Notes
Distributed by Medsurge Healthcare Pty Ltd
1 Name of Medicine
Esmolol hydrochloride.
2 Qualitative and Quantitative Composition
Esmolol Hydrochloride Medsurge Injection is supplied as 100 mg/10 mL vial containing 100 mg esmolol hydrochloride.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
100 mg/10 mL vial.
Esmolol Hydrochloride Medsurge Injection is a clear, colourless to light yellow, sterile, nonpyrogenic solution of esmolol hydrochloride for intravenous infusion. The single dose vial has a pH range of 4.5 to 5.5.4.1 Therapeutic Indications
Supraventricular tachycardia.
Esmolol Hydrochloride Medsurge is indicated for the rapid control of ventricular rate in patients with atrial fibrillation or atrial flutter in perioperative, postoperative, or other emergent circumstances where short term control of ventricular rate with a short-acting agent is desirable. Esmolol Hydrochloride Medsurge is also indicated in non-compensatory sinus tachycardia where, in the physician's judgement, the rapid heart rate requires specific intervention. Esmolol Hydrochloride Medsurge is not intended for use in chronic settings where transfer to another agent is anticipated or for treatment periods greater than 24 hours duration.4.2 Dose and Method of Administration
Note.
Parenteral drug products should be inspected visually prior to administration. Any solutions which contain visible particulate matter or are hazy or discoloured should not be used. Product is for single use in one patient only. Discard any residue.
Esmolol Hydrochloride Medsurge is available as a 100 mg/10 mL solution for injection vial. Esmolol hydrochloride powder for injection is available in another brand (for maintenance infusion dosing only). If using the esmolol hydrochloride powder of injection, refer to the specific Product Information for complete dosage and administration instructions.
100 mg/10 mL vial.
This dosage form is prediluted to provide a ready-to-use 10 mg/mL concentration recommended for esmolol hydrochloride intravenous administration. It may be used to administer the appropriate esmolol hydrochloride loading dosage infusions by hand-held syringe while the maintenance infusion is being prepared. Maintenance infusion solutions must have a concentration of 10 mg/mL.
When using the 100 mg vial, a loading dose of 0.5 mg/kg for a 70 kg patient would be 3.5 mL.
Dosage.
Supraventricular tachycardia.
In the treatment of supraventricular tachycardia, responses to esmolol hydrochloride usually (over 95%) occur within the range of 50 to 200 microgram/kg/min (0.05 to 0.2 mg/kg/min). The average effective dosage is approximately 100 microgram/kg/min (0.1 mg/kg/min) although dosages as low as 25 microgram/kg/min (0.025 mg/kg/min) have been adequate in some patients. Dosages as high as 300 microgram/kg/min (0.3 mg/kg/min) have been used, but these provide little added effect and an increased rate of adverse effects, and are not recommended. Dosage of esmolol hydrochloride in supraventricular tachycardia must be individualised by titration in which each step consists of a loading dosage followed by a maintenance dosage.
To initiate treatment of a patient with supraventricular tachycardia, administer a loading infusion of 500 microgram/kg/min (0.5 mg/kg/min) over one minute followed by a 4 minute maintenance infusion of 50 microgram/kg/min (0.05 mg/kg/min). If an adequate therapeutic effect is observed over the five minutes of drug administration, maintain the maintenance infusion dosage with periodic check and adjustments up or down as needed. If an adequate therapeutic effect is not observed, repeat the same loading dosage infusion over one minute and increase the maintenance infusion to 100 microgram/kg/min (0.1 mg/kg/min).
Continue titration procedure as above, repeating the original loading dose of 500 microgram/kg/min (0.5 mg/kg/min) over 1 minute, and further increasing the maintenance infusion rate over the subsequent four minutes by 50 microgram/kg/min (0.05 mg/kg/min) increments. As the desired heart rate or blood pressure is approached reduce the maintenance infusion rate downward as appropriate. If desired, increase the interval between steps from 5-10 minutes. Maintenance dosages above 200 microgram/kg/min (0.2 mg/kg/min) have not been shown to have significantly increased benefits and are not recommended. The interval between titration steps may be increased.
The safety of maintenance dosages above 300 microgram/kg/min (0.3 mg/kg/min) has not been studied.
This specific dosage and administration regimen has not been studied intraoperatively and, because of the time required for titration, may not be optimal for intraoperative use.
In the event of an adverse reaction, esmolol hydrochloride should be discontinued. If benefits outweigh risks, esmolol hydrochloride may be resumed at a lower infusion rate without a loading dose after the condition has subsided. If a local infusion site reaction develops, an alternative infusion site should be used and caution should be taken to prevent extravasation. The use of butterfly needles should be avoided.
Abrupt cessation of esmolol hydrochloride in patients has not been reported to produce the withdrawal effects which may occur with abrupt withdrawal of beta-blockers following chronic use in coronary artery disease (CAD) patients. However, caution should still be used in abruptly discontinuing infusions of esmolol hydrochloride in CAD patients.
After achieving an adequate control of the heart rate and a stable clinical status in patients with supraventricular tachycardia, transition to alternative antiarrhythmic agents, such as propranolol, or digoxin, may be accomplished. A recommended guideline for such a transition is given in Table 1 but the physician should carefully consider the labelling instructions for the alternative agent selected.
 The dosage of esmolol hydrochloride should be reduced as follows:
The dosage of esmolol hydrochloride should be reduced as follows:
1. Thirty minutes following the first dose of the alternative agent, reduce the infusion rate of esmolol hydrochloride by one-half (50%).
2. Following the second dose of the alternative agent, monitor the patient's response and, if satisfactory control is maintained for the first hour, discontinue esmolol hydrochloride.
The use of infusions of esmolol hydrochloride up to 24 hours duration has been well documented.
Compatibility with commonly used intravenous fluids.
100 mg/10 mL vial.
Esmolol hydrochloride 100 mg/10 mL solution for injection was tested for compatibility with eight commonly used intravenous fluids at a final concentration of 10 mg esmolol hydrochloride per mL. Esmolol hydrochloride was found to be physically and chemically compatible with the solutions listed below for at least 24 hours when stored below 25°C or under refrigeration. However, in order to reduce microbial contamination hazards, infusion should be commenced as soon as practicable after preparation of the admixture. The resulting solutions should be used within 24 hours of preparation and any residue discarded.
Glucose (5%) Injection USP.
Glucose (5%) in Ringer's Injection.
Glucose (5%) in Lactated Ringer's Injection.
Glucose (5%) and Sodium Chloride (0.45%) Injection USP.
Glucose (5%) and Sodium Chloride (0.9%) Injection USP.
Lactated Ringer's Injection USP.
Sodium Chloride (0.45%) Injection USP.
Sodium Chloride (0.9%) Injection USP.4.3 Contraindications
Patients with hypersensitivity to esmolol hydrochloride or any of the excipients should not be given Esmolol Hydrochloride Medsurge.
Esmolol hydrochloride is contraindicated in patients with sinus bradycardia, heart block greater than first degree, cardiogenic shock or overt heart failure (see Section 4.4 Special Warnings and Precautions for Use). Esmolol hydrochloride is also contraindicated in patients with severe bradycardia (less than 50 beats per minute), sick sinus syndrome, severe AV-nodal conductance disorders (without pacemaker), second and third degree AV-block, severe hypotension, non-treated phaeochromocytoma, pulmonary hypertension, acute asthma attack and metabolic acidosis.
Esmolol hydrochloride is contraindicated in patients who require inotropic agents and/or vasopressors to maintain systemic blood pressure and cardiac output. The use of intravenous calcium channel antagonist agents with a beta-blocker may cause severe depression of myocardial function. Esmolol hydrochloride should not be administered concomitantly with IV verapamil or within close proximity since fatal cardiac arrest has occurred in patients receiving both drugs. (The half-life of esmolol hydrochloride is approximately 9 minutes with a range of 5-23 minutes. In normal patients the elimination half-life of IV verapamil is 2-5 hours.)
4.4 Special Warnings and Precautions for Use
Hypotension.
In clinical trials 20-50% of patients treated with esmolol hydrochloride have had hypotension, generally defined as systolic pressure less than 90 mmHg and/or diastolic pressure less than 50 mmHg. About 12% of the patients have been symptomatic (mainly sweating or dizziness). Hypotension can occur at any dose but is dose-related so that maintenance doses beyond 200 microgram/kg/min (0.2 mg/kg/min) are not recommended. Patients should be closely monitored, especially if pre-treatment blood pressure is low. Decrease of dose or termination of infusion reverses hypotension, usually within 30 minutes. It is advised to continuously monitor the blood pressure and ECG in all patients treated with esmolol hydrochloride.
Cardiac failure.
Sympathetic stimulation is necessary in supporting circulatory function in congestive heart failure and beta-blockade carries the potential hazard of further depressing myocardial contractility and precipitating more severe failure. Continued depression of the myocardium with beta-blocking agents over a period of time can, in some cases, lead to cardiac failure. At the first sign or symptom of impending cardiac failure esmolol hydrochloride should be withdrawn. Although withdrawal may be sufficient because of the short elimination half-life of esmolol hydrochloride, specific treatment may also be considered. (See Section 4.9 Overdose.)
The use of esmolol hydrochloride for control of ventricular response in patients with supraventricular arrhythmias should be undertaken with caution when the patient is compromised haemodynamically or is taking other drugs that decrease any or all of the following: peripheral resistance, myocardial filling, myocardial contractility or electrical impulse propagation in the myocardium. Despite the rapid onset and offset of the effects of esmolol hydrochloride, several cases of death have been reported in complex clinical states where esmolol hydrochloride was presumably being used to control ventricular rate.
Esmolol hydrochloride should not be used to slow the heart rate in the presence of agents which are both inotropic and vasoconstrictive such as dopamine, adrenaline (epinephrine) and noradrenaline (norepinephrine) because of the danger of blocking contractility when systemic vascular resistance is high.
Beta-blockers.
Due to its negative effect on conduction time, beta-blockers should only be given with caution to patients with first degree heart block. The elderly should be treated with caution, starting with a lower dosage, but tolerance is usually good in the elderly.
Beta-blockers may increase the number and the duration of anginal attacks in patients with Prinzmetal's angina due to unopposed alpha-receptor mediated coronary artery vasoconstriction. Non-selective beta-blockers should not be used for these patients and beta1-selective blockers only with the utmost care.
If the patient is already on a beta2-receptor stimulating agent, re-evaluate the dose of esmolol hydrochloride.
In patients with peripheral circulatory disorders (Raynaud's disease or syndrome, intermittent claudication), beta-blockers should be used with great caution as aggravation of these disorders may occur.
Beta-blockers may induce bradycardia. If the pulse rate decreases to less than 50-55 beats per minute at rest and the patient experiences symptoms related to bradycardia, the dosage should be reduced.
Anaphylactic reaction.
While taking beta-blockers, patients with a history of severe anaphylactic reaction to a variety of allergens may be more reactive to repeated challenge, either accidental, diagnostic or therapeutic. Such patients may be unresponsive to the usual doses of adrenaline (epinephrine) used to treat the allergic reaction.
Bronchospastic diseases.
Patients with bronchospastic diseases should, in general, not receive beta-blockers.
Because of its relative beta1-selectivity and titratability, esmolol hydrochloride may be used with caution in patients with bronchospastic diseases. However, since beta1-selectivity is not absolute, esmolol hydrochloride should be carefully titrated to obtain the lowest possible effective dose. In the event of bronchospasm, the infusion should be terminated immediately; a beta2-stimulating agent may be administered if conditions warrant but should be used with particular caution as patients already have rapid ventricular rates.
Esmolol hydrochloride should be used with caution in patients with a history of wheezing or asthma.
Diabetes mellitus and hypoglycaemia.
Esmolol hydrochloride should be used with caution in diabetic patients requiring a beta-blocking agent. Beta-blockers may mask tachycardia occurring with hypoglycaemia, but other manifestations such as dizziness and sweating may not be significantly affected.
Psoriasis.
In patients with psoriasis or a history of psoriasis, the administration of esmolol hydrochloride should be carefully weighed.
Infusion concentrations of 20 mg/mL were associated with more venous irritation, including thrombophlebitis, than concentrations of 10 mg/mL. Concentrations greater than 10 mg/mL or infusion into small veins or through a butterfly catheter should be avoided. Extravasation may lead to a serious local reaction and possible skin necrosis. Care should be taken in the intravenous administration of esmolol hydrochloride as sloughing of the skin and necrosis have been reported in association with infiltration and extravasation of intravenous infusions.
Use in renal impairment.
Because the acid metabolite of esmolol hydrochloride is primarily excreted unchanged by the kidney, esmolol hydrochloride should be administered with caution to patients with impaired renal function. The elimination half-life of the acid metabolite was prolonged ten-fold and the plasma level was considerably elevated in patients with end-stage renal disease.
In all patients, it is advised to terminate the infusion of esmolol hydrochloride gradually because of the risk of rebound tachycardia.
Use in the elderly.
See Section 4.4 Special Warnings and Precautions for Use, Beta-blockers.
Paediatric use.
The safety and effectiveness of esmolol hydrochloride in children (under 18 years) has not been established.
Effects on laboratory tests.
No data available.4.5 Interactions with Other Medicines and Other Forms of Interactions
Also see Section 6.2 Incompatibilities.
Calcium antagonists such as verapamil and to a lesser extent diltiazem, have a negative influence on contractility and AV-conduction. As with other beta-blocking agents esmolol hydrochloride should be used with caution in combination with verapamil in patients with impaired ventricular function. Fatal cardiac arrests have occurred in patients receiving both drugs. Both esmolol hydrochloride and verapamil decrease myocardial contractility and atrioventricular conduction. Serious adverse events with this combination are more likely to occur in patients with severe cardiac myopathy, congestive heart failure or recent myocardial infarction (see Section 4.3 Contraindications). The combination should not be given to patients with conduction abnormalities and esmolol hydrochloride should not be administered within 48 hours of discontinuing verapamil.
Calcium antagonists such as dihydropyridine derivatives (e.g. nifedipine and amlodipine) may increase the risk of hypotension. In patients with cardiac insufficiency and who are being treated with a calcium antagonist, treatment with beta-blocking agents may lead to cardiac failure. Careful titration of esmolol hydrochloride and appropriate haemodynamic monitoring is recommended.
Esmolol hydrochloride should not be used to slow the heart rate in the presence of agents which are both inotropic and vasoconstrictive such as dopamine, adrenaline (epinephrine) and noradrenaline (norepinephrine) because of the danger of blocking contractility when systemic vascular resistance is high (see Section 4.4 Special Warnings and Precautions for Use).
Concomitant use of esmolol hydrochloride and class I antiarrhythmic agents (such as disopyramide and quinidine) and also amiodarone can increase the action of both on the AV-conductance time and induce negative inotropic effect.
Sympathomimetic agents may counteract the effect of beta-adrenergic blocking agents.
Catecholamine-depleting drugs, e.g. reserpine, may have an additive effect when given with beta-blocking agents. Patients treated concurrently with esmolol hydrochloride and a catecholamine depletor should therefore be closely observed for evidence of hypotension or marked bradycardia, which may result in vertigo, syncope, or postural hypotension.
A study of interaction between esmolol hydrochloride and warfarin showed that concomitant administration of esmolol hydrochloride and warfarin does not alter warfarin plasma levels. esmolol hydrochloride concentrations were equivocally higher when given with warfarin, but this is not likely to be clinically important.
When digoxin and esmolol hydrochloride were concomitantly administered intravenously to normal volunteers, there was a 10-20% increase in digoxin blood levels at some time points. The combination of digitalis glycosides and esmolol hydrochloride may increase AV-conduction time. Digoxin did not affect esmolol hydrochloride pharmacokinetics.
Concomitant use of clonidine and beta-blockers increases the risk of "rebound hypertension". When clonidine is used in conjunction with non-selective beta-blockers, such as propranolol, treatment with clonidine should be continued for some time after treatment with the beta-blocker has been discontinued.
When intravenous morphine and esmolol hydrochloride were concomitantly administered in normal subjects, no effect on morphine blood levels was seen, but esmolol hydrochloride steady-state blood levels were increased by 46% in the presence of morphine. No other pharmacokinetic parameters were changed.
The effect of esmolol hydrochloride on the duration of suxamethonium-induced neuromuscular blockade was studied in patients undergoing surgery. The onset of neuromuscular blockade by suxamethonium was unaffected by esmolol hydrochloride, but the duration of neuromuscular blockade was prolonged from 5 minutes to 8 minutes.
Although the interactions observed in these studies do not appear to be of major clinical importance, esmolol hydrochloride should be titrated with caution in patients being treated concurrently with digoxin, morphine, suxamethonium or warfarin.
Concomitant use of esmolol hydrochloride and insulin and oral antidiabetic drugs may intensify the blood sugar lowering effect (especially non-selective beta-blockers). Beta-adrenergic blockade may prevent the appearance of signs of hypoglycemia (tachycardia).
Anaesthetic medicines: In the situation where the patient's volume status is uncertain or concomitant antihypertensive drugs are utilized, there may be attenuation of reflex tachycardia and an increase of the risk of hypotension. Continuation of beta-blockade reduces the risk of arrhythmia during induction and intubation. The anaesthesiologist should be informed when the patient is receiving a beta-blocking agent in addition to esmolol hydrochloride.
The hypotensive effects of inhalation anaesthetic agents may be increased in the presence of esmolol hydrochloride. The dosage of either agent may be modified, as needed, to maintain the desired haemodynamics.
NSAIDs may decrease the hypotensive effects of beta-blockers.
Concomitant administration of tricyclic antidepressants, barbiturates and phenothiazines as well as other antihypertensive agents may increase the blood pressure lowering effect. Dosing of esmolol hydrochloride should be adjusted downward to avoid unexpected hypotension.
Special caution must be taken when using amisulpride concomitantly with beta-blockers.
The combination of esmolol hydrochloride with ganglion blocking agents can enhance the hypotensive effect.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
Because of its short term usage no carcinogenicity, mutagenicity or reproductive performance studies have been conducted with esmolol hydrochloride.
(Category C)
There are no adequate and well controlled studies in pregnant women. Beta-adrenergic blocking agents may cause pharmacological effects such as bradycardia in the foetus and newborn infant.
It is not known whether esmolol hydrochloride is excreted in human milk. Lactation is not advised during the use of esmolol hydrochloride.4.7 Effects on Ability to Drive and Use Machines
No specific studies have been conducted to assess the direct effect of esmolol hydrochloride on the ability to drive and use machines. However, adverse effects of esmolol hydrochloride include dizziness which could affect the ability to drive or use machines. See Section 4.8 Adverse Effects (Undesirable Effects).
4.8 Adverse Effects (Undesirable Effects)
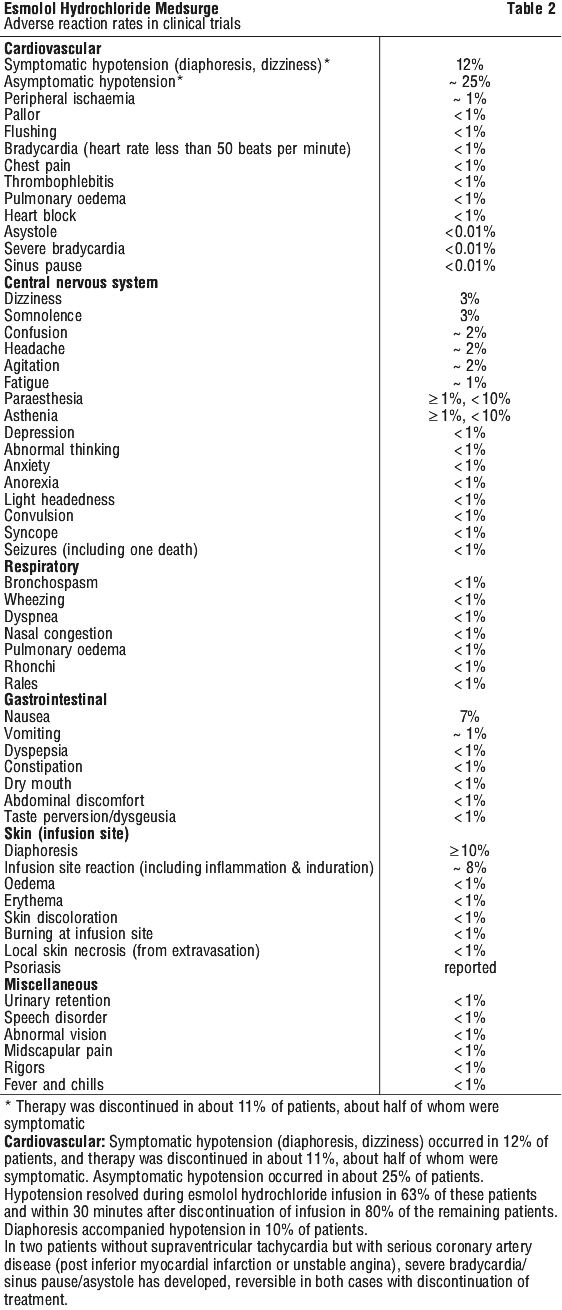
The adverse reaction rates provided in Table 2 are based on use of esmolol hydrochloride in clinical trials involving 369 patients with supraventricular tachycardia and over 600 intraoperative and postoperative patients enrolled in clinical trials. Most adverse effects observed in controlled clinical trial settings have been mild and transient. The most important adverse effect has been hypotension (see Section 4.4 Special Warnings and Precautions for Use). Deaths have been reported in postmarketing experience occurring during complex clinical states where esmolol hydrochloride was presumably being used simply to control ventricular rate (see Section 4.4 Special Warnings and Precautions for Use, Cardiac failure).
 The following experiences are based on spontaneous adverse event reports. Data are insufficient to establish an estimate of their incidence or to establish causation. Some of these events may occur as part of the underlying illness.
The following experiences are based on spontaneous adverse event reports. Data are insufficient to establish an estimate of their incidence or to establish causation. Some of these events may occur as part of the underlying illness.
Cardiovascular.
Death, cardiac arrest, hypertension, ventricular tachycardia and idioventricular rhythm.
Dermatological reactions.
Discolouration, blistering, rash, facial flushing and skin dryness.
Neurological.
Cerebral hypoxia, anoxic encephalopathy, aphasia, coma, dysphagia, lethargy, somnolence and prolonged response to neuromuscular blockage.
Haematological.
Leucopenia, thrombocytopenia.
Respiratory.
Apnoea, hypoxia, respiratory arrest, pneumonia.
Renal.
Renal failure, metabolic acidosis.
Esmolol hydrochloride can cause psoriasis in some situations or worsen it or cause rash in similar skin disorders.
In case of undesirable effects, the infusion of esmolol hydrochloride shall be reduced or interrupted. Most of these undesirable effects disappear within 30 minutes after discontinuation of the administration of esmolol hydrochloride.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at http://www.tga.gov.au/reporting-problems.4.9 Overdose
Acute toxicity.
Overdoses of esmolol hydrochloride can cause cardiac arrest. In addition, overdoses can produce bradycardia, hypotension, electro-mechanical dissociation and loss of consciousness. Cases of massive accidental overdoses of esmolol hydrochloride have occurred due to dilution errors. Some of these overdoses have been fatal while others resulted in permanent disability. Bolus doses in the range of 625 to 2500 mg (12.5-50 mg/kg) have been fatal. Patients have recovered completely from overdoses as high as 1.75 g given over one minute or doses of 7.5 g given over one hour for cardiovascular surgery. The patients who survived appear to be those whose circulation could be supported until the effects of esmolol hydrochloride resolved.
Because of its approximately 9-minute elimination half-life, the first step in the event of toxicity should be to discontinue the esmolol hydrochloride infusion. Then, based on the observed clinical effects, the following general measures should also be considered.
Bradycardia.
Intravenous administration of atropine or another anticholinergic drug.
Bronchospasm.
Nebulised beta2-stimulating agent should be given. If this is not sufficient, intravenous administration of a beta2-stimulating agent and/or a theophylline derivative can be considered.
Cardiac failure.
Intravenous administration of a diuretic and/or digitalis glycoside. In shock resulting from inadequate cardiac contractility, intravenous administration of dopamine, dobutamine or isoprenaline may be considered. In case further treatment is necessary, the following agents can be given intravenously: atropine, inotropic agents, calcium ions.
Symptomatic hypotension.
Intravenous administration of fluids and/or pressor agents.
For information on the management of overdose, contact the Poisons Information Centre on 131126 (Australia).5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Esmolol hydrochloride is a beta1-selective (cardioselective) adrenergic blocking agent with rapid onset and a short duration of action (elimination half-life is approximately 9 minutes).
Mechanism of action.
Esmolol hydrochloride is a beta1-selective (cardioselective) adrenergic receptor blocking agent with rapid onset, a very short duration of action and no significant intrinsic sympathomimetic or membrane stabilising activity at therapeutic dosages. Its elimination half-life after intravenous infusion is approximately 9 minutes. Esmolol hydrochloride inhibits the beta1-receptors located chiefly in cardiac muscle, but this preferential effect is not absolute and at higher doses it begins to inhibit beta2-receptors located chiefly in the bronchial and vascular musculature.
Pharmacodynamics.
Clinical pharmacology studies in normal volunteers have confirmed the beta-blocking activity of esmolol hydrochloride, showing reduction in heart rate at rest and during exercise, and attenuation of isoprenaline-induced increases in heart rate. Blood levels of esmolol hydrochloride have been shown to correlate with extent of beta-blockade. After termination of infusion, substantial recovery from beta-blockade is observed in 10-20 minutes.
In human electro-physiology studies, esmolol hydrochloride produced effects typical of a beta-blocker: a decrease in the heart rate, increase in sinus cycle length, prolongation of the sinus node recovery time, prolongation of the AH interval during normal sinus rhythm and during atrial pacing, and an increase in antegrade Wenckebach cycle length.
In patients undergoing radionuclide angiography, esmolol hydrochloride at dosages of 200 microgram/kg/min (0.2 mg/kg/min) produced reductions in heart rate, systolic blood pressure, rate pressure product, left and right ventricular ejection fraction and cardiac index at rest, which were similar in magnitude to those produced by intravenous propranolol (4 mg). During exercise, esmolol hydrochloride produced reductions in heart rate, rate pressure product and cardiac index which were also similar to those produced by propranolol, but produced a significantly larger fall in systolic blood pressure. In patients undergoing cardiac catheterisation, the maximum therapeutic dose of 300 microgram/kg/min (0.3 mg/kg/min) of esmolol hydrochloride produced similar effects and, in addition, there were small, clinically insignificant increases in the left ventricular end diastolic pressure and pulmonary capillary wedge pressure. At thirty minutes after the discontinuation of esmolol hydrochloride infusion, all the haemodynamic parameters had returned to pre-treatment levels.
The relative cardioselectivity of esmolol hydrochloride was demonstrated in 10 mildly asthmatic patients. Infusions of esmolol hydrochloride [100, 200 and 300 microgram/kg/min (0.1, 0.2 and 0.3 mg/kg/min)] produced no significant increases in specific airway resistance compared to placebo. At 300 microgram/kg/min (0.3 mg/kg/min), esmolol hydrochloride produced slightly enhanced bronchomotor sensitivity to dry air stimulus. These effects were not clinically significant and esmolol hydrochloride was well tolerated by all patients. Six of the patients also received intravenous propranolol and, at a dosage of 1 mg, two experienced significant, symptomatic bronchospasm requiring bronchodilator treatment.
One other propranolol-treated patient also experienced dry air-induced bronchospasm. No adverse pulmonary effects were observed in patients with chronic obstructive pulmonary disease who received therapeutic dosages of esmolol hydrochloride for treatment of supraventricular tachycardia (51 patients) or in perioperative settings (32 patients).
Clinical trials.
No data available.
5.2 Pharmacokinetic Properties
Absorption.
No data available.
Distribution.
Esmolol hydrochloride has been shown to be 55% bound to human plasma protein, while the acid metabolite is only 10% bound.
Metabolism.
Esmolol hydrochloride is rapidly metabolised by hydrolysis of the ester linkage, chiefly by the esterases in the cytosol of red blood cells and not by plasma cholinesterases or red cell membrane acetylcholinesterase. Total body clearance in man was found to be about 20 L/kg/hr, which is greater than cardiac output; thus the metabolism of esmolol hydrochloride is not limited by the rate of blood flow to metabolising tissues such as the liver, or affected by hepatic or renal blood flow. Esmolol hydrochloride has a rapid distribution half-life of about 2 minutes and an elimination half-life of about 9 minutes. Using an appropriate loading dose, steady-state blood levels of esmolol hydrochloride for dosages from 50-300 microgram/kg/min (0.05-0.3 mg/kg/min) are obtained within five minutes. (Steady-state is reached in about 30 minutes without the loading dose.) Steady-state blood levels of esmolol hydrochloride increase linearly over this dosage range and elimination kinetics are dose independent over this range. Steady-state blood levels are maintained during infusion but decrease rapidly after termination of the infusion. Because of its short half-life, blood levels of esmolol hydrochloride can be rapidly altered by increasing or decreasing the infusion rate and rapidly eliminated by discontinuing the infusion.
Excretion.
Consistent with the high rate of blood-based metabolism of esmolol hydrochloride, less than 2% of the drug is excreted unchanged in the urine. Within 24 hours of the end of infusion, approximately 73-88% of the dosage has been accounted for in the urine as the acid metabolite of esmolol hydrochloride.
Metabolism of esmolol hydrochloride results in the formation of the corresponding free acid and methanol. The acid metabolite has been shown in animals to have about 1/1,500 of the activity of esmolol hydrochloride and in normal volunteers its blood levels do not correspond to the level of beta-blockade. The acid metabolite has an elimination half-life of about 3.7 hours and is excreted in the urine with a clearance approximately equivalent to the glomerular filtration rate. Excretion of the acid metabolite is significantly decreased in patients with renal disease, with the elimination half-life increased to about ten-fold that of normal and plasma levels considerably elevated. Methanol blood levels, monitored in subjects receiving esmolol hydrochloride for up to 6 hours at 300 microgram/kg/min (0.3 mg/kg/min) and 24 hours at 150 microgram/kg/min (0.15 mg/kg/min), approximated endogenous levels and were less than 2% of levels usually associated with methanol toxicity.
5.3 Preclinical Safety Data
Genotoxicity.
Because of its short term usage no carcinogenicity, mutagenicity or reproductive performance studies have been conducted with esmolol hydrochloride.
Carcinogenicity.
Because of its short term usage no carcinogenicity, mutagenicity or reproductive performance studies have been conducted with esmolol hydrochloride.6 Pharmaceutical Particulars
6.1 List of Excipients
Sodium chloride, sodium acetate trihydrate, glacial acetic acid, sodium hydroxide/ hydrochloric acid as pH adjustors, water for injections.
6.2 Incompatibilities
Esmolol Hydrochloride Medsurge must not be used in combination with sodium carbonate solutions or other medicinal products (e.g. furosemide, diazepam and thiopental) that are chemically incompatible with esmolol hydrochloride.
Esmolol hydrochloride is not compatible with Sodium Bicarbonate (5%) Injection USP. Please see Section 4.2 Dose and Method of Administration for list of compatible diluents.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG).
The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
100 mg/10 mL Type I amber glass vials are supplied in a carton containing 5, 20 or 25 vials.
The vial stopper is not made with natural rubber latex.
Not all pack sizes may be marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Esmolol hydrochloride is ± methyl 3-[4-[2-hydroxy- 3-(isopropylamino) propoxy]phenyl] propionate hydrochloride. Esmolol hydrochloride has the empirical formula C16H25NO4.HCl and a molecular weight of 331.8. It has one asymmetric centre and exists as a racemic mixture. It is a relatively hydrophilic compound which is very soluble in water and freely soluble in alcohol. Its partition coefficient (octanol/water) at pH 7.0 is 0.42 compared to 17.0 for propranolol.
Chemical structure.

CAS number.
81161-17-3.7 Medicine Schedule (Poisons Standard)
Prescription only medicine (Schedule 4).
Summary Table of Changes


 The dosage of esmolol hydrochloride should be reduced as follows:
The dosage of esmolol hydrochloride should be reduced as follows: The following experiences are based on spontaneous adverse event reports. Data are insufficient to establish an estimate of their incidence or to establish causation. Some of these events may occur as part of the underlying illness.
The following experiences are based on spontaneous adverse event reports. Data are insufficient to establish an estimate of their incidence or to establish causation. Some of these events may occur as part of the underlying illness.
