What is in this leaflet
This leaflet answers some common questions about DBL Fentanyl Injection.
It does not contain all the available information.
It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you being given DBL Fentanyl Injection against the benefits they expect it will have for you.
If you have any concerns about this medicine, ask your doctor or pharmacist.
Keep this leaflet in a safe place. You may need to read it again.
What DBL Fentanyl Injection is used for
Fentanyl is a short-term pain reliever that belongs to a group of medicines called opioid analgesics.
Fentanyl acts in the brain and spinal cord. It works quickly to reduce pain and its effects wear off quickly.
Fentanyl may be used alone but is usually used in hospital with other anaesthetics or with a sedative such as droperidol before an operation to provide an anaesthetic effect and during an operation to help continue the anaesthesia.
Your doctor may have prescribed it for another reason.
Ask your doctor if you have any questions about why this medicine has been prescribed for you.
Fentanyl may produce physical dependence (ie it can be habit-forming or addictive), if used for a long time. Physical dependence means you may experience unpleasant feelings if you stop fentanyl suddenly.
However, it is also important to keep your pain under control. Your doctor can advise you on how to manage this.
This medicine is available only with a doctor’s prescription.
There is not enough information to recommend the use of this medicine for children under the age of 2 years.
Before you are given DBL Fentanyl Injection
When you must not be given it
You should not be given DBL Fentanyl Injection if you have an allergy to fentanyl or any of the ingredients listed at the end of this leaflet.
Symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
You should not be given DBL Fentanyl Injection if:
- you suffer from bronchial asthma or have severe disease relating to the lungs.
- you have breathing difficulties or shallow breathing.
- you are undergoing treatment with monoamine oxidase (MAO) inhibitors (eg phenelzine, tranylcypromine, moclobemide or selegeline) or have stopped MAO inhibitor treatment during the last fourteen days
- you suffer from myasthenia gravis (severe muscle weakness).
- long-standing pain not related to cancer.
DBL Fentanyl Injection should not be given to children under the age of 2 years.
Do not use DBL Fentanyl Injection after the expiry date (EXP) printed on the pack. If this medicine is used after the expiry date has passed it may not work as well.
Do not use DBL Fentanyl Injection if the packaging is torn or shows signs of tampering
If you are not sure whether you should be given this medicine, talk to your doctor or pharmacist.
Before you are given it
Tell your doctor or pharmacist if you have allergies to:
- any other medicines
- any other substances, such as foods, preservatives or dyes.
Tell your doctor or pharmacist if you are pregnant or intend to become pregnant. As fentanyl crosses the placenta, your doctor or pharmacist will discuss the possible risks and benefits of you being given DBL Fentanyl Injection during pregnancy.
Tell your doctor or pharmacist if you are breast-feeding or plan to breastfeed. As fentanyl may pass into breast milk, breastfeeding is not recommended for 24 hours following use of DBL Fentanyl Injection. Your doctor or pharmacist will discuss the possible risks and benefits of being given DBL Fentanyl Injection during breastfeeding.
Tell your doctor or pharmacist if you have or have had any medical conditions, especially the following:
- kidney or liver problems
- lung or breathing problems
- slow or irregular heartbeats; heart problems
- snoring or sleep apnoea (you temporarily stop breathing or have difficulty breathing while asleep).
If you have not told your doctor or pharmacist about any of the above, tell them before you are given DBL Fentanyl Injection.
Addiction
You can become addicted to fentanyl even if you use it exactly as prescribed. Fentanyl may become habit forming causing mental and physical dependence. If abused it may become less able to reduce pain.
Dependence
As with all other opioid containing products, your body may become used to you using fentanyl. Using it may result in physical dependence. Physical dependence means that you may experience withdrawal symptoms if you stop using fentanyl suddenly, so it is important to use it exactly as directed by your doctor.
Tolerance
Tolerance to fentanyl may develop, which means that the effect of the medicine may decrease. If this happens, more may be needed to maintain the same effect.
Withdrawal
Continue using your medicine for as long as your doctor tells you. If you stop having this medicine suddenly, your pain may worsen and you may experience some or all of the following withdrawal symptoms:
- nervousness, restlessness, agitation, trouble sleeping or anxiety
- body aches, weakness or stomach cramps
- loss of appetite, nausea, vomiting or diarrhoea
- increased heart rate, breathing rate or pupil size
- watery eyes, runny nose, chills or yawning
- increased sweating.
DBL Fentanyl Injection given to the mother during labour can cause breathing problems and signs of withdrawal in the newborn.
Taking other medicines
Tell your doctor or pharmacist if you are taking/using any other medicines, including any that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and fentanyl may interfere with each other. These include:
- barbiturates
- general anaesthetics and strong pain killers (e.g. opioid analgesics)
- alcohol
- sedating antipsychotics (e.g. droperidol, chlorpromazine, fluphenazine and thioridazine) and centrally-active anti-emetics (e.g. metoclopramide and promethazine)
- benzodiazepines (and other medicines) to treat anxiety, acute stress reactions, agitation, tremor, such as diazepam (Valium), alprazolam, lorazepam or midazolam
- other medicines which may make you drowsy such as sleeping tablets, tablets to calm your nerves, sedatives, tranquilisers, hypnotics and muscle relaxants
- antidepressants which belong to the group of medicines called Selective Serotonin Re-uptake Inhibitors (SSRI)
- antidepressants which belong to the group of medicines called Serotonin Norepinephrine Re-uptake Inhibitors (SNRI)
- antidepressants which belong to the group of medicines called monoamine oxidase (MAO) inhibitors (i.e. phenelzine, tranylcypromine and moclobemide)
- MAO inhibitor used to treat Parkinson’s disease e.g. selegeline, rasagiline and safinamide.
- medicines to treat mental disorders
- medicines to treat seizures (gabapentinoids e.g. gabapentin, pregabalin)
- medicines which may reduce the effects of fentanyl such as rifampin (anti-tuberculosis medication), carbamazepine and phenytoin, medicines used to control fits or seizures
- medicines which may increase the effects of fentanyl such as macrolide antibiotics (e.g. erythromycin), azole-antifungal agents (e.g. ketoconizole) and protease inhibitors or medication for HIV (e.g. ritonavir).
These medicines may be affected by DBL Fentanyl Injection or may affect how well it works. You may need different amounts of your medicine, or different medicines. Your doctor or pharmacist will advise you.
Your doctor and pharmacist may have more information on medicines to be careful with or avoid while you are being given this medicine.
How DBL Fentanyl Injection is given
How much is given
Your doctor will decide what dose you will receive. This depends on your age, physical condition and other factors, such as your weight.
How it is given
DBL Fentanyl Injection is given as an injection into a vein or a muscle. It must only be given by a doctor or nurse.
If you are given too much (overdose)
DBL Fentanyl Injection is administered under the care of a highly trained doctor so overdose rarely occurs.
However, if you or someone else receive too much (overdose), and experience one or more of the symptoms below, call triple zero (000) for an ambulance. Keep the person awake by talking to them or gently shaking them every now and then. You should follow the above steps even if someone other than you have accidentally used DBL Fentanyl Injection that was prescribed for you.
If someone has an overdose they may experience one or more of the following symptoms:
- slow, unusual or difficult breathing causing skin to turn blue
- severe drowsiness, dizziness or unconsciousness
- slow or weak heartbeat, decreases in heart rate and blood pressure
- nausea or vomiting
- convulsions or fits,
- severe weakness or muscle stiffness
If you think you or someone else may have used too much DBL Fentanyl Injection, you should immediately:
- phone the Poisons Information Centre (by calling 13 11 26), or
- contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
While you are being given DBL Fentanyl Injection
Things you must do
Tell any other doctors, dentists and pharmacists who are treating you that you are being given DBL Fentanyl Injection.
If you are about to be started on any new medicine, tell your doctor, dentist or pharmacist that you are being given DBL Fentanyl Injection.
If you plan to have surgery that needs a local or general anaesthetic, tell your doctor or dentist you are being given DBL Fentanyl Injection.
Things you must not do
Do not give DBL Fentanyl Injection to anyone else, even if they have the same condition as you.
Do not use DBL Fentanyl Injection to treat any other complaints unless your doctor tells you to.
Do not stop using DBL Fentanyl Injection, or lower the dosage, without checking with your doctor or pharmacist.
Do not take any other medicines, whether they are prescription or over-the-counter medicines, unless they have been approved or recommended by a doctor or pharmacist who knows you are being treated with DBL Fentanyl Injection.
Things to be careful of
Feelings of weakness, dizziness, or nausea. Avoid smoking or taking other drugs unless your doctor tells you to.
Be careful driving or operating machinery until you know how DBL Fentanyl Injection affects you.
This medicine may cause drowsiness and impairment of co-ordination, in some people.
Do not drive a car, operate machinery, or do anything else that could be dangerous if you are drowsy or feeling uncoordinated.
Do not drink alcohol, while you are undergoing treatment with fentanyl, unless otherwise advised by your doctor or pharmacist, as drowsiness and co-ordination impairment may be worse.
Tell your doctor, pharmacist or nurse if you have any concerns about being given DBL Fentanyl Injection.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are receiving DBL Fentanyl Injection.
This medicine helps most people but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor or pharmacist if you notice any of the following and they worry you:
- sweating
- dizziness, faintness
- nausea, vomiting.
These are the more common side effects of DBL Fentanyl Injection.
Tell your doctor or pharmacist immediately if you notice any of the following:
- slow or troubled breathing
- muscle stiffness
- a slowed heart rate
- blurred vision
- spasm of the larynx (voice box)
- itching.
These are less common side effects of fentanyl.
The following side effects may occur when a sedating medicine (e.g. droperidol) is used with DBL Fentanyl Injection:
- chills, shivering
- restlessness
- drowsiness
- short periods of depression
- imaginary events
- uncontrolled movement of the body or eyes.
Your doctor will be able to treat you for these symptoms so tell your doctor immediately if you experience any of these symptoms.
If any of the following happen, tell your doctor, pharmacist or nurse immediately, or go to the Accident and Emergency department at your nearest hospital:
- agitation, hallucinations
- slow or troubled breathing
- muscle stiffness, twitching or loss of coordination
- severe dizziness and weakness
- slow, fast or irregular heart rate
- increase or decrease in blood pressure
- skin turning blue and clammy
- unconsciousness.
These are very serious side effects. You may need urgent medical treatment or hospitalisation.
Other side effects not listed may also occur in some patients.
Tell your doctor if you notice anything else that is making you feel unwell.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
Allergic reactions may also occur.
After being given DBL Fentanyl Injection
Tell your doctor immediately if you have unwanted side effects which continue after your treatment has stopped.
Storage
If you are being given DBL Fentanyl Injection while in hospital, it will be stored in the pharmacy or on the ward.
DBL Fentanyl Injection should be stored in a cool, dry place, protected from light where the temperature stays below 25C.
Do not store DBL Fentanyl Injection or any medicine in the bathroom or near a sink. Do not leave it in the car on hot days or on window sills. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor or pharmacist tells you to stop using this medicine or the expiry date has passed, ask your pharmacist what to do with any that is left over.
Product description
What it looks like
DBL Fentanyl Injection is a sterile, aqueous, preservative-free, colourless or almost colourless solution in glass ampoules.
Ingredients
Active ingredient:
- fentanyl citrate
Other ingredients:
- sodium hydroxide
- sodium chloride
- hydrochloric acid
- water for injections.
DBL Fentanyl Injection does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
Sponsor
Pfizer Australia Pty Ltd
Sydney NSW
Toll Free Number : 1800 675 229
www.pfizer.com.au
DBL Fentanyl Injection is available in the following strengths and pack sizes:
- 100 microgram / 2 mL x 5 ampoules AUST R 107025
- 500 microgram / 10 mL x 5 ampoules AUST R 107027.
This leaflet was updated in September 2021.
™ = Trademark
© Copyright
Published by MIMS November 2021



 Additional ADRs that occurred in < 1% of fentanyl injection-treated subjects in the 20 clinical trials are listed in Table 4.
Additional ADRs that occurred in < 1% of fentanyl injection-treated subjects in the 20 clinical trials are listed in Table 4.
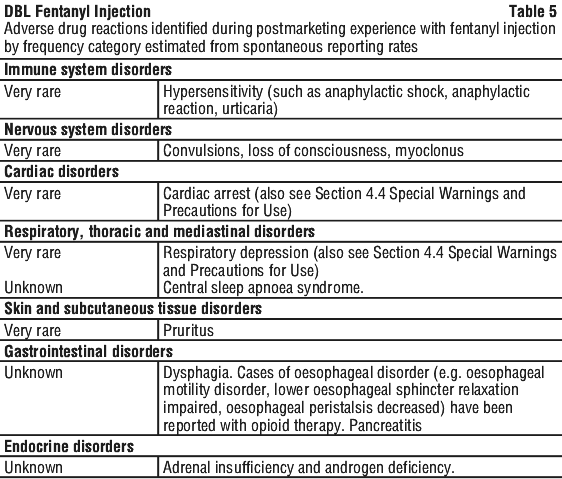 The major adverse reactions associated with fentanyl are respiratory depression, apnoea, muscle rigidity, myoclonic movements and bradycardia, which if untreated, can lead to conditions such as cardiac arrest, circulatory depression and respiratory arrest.
The major adverse reactions associated with fentanyl are respiratory depression, apnoea, muscle rigidity, myoclonic movements and bradycardia, which if untreated, can lead to conditions such as cardiac arrest, circulatory depression and respiratory arrest.
