1 Name of Medicine
Cyclizine lactate.
2 Qualitative and Quantitative Composition
Each 1 mL ampoule contains 50 mg cyclizine lactate.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Cyclizine Juno injection is a clear, colourless sterile solution for injection.
4.1 Therapeutic Indications
Cyclizine Juno is indicated for the prevention of nausea and vomiting in the post-operative period.
4.2 Dose and Method of Administration
Treatment with Cyclizine Juno should commence within the first 24 hours of surgery and should not continue beyond 48 hours.
There are no data on the use of Cyclizine Juno in the treatment of established post-operative nausea and vomiting.
Product is for single use in one patient only. Discard any residue.
Route of administration.
Intravenous.
Adults.
50 mg intravenously up to three times daily.
When used intravenously, Cyclizine Juno should be injected slowly into the bloodstream, with only minimal withdrawal of blood into the syringe.
For the prevention of postoperative nausea and vomiting, administer the first dose by slow intravenous injection 20 minutes before the anticipated end of surgery.
Elderly.
There have been no specific studies of Cyclizine Juno Injection in the elderly. Experience has indicated that normal adult dosage is appropriate.4.3 Contraindications
Cyclizine Juno should not be given to individuals with known hypersensitivity to cyclizine or to any of the excipients.
Cyclizine Juno should not be given to patients who have severe heart failure or acute myocardial infarction. In such patients, cyclizine may cause a fall in cardiac output associated with increases in heart rate, mean arterial pressure and pulmonary wedge pressure.
Cyclizine Juno should not be given to patients who have acute alcohol intoxication. The anti-emetic properties of cyclizine may increase the toxicity of alcohol.
4.4 Special Warnings and Precautions for Use
Anticholinergic effects.
Cyclizine has anticholinergic effects and may precipitate pre-existing conditions that are likely to be exacerbated by anticholinergic activity, such as urinary retention or obstruction, hepatic disease, phaeochromocytoma, hypertension, epilepsy, prostatic hypertrophy, angle- closure glaucoma, untreated intraocular hypertension, or uncontrolled primary open-angle glaucoma. It may also exacerbate gastrointestinal obstructive disorders and cause dry mouth and constipation.
It has been suggested that the anticholinergic effect of antihistamines such as cyclizine may reduce the volume and cause thickening of bronchial secretions, resulting in obstruction of respiratory tract. Cyclizine should be administered cautiously in patients with asthma or chronic obstructive pulmonary disease.
Cardiovascular effects.
Cyclizine should not be used in patients with severe heart failure or acute myocardial infarction (see Section 4.3 Contraindications). In such patients, cyclizine may cause a fall in cardiac output associated with increases in heart rate, mean arterial pressure and pulmonary wedge pressure.
Use in porphyria.
Cyclizine should be avoided in porphyria.
Nervous system.
Nervous system side effects of cyclizine have included drowsiness and sedation in many patients. Motor skills may be impaired. Cyclizine may also cause restlessness, excitation, nervousness and insomnia. Extrapyramidal effects may occur and dystonic reactions have been reported after single doses of cyclizine.
There have been reports of abuse of cyclizine, either oral or intravenous, for its euphoric or hallucinatory effects. The concomitant misuse of Cyclizine Juno with large amounts of alcohol is particularly dangerous, since the antiemetic effect of cyclizine may increase the toxicity of alcohol (see Section 4.3 Contraindications).
There have been case reports of paralysis occurring in patients using intravenous cyclizine. Some of the patients mentioned in these reports had an underlying neuromuscular disorder. Thus, intravenous cyclizine should be used with caution in all patients in general, and in patients with underlying neuromuscular disorders in particular.
Studies designed to detect drowsiness did not reveal sedation in healthy adults who took a single oral therapeutic dose (50 mg) of cyclizine lactate. Sedation of short duration was reported by subjects receiving intravenous cyclizine. Patients should not drive or operate machinery until they have determined their own response.
Although there are no data available, patients should be cautioned that Cyclizine Juno may have additive effects with alcohol and other central nervous system depressants, e.g. hypnotics and tranquillisers.
In studies in which atropine has been used as part of the anaesthetic regime, cyclizine has been found to be not effective in treating PONV. This may be due to the central anti-cholinergic activity of atropine affecting the anti-emetic effect of cyclizine.
Use in the elderly.
There have been no specific studies of Cyclizine Juno in the elderly. Experience has indicated that normal adult dosage is appropriate.
Paediatric use.
The safety and effectiveness of cyclizine in the treatment of post-operative nausea and vomiting has not been assessed in children. Children may be more sensitive to the anticholinergic side effects of cyclizine. Use is not recommended.
Effects on laboratory tests.
No data available.4.5 Interactions with Other Medicines and Other Forms of Interactions
Cyclizine Juno may have additive effects with alcohol and other central nervous system depressants e.g. hypnotics, tranquilisers, anaesthetics, antipsychotics, barbiturates.
Cyclizine Juno enhances the soporific effect of pethidine and may counteract the haemodynamic benefits of opioid analgesics. In nonclinical studies, cyclizine potentiated the antinociceptive effects of pentazocine and morphine in rodents.
Because of its anticholinergic activity, cyclizine may enhance the adverse effects of other anticholinergic medicines, and have an additive antimuscarinic action with other antimuscarinic drugs, such as atropine and some antidepressants (both tricyclics and monoamine oxidase inhibitors).
Cyclizine Juno may mask the warning signs of damage caused by ototoxic drugs such as aminoglycoside antibacterials.
In studies in which atropine has been used as part of the anaesthetic regime, cyclizine has been found to be not effective in treating PONV. This may be due to the central anticholinergic activity of atropine affecting the anti-emetic effect of cyclizine.
In vitro studies using human liver preparations identified a weak inhibitory effect of cyclizine on CYP2D6 (IC50 109 microM) which is unlikely to be clinically relevant, and moderate inhibitory activity on estrone sulfotransferase at a concentration (IC50 0.44 microM) close to clinical plasma concentrations, although the clinical significance is not known.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
The effects of cyclizine on human fertility are unknown. There are no adequate nonclinical studies of the effects of cyclizine on fertility.
(Category B3)
Administration of cyclizine to rats, mice and rabbits during gestation was associated with malformations including cleft palate and various cephalic abnormalities; the no-effect doses determined in rats and rabbits were 50 and 25 mg/kg/day, respectively. There has been no systematic assessment of the safety of cyclizine in human pregnancy therefore the use of Cyclizine Juno in pregnancy is not recommended.
It is not known whether cyclizine and/or its metabolites are excreted in human milk. The use of Cyclizine Juno in breastfeeding women is not recommended.4.7 Effects on Ability to Drive and Use Machines
Patients given intravenous cyclizine should not drive or operate machinery until they have determined their own response.
Although there are no data available, patients should be cautioned that Cyclizine Juno may have additive effects with alcohol and other central nervous system depressants, e.g. anaesthetic agents, hypnotics and tranquillizers.
4.8 Adverse Effects (Undesirable Effects)
The incidence of adverse effects due to cyclizine alone has not been examined in clinical trials and the incidence of adverse events listed in this section has not been accurately determined.
Blood and lymphatic system disorders.
Agranulocytosis, leukopenia, haemolytic anaemia, thrombocytopenia.
Cardiac disorders.
Tachycardia, palpitations, arrhythmias.
Eye disorders.
Blurred vision, oculogyric crisis.
Ear and labyrinth disorders.
Tinnitus.
Gastrointestinal system disorders.
Dry mouth, nose and throat, constipation, duodenogastric reflux, nausea, vomiting, diarrhoea, abdominal pain upper, decreased appetite.
General disorders and administration site conditions.
Asthenia.
Injection site reactions (including vein tracking, erythema, pain, thrombophlebitis and blisters). A sensation of heaviness, chills and pruritus have been reported rarely.
Anaphylaxis has been recorded following intravenous administration of cyclizine co- administered with propanidid in the same syringe.
Hepatobiliary disorders.
Hepatic dysfunction, hypersensitivity hepatitis, cholestatic jaundice and cholestatic hepatitis.
Immune system disorders.
Hypersensitivity reactions, including anaphylaxis.
Musculoskeletal and connective tissue disorders.
Twitching, muscle spasms.
Nervous system disorders.
Effects on the central nervous system have been reported with cyclizine. These include somnolence, headache, coordination abnormal, dystonia, dyskinesia, extrapyramidal motor disturbances, tremor, convulsions, dizziness, decreased consciousness, transient speech disorders, paraesthesia, generalised chorea and paralysis. The use of intravenous cyclizine has been associated with cases of paralysis. The onset of paralysis is usually within minutes of administration, affects the limbs, and in most cases it resolves fully within hours of discontinuation of the medicine.
There have been rare case reports of patients experiencing depressed levels of consciousness/loss of consciousness.
Psychiatric disorders.
Disorientation, restlessness or agitation, nervousness, euphoria, insomnia and auditory and visual hallucinations have been reported, particularly when dosage recommendations have been exceeded.
Renal and urinary disorders.
Urinary retention.
Respiratory, thoracic and mediastinal disorders.
Bronchospasm, apnoea.
Skin and subcutaneous tissue disorders.
Urticaria, pruritus, drug rash, angioedema, allergic skin reactions, fixed drug eruption, photosensitivity reaction.
Vascular disorders.
Hypertension, hypotension.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at http://www.tga.gov.au/reporting-problems.4.9 Overdose
Symptoms.
Symptoms of acute toxicity from cyclizine arise from peripheral anticholinergic effects and effects on the central nervous system.
Peripheral anticholinergic symptoms include dry mouth, nose and throat, blurred vision, tachycardia and urinary retention. Central nervous system effects include drowsiness, dizziness, incoordination, ataxia, weakness, hyperexcitability, disorientation, impaired judgement, hallucinations, hyperkinesia, extrapyramidal motor disturbances, convulsions, hyperpyrexia and respiratory depression.
Treatment.
In the management of acute overdosage with Cyclizine Juno, supportive measures for respiration and circulation should be performed if necessary. Convulsions should be controlled in the usual way with parenteral anticonvulsant therapy.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
ATC code: R60AE03.
Pharmacotherapeutic group: Piperazine derivatives.
Cyclizine is a histamine H1 receptor antagonist of the piperazine class. It possesses anticholinergic and antiemetic properties. The exact mechanism by which cyclizine can prevent or suppress both nausea and vomiting from various causes is unknown.
Clinical trials.
The principal studies were conducted in young female patients only and may include data from older studies that may not align with current anaesthetic regimens and practice.
A Cochrane review of Drugs for Preventing Post-operative Nausea and Vomiting (PONV) was conducted. This systematic review included randomised, controlled trials that compared a drug with placebo or another drug prevention of PONV, or compared doses or timing of administration and reported PONV as an outcome. Studies of treatment for established PONV were excluded. Study drug could be given pre-operatively, at induction of anaesthesia, intra-operatively or post-operatively (before nausea and vomiting had occurred). Studies in the review could include participants undergoing general anaesthesia, regional anaesthesia or sedation. Overall the review included 737 studies involving 103,237 people. 60 different medications were identified, including cyclizine. A medication was considered effective if it achieved statistically significant benefits when compared to placebo for all four of the following outcomes: nausea, vomiting, nausea or vomiting; and use of rescue anti-emetic.
Efficacy in prevention of PONV was demonstrated for 8 of these 60 drugs, including cyclizine. The review included 10 studies that assessed the efficacy and safety of cyclizine. Compared with placebo, cyclizine had a Relative Risk of 0.65 (95% CI 0.47-0.90) for nausea, 0.57 (95% CI 0.43-0.75) for vomiting and 0.68 (95% CI 0.58-0.80) for nausea or vomiting and 0.27 (95% CI 0.14-0.62) for rescue antiemetic.
Summary results on the prevention of drug therapy related nausea and vomiting.
A study was carried out to compare the effectiveness of standard single-dose dexamethasone (n=30) and cyclizine (n=30) on PONV in women receiving spinal morphine and fentanyl for caesarean section under general anaesthesia. In relation to nausea severity scales, cyclizine was found to be superior to placebo (n=30) at 3 and 6 hours and superior to dexamethasone. With respect to vomiting episodes, cyclizine was found to be superior at 3 and 6 hours versus placebo and at 3 hours versus dexamethasone.
A study was carried out to examine the anti-emetic effect of cyclizine compared to droperidol when included in a patient-controlled analgesia (PCA) regime. No statistically significant differences between groups was found, results were closely similar and better than historical controls leading to author conclusion that "... we have shown cyclizine to be as effective as droperidol in the prevention of PONV when included in a PCA infusion of morphine."
A prospective randomised, double-blind study compared the (antiemetic) effects of cyclizine and perphenazine in reducing the emetic effects of morphine and pethidine. Cyclizine reduced sickness after pethidine pre-operatively p < 0.0001. Cyclizine reduced post- operative vomiting and nausea after morphine 10 mg, p < 0.001 and pethidine 100 mg, p < 0.0001. Cyclizine reduced PONV after morphine 15 mg (p < 0.0005).
5.2 Pharmacokinetic Properties
Distribution.
In healthy adult volunteers the following data were obtained from 6 subjects given a single bolus intravenous 25 mg dose of cyclizine lactate. See Table 1.
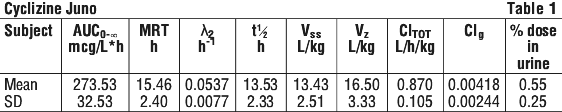
Metabolism.
The N-demethylated derivative, norcyclizine, has been identified as a metabolite of cyclizine.
Norcyclizine has little antihistaminic (H1) activity compared to cyclizine and has a plasma elimination half-life of approximately 14 hours.
Excretion.
After a single dose of 50 mg cyclizine lactate given to a single adult male volunteer, urine collected over the following 24 hours contained less than 1% of the total dose administered.
5.3 Preclinical Safety Data
Genotoxicity.
In bacterial reverse mutation assays, cyclizine per se was negative in all tested strains, while nitrosated cyclizine was positive in some strains. No other genotoxicity studies have been conducted with cyclizine.
Carcinogenicity.
No data available.6 Pharmaceutical Particulars
6.1 List of Excipients
Cyclizine Juno contains lactic acid and water for injections.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 30°C.
6.5 Nature and Contents of Container
1 mL clear, colourless, type 1 glass ampoules.
The ampoules are blister wrapped and placed in packs of 5 and 10.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Cyclizine Juno injection contains 50 mg/1 mL cyclizine lactate and has the following structural formula:
Chemical structure.

CAS number.
[82-92-8].
Molecular formula: C18H22N2.
Molecular weight: 266.
Cyclizine is a piperazine-derivative antihistamine used as an anti-emetic agent when given as cyclizine lactate solution by intravenous injection. Cyclizine is a water soluble, bitter, white crystalline, solid, with pKa1 = 2.16 and pKa2 = 8.05 and pH of 3.3 to 3.7.7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription only medicine.
Summary Table of Changes




