1 Name of Medicine
Fluvoxamine maleate.
2 Qualitative and Quantitative Composition
Each tablet contains 50 mg or 100 mg fluvoxamine maleate.
For the full list of excipients see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Fluvoxamine-WGR tablets 50 mg.
Golden, round, scored, film-coated tablets engraved APO on one side, "F" over bisect "50" on the other side.
Fluvoxamine-WGR tablets 100 mg.
Reddish-brown, pillow shaped, scored, film-coated tablet engraved APO on one side, FLU bisect 100 on the other side.4.1 Therapeutic Indications
The treatment of major depression in adults.
The treatment of Obsessive Compulsive Disorder (OCD) in children aged 8 years of age and older, adolescents, and adults.
4.2 Dose and Method of Administration
Fluvoxamine-WGR tablets are intended for oral administration.
Dosage.
Depression. The recommended starting dose of fluvoxamine is 50 mg per day for one week, given as a single dose in the evening. Doses should be gradually increased (by 50 mg per week) until an effective dose is reached, with a maximum of 300 mg per day (the usually effective dose is 100 mg/day). Doses up to 150 mg can be given as a single dose. It is recommended that total daily doses of greater than 150 mg be given in 2 or 3 divided doses.
If no improvement is observed within 6 weeks of initiation of therapy, treatment with fluvoxamine should be reconsidered. It is important to ascertain that an adequate therapeutic dose has been maintained throughout this period.
In agreement with the consensus statement of the WHO, antidepressant medication should be continued for at least 6 months after recovery from a depressive episode.
Obsessive compulsive disorder. Adults.
The recommended starting dose of fluvoxamine is 50 mg per day for 3 to 4 days. The dosage should be increased gradually (i.e. by 50 mg every 4 to 6 days) until an effective dose is achieved, with a maximum of 300 mg per day. (The usually effective dose is in the range of 100-300 mg/day.) Doses up to 150 mg per day can be given as a single dose, preferably in the evening. It is recommended that a total daily dose of more than 150 mg is given in 2 or 3 divided doses.
Children and adolescents (8-17 years).
The recommended starting dose of fluvoxamine in paediatric populations (ages 8-17 years) is 25 mg administered as a single daily dose at bedtime. In a controlled clinical trial establishing the effectiveness of fluvoxamine in OCD, paediatric patients (ages 8-17) were titrated within a dose range of 50 to 200 mg/day. The dose should be increased in 25 mg increments every 4 to 7 days, as tolerated, until maximum therapeutic benefit is achieved. Physicians should consider age and gender differences when dosing paediatric patients. The maximum dose should not exceed 200 mg/day. Therapeutic effect in female children may be achieved with lower doses. It is advisable that a total daily dose of more than 50 mg should be given in two divided doses. If the two divided doses are not equal, the larger dose should be given at bedtime.
If a good therapeutic response is achieved, treatment can be continued at the required dosage. There are no systematic studies which address the issue of the length of treatment. However, since obsessive compulsive disorder (OCD) is a chronic condition, it is reasonable to consider continuation beyond 10 weeks in responding patients. Data from the long-term (up to two years) open-extension phase of the placebo-controlled study in children supports sustained efficacy of the medicine. Dosage adjustments should be made carefully, on an individual patient basis, throughout therapy to maintain the patient at the lowest effective dose. The need for treatment should be reassessed periodically.
Some clinicians advocate concomitant behavioural psychotherapy in conjunction with pharmacotherapy.
If no improvement is observed within 10 weeks of initiation of therapy, treatment with fluvoxamine should be reconsidered. It is important to ascertain that an adequate therapeutic dose has been maintained throughout this period.
Administration.
The tablets should be swallowed with water, without chewing.
Withdrawal symptoms seen on discontinuation of fluvoxamine.
Abrupt discontinuation should be avoided. When stopping treatment with fluvoxamine, the dose should be gradually reduced over a period of at least one or two weeks in order to reduce the risk of withdrawal reactions (see Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects)). If intolerable symptoms occur following a decrease in the dose or upon discontinuation of treatment, then resuming the previously prescribed dose may be considered. Subsequently, the physician may continue decreasing the dose, but at a more gradual rate.4.3 Contraindications
Fluvoxamine is contraindicated in combination with tizanidine.
Fluvoxamine should not be used in combination with monoamine oxidase inhibitors (MAOIs) or the reversible MAOI (RIMA), moclobemide, or linezolid within 14 days of discontinuing treatment with a MAOI. Similarly, at least one week should be allowed after stopping fluvoxamine before starting a MAOI. Cases of serious reactions, such as potentially lifethreatening serotonin syndrome (characterised by neuromuscular excitation, altered mental status and autonomic dysfunction) have been reported in patients receiving an SSRI in combination with MAOIs and RIMA, and in patients who have recently discontinued an SSRI and have started on a MAOI (also see Section 4.4 Special Warnings and Precautions for Use).
Fluvoxamine tablets should not be used in combination with pimozide and ramelteon (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Fluvoxamine is contraindicated in combination with cisapride.
Fluvoxamine tablets are contraindicated in patients with hypersensitivity to any component of the product (see Section 6.1 List of Excipients).
Fluvoxamine has been shown to increase postnatal mortality in rats at doses greater than 1 mg/kg/day, and should not be used by nursing mothers.
4.4 Special Warnings and Precautions for Use
Bipolar disorder.
A major depressive episode may be the initial presentation of bipolar disorder. It is generally believed that treating such an episode with an antidepressant alone may increase the likelihood of precipitation of a mixed/manic episode in patients at risk of bipolar disorder. Prior to initiating treatment with an antidepressant, patients should be adequately screened to determine if they are a risk for bipolar disorder; such screening should include a detailed psychiatric history, including a family history of suicide, bipolar disorder and depression.
Clinical worsening and suicide risk associated with psychiatric disorders.
The risk of suicide attempt is inherent in depression and may persist until significant remission occurs. This risk must be considered in all depressed patients.
Patients with depression may experience worsening of their depressive symptoms and/or the emergence of suicidal ideation and behaviours (suicidality) whether or not they are taking antidepressant medications, and this risk may persist until significant remission occurs. As improvement may not occur during the first few weeks or more of treatment, patients should be closely monitored for clinical worsening and suicidality, especially at the beginning of a course of treatment, or at the time of dose changes, either increases or decreases. Consideration should be given to changing the therapeutic regimen, including possibly discontinuing the medication, in patients whose depression is persistently worse or whose emergent suicidality is severe, abrupt in onset, or was not part of the patient's presenting symptoms.
Patients (and caregivers of patients) should be alerted about the need to monitor for any worsening of their condition and/or the emergence of suicidal ideation/ behaviour or thoughts of harming themselves and to seek medical advice immediately if these symptoms present. Patients with co-morbid depression associated with other psychiatric disorders being treated with antidepressants should be similarly observed for clinical worsening and suicidality.
Obsessive compulsive disorders may also be associated with an increased risk of suicide related events. The same precautions should therefore be observed for these patients.
Patients with a history of suicide-related events, or those exhibiting a significant degree of suicidal ideation prior to commencement of treatment, are at a greater risk of suicidal thoughts or suicide attempts, and should receive careful monitoring during treatment.
Pooled analyses of 24 short-term (4 to 16 weeks), placebo-controlled trials of nine antidepressant medicines (SSRIs and others) in 4400 children and adolescents with major depressive disorder (16 trials), obsessive compulsive disorder (4 trials), or other psychiatric disorders (4 trials) have revealed a greater risk of adverse events representing suicidal behaviour or thinking (suicidality) during the first few months of treatment in those receiving antidepressants. The average risk of such events in patients treated with an antidepressant was 4%, compared with 2% of patients given placebo. There was considerable variation in risk among the antidepressants, but there was a tendency towards an increase for almost all antidepressants studied. The risk of suicidality was most consistently observed in the major depressive disorder trials, but there were signals of risk arising from trials in other psychiatric indications (obsessive compulsive disorder and social anxiety disorder) as well. No suicides occurred in these trials. It is unknown whether the suicidality risk in children and adolescent patients extends to use beyond several months. The nine antidepressant medicines in the pooled analyses included five SSRIs (citalopram, fluoxetine, fluvoxamine, paroxetine, sertraline) and four non-SSRIs (bupropion, mirtazapine, nefazodone, venlafaxine).
Pooled analysis of short term studies of antidepressant medications have also shown an increased risk of suicidality in young adults aged 18 to 24 during initial treatment (generally the first one to two months). Short term studies did not show an increase in the risk of suicidality with antidepressants compared to placebo in adults beyond the age of 24 years; there was a reduction with antidepressants compared to placebo in adults aged 65 years and older.
Symptoms of anxiety, agitation, panic attacks, insomnia, irritability, hostility (aggressiveness), impulsivity, akathisia (psychomotor restlessness), hypomania, and mania, have been reported in adults, adolescents and children being treated with antidepressants for major depressive disorder as well as for other indications, both psychiatric and non-psychiatric. Although a causal link between the emergence of such symptoms and either worsening of depression and/or emergence of suicidal impulses has not been established, there is concern that such symptoms may be precursors of emerging suicidality.
Families and caregivers of children and adolescents being treated with antidepressants for major depressive disorder or for any other condition (psychiatric or non-psychiatric) should be informed about the need to monitor these patients for the emergence of agitation, irritability, unusual changes in behaviour, and other symptoms described above, as well as the emergence of suicidality, and to report such symptoms immediately to health care providers. It is particularly important that monitoring be undertaken during the initial few months of antidepressant treatment or at times of dose increase or decrease.
Prescriptions of this medicine should be written for the smallest quantity of tablets consistent with good patient management, in order to reduce the risk of overdose.
Akathisia/psychomotor restlessness.
The use of fluvoxamine has been associated with the development of akathisia. This is most likely to occur within the first few weeks of treatment. In patients who develop these symptoms, increasing the dose may be detrimental.
The presentation of akathisia may be variable and comprises subjective complaints of restlessness and an overwhelming urge to move and either distress or motor phenomena such as pacing, swinging of the legs while seated, rocking from foot to foot, or both. Particular attention should be paid to the monitoring for such symptoms and signs as, left untreated, akathisia is associated with poor compliance and an increased risk of relapse.
Nervous system disorders.
Although in animal studies, fluvoxamine has no pro-convulsive properties, caution is recommended when the drug is administered to patients with a history of convulsive disorders. Fluvoxamine should be avoided in patients with unstable epilepsy and patients with controlled epilepsy should be carefully monitored. Treatment with fluvoxamine should be discontinued if seizures occur or if seizure frequency increases.
Metabolism and nutrition disorders.
As with other SSRIs, hyponatraemia has been rarely reported, and appears to be reversible when fluvoxamine is discontinued. Some cases were possibly due to the syndrome of inappropriate antidiuretic hormone secretion. The majority of reports were associated with older patients.
Glycaemic control may be disturbed (i.e. hyperglycaemia, hypoglycaemia, decreased glucose tolerance), especially in the early stages of treatment. When fluvoxamine is given to patients with a known history of diabetes mellitus, the dosage of anti-diabetic drugs may need to be adjusted.
Eye disorders.
Mydriasis has been reported in association with SSRIs such as fluvoxamine. Therefore caution is recommended when prescribing fluvoxamine for patients with raised intraocular pressure or those at risk of acute narrow-angle glaucoma.
Haematological disorders.
There have been reports of cutaneous bleeding abnormalities such as ecchymoses and purpura as well as other haemorrhagic manifestations e.g. gastrointestinal bleeding or gynaecological haemorrhage with SSRIs. Caution is advised in patients taking SSRIs, particularly in elderly patients and in patients who concomitantly use drugs known to affect platelet function (e.g. atypical antipsychotics and phenothiazines, most tricyclic antidepressants, aspirin and NSAIDs) or drugs that increase risk of bleeding as well as in patients with a history of bleeding disorders and in those with predisposing conditions (e.g. thrombocytopenia or coagulation disorders). If any significant bleeding or bruising is observed, it is recommended that a platelet count should be performed.
Cardiac disorders.
When combined with fluvoxamine plasma concentrations of terfenadine, astemizole or cisapride may be increased resulting in an increased risk for QT-prolongation/ Torsades de Pointes. Therefore fluvoxamine should not be co-administered with these agents.
Fluvoxamine may cause an insignificant decrease in heartbeat (2-6 beats per minute).
Dermatological effects.
Serious skin reactions, some of them fatal, including Stevens-Johnson syndrome and toxic epidermal necrolysis, have been reported in association with fluvoxamine (see Section 4.8 Adverse Effects (Undesirable Effects)). Patients appear to be at highest risk of these reactions early in the course of therapy. If skin reactions occur, fluvoxamine should be discontinued immediately, and the patient should be closely monitored.
Electroconvulsive therapy (ECT).
There is limited clinical experience of concomitant administration of fluvoxamine and ECT; therefore caution is advisable.
Serotonin syndrome.
Development of serotonin syndrome or neuroleptic malignant syndrome-like events may occur in association with treatment with SSRIs, particularly when given in combination with MAOIs or other serotonergic and/or neuroleptic agents or in combination with opiate/opioid drugs (e.g. buprenorphine) or in combination with the fixed-dose combination preparation buprenorphine/naloxone. Symptoms and signs of serotonin syndrome include rapid onset of neuromuscular excitation (hyperreflexia, incoordination, myoclonus, tremor), altered mental status (confusion, agitation, hypomania) and autonomic dysfunction (diaphoresis, diarrhoea, fever, shivering and rapidly fluctuating vital signs). Treatment with fluvoxamine should be discontinued if such events occur and supportive symptomatic treatment initiated.
Discontinuation/withdrawal symptoms (also see Section 4.2 Dose and Method of Administration).
The onset of symptoms may occur one to three days after abrupt discontinuation of SSRI therapy and (rarely) after dosage lowering. It is important but may be difficult to distinguish the discontinuation symptoms from a recurrence of the underlying disease. Both may present with disturbances of the equilibrium and of the sensory system. However, they may differ in view of the severity, onset and duration of the symptoms.
Discontinuation symptoms rarely occur after treatment of less than 5 weeks duration and usually last from one day to three weeks.
The most commonly reported symptoms in association with withdrawal of the medicine include: dizziness, sensory disturbances (including paraesthesia, visual disturbances and electric shock sensations), sleep disturbances (including insomnia and intense dreams), agitation, irritability, confusion, emotional instability, headache, nausea and/or vomiting, diarrhoea, sweating, palpitations, tremor and anxiety (see Section 4.8 Adverse Effects (Undesirable Effects)). Generally these effects are mild to moderate and are self-limiting; however in some patients they may be severe and/or prolonged. They usually occur within the first few days of discontinuing treatment.
It is advised that in accordance with clinical experience and individual need of a patient the dosage should be gradually tapered over a couple of weeks when discontinuing treatment (see Section 4.2 Dose and Method of Administration).
Mania/hypomania.
Fluvoxamine should be used with caution in patients with a history of mania/hypomania. Fluvoxamine should be discontinued in any patient entering a manic phase.
Postpartum haemorrhage.
SSRI/SNRIs may increase the risk of postpartum haemorrhage (see Section 4.6 Fertility, Pregnancy and Lactation; Section 4.8 Adverse Effects (Undesirable Effects)).
Sexual dysfunction.
Selective serotonin reuptake inhibitors (SSRIs)/serotonin norepinephrine reuptake inhibitors (SNRIs) may cause symptoms of sexual dysfunction (see Section 4.8 Adverse Effects (Undesirable Effects)). There have been reports of long-lasting sexual dysfunction where the symptoms have continued despite discontinuation of SSRIs/SNRI.
Use in renal impairment.
Patients suffering from renal insufficiency should start on a low dose and be carefully monitored when treated with fluvoxamine. Upward dose titration should be carried out more slowly in this patient population.
Use in hepatic impairment.
Patients suffering from hepatic insufficiency should start on a low dose and be carefully monitored when treated with fluvoxamine. Upward dose titration should be carried out more slowly in this patient population. Clearance of fluvoxamine is slower in patients with hepatic impairment (e.g. cirrhosis).
Treatment with fluvoxamine has rarely been associated with an increase in hepatic enzymes, generally accompanied by clinical symptoms. In such cases treatment should be discontinued.
Use in the elderly.
Data in elderly subjects gives no indication of clinically significant differences in pharmacokinetics compared with younger subjects. Nevertheless, upward dose titration should be carried out more slowly in this patient population, and dosing should always be handled with caution.
Paediatric use.
Fluvoxamine should not be used in children and adolescents (age < 18 years) for the treatment of major depressive disorder as the efficacy and safety of the medicine in these patients for this condition has not been satisfactorily investigated.
Decreased appetite and weight loss have been observed in association with the use of fluvoxamine as well as with other SSRIs. Although no detrimental effect on growth, development and maturation was apparent in the long-term, open-label clinical studies in children, regular monitoring of weight and growth is recommended if treatment of a child with an SSRI is to be continued long term.
Effects on laboratory tests.
Rarely, treatment with fluvoxamine has been associated with an increase in hepatic enzymes, mostly accompanied by clinical symptoms. In these cases, treatment should be discontinued.
Effects on other laboratory tests have not been established.4.5 Interactions with Other Medicines and Other Forms of Interactions
The concurrent use of fluvoxamine with tizanidine or cisapride is contraindicated (see Section 4.3 Contraindications).
Fluvoxamine tablets should not be used in combination with ramelteon (see Section 4.3 Contraindications). When immediate-release fluvoxamine maleate tablets 100 mg twice daily was administered for 3 days prior to single-dose co-administration of ramelteon 16 mg and immediate-release fluvoxamine maleate tablets, the AUC for ramelteon increased approximately 190-fold and the Cmax increased approximately 70-fold compared to ramelteon administered alone.
Pharmacodynamic interactions.
The serotonergic effects of fluvoxamine may be enhanced when used in combination with other serotonergic agents and/or neuroleptic drugs including opioid preparations (e.g. tramadol, buprenorphine and buprenorphine/naloxone), triptans, SSRIs and St John's Wort preparations. In rare cases, this could lead to the development of a serotonin syndrome or neuroleptic malignant syndrome (NMS)-like events. As these syndromes may result in potentially life-threatening conditions, treatment with fluvoxamine should be discontinued if such events (characterised by clusters of symptoms such as hyperthermia, rigidity, myoclonus, autonomic instability with possible rapid fluctuations of vital signs, mental status changes including confusion, hypomania, extreme agitation progressing to delirium and coma) occur and supportive symptomatic treatment should be initiated.
Fluvoxamine should not be used in combination with monoamine oxidase inhibitors (MAOIs) including linezolid, due to risk of serotonin syndrome (see Section 4.3 Contraindications). It should be used with caution in combination with other SSRIs, tricyclic antidepressants, tryptophan, triptans phentermine, tramadol or opioid preparations.
Although fluvoxamine has been used in combination with lithium in the treatment of severely ill, drug-resistant patients, possible potentiation of serotonergic effect should be kept in mind.
As with other psychotropic drugs, patients should be advised to avoid using alcohol while taking fluvoxamine.
When fluvoxamine was co-administered with warfarin for 2 weeks, plasma prothrombin times were prolonged. This can be ascribed to the intrinsic ability of SSRIs to lower the serotonin concentration in blood platelets (which can lead to prolonged bleeding in sensitive patients), and to fluvoxamine increasing the warfarin plasma concentrations (see below). As the risk for haemorrhage may increase, patients receiving anticoagulants should have their prothrombin time monitored and their anticoagulant dose adjusted accordingly when administered fluvoxamine.
Pharmacokinetic interactions.
Fluvoxamine is metabolised in the liver, mostly via the cytochrome P450 system. While the specific enzymes involved are not definitively known, it would appear, based on available in vitro data, that CYP1A2 is the main isoenzyme involved. To a much lesser extent CYP3A4 and CYP2C19 may also be involved in the metabolism of fluvoxamine.
In addition, fluvoxamine can inhibit the metabolism of drugs metabolised by certain P450 isoenzymes. A strong inhibition of CYP1A2 and CYP2C19 is demonstrated in in vitro and in vivo studies. CYP2C9, CYP2D6 and CYP3A4 are inhibited to a lesser extent.
Fluvoxamine increases or decreases (e.g. in case of prodrugs like clopidogrel) the plasma concentrations of active substance/metabolites of drugs which are largely metabolised via these isoenzymes.
Fluvoxamine has only a weak inhibitory effect on CYP2D6, and is therefore not likely to increase plasma concentrations of drugs metabolised by CYP2D6 to a clinically relevant extent.
Concomitant therapy of fluvoxamine and these drugs should be initiated at or adjusted to the low end of their dosage range. Plasma concentrations, effects or adverse effects of coadministered drugs should be monitored and their dosage should be reduced if necessary. This is particularly relevant for drugs with a narrow therapeutic index.
CYP1A2. Tricyclic antidepressants and neuroleptics.
An increase in previously stable plasma levels of those tricyclic antidepressants (such as clomipramine, amitriptyline and imipramine) and neuroleptics (or antipsychotics such as clozapine, olanzapine, quetiapine) which are largely metabolised through CYP1A2 has been reported when used together with fluvoxamine. The combination of fluvoxamine with these drugs is not recommended.
Compounds with a narrow therapeutic index.
Patients co-administered fluvoxamine and CYP1A2 metabolised drugs with a narrow therapeutic index (such as tacrine, theophylline, methadone, mexiletine, phenytoin, carbamazepine and ciclosporin) should be carefully monitored when these agents are metabolised exclusively or by a combination of CYPs inhibited by fluvoxamine. If necessary, dose adjustment of these drugs is recommended.
Due to the narrow therapeutic index of pimozide and its known ability to prolong QT interval, concomitant use of pimozide and fluvoxamine is contraindicated (see Section 4.3 Contraindications).
Cases of increased side effects.
Isolated cases of cardiac toxicity have been reported when fluvoxamine was combined with thioridazine.
Caffeine plasma levels are likely to be increased during co-administration with fluvoxamine. Thus, patients who consume high quantities of caffeine-containing beverages should lower their intake when fluvoxamine is administered and adverse caffeine effects (like tremor, palpitations, nausea, restlessness, insomnia) are observed.
Side effects may be increased when fluvoxamine is used in combination with terfenadine, astemizole, cisapride and sildenafil (see Section 4.4 Special Warnings and Precautions for Use).
CYP3A4. When combined with fluvoxamine, plasma concentrations of cisapride may be increased resulting in an increased risk of QT-prolongation Torsades de Pointes. Therefore fluvoxamine should not be co-administered with cisapride.
The plasma concentrations of benzodiazepines metabolised by oxidation (such as triazolam, midazolam, alprazolam and diazepam) are likely to increase when co-administered with fluvoxamine. The dosages of these benzodiazepines should be reduced during coadministration with fluvoxamine. For benzodiazepines metabolised by glucuronidation (lorazepam, lormetazepam, oxazepam, temazepam) or nitro-reduction (clonazepam, nitrazepam) such an effect is not likely to occur.
Increased serum concentrations of haloperidol have also been reported after concomitant use of haloperidol and fluvoxamine.
Patients co-administered fluvoxamine and CYP3A4 metabolised drugs with a narrow therapeutic index (e.g. ciclosporin, methadone or carbamazepine) should be carefully monitored and, if necessary, dose adjustments of these drugs is recommended.
CYP2C. Patients co-administered fluvoxamine and CYP2C metabolised drugs with a narrow therapeutic index (such as phenytoin) should be carefully monitored and, if necessary, dose adjustments of these drugs is recommended.
Cases of increased plasma concentration. As plasma concentrations of ropinirole may be increased in combination with fluvoxamine thus increasing the risk of overdose, surveillance and reduction in the dosing of ropinirole during fluvoxamine treatment and after its withdrawal may be required.
As plasma concentration of propranolol is increased in combination with fluvoxamine, the propranolol dose may need to be lowered.
When given with fluvoxamine warfarin plasma concentrations were significantly increased and prothrombin time prolonged.
Other. No interactions were seen with digoxin or atenolol, which are renally excreted.
After a single oral dose, fluvoxamine plasma concentrations were lower in smokers than in non-smokers.4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
No evidence of impairment of fertility in male or female rats was observed with fluvoxamine at oral doses up to 80 mg/kg/day.
Reproduction studies in animals revealed impaired fertility (Note: at doses exceeding 2 times the maximum recommended human dosage), increased embryofoetal death, decreased foetal body weight and increased incidences of foetal eye abnormalities (folded retina) in fluvoxamine doses which markedly exceed maximum recommended human dose.
The potential risk for humans is unknown.
Fluvoxamine should not be used in patients attempting to conceive unless the clinical condition of the patient requires treatment with fluvoxamine.
(Category C)
Epidemiological data have suggested that the use of SSRIs in pregnancy, particularly in late pregnancy, may increase the risk of persistent pulmonary hypertension in the newborn (PPHN). The observed risk was approximately 5 cases per 100 pregnancies. In the general population 1 to 2 cases of PPHN occur per 1000 pregnancies.
There was no evidence of teratogenic effects following administration of fluvoxamine at oral doses up to 80 mg/kg/day to rats and rabbits during the period of organogenesis, with rat exposure (based on plasma AUC similar to human exposure at the maximum recommended human dose). Oral administration of fluvoxamine to rats at doses of 5 - 160 mg/kg/day during late gestation and lactation was associated with increased postnatal pup mortality.
Fluvoxamine should not be used during pregnancy unless the clinical condition of the woman requires such treatment. Cases of withdrawal symptoms in the newborn child have been described after the use of fluvoxamine at the end of pregnancy. Neonates exposed to fluvoxamine, other SNRIs (Serotonin and Norepinephrine Reuptake Inhibitors), or SSRIs (Selective Serotonin Reuptake Inhibitors), late in the third trimester have developed complications requiring prolonged hospitalisation, respiratory support, and tube feeding. Such complications can arise immediately upon delivery. Reported clinical findings have included respiratory distress, cyanosis, apnoea, seizures, temperature instability, feeding difficulty, vomiting, hypoglycemia, hypotonia, hypertonia, hyperreflexia, tremor, jitteriness, lethargy, somnolence, difficulty in sleeping, irritability and constant crying. These features are consistent with either a direct effect of SSRIs and SNRIs or, possibly, a drug discontinuation syndrome. Observational data indicate an increased risk (less than 2-fold) of postpartum haemorrhage following SSRI/SNRI exposure within the month prior to birth (see Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects)).
Oral administration of fluvoxamine to rats at doses greater than 1 mg/kg/day during late gestation and lactation was associated with increased postnatal pup mortality. Since fluvoxamine is excreted in human milk, the drug should not be used by lactating women (see Section 4.3 Contraindications).4.7 Effects on Ability to Drive and Use Machines
Fluvoxamine at doses up to 150 mg per day exhibited no effect on psychomotor skills associated with driving and operating machinery in healthy volunteers. However, somnolence has been reported during treatment with fluvoxamine. Therefore, caution is recommended until the individual response to the drug has been determined.
4.8 Adverse Effects (Undesirable Effects)
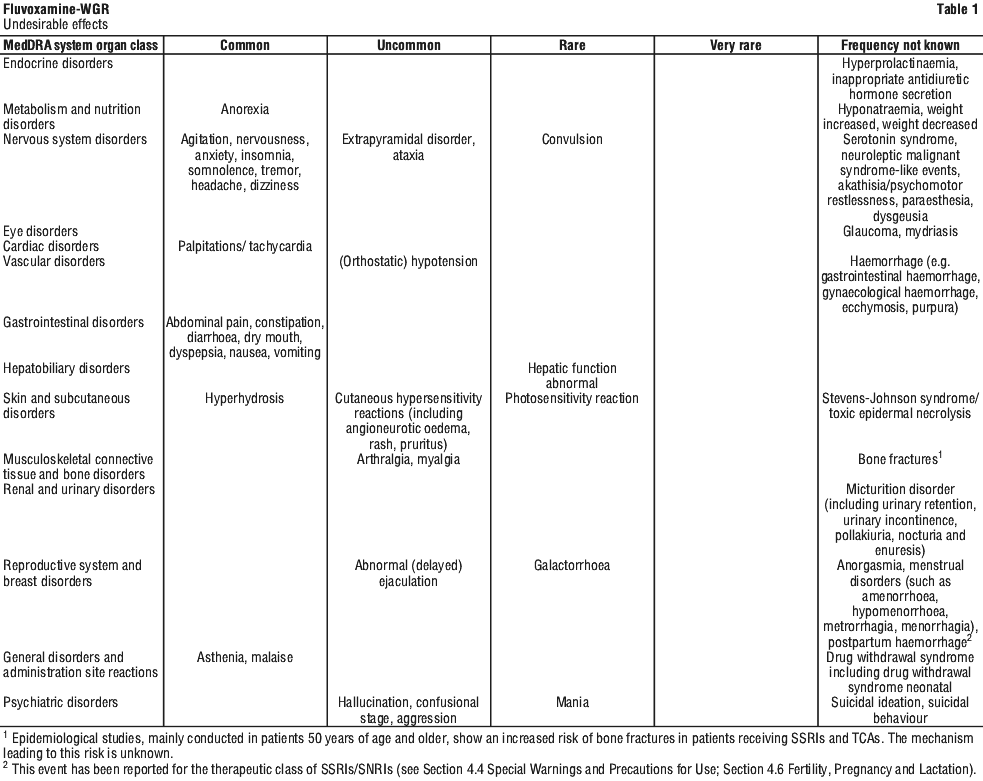
Nausea, sometimes accompanied by vomiting, is the most frequently observed symptom associated with fluvoxamine treatment. This side effect usually diminishes within the first two weeks of treatment. Other adverse events, observed in clinical studies at frequencies listed (database size approx - 35,000 patients; dose range 50-300 mg/day), are often associated with the illness and are not necessarily related to treatment.
Events are listed within body systems and categorised by frequency according to the following definitions: very common (frequency > 10%); common (frequency ≥ 1 and < 10%); uncommon (frequency ≥ 0.1% and < 1%); rare (frequency ≥ 0.01% and < 0.1%); very rare (frequency < 0.01%); not known (cannot be estimated from the available data). See Table 1.
Withdrawal symptoms seen on discontinuation of fluvoxamine treatment.
Discontinuation of fluvoxamine treatment (particularly when abrupt) commonly leads to withdrawal symptoms. It is therefore advised that when fluvoxamine treatment is no longer required, gradual discontinuation by dose tapering should be carried out (see Section 4.2 Dose and Method of Administration; Section 4.4 Special Warnings and Precautions for Use).
Post-marketing data.
As with other SSRIs, hyponatraemia has been rarely reported with fluvoxamine and appeared to be reversible when fluvoxamine was discontinued. Some cases were probably due to the syndrome of inappropriate antidiuretic hormone secretion. The majority of reports were associated with older patients.
Haemorrhage ecchymoses, purpura and gastrointestinal bleeding have been reported (see Section 4.4 Special Warnings and Precautions for Use).
Changes in weight (weight gain or weight loss), and hyperprolactinaemia have also been reported.
Very rarely, paraesthesia, taste perversion, visual disturbance and hepatitis have been reported.
Urogenital.
Very rare - anorgasmia and impotence.
Skin.
Uncommon - cutaneous hypersensitivity reaction (including angioedema).
Reproductive system and breast disorders.
Anorgasmia, menstrual disorders (such as amenorrhea, hypomenorrhea, metrorrhagia, menorrhagia).
Class effects. Epidemiological studies, mainly conducted in patients 50 years of age and older, show an increased risk of bone fractures in patients receiving SSRIs and TCAs. The mechanism leading to this risk is unknown.
Other adverse events in OCD paediatric population.
In paediatric patients (n = 57) treated with fluvoxamine the overall profile of adverse events was generally similar to that seen in adult studies. However the following events not appearing above have been reported in two or more of the paediatric patients and were more frequent with fluvoxamine than placebo: abnormal thinking, cough increase, dysmenorrhoea, emotional lability, epistaxis, hyperkinesia, infection and sinusitis.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.4.9 Overdose
Symptoms.
The most common symptoms of overdose include gastrointestinal complaints (nausea, vomiting and diarrhoea). Somnolence and dizziness, cardiac events (tachycardia, bradycardia, hypotension), liver function disturbances, convulsions and coma have also been reported.
Occasionally, more serious complications have been observed in cases of deliberate overdosage of fluvoxamine in combination with other drugs. Deaths due to an overdose of fluvoxamine alone have also been reported.
Treatment.
There is no specific antidote to fluvoxamine. Treatment should consist of general measures employed in the management of overdose along with general symptomatic and supportive measures.
For information on the management of overdose, contact the Poisons Information Centre on 131126 (Australia).5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
Fluvoxamine has two isomeric forms: an E isomer which is pharmacologically active, and a Z isomer which is non-active. Fluvoxamine tablets contain only the E isomer.
The mechanism of action of fluvoxamine is believed to be related to its ability to selectively inhibit presynaptic reuptake of serotonin, and thus increase the serotonin concentrations within the synaptic cleft. This is accompanied by minimal interference with the noradrenergic and dopaminergic processes.
Unlike tricyclic antidepressants, fluvoxamine has limited affinity for alpha adrenergic, beta adrenergic, histaminergic, muscarinic, dopaminergic or serotoninergic receptors. Antagonism of these post-synaptic receptors are believed to be associated with some of the cardiovascular, anticholinergic and sedative effects of classical tricyclic antidepressant drugs.
Dose-dependent decreases in rapid eye movement (REM) sleep and increased REM latency were found with fluvoxamine. These effects are similar to those of other antidepressant drugs.
Clinical trials.
Depression. In depression, the efficacy of fluvoxamine was established in 15 three-way trials in which fluvoxamine (≥ 100 mg/day) was compared with both placebo and a tricyclic antidepressant (imipramine ≥ 150 mg/day or desipramine ≥ 100 mg/day) generally over a period of 6 weeks and using HAM-D, CGI severity and MADRS as the main efficacy criteria. Of these studies, seven showed conclusive results: four were positive for both fluvoxamine and active reference therapy, whereas the other three studies showed only efficacy for active reference therapy. In a pooled analysis of the results of all these studies, both fluvoxamine (n = 837) and active reference therapy (n = 779) were found to be more effective than placebo (n = 837). HAM-D improvements (LOCF) after 6 weeks were 39.1%, 41.9% and 33.9%, respectively. In these studies, the effective dose range for fluvoxamine was determined to lie between 100 mg and 300 mg per day. Using various definitions of response based on HAM-D or CGI criteria, there were no statistically significant differences in response rates between fluvoxamine and active reference therapy. Statistical analyses of the data did not reveal any patient features (such as age, sex, race etc.) which predict treatment response to fluvoxamine.
Prevention of relapse of depression.
A study of depressed outpatients who had responded to fluvoxamine (MADRS ≤ 10) during an initial 26 week open treatment phase (n = 204) and were then double-blind randomised to continuation on fluvoxamine (100 mg/day) or placebo for 1 year demonstrated a significantly lower relapse rate for fluvoxamine (13%) compared to those on placebo (35%).
Obsessive compulsive disorder (OCD). Adult OCD studies.
The effectiveness of fluvoxamine in the treatment of Obsessive Compulsive Disorder (OCD) was demonstrated in two 10-week placebo-controlled studies (Studies 1 and 2). The results of two 10 week clomipramine-controlled studies (Studies 3 and 4) support the effectiveness of fluvoxamine in the treatment of OCD.
Studies 1 and 2 were flexible dose double-blind parallel group, multicentre studies in which patients with moderate to severe OCD received fluvoxamine in doses up to 300 mg/day or placebo. 157 patients received fluvoxamine versus 158 patients who received placebo. Improvements from baseline in Yale-Brown Obsessive Compulsive Disorder (Y-BOCS) and NIMH-OC scores and the CGI improvement score were significantly greater in fluvoxamine treated patients. In these studies, the overall response rates were 36% for fluvoxamine and 12% for placebo, and the effective dosage range for fluvoxamine was between 100 mg and 300 mg daily. In open extension studies, efficacy in OCD was demonstrated to be maintained in a total of 72 patients treated for a total of 46 weeks or more.
Studies 3 and 4 were flexible dose double-blind parallel group multicentre studies comparing fluvoxamine (100-300 mg/day) with clomipramine (100 mg-250 mg/day). 69 patients received fluvoxamine versus 76 patients who received clomipramine. Fluvoxamine and clomipramine were equally efficacious on the Y-BOCS, NIMH-OC and CGI improvement scores.
Paediatric OCD study.
The effectiveness of fluvoxamine for the treatment of OCD was also demonstrated in a 10-week multicentre, parallel group, placebo-controlled study in a paediatric outpatient population (children and adolescents, ages 8-17) followed by an open-label extension of up to two years.
In the double-blind phase of the study, patients were titrated to a total daily fluvoxamine dose of approximately 100 mg/day over the first two weeks of the trial, following which the dose was adjusted within a range of 50-200 mg/day (on a b.i.d. schedule) on the basis of response and tolerance. All patients had moderate to severe OCD (DSM-III-R) with mean baseline ratings on the Children's Yale-Brown Obsessive Compulsive Scale (CY-BOCS), total score of 24. Patients receiving fluvoxamine maleate experienced mean reductions of approximately 6 units on the CYBOCS total score, compared to a 3 unit reduction for placebo patients.
Table 2 provides the outcome classification by treatment group on the Global Improvement item of the Clinical Global Impression (CGI) scale for the paediatric study.
 Post hoc exploratory analyses for gender effects on outcomes did not suggest any differential responsiveness on the basis of gender. Further exploratory analyses revealed a prominent treatment effect in the 8-11 age group and essentially no effect in the 12-17 age group. The reason for the difference in these results is unknown. However, follow up data from the open extension of the study showed a further improvement as demonstrated by a decrease of an additional 3 to 6 units on the CY-BOCS in young, as well as adolescent, patients. This improvement was sustained over a one-year period in 54 of the 98 patients who completed the one-year extension and in 12 of the 22 patients who completed the two year extension.
Post hoc exploratory analyses for gender effects on outcomes did not suggest any differential responsiveness on the basis of gender. Further exploratory analyses revealed a prominent treatment effect in the 8-11 age group and essentially no effect in the 12-17 age group. The reason for the difference in these results is unknown. However, follow up data from the open extension of the study showed a further improvement as demonstrated by a decrease of an additional 3 to 6 units on the CY-BOCS in young, as well as adolescent, patients. This improvement was sustained over a one-year period in 54 of the 98 patients who completed the one-year extension and in 12 of the 22 patients who completed the two year extension.
5.2 Pharmacokinetic Properties
Absorption and bioavailability.
Fluvoxamine is almost completely absorbed following oral administration. The absolute bioavailability is 53% (90% confidence interval: 44-62%). Absorption is unaffected by the presence of food.
Distribution.
Maximum plasma levels occur within 3-8 hours of dosing. Steady state levels are usually achieved within one week. The mean plasma half-life is approximately 12-13 hours after a single dose and approximately 22 hours following repeated dosing. In vitro binding of fluvoxamine to human plasma proteins is 80%, and the volume of distribution is estimated to be 20 L/kg.
Metabolism.
The pharmacokinetics of fluvoxamine is linear between single oral doses of 25-100 mg. During multiple dosing in the range of 100-300 mg per day, the higher doses produced disproportionally higher plasma concentrations than predicted from data obtained with the lower dose.
Excretion.
Fluvoxamine undergoes extensive hepatic transformation, mainly via oxidative demethylation, into at least 9 metabolites. Less than 4% of the dose is excreted in the urine as unchanged parent compound, while approximately 94% of the dose is recovered in the urine as metabolites. The two principal metabolites exhibit negligible pharmacological activity. In view of the structures of the other metabolites, it is not expected that the other metabolites would be pharmacologically active.
The pharmacokinetics of fluvoxamine in patients with renal dysfunction do not appear to differ significantly from those in healthy, young volunteers. The area under the plasma concentration-time curve (AUC) and half-life were greater, however, in patients with liver dysfunction. Patients suffering from renal or hepatic insufficiency should be carefully monitored when treated with fluvoxamine. Upward dose titration should be carried out more slowly in this patient population.
Paediatric subjects.
The multiple-dose pharmacokinetics of fluvoxamine was determined in male and female children (ages 6-11) and adolescents (ages 12-17). The clearance of fluvoxamine in children was approximately half that observed in adolescents. AUC and Cmax in children were 1.5 to 2.7-fold higher than that in adolescents. As in adults, both children and adolescents exhibited nonlinear multi-dose pharmacokinetics. Female children showed significantly lower clearance values and higher AUC0-12 and Cmax compared to male children and, therefore, lower doses of fluvoxamine may produce therapeutic benefit. No gender differences were observed in adolescents. Body weight adjusted mean clearance at a dose of 300 mg/day was approximately 50% higher in adolescents compared to adults in previous studies.
5.3 Preclinical Safety Data
Genotoxicity.
No evidence of mutagenicity or chromosomal damage was observed in vitro. An in vivo test for chromosomal damage in mice (micronucleus test) gave no clear evidence of clastogenic activity.
Carcinogenicity.
In animal studies, there was no evidence of carcinogenic activity when fluvoxamine was given to rats at dietary doses up to 211 mg/kg/day for 30 months (approximately 2-5 times the maximum human exposure, based on plasma AUC), or to hamsters at about the same dose level for 112 weeks (male) and 85 weeks (female) (approximately two thirds the maximum human exposure, based on plasma AUC).6 Pharmaceutical Particulars
6.1 List of Excipients
Magnesium stearate, mannitol, hyetellose, macrogol 8000, titanium dioxide, iron oxide yellow, iron oxide red (100 mg tablets only), iron oxide black (100 mg tablets only).
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 30°C.
6.5 Nature and Contents of Container
Fluvoxamine-WGR tablets 50 mg.
AUST R 147396.
Fluvoxamine-WGR tablets 100 mg.
AUST R 147397.
30 tablets in blister packs.
Not all strengths may be available.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Fluvoxamine maleate is a white to slightly off-white, odourless, crystalline powder, sparingly soluble in water, freely soluble in ethanol and chloroform, practically insoluble in diethylether. It has a partition coefficient (n-octanol/water, own pH) P=38.7.
Fluvoxamine is a member of a class of antidepressant agents known as selective serotonin reuptake inhibitors (SSRI). It is chemically unrelated to the tricyclic antidepressants, and to other serotonin reuptake inhibitors as it is a monocyclic compound.
Chemical structure.
 Chemical name: (E)-5-methoxy-4'-trifluoromethylvalerophenone O-2-aminoethyloxime maleate.
Chemical name: (E)-5-methoxy-4'-trifluoromethylvalerophenone O-2-aminoethyloxime maleate.
Molecular formula: C15H21F3N2O2.C4H4O4. Molecular weight: 434.4.
CAS number.
61718-82-9.7 Medicine Schedule (Poisons Standard)
S4 - Prescription Only Medicine.
Summary Table of Changes





 Post hoc exploratory analyses for gender effects on outcomes did not suggest any differential responsiveness on the basis of gender. Further exploratory analyses revealed a prominent treatment effect in the 8-11 age group and essentially no effect in the 12-17 age group. The reason for the difference in these results is unknown. However, follow up data from the open extension of the study showed a further improvement as demonstrated by a decrease of an additional 3 to 6 units on the CY-BOCS in young, as well as adolescent, patients. This improvement was sustained over a one-year period in 54 of the 98 patients who completed the one-year extension and in 12 of the 22 patients who completed the two year extension.
Post hoc exploratory analyses for gender effects on outcomes did not suggest any differential responsiveness on the basis of gender. Further exploratory analyses revealed a prominent treatment effect in the 8-11 age group and essentially no effect in the 12-17 age group. The reason for the difference in these results is unknown. However, follow up data from the open extension of the study showed a further improvement as demonstrated by a decrease of an additional 3 to 6 units on the CY-BOCS in young, as well as adolescent, patients. This improvement was sustained over a one-year period in 54 of the 98 patients who completed the one-year extension and in 12 of the 22 patients who completed the two year extension. Chemical name: (E)-5-methoxy-4'-trifluoromethylvalerophenone O-2-aminoethyloxime maleate.
Chemical name: (E)-5-methoxy-4'-trifluoromethylvalerophenone O-2-aminoethyloxime maleate.
