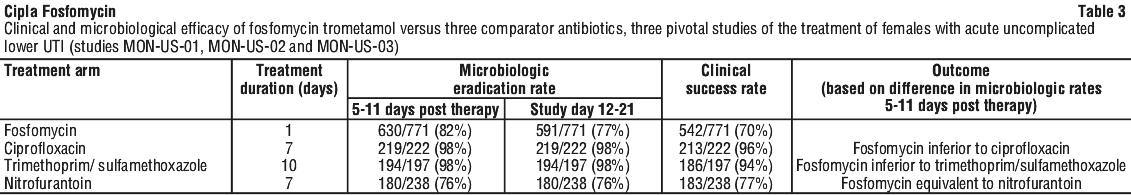 In the 3 pivotal studies, median age of patients enrolled was 27-32 years (fosfomycin) and 27-32 years (comparator arms). In all 3 studies, approximately half the patients were aged 30 years or less. The most common pathogen in the three pivotal studies was E. coli, which caused 82-86% of UTIs. Table 4 shows microbiological cure rates from pooled data from the 3 studies by pathogen.
In the 3 pivotal studies, median age of patients enrolled was 27-32 years (fosfomycin) and 27-32 years (comparator arms). In all 3 studies, approximately half the patients were aged 30 years or less. The most common pathogen in the three pivotal studies was E. coli, which caused 82-86% of UTIs. Table 4 shows microbiological cure rates from pooled data from the 3 studies by pathogen.
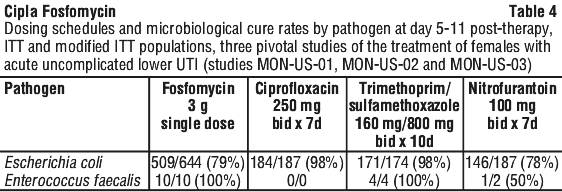 There have been no other phase 3 prospective, parallel, multicentre, double-blind, double-dummy randomised efficacy and safety trials for the treatment of acute uncomplicated UTI since the three pivotal studies MON-US-01, MON-US-02, and MON-US-03 performed in the 1990s.
There have been no other phase 3 prospective, parallel, multicentre, double-blind, double-dummy randomised efficacy and safety trials for the treatment of acute uncomplicated UTI since the three pivotal studies MON-US-01, MON-US-02, and MON-US-03 performed in the 1990s.
5.2 Pharmacokinetic Properties
Absorption.
After oral administration, fosfomycin is well absorbed from the gut and has an absolute bioavailability of about 35-40%. Food delays absorption, not influencing urinary concentrations.
Distribution.
Fosfomycin is distributed to the kidneys, bladder wall, prostate and seminal vesicles. Sustained concentrations of fosfomycin higher than the MIC are obtained in urine for 24-48 hours after oral administration.
Fosfomycin does not bind to plasma proteins, fosfomycin has been shown to cross the placental barrier in humans and animals.
Metabolism.
Fosfomycin does not appear to be metabolised.
Excretion.
Fosfomycin is excreted unchanged mainly via the kidneys by glomerular filtration (40-50% of the dose is found in the urine) with an elimination half-life of about 4 hours and to a lesser extent in faeces (18-28% of the dose). The appearance of a second serum peak 6 and 10 hours after drug intake suggests that the drug is subject to enterohepatic recirculation.
Special populations.
Elderly.
The pharmacokinetic features of fosfomycin are not modified by age (see Section 4.4 Special Warnings and Precautions for Use, Use in the elderly).
Pregnancy.
The pharmacokinetic features of fosfomycin do not appear to be modified by pregnancy in a study of 4 pregnant patients (also see Section 4.6 Fertility, Pregnancy and Lactation, Use in pregnancy).
Hepatic impairment.
The pharmacokinetic features of fosfomycin have not been studied in patients with impaired hepatic function. However, fosfomycin does not undergo hepatic metabolism and clearance is known to be predominantly renal with urinary excretion. Limited studies confirm that there is an enterohepatic recirculation which does not influence bioavailability (also see Section 4.3 Contraindications; Section 4.4 Special Warnings and Precautions for Use, Use in hepatic impairment).
Renal impairment.
The pharmacokinetics of fosfomycin trometamol have not been studied in patients undergoing peritoneal dialysis or haemofiltration.
In 5 anuric patients undergoing haemodialysis, the t1/2 of fosfomycin during haemodialysis was 40 hours. In patients with varying degrees of renal impairment (creatinine clearances varying from 54 mL/min to 7 mL/min), the t1/2 of fosfomycin increased from 11 hours to 50 hours. The percent of fosfomycin recovered in urine decreased from 32% to 11% indicating that renal impairment significantly decreases the excretion of fosfomycin.
The drug accumulates in patients with severe renal impairment but the significance of this is unknown. Linear relationships have been established between fosfomycin pharmacokinetic parameters and glomerular filtration rate.
Also see Section 4.3 Contraindications; Section 4.4 Special Warnings and Precautions for Use, Use in renal impairment.
5.3 Preclinical Safety Data
Genotoxicity.
Fosfomycin was not found to be genotoxic under in vitro (bacterial reverse mutation assay, mammalian mutation assay, chromosomal aberration test) or in vivo conditions (mouse micronucleus test).
Carcinogenicity.
Carcinogenicity studies in rodents have not been conducted. Based on the short-term use of fosfomycin and the lack of evidence of genotoxicity, fosfomycin is not anticipated to be carcinogenic.6 Pharmaceutical Particulars
6.1 List of Excipients
Each sachet of Cipla Fosfomycin also contains the following excipients: Mandarin flavour spray dried 0470277 (141665), Orange flavour 501071 AP0551 (111446), saccharin and 2.213 g of sucrose.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
Each carton contains 1 sachet which is a 4 ply laminate foil (41 gsm OLB paper/17 gsm PE/ 12 micron aluminum foil/35 gsm PE).
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure.
Chemically, fosfomycin trometamol is 2-Amino-2-(hydroxymethyl)propane-1,3-diol hydrogen (2R, 3S)-(3-methyloxiran-2-yl)phosphonate and has the following chemical structure:
 Molecular formula: C7H18NO7P.
Molecular formula: C7H18NO7P.
Relative molecular mass: 259.2.
CAS number.
78964-85-9.7 Medicine Schedule (Poisons Standard)
Prescription only medicine (Schedule 4).
Summary Table of Changes


 The following list displays adverse drug reactions that have been reported with the use of fosfomycin from either clinical-trial or post-marketing experiences.
The following list displays adverse drug reactions that have been reported with the use of fosfomycin from either clinical-trial or post-marketing experiences. Based on EUCAST criteria, fosfomycin trometamol single 3 g oral dose is calibrated for the treatment of acute uncomplicated UTI caused by Escherichia coli. The minimum inhibitory concentration (MIC) breakpoints are ≤ 8 (less than or equal to) mg/L (S) and > 8 mg/L (R). EUCAST disk diffusion zone diameter breakpoints for E. coli only are ≥ 24 mm (S) and < 24 mm (R). All methods require glucose-6-phosphate supplementation.
Based on EUCAST criteria, fosfomycin trometamol single 3 g oral dose is calibrated for the treatment of acute uncomplicated UTI caused by Escherichia coli. The minimum inhibitory concentration (MIC) breakpoints are ≤ 8 (less than or equal to) mg/L (S) and > 8 mg/L (R). EUCAST disk diffusion zone diameter breakpoints for E. coli only are ≥ 24 mm (S) and < 24 mm (R). All methods require glucose-6-phosphate supplementation. In the 3 pivotal studies, median age of patients enrolled was 27-32 years (fosfomycin) and 27-32 years (comparator arms). In all 3 studies, approximately half the patients were aged 30 years or less. The most common pathogen in the three pivotal studies was E. coli, which caused 82-86% of UTIs. Table 4 shows microbiological cure rates from pooled data from the 3 studies by pathogen.
In the 3 pivotal studies, median age of patients enrolled was 27-32 years (fosfomycin) and 27-32 years (comparator arms). In all 3 studies, approximately half the patients were aged 30 years or less. The most common pathogen in the three pivotal studies was E. coli, which caused 82-86% of UTIs. Table 4 shows microbiological cure rates from pooled data from the 3 studies by pathogen. There have been no other phase 3 prospective, parallel, multicentre, double-blind, double-dummy randomised efficacy and safety trials for the treatment of acute uncomplicated UTI since the three pivotal studies MON-US-01, MON-US-02, and MON-US-03 performed in the 1990s.
There have been no other phase 3 prospective, parallel, multicentre, double-blind, double-dummy randomised efficacy and safety trials for the treatment of acute uncomplicated UTI since the three pivotal studies MON-US-01, MON-US-02, and MON-US-03 performed in the 1990s. Molecular formula: C7H18NO7P.
Molecular formula: C7H18NO7P.