What is in this leaflet
This leaflet answers some common questions about this medicine. It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you taking this medicine against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What this medicine is used for
Dasatinib is used to treat adults aged 18 years or over with:
- Newly diagnosed Philadelphia chromosome positive (Ph+) chronic myeloid leukaemia (CML) in the chronic phase.
- Chronic, accelerated or myeloid or lymphoid blast phase chronic myeloid leukaemia with resistance or intolerance to prior therapy including imatinib.
- Philadelphia chromosome positive acute lymphoblastic leukaemia (ALL) with resistance or intolerance to prior therapy.
It belongs to a group of medicines called protein-tyrosinekinase inhibitors.
This medicine works by inhibiting the activity of proteins within the leukaemia cells of patients with CML or Ph+ ALL. These proteins are responsible for the uncontrolled growth of the leukaemia cells. By inhibiting these proteins dasatinib kills the leukaemia cells in the bone marrow and allows normal red cell, white cell and platelet production to resume.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another reason.
This medicine is available only with a doctor's prescription.
Before you take this medicine
When you must not take it
Do not take this medicine if you have an allergy to:
- any medicine containing dasatinib
- any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
If you think you are having an allergic reaction, do not take any more of the medicine and contact your doctor immediately or go to the Accident and Emergency department at the nearest hospital.
Do not take this medicine if you are pregnant or plan to become pregnant. Dasatinib can cause harm to the unborn baby if it is given to a pregnant woman.
Do not give this medicine to a child under the age of 18 years.
Do not take this medicine after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking this medicine, talk to your doctor.
Before you start to take it
Tell your doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any of the following medical conditions:
- problems with your immune system
- liver problem
- heart problem
- lactose intolerant
- hepatitis B infection.
Tell your doctor if you are pregnant or plan to become pregnant or are breastfeeding.
Women who are taking dasatinib should not breast-feed.
Tell your doctor if you are a sexually active man. Men who take dasatinib are advised to use a condom to avoid pregnancy in their partner.
Tell your doctor if you have recently been vaccinated or plan to get a vaccination.
Tell your doctor if you are planning to have surgery or an anaesthetic.
Tell your doctor if you are currently receiving or are planning to receive dental treatment.
If you have not told your doctor about any of the above, tell them before you start taking this medicine.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and dasatinib may interfere with each other. These include:
- Drugs that may increase dasatinib plasma concentrations, such as ketoconazole, itraconazole, erythromycin, clarithromycin, ritonavir, atazanavir, lopinavir, grapefruit juice.
- Drugs that may decrease dasatinib plasma concentrations, such as dexamethasone, phenytoin, carbamazepine, rifampicin, phenobarbital and St John’s wort.
- Dasatinib may alter the blood levels of ciclosporin.
- Medicines that reduce stomach acid, such as antacids and histamine-2 antagonists/proton pump inhibitors (famotidine and omeprazole).
- Drugs that may have their plasma concentration altered by dasatinib, such as simvastatin, astemizole, terfenadine, cisapride, pimozide, quinidine, bepridil or ergot alkaloids.
- Blood thinning medicines, such as warfarin, aspirin and nonsteroidal anti-inflammatory drugs (NSAIDs) may increase the risk of unwanted bleeding.
- Oral diabetes medicines from the glitazone family of drugs may interact with dasatinib.
- Medicines that neutralise stomach acid, such as aluminium hydroxide/magnesium hydroxide. Calcium carbonate and calcium carbonate/hydroxide. These medicines may be taken up to 2 hours before or 2 hours after dasatinib.
These medicines may be affected by dasatinib or may affect how well it works. You may need different amounts of your medicines, or you may need to take different medicines.
Other medicines not listed above may also interact with dasatinib.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while taking this medicine.
How to take this medicine
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
If you do not understand the directions, ask your doctor or pharmacist for help.
How much to take
Your doctor will tell you how much of this medicine you should take. This will depend on your condition and whether you are taking any other medicines.
You should take your tablets consistently either in the morning or in the evening.
100 mg per day
The usual starting dose is 100 mg once daily (either as one 100 mg tablet or two 50 mg tablets). The entire dose of 100 mg is to be taken at one time either in the morning or the evening.
OR
140 mg per day
Some patients may require an alternative starting dose (140 mg daily taken as two 70 mg tablets). The entire dose of 140 mg is to be taken at one time either in the morning or the evening.
Do not stop taking your medicine or change your dosage without first talking with your doctor.
Depending on your response and on any side effects that you may experience, your doctor may adjust your dose of dasatinib, upward or downward, or may temporarily discontinue your medicine.
How to take it
Swallow the tablets whole with a full glass of water.
Do not break, cut, chew or crush the tablet.
Do not take dasatinib with grapefruit or grapefruit juice.
When to take it
Take your medicine at about the same time each day. Taking it at the same time each day will have the best effect. It will also help you remember when to take it.
It does not matter if you take this medicine before or after food.
How long to take it
Continue taking your medicine for as long as your doctor tells you.
This medicine helps to control your condition but does not cure it. It is important to keep taking your medicine even if you feel well.
Make sure you have enough to last over weekends and holidays.
Continue taking your medicine until you finish the pack.
If you forget to take it
If it is almost time to take your next dose, skip the dose you missed and take your next dose when you are meant to.
Otherwise, take it as soon as you remember, and then go back to taking your medicine as you would normally.
Do not take a double dose to make up for the dose that you missed. This may increase the chance of you getting an unwanted side effect.
If you are not sure what to do, ask your doctor or pharmacist.
If you have trouble remembering to take your medicine, ask your pharmacist for some hints.
If you take too much (overdose)
Immediately telephone your doctor or the Poisons Information Centre (telephone 13 11 26) for advice or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have taken too much of this medicine. Do this even if there are no signs of discomfort or poisoning.
You may need urgent medical attention.
While you are using this medicine
Things you must do
If you become pregnant or plan to breastfeed while taking this medicine, tell your doctor immediately.
Tell any other doctors, dentists, and pharmacists who treat you that you are taking this medicine.
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking this medicine.
If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine. It may affect other medicines used during surgery.
Tell your doctor immediately if you experience bleeding or easy bruising, no matter how mild.
Notify your doctor immediately if you develop a fever while taking dasatinib.
Tell your doctor immediately if you experience shortness of breath and fatigue while taking dasatinib.
If you are about to have any blood tests, tell your doctor that you are taking this medicine. It may interfere with the results of some tests.
Keep all your doctor's appointments so that your progress can be checked.
Have any tests recommended by your doctor done as soon, as possible.
Your doctor may order routine laboratory tests to evaluate your blood counts to see how well dasatinib is working.
Things you must not do
Do not take this medicine to treat any other complaints unless your doctor tells you to.
Do not give your medicine to anyone else, even if they have the same condition as you.
Do not stop taking your medicine or change the dosage without checking with your doctor.
Things to be careful of
Be careful driving or operating machinery until you know how this medicine affects you. This medicine has been known to cause dizziness and light-headedness, in some people. If you have any of these symptoms, do not drive, operate machinery or do anything else that could be dangerous.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking this medicine.
Like all medicines, it is possible that dasatinib may have unwanted side effects in some people. There are many side effects caused by medicines used to treat leukaemia. During treatment with dasatinib you will require close medical supervision.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor or pharmacist if you notice any of the following and they worry you:
- headache; dizziness; numbness or tingling in arms, legs, fingers or toes; altered taste
- diarrhoea, nausea, vomiting
- shortness of breath, cough, accumulation of fluid in or around the lungs, pneumonia, chest pain
- infection, fever
- abdominal pain, bloating, flatulence, constipation, indigestion
- high blood pressure
- mouth ulcers
- skin rash, dermatitis (including eczema), dry skin, itching or peeling skin, flushing
- hair loss
- visual disturbances: blurry or diminished vision, dry eye
- fatigue
- swelling of the liver, abdomen, hands, lower legs, feet or face
- back pain, bone pain, joint pain, pain in fingers or toes, muscle aches or spasm, muscle weakness
- weight decrease, appetite disturbance
- gout
- conjunctivitis
- tinnitus (ringing in the ears)
- accumulation of fluid, foamy urine, weight gain (also known as nephrotic syndrome).
These are the more common side effects.
Tell your doctor as soon as possible if you notice any of the following:
- swelling, weight gain, shortness of breath or chest pain
- swelling around your eyes
- skin infection - folliculitis, herpes
- shortness of breath and fatigue
- dark coloured urine or yellowing of your skin and eyes.
If any of the following happen, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- changes in the way your heart beats, for example - if you notice it beating faster
- bleeding - for example from: gastrointestinal tract; eye; nose; gums; serious bruising or excessive menstrual bleeding
- infections - urinary tract; eye infection; difficulty breathing; coughing
- fever
- painful rash with blisters.
The use of dasatinib is also associated with a reduction in certain types of blood cells in the body:
- a reduction in red blood cells, which may result in fatigue or dizziness
- a reduction in white blood cells, which are used to fight infection
- a reduction in cells that help your blood to clot after injury.
The above list includes very serious side effects. You may need urgent medical attention or hospitalisation.
Other side effects not listed above may also occur in some people.
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Storage and Disposal
Storage
Keep your tablets in the pack until it is time to take them. If you take the tablets out of the pack they may not keep well.
Keep your medicine in a cool dry place where the temperature stays below 25°C.
Do not store this medicine or any other medicine in the bathroom or near a sink. Do not leave it on a window sill or in the car. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop taking this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Product description
What it looks like
Dasatinib 20 mg tablet
White to off-white, round, biconvex coated tablet. Engraved “APO” on one side, over “DA” over “20” on the other side.
Dasatinib 50 mg tablet
White to off-white, oval, bevelled- edged, biconvex coated tablet. Engraved “APO” on one side, “DAS50” on the other side.
Dasatinib 70 mg tablet
White to off-white, round, biconvex coated tablet. Engraved “APO” on one side, “DA” over “70” on the other side.
Dasatinib 100 mg tablet
White to off-white, oval, bevelled- edged, biconvex coated tablet. Engraved “APO” on one side, “DAS100” on the other side.
Note: Not all pack sizes may be available.
Ingredients
Each tablet contains 20 mg, 50 mg, 70 mg and 100 mg of dasatinib as the active ingredient.
This medicine also contains the following:
- microcrystalline cellulose
- ethylcellulose
- lactose monohydrate
- croscarmellose sodium
- magnesium stearate
- colloidal silicon dioxide
- hypromellose
- hyprolose
- triethyl citrate
- titanium dioxide
This medicine contains sugars as lactose.
This medicine does not contain gluten.
Australian Registration Numbers
Dasatinib ARX 20 mg tablets (blister): AUST R 290137.
Dasatinib ARX 20 mg tablets (bottle): AUST R 290129.
Dasatinib ARX 50 mg tablets (blister): AUST R 290131.
Dasatinib ARX 50 mg tablets (bottle): AUST R 290128.
Dasatinib ARX 70 mg tablets (blister): AUST R 290140.
Dasatinib ARX 70 mg tablets (bottle): AUST R 290136.
Dasatinib ARX 100 mg tablets (blister): AUST R 290143.
Dasatinib ARX 100 mg tablets (bottle): AUST R 290134.
Sponsor
This medicine is supplied in Australia by:
Arrotex Pharmaceuticals Pty Ltd
15-17 Chapel St
Cremorne VIC 2121
Tel: 1300 927 769
http://arrotex.com.au/
This leaflet was prepared in August 2023.
Published by MIMS October 2023





 Myelosuppression was commonly reported in all patient populations. In newly diagnosed chronic phase CML, myelosuppression was less frequently reported than in chronic phase CML patients with resistance or intolerance to prior imatinib therapy. The frequency of Grade 3 or 4 neutropenia, thrombocytopenia and anaemia was higher in patients with advanced CML or Ph+ ALL than in chronic phase CML.
Myelosuppression was commonly reported in all patient populations. In newly diagnosed chronic phase CML, myelosuppression was less frequently reported than in chronic phase CML patients with resistance or intolerance to prior imatinib therapy. The frequency of Grade 3 or 4 neutropenia, thrombocytopenia and anaemia was higher in patients with advanced CML or Ph+ ALL than in chronic phase CML.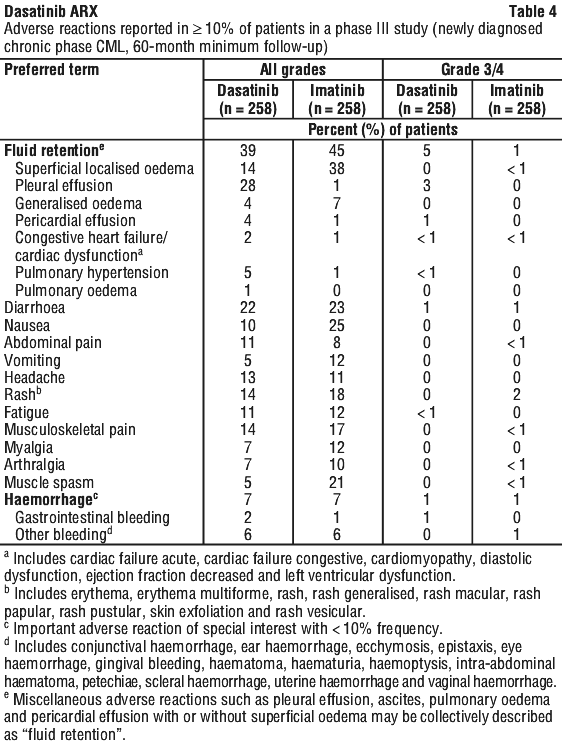 A comparison of cumulative rates of selected adverse reactions in the Phase III study of newly diagnosed patients with chronic phase CML with minimum follow-up of one and five years are shown in Table 5.
A comparison of cumulative rates of selected adverse reactions in the Phase III study of newly diagnosed patients with chronic phase CML with minimum follow-up of one and five years are shown in Table 5.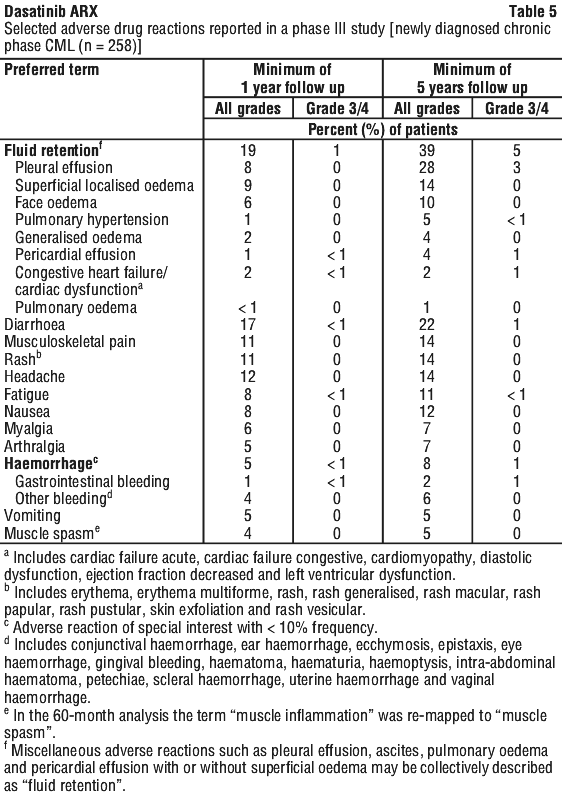 In the Phase III dose-optimisation study in patients with chronic phase CML resistant or intolerant to imatinib, the overall median duration of therapy was approximately 30 months (range < 1-93 months), with a median duration in the 100 mg once daily group of 37 months (range 1-91 months). The study evaluated once daily and twice daily dosage regimens (100 mg and 140 mg once daily, and 50 mg and 70 mg twice daily). Following Year 2 analysis many patients switched to once daily dosing regimens during the subsequent extension of the study. Cumulative rates of selected adverse reactions that were reported in the 100 mg once daily recommended starting dose (n = 165) are shown in Table 6.
In the Phase III dose-optimisation study in patients with chronic phase CML resistant or intolerant to imatinib, the overall median duration of therapy was approximately 30 months (range < 1-93 months), with a median duration in the 100 mg once daily group of 37 months (range 1-91 months). The study evaluated once daily and twice daily dosage regimens (100 mg and 140 mg once daily, and 50 mg and 70 mg twice daily). Following Year 2 analysis many patients switched to once daily dosing regimens during the subsequent extension of the study. Cumulative rates of selected adverse reactions that were reported in the 100 mg once daily recommended starting dose (n = 165) are shown in Table 6. In the Phase III dose-optimisation study in patients with advanced phase CML and Ph+ ALL, the median duration of treatment was 14 months (range < 1-36 months) for accelerated phase CML; 3 months (range < 1-32 months) for myeloid blast CML; 4 months (< 1-22 months) for lymphoid blast CML; and 3 months (< 1-29 months) for Ph+ ALL. Selected adverse drug reactions that were reported at the recommended starting dose of 140 mg once daily are shown in Table 7. A 70 mg twice daily regimen was also studied. At Year 2 analysis, the 70 mg twice daily regimen showed a comparable efficacy profile to the 140 mg once daily regimen, but a less favourable safety profile; particularly the fluid retention (pleural effusion and pericardial effusion) was reported less frequently in patients treated with dasatinib 140 mg once daily than in those treated with 70 mg twice daily.
In the Phase III dose-optimisation study in patients with advanced phase CML and Ph+ ALL, the median duration of treatment was 14 months (range < 1-36 months) for accelerated phase CML; 3 months (range < 1-32 months) for myeloid blast CML; 4 months (< 1-22 months) for lymphoid blast CML; and 3 months (< 1-29 months) for Ph+ ALL. Selected adverse drug reactions that were reported at the recommended starting dose of 140 mg once daily are shown in Table 7. A 70 mg twice daily regimen was also studied. At Year 2 analysis, the 70 mg twice daily regimen showed a comparable efficacy profile to the 140 mg once daily regimen, but a less favourable safety profile; particularly the fluid retention (pleural effusion and pericardial effusion) was reported less frequently in patients treated with dasatinib 140 mg once daily than in those treated with 70 mg twice daily. The following adverse reactions, excluding laboratory abnormalities, were reported in patients in dasatinib clinical trials. These reactions are presented by system organ class and by frequency. Frequencies are defined as: very common (≥ 1/10); common (≥ 1/100 to < 1/10); uncommon (≥ 1/1,000 to < 1/100); rare (≥ 1/10,000 to < 1/1,000). Within each frequency grouping, undesirable effects are presented in order of decreasing seriousness.
The following adverse reactions, excluding laboratory abnormalities, were reported in patients in dasatinib clinical trials. These reactions are presented by system organ class and by frequency. Frequencies are defined as: very common (≥ 1/10); common (≥ 1/100 to < 1/10); uncommon (≥ 1/1,000 to < 1/100); rare (≥ 1/10,000 to < 1/1,000). Within each frequency grouping, undesirable effects are presented in order of decreasing seriousness. After 60 months follow-up, median time to cCCyR was 3.1 months in the 214 dasatinib group responders and 5.8 months in the 204 imatinib group responders. Median time to MMR after 60 months follow-up was 9.3 months in the 196 dasatinib group responders and 15.0 months in the 163 imatinib group responders. The rates of cCCyR in the dasatinib and imatinib treatment groups, respectively, within 3 months (54% and 30%), 6 months (70% and 56%), 9 months (75% and 63%), 24 months (80% and 74%), 36 months (83% and 77%), 48 months (83% and 79%) and 60 months (83% and 79%) were consistent with the primary endpoint. The rates of MMR in the dasatinib and imatinib treatment groups, respectively, within 3 months (8% and 0.4%), 6 months (27% and 8%), 9 months (39% and 18%), 12 months (46% and 28%), 24 months (64% and 46%), 36 months (67% and 55%), 48 months (73% and 60%) and 60 months (76% and 64%) were also consistent with the primary endpoint. With a minimum of 60 months follow up, the rate of CMR (i.e. at least 4.5-log reduction from a standardised baseline value BCR-ABL ratio ≤ 0.0032%) at any time was 44% versus 34% in the dasatinib and imatinib treatment groups, respectively.
After 60 months follow-up, median time to cCCyR was 3.1 months in the 214 dasatinib group responders and 5.8 months in the 204 imatinib group responders. Median time to MMR after 60 months follow-up was 9.3 months in the 196 dasatinib group responders and 15.0 months in the 163 imatinib group responders. The rates of cCCyR in the dasatinib and imatinib treatment groups, respectively, within 3 months (54% and 30%), 6 months (70% and 56%), 9 months (75% and 63%), 24 months (80% and 74%), 36 months (83% and 77%), 48 months (83% and 79%) and 60 months (83% and 79%) were consistent with the primary endpoint. The rates of MMR in the dasatinib and imatinib treatment groups, respectively, within 3 months (8% and 0.4%), 6 months (27% and 8%), 9 months (39% and 18%), 12 months (46% and 28%), 24 months (64% and 46%), 36 months (67% and 55%), 48 months (73% and 60%) and 60 months (76% and 64%) were also consistent with the primary endpoint. With a minimum of 60 months follow up, the rate of CMR (i.e. at least 4.5-log reduction from a standardised baseline value BCR-ABL ratio ≤ 0.0032%) at any time was 44% versus 34% in the dasatinib and imatinib treatment groups, respectively.
 The progression-free survival rate by specific timepoint is displayed graphically in Figure 1. Rate of PFS was consistently higher in dasatinib-treated patients who achieved BCR-ABL level ≤ 10% at 3 months than those who did not.
The progression-free survival rate by specific timepoint is displayed graphically in Figure 1. Rate of PFS was consistently higher in dasatinib-treated patients who achieved BCR-ABL level ≤ 10% at 3 months than those who did not. The overall survival rate by specific timepoint is displayed graphically in Figure 2. Rate of OS was consistently higher in dasatinib-treated patients who achieved BCR-ABL level ≤ 10% at 3 months than those who did not.
The overall survival rate by specific timepoint is displayed graphically in Figure 2. Rate of OS was consistently higher in dasatinib-treated patients who achieved BCR-ABL level ≤ 10% at 3 months than those who did not. The time to MMR is displayed graphically in Figure 3. The time to MMR was consistently shorter in dasatinib-treated subjects compared with imatinib-treated subjects.
The time to MMR is displayed graphically in Figure 3. The time to MMR was consistently shorter in dasatinib-treated subjects compared with imatinib-treated subjects. MMR rates by specific timepoint are displayed graphically in Figure 4. Rates of MMR were consistently higher in dasatinib-treated subjects compared with imatinib-treated subjects.
MMR rates by specific timepoint are displayed graphically in Figure 4. Rates of MMR were consistently higher in dasatinib-treated subjects compared with imatinib-treated subjects. MR4.5 rates over time are displayed graphically in Figure 5. Rate of MR4.5 over time was consistently higher in dasatinib-treated subjects compared with imatinib-treated subjects.
MR4.5 rates over time are displayed graphically in Figure 5. Rate of MR4.5 over time was consistently higher in dasatinib-treated subjects compared with imatinib-treated subjects. Disease progression was defined as increasing white blood cells despite appropriate therapeutic management, loss of CHR (complete haematological response), partial CyR or CCyR, progression to accelerated phase or blast phase, or death. The estimated 60-month PFS rate was 88.9% (CI: 84.0%-92.4%) and 89.2% (CI: 84.3%-92.7%) for the dasatinib and imatinib treatment groups, respectively. Transformation to accelerated or blast phase occurred less frequently with dasatinib (n = 8; 3.1%) than with imatinib-treated patients (n = 15; 5.8%). The estimated 60-month survival rates for dasatinib and imatinib-treated patients were 90.9% (CI: 86.6%-93.8%) and 89.6% (CI: 85.2%-92.8%), respectively.
Disease progression was defined as increasing white blood cells despite appropriate therapeutic management, loss of CHR (complete haematological response), partial CyR or CCyR, progression to accelerated phase or blast phase, or death. The estimated 60-month PFS rate was 88.9% (CI: 84.0%-92.4%) and 89.2% (CI: 84.3%-92.7%) for the dasatinib and imatinib treatment groups, respectively. Transformation to accelerated or blast phase occurred less frequently with dasatinib (n = 8; 3.1%) than with imatinib-treated patients (n = 15; 5.8%). The estimated 60-month survival rates for dasatinib and imatinib-treated patients were 90.9% (CI: 86.6%-93.8%) and 89.6% (CI: 85.2%-92.8%), respectively. Efficacy was also assessed in patients who were intolerant to imatinib. In this population of patients who received 100 mg once daily, MCyR was achieved in 77% and CCyR in 67% with a minimum of 2 years follow-up.
Efficacy was also assessed in patients who were intolerant to imatinib. In this population of patients who received 100 mg once daily, MCyR was achieved in 77% and CCyR in 67% with a minimum of 2 years follow-up. In the Phase III, randomized, open-label study in patients with advanced phase CML and Ph+ ALL, whose disease was resistant to or who were intolerant to imatinib, the primary endpoint was MaHR. A total of 611 patients were randomized to either the dasatinib 140 mg once daily or 70 mg twice daily group. Median duration of treatment was approximately 6 months (range < 1-31 months).
In the Phase III, randomized, open-label study in patients with advanced phase CML and Ph+ ALL, whose disease was resistant to or who were intolerant to imatinib, the primary endpoint was MaHR. A total of 611 patients were randomized to either the dasatinib 140 mg once daily or 70 mg twice daily group. Median duration of treatment was approximately 6 months (range < 1-31 months). In patients with accelerated phase CML treated with the 140 mg once daily regimen, the median duration of MaHR and the median overall survival in patients with accelerated phase CML was not reached for either group; the median PFS was 25 months and 26 months for the 140 mg once daily group and the 70 mg twice daily group, respectively; and the median overall survival was not reached for the 140 mg once daily group and 31 months for the 70 mg twice daily group.
In patients with accelerated phase CML treated with the 140 mg once daily regimen, the median duration of MaHR and the median overall survival in patients with accelerated phase CML was not reached for either group; the median PFS was 25 months and 26 months for the 140 mg once daily group and the 70 mg twice daily group, respectively; and the median overall survival was not reached for the 140 mg once daily group and 31 months for the 70 mg twice daily group. Chemical Name: N-(2-chloro-6-methylphenyl)-2-[[6-[4-(2-hydroxyethyl)-1-piperazinyl]-2-methyl-4-pyrimidinyl]amino]-5-thiazolecarboxamide.
Chemical Name: N-(2-chloro-6-methylphenyl)-2-[[6-[4-(2-hydroxyethyl)-1-piperazinyl]-2-methyl-4-pyrimidinyl]amino]-5-thiazolecarboxamide.