What is in this leaflet
This leaflet answers some common questions about HYQVIA.
It does not contain all of the available information. All medicines have risks and benefits. Your doctor has weighed the risks of using your medicine against the benefit that it will have for you.
It does not take the place of talking to your doctor or pharmacist.
If you have any concerns about having this medicine, ask your doctor or pharmacist.
Please read this leaflet carefully and keep it for future reference. Please also note that this leaflet is subjected to change, therefore, ask your doctor whether this is the latest information regarding this medicine.
What HYQVIA is
Your medicine is HYQVIA, a solution for subcutaneous infusion.
HYQVIA contains two solutions for infusion (drip) under the skin (subcutaneous infusion).
It is supplied as a package containing one vial of Normal Immunoglobulin Infusion 10% (Human) (the active substance) and one vial of Vorhyaluronidase alfa (a substance which helps the immunoglobulin reach your blood).
Normal Immunoglobulin Infusion 10% (Human) belongs to a class of medicines called "human normal immunoglobulins". Immunoglobulins are also known as antibodies and are found in healthy people's blood.
Antibodies are part of the immune system (the body's natural defences) and help your body to fight infections. If you do not have enough antibodies you may not be able to fight off infections.
What HYQVIA is used for
HYQVIA is used in patients who do not have enough antibodies in their blood. HYQVIA can be used as antibody replacement therapy to raise antibody levels in your blood to normal levels.
HYQVIA should only be used in adults.
Before you use HYQVIA
About blood products
When medicines are made from human blood or plasma, processes are used to prevent infections being passed from the blood/plasma donor to the person receiving the medicine.
These processes include careful selection of the people who donate blood and plasma to make sure that those who might be carrying infections are excluded. In addition, each donation and pools of donations are tested for indicators of virus or virus infection(s).
Manufacturers of these medicines also include steps in the processing of blood or plasma that inactivate or remove viruses. A three step viral inactivation/reduction has been applied during the manufacturing of the Normal Immunoglobulin Infusion. Despite the stringent measures, which have been put in place during the manufacturing processes, the risk of contamination by viral and other unknown agents cannot be totally excluded.
The measures taken during manufacturing are considered effective for enveloped viruses such as human immunodeficiency virus (HIV), hepatitis B virus and hepatitis C virus, and for the non-enveloped viruses hepatitis A (HAV) and B19 virus (B19V).
Immunoglobulins have not been associated with hepatitis A or parvovirus B19 infections possibly because the antibodies against these infections, which are contained in the product, are protective.
HYQVIA must not be used if
You are allergic to immunoglobulins, hyaluronidase, recombinant hyaluronidase or are allergic to any ingredients in HYQVIA (see "Product Description").
Tell your doctor if you:
- if you have antibodies against immunoglobulin A (IgA) in your blood. This may occur if you have IgA deficiency.
- have allergies to any other medicines, or if you have ever had an allergic reaction to an injection.
Please discuss the risks and benefits of this product with your doctor.
What should I tell my doctor before using HYQVIA?
You should tell your doctor if you:
- have or have had any medical problems.
- take any medicines, including prescription and non-prescription medicines, such as over-the-counter medicines, supplements or herbal remedies.
- Have had a vaccination recently
- are planning to become pregnant, pregnant or breastfeeding
How to use HYQVIA
Always use HYQVIA exactly as your doctor has told you. Check with your doctor if you are not sure.
HYQVIA has to be infused under the skin.
Treatment with HYQVIA will be started by your doctor or nurse, but you may be allowed to use the medicine at home once you have received the first few infusions under medical supervision and you (and/or your guardian) have been adequately trained. You and your doctor will decide if you can use HYQVIA at home. Do not begin treatment with HYQVIA at home until you have received complete instructions.
Always wash your hands before doing the following procedures. Use germ-free methods during the making up procedure and during injection.
HYQVIA must not be mixed with other injectable medicines.
Instructions for use
If you do not understand the instructions, ask your doctor or health professional.
Always follow the specific instructions given by your healthcare provider. The steps listed below are general guidelines for using your medicine.
For the ease of identification the Vorhyaluronidase alfa (Hyaluronidase) vial is labelled HY and the Normal Immunoglobulin Infusion 10% (human) vial is labelled IG.
- Check each vial of HYQVIA before using:
- Expiration date:
Do not use beyond expiration date. - Colour:
- The Vorhyaluronidase alfa should be clear and colourless.
- The Normal Immunoglobulin Infusion should be clear and colourless or pale yellow.
- If either liquid is cloudy or has particles, do not use. - Cap:
Protective cap is on the dual vial unit. Do not use the product if it does not have the cap.
- Prepare for infusion:
- Gather supplies: HYQVIA dual vial unit(s), ancillary supplies, sharps container and infusion pump (program pump per physician recommendation following manufacturer's instructions).
- Prepare a clean work area.
- Wash hands.
If the Normal Immunoglobulin Infusion 10% (Human) and Vorhyaluronidase alfa are pooled into separate containers, skip to Step 5.
- Prepare the Vorhyaluronidase alfa of HYQVIA (Labelled as "HY"):
- Remove the protective cap.
- Wipe each stopper with a sterile alcohol wipe and allow to dry.
- Attach a syringe to a needle/ needle-less transfer device.
- Pull back on plunger of the syringe to fill the syringe with air equal to the amount in the HY vial.
- Insert needle into the centre of the vial stopper.
- Inject air into the vial and withdraw the full contents of the HY vial(s) into a syringe.
- Attach the syringe containing the Vorhyaluronidase alfa to the subcutaneous needle set.
- Point the syringe tip up and push the plunger of the syringe to remove the air and fill the needle set up to the needle hub with the HY.
- Prepare Normal Immunoglobulin Infusion 10% (Human) of HYQVIA (Labelled as "IG"):
- Wipe each stopper with a sterile alcohol wipe and allow to dry.
- Transfer the vial(s) labelled IG into either syringe(s), infusion bag or directly from the vial as shown by your healthcare professional:
a. If using syringe(s):
- Attach a sterile syringe to a vented spike.
- Insert the vented spike into the centre of the IG vials.
- Turn the vial upside down and pull back on the plunger to pull the IG into the syringe(s).
- Repeat these steps, if using multiple vials to achieve the desired dose.
b. If using an infusion bag:
- Insert the vented spike into the centre of each IG vial. Open the vent.
- Turn the vial upside down and fill the bag with the IG. Repeat this step, if using multiple vials to achieve the desired dose.
- Remove the filling tube(s) of the bag and place a sterile cap over the open end of the bag and close the clamp on bag.
- Insert the spike of the administration pump tubing into the bag and fill as directed by your healthcare professional.
c. If directly from the IG vial:
- Insert the spike of the vented pump tubing into centre of the stopper of the IG vial(s). Fill the administration pump tubing and set aside until the Vorhyaluronidase alfa has been administered.
Repeat the steps above for each remaining vial of the IG
- Prepare the infusion site(s):
- Potential sites for infusion include the middle to upper abdomen and thighs.
- Avoid: bony prominences, blood vessels, scars, or areas that are inflamed or infected.
- If two sites are desired, a bifurcated needle set may be used on opposite sides of the body, for doses above 600mL.
- Rotate sites by choosing opposite sides of the body between successive infusions.
Cleanse the infusion site(s) with a sterile alcohol wipe beginning at the centre of each infusion site and moving outward in a circular motion. Allow the infusion site(s) to dry (at least 30 seconds).
- Insert and secure the 24 gauge subcutaneous needle:
- Pinch at least one inch (2 to 2.5 cm) of skin between two fingers. Insert the needle at a 90-degree angle into the subcutaneous tissue and secure the needle with sterile tape.
- Check placement: gently pull back on the plunger of attached syringe and monitor for any blood return in the tubing.
- If blood is seen in the tubing, remove and discard the needle and repeat steps 3, 5 and 6 with a new subcutaneous needle and infusion site. - Secure the needle in place with a sterile protective dressing.
- Administer the Vorhyaluronidase alfa of HYQVIA:
Administer the entire Vorhyaluronidase alfa dose first. Start at a rate of 1 to 2 mL per minute per site or as tolerated. If more than one site is used, divide the contents equally between sites. At the end of infusion, disconnect the empty syringe and attach pump tubing/syringe containing the Normal Immunoglobulin of HYQVIA to the same subcutaneous needle set.
- Administer the Normal Immunoglobulin of HYQVIA:
Within approximately 10 minutes of completing the infusion of the Vorhyaluronidase alfa of HYQVIA, start the variable rate program of the infusion pump to initiate the infusion of the full therapeutic dose of Normal Immunoglobulin Infusion of HYQVIA. At the end of infusion, flush infusion tubing up to the needle with normal saline or 5% Glucose in water, If directed by your healthcare professional.
- Remove subcutaneous needle(s) from the infusion site(s):
After the infusion is complete, remove the needle set and cover with a protective dressing.
- Document the infusion:
Remove the peel-off label from each Normal Immunoglobulin Infusion vial of HYQVIA used and affix to the patient's treatment record or infusion log. In addition, record the time, date, dose, infusion site location and any reactions after each infusion.
For self-administration, provide the patient with instructions and training for infusion in the home or other appropriate setting.
If you miss/forget your injection
Do not infuse a double dose of HYQVIA to make up for a missed dose. If you think that you have missed a dose speak to your doctor as soon as possible.
If you take too much (Overdose)
The effects of an overdose of HYQVIA are not known. Please tell your doctor if you accidently use more than instructed.
While you are using HYQVIA
Things you must do
- Stop the infusion immediately and contact your doctor, if you experience allergic reactions such as skin rash, itching, chest tightness, wheezing, dizziness, hives, faintness, chills, flushing, rapid heartbeat, shortness of breath and/or a swollen face
- Always follow your doctor's instructions carefully
- Tell all the doctors, dentists and pharmacists who are treating you that you are using HYQVIA
- If you are about to be started on any new medicine, tell your doctor and pharmacist that you are using HYQVIA
- If you become pregnant while you are using your medicine, tell your doctor.
- Talk to your healthcare provider before traveling. Plan to bring enough medicine for your treatment during this time. It is important to obtain a written statement from your physician, explaining the reasons why you need to have this medicine and injecting devices with you, otherwise you may not be allowed to bring it into the country of travelling.
Things you must not do
- Do not give your medicine to anyone else, even if they have the same condition as you
- Do not use your medicine to treat any other complaints unless your doctor tells you to
- Do not stop using your medicine or lower the dosage, without checking with your doctor, unless you have an allergic reaction.
Side effects
Like all medicines, this medicine can have side effects, although not everybody gets them. Certain side effects, such as headache, chills, or body aches, may be reduced by slowing the infusion rate.
Tell your doctor immediately or go to Accident and Emergency Department at your nearest hospital if you notice any of the following symptoms:
- chest pain or tightness
- difficulty breathing
- lightheadedness,
- dizziness, nausea or fainting.
- Fast heart rate
- swelling in the mouth or throat, difficulty breathing, wheezing,
- abnormal heart rate, blueness of lips or fingers and toes,
- blurred vision
Tell your doctor or nurse immediately if you notice any of the following and they worry you.
This list includes the more common side effects of HYQVIA. They are usually mild and often reduce over time:
- pain, itching, redness or swelling where the injection was given
- nausea or vomiting
- back and muscle pain
- diarrhoea
- headache
- fever or chills
- feeling faint (fall in blood pressure).
These are not all the possible side effects with your medicine. You can ask your doctor or pharmacist for information that is written for healthcare professionals.
After using HYQVIA
HYQVIA contains no preservatives.
Discard any medicine left in the vials at the end of your infusion.
Dispose of all materials, including any leftover reconstituted medicine, in an appropriate container.
Medicines should not be disposed of via wastewater or household waste. Ask your pharmacist how to dispose of medicines no longer required. These measures will help to protect the environment.
Storage
HYQVIA should be stored at 2°C - 8°C in a refrigerator for the duration of its shelf life. Store in the original package in order to protect from light.
Do not freeze.
Keep out of the reach and sight of children.
Do not use HYQVIA after the expiry date which is printed on the label after the word 'EXP'. The expiry date refers to the last day of that month.
Product Description
What HYQVIA looks like?
HYQVIA is a dual vial unit consisting of one vial of Normal Immunoglobulin Infusion 10% (Human) and one vial of Vorhyaluronidase alfa.
The Normal Immunoglobulin Infusion is a clear or slightly opalescent and colourless or pale yellow solution.
Vorhyaluronidase alfa is a clear, colourless solution.
HyQvia is a dual vial unit containing:
- a solution of Vorhyaluronidase alfa (Step 1 of HyQvia/Infuse first) and
- a solution of Normal Immunoglobulin Infusion (Step 2 of HyQvia/Infuse second).
The contents of each vial are described below:
Normal Immunoglobulin Infusion is available in single use glass vials of:
- 2.5 g in 25 mL
- 5 g in 50 mL
- 10 g in 100 mL
- 20 g in 200 mL
- 30 g in 300 mL
Inactive ingredients: Glycine, water for injection
Vorhyaluronidase alfa is available in single use glass vials of:
1.25, 2.5, 5, 10 or 15 ml of solution in a vial
Inactive ingredients: Sodium phosphate dibasic, sodium hydroxide human albumin, 25%, calcium chloride, sodium chloride, edetate disodium and water for inject.
The following pack sizes are available:
Recombinant human hyaluronidase - 1.25mL (volume); Human normal immunoglobulin 10% - 2.5g (protein) 25mL (volume)
Recombinant human hyaluronidase - 2.5mL (volume); Human normal immunoglobulin 10% - 5g (protein) 50mL (volume)
Recombinant human hyaluronidase - 5mL (volume); Human normal immunoglobulin 10% - 10g (protein) 100mL (volume)
Recombinant human hyaluronidase - 10mL (volume); Human normal immunoglobulin 10% - 20g (protein) 200mL (volume)
Recombinant human hyaluronidase - 15mL (volume); Human normal immunoglobulin 10% - 30g (protein) 300mL (volume)
Not all pack sizes may be marketed.
Name and address of the sponsor
HYQVIA is distributed in Australia by:
Takeda Pharmaceuticals Australia Pty Limited
Level 39
225 George Street,
Sydney NSW 2000
Australia
Phone: 1800 012 612
Australian Registration Number
AUST R 235178
HYQVIA is a trademark Baxalta Incorporated. TAKEDA® and the TAKEDA Logo® are registered trademarks of Takeda Pharmaceutical Company Limited.
This leaflet was prepared in December 2020.
Published by MIMS January 2021



 The two components of Hyqvia must be administered sequentially through the same needle beginning with the vorhyaluronidase alfa followed by normal immunoglobulin 10% (human), as described below.
The two components of Hyqvia must be administered sequentially through the same needle beginning with the vorhyaluronidase alfa followed by normal immunoglobulin 10% (human), as described below.


 An objective of the trial was to achieve the same number or fewer infusions with Hyqvia per month as with intravenous administration and significantly fewer than with conventional subcutaneous administration. Summary of infusions of intravenous administration compared to Hyqvia administration is presented in Table 8.
An objective of the trial was to achieve the same number or fewer infusions with Hyqvia per month as with intravenous administration and significantly fewer than with conventional subcutaneous administration. Summary of infusions of intravenous administration compared to Hyqvia administration is presented in Table 8. Sixteen of 83 subjects (19.3%) were infused every 3 weeks and 67 (80.7%) were infused every 4 weeks. Seventy eight of 83 (94%) of subjects attained the same 3 or 4 week dosing as their previous IVIG treatment. One decreased from 4 to 3 weeks, one from 4 to 2 weeks and one from 3 to 2 weeks. The primary reason for decreasing the interval was discomfort due to swelling.
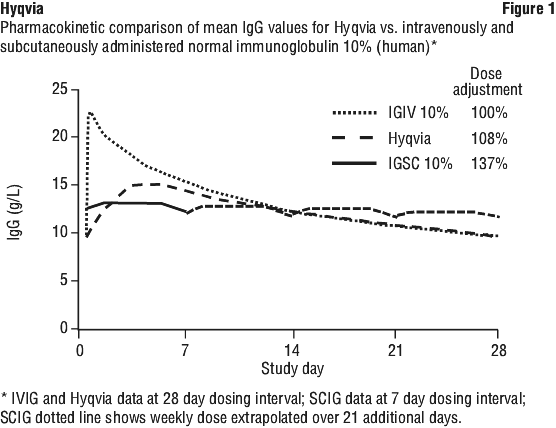
Sixteen of 83 subjects (19.3%) were infused every 3 weeks and 67 (80.7%) were infused every 4 weeks. Seventy eight of 83 (94%) of subjects attained the same 3 or 4 week dosing as their previous IVIG treatment. One decreased from 4 to 3 weeks, one from 4 to 2 weeks and one from 3 to 2 weeks. The primary reason for decreasing the interval was discomfort due to swelling. Figure 1 shows mean concentration time plot of IgG in subjects 12 years and older. The concentration time profile of Hyqvia is similar to that of intravenous administration but without the high peak. The peak to trough variation is more similar to subcutaneous administration.
Figure 1 shows mean concentration time plot of IgG in subjects 12 years and older. The concentration time profile of Hyqvia is similar to that of intravenous administration but without the high peak. The peak to trough variation is more similar to subcutaneous administration.