What is in this leaflet
This leaflet answers some common questions about Colese.
It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you taking this medicine against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What Colese is used for
Colese is used relieve the symptoms of irritable bowel syndrome, which can include, abdominal pain and cramps, bowel spasm, diarrhoea and flatulence.
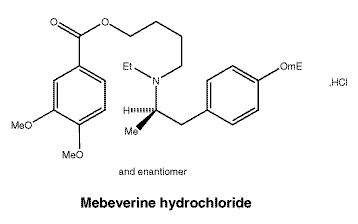
Colese belongs to a group of medicines called known as antispasmodic agents. Colese is also known as mebeverine hydrochloride.
Colese works by relaxing the muscles in the gut, thereby relieving the symptoms of irritable bowel syndrome.
Ask your doctor if you have any questions about why it has been prescribed for you. Your doctor may have prescribed it for another purpose.
This medicine is available only with a doctor's prescription.
Before you take Colese
When you must not take it
Do not take Colese if you have an allergy to:
- any medicine containing mebeverine hydrochloride
- any of the ingredients listed at the end of this leaflet
Some symptoms of an allergic reaction include skin rash, itching, shortness of breath or swelling of the face, lips or tongue, which may cause difficulty in swallowing or breathing.
Do not take it after the expiry date printed on the pack or if the packaging is damaged or shows signs of tampering. If it has expired or is damaged return it to your pharmacist for disposal.
Before you start to take it
Tell your doctor or pharmacist if you have any allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any of the following medical conditions:
- angina or other heart conditions
- liver problems
- kidney problems
- lactose intolerance
Tell your doctor if you are pregnant, intend to become pregnant, or are breastfeeding Your doctor can discuss the risks and benefits involved.
If you have not told your doctor about any of the above, tell them before you start taking Colese.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you buy without a prescription from your pharmacy, supermarket or health food store.
How to take Colese
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
If you do not understand the instructions on the box ask your doctor or pharmacist for help.
How much to take
The usual dose is one tablet three times a day.
How to take it
Swallow the tablets with a glass of water.
When to take it
Take Colese immediately before or during a meal.
Take Colese at about the same time each day. Taking it at the same time each day will have the best effect. It will also help you remember when to take it.
How long to take it
Continue taking your medicine for as long as your doctor tells you.
It is important to keep taking your medicine even if you feel well.
If you forget to take it
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Otherwise, take it as soon as you remember, and then go back to taking your medicine as you would normally.
Do not take a double dose to make up for the dose that you missed. This may increase the chance of getting an unwanted side effect.
If you are not sure what to do, ask your doctor or pharmacist.
If you have trouble remembering when to take your medicine, ask your pharmacist for advice.
If you take too much (overdose)
Immediately telephone your doctor, or the Poisons Information Centre (telephone Australia 13 11 26 or New Zealand 0800 764766), or go to Accident and Emergency at your nearest hospital, if you think you or anyone else may have taken too much Colese. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
While you are taking Colese
Things you must do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking Colese.
Tell any other doctors, dentists and pharmacists who treat you that you are taking this medicine.
If you are going to have surgery, tell the surgeon that you are taking this medicine.
If you become pregnant while you are taking this medicine, tell your doctor or pharmacist immediately.
Things you must not do
Do not use this medicine to treat any other complaints unless your doctor or pharmacist tells you to.
Do not give this medicine to anyone else, even if they have the same condition as you.
Do not stop taking Colese, or lower the dosage, without checking with your doctor.
Things to be careful of
Be careful driving or operating machinery until you know how Colese affects you.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking Colese.
It helps most people with irritable bowel syndrome, but it may have unwanted side effects in a few people. All medicines have some unwanted side effects. Sometimes they are serious, but most of the time they are not. You may need medical attention if you get some of the side-effects.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor or pharmacist if you notice any of the following and they worry you:
- indigestion or heartburn
- constipation
- dizziness
- headache
- tiredness
- difficulty sleeping
- loss of appetite
The above list includes the more common side effects of your medicine. They are usually mild and short-lived.
If any of the following happen, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- swelling of the face, lips or tongue
- difficulty swallowing or breathing
The above list includes very serious side effects. You may need urgent medical attention. These side effects are rare.
Tell your doctor or pharmacist if you notice anything else that is making you feel unwell. Other side effects not listed above may occur in some people.
After using Colese
Storage
Keep your tablets in the pack until it is time to take them. If you take the tablets out of the box or the blister pack they may not keep well.
Keep the medicine in a cool, dry place where the temperature stays below 25°C.
Do not store it or any other medicine in the bathroom, near a sink, or on a windowsill. Do not leave it in the car. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor or pharmacist tells you to stop taking this medicine, or the medicine has passed its expiry date, ask your pharmacist what to do with any that are left over.
Product description
What it looks like
Colese tablets are white, round sugar-coated tablets.
Colese tablets are available in boxes of 30 and 90 tablets.
Ingredients
Each Colese tablet contains 135 mg of mebeverine hydrochloride as the active ingredient:
It also contains
- lactose monohydrate
- potato starch
- povidone
- purified talc
- magnesium stearate
- sucrose
- gelatine
- acacia
- carnauba wax
Colese tablets contain lactose, sugars and sulfites. This medicine does not contain gluten.
Supplier
Colese is made in France.
Colese is distributed in Australia by:
Mylan Health Pty Ltd
Level 1, 30 The Bond
30-34 Hickson Road
Millers Point NSW 2000
www.mylan.com.au
Phone: 1800 314 527
®Registered Trademark
This leaflet was prepared in April 2020
Australian Registration Number(s)
316010
Colese_cmi\Apr20/00
Published by MIMS June 2020