What is in this leaflet
This leaflet answers some common questions about IKOTAB. It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you taking IKOTAB against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What IKOTAB is used for
This medicine is used to treat chronic stable angina pectoris (chest pain or discomfort due to coronary heart disease).
This medicine belongs to a group of medicines called potassium channel activators.
This medicine works by widening blood vessels and increasing blood supply to the heart muscle.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another reason.
This medicine is not addictive.
Before you take IKOTAB
When you must not take it
Do not take IKOTAB if you have an allergy to:
- any medicine containing nicorandil
- any of the ingredients listed at the end of this leaflet
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin
Do not take IKOTAB if:
- you have low blood pressure (which could make you feel faint, weak, or dizzy, especially when you stand up suddenly)
- you suffer from any other type of serious heart diseases
- you have been prescribed a type of medicine called a 'phosphodiesterase 5 inhibitor' - these medicines are used to treat impaired sexual function
- you have been prescribed any soluble guanylate cyclase stimulators e.g. riociguat
Do not take this medicine if you are pregnant. It may affect your developing baby if you take it during pregnancy.
Do not breast-feed if you are taking this medicine.
Do not give this medicine to children. Safety and effectiveness in children have not been established.
Do not take this medicine after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking this medicine, talk to your doctor.
Before you start to take it
Tell your doctor if you have had any of the following medical conditions:
- kidney or liver disease
- diverticular disease (a condition affecting the muscles of the bowel)
- low blood pressure (common signs of low blood pressure are feeling faint, weakness or dizziness, especially when you stand up quickly)
- other types of serious heart diseases
- depression
- glaucoma
- hyperkalaemia (high potassium levels in the blood)
- mouth, stomach, or skin ulcers
Tell your doctor if you are pregnant or plan to become pregnant or are breast-feeding. Your doctor can discuss with you the risks and benefits involved.
If you have not told your doctor about any of the above, tell them before you start taking IKOTAB.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and IKOTAB may interfere with each other. These include:
- phosphodiesterase 5 inhibitors, medicines often used to treat impaired sexual function
- soluble guanylate cyclase stimulators
- vasodilator medicines, used to widen blood vessels
- tricyclic antidepressants, used to treat depression
- nitrates, medicines used to treat angina (chest pain)
- antihypertensive medicines, used to treat high blood pressure
- corticosteroid medicines
- aspirin or other non-steroidal anti-inflammatories (NSAIDs) e.g. ibuprofen, diclofenac
These medicines may be affected by IKOTAB or may affect how well it works. You may need different amounts of your medicines, or you may need to take different medicines.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while taking this medicine.
How to take IKOTAB
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
If you do not understand the instructions on the box, ask your doctor or pharmacist for help.
How much to take
The usual dose is 10 mg to 20 mg, two times a day. The usual starting dose is 10 mg, two times a day however a lower starting dose may be required in some patients. Your doctor will tell you how much IKOTAB to take.
How to take it
Swallow the tablet with a full glass of water.
When to take it
Take a dose of your medicine in the morning and the evening. Taking it this way each day will have the best effect. It will also help you remember when to take it.
It does not matter if you take this medicine before or after food.
How long to take it
Continue taking your medicine for as long as your doctor tells you.
This medicine helps to control your condition but does not cure it. It is important to keep taking your medicine even if you feel well.
If you forget to take it
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Otherwise, take it as soon as you remember, and then go back to taking your medicine as you would normally.
Do not take a double dose to make up for the dose that you missed. This may increase the chance of you getting an unwanted side effect.
If you are not sure what to do, ask your doctor or pharmacist.
If you have trouble remembering to take your medicine, ask your pharmacist for some hints.
If you take too much (overdose)
Immediately telephone your doctor or the Poisons Information Centre (telephone 13 11 26) for advice, or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have taken too much IKOTAB. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
Symptoms of an overdose may include feeling light-headed, or dizzy, and a faster than normal heartbeat.
While you are using IKOTAB
Things you must do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking IKOTAB.
Tell any other doctors, dentists and pharmacists who treat you that you are taking this medicine.
If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine. It may affect other medicines used during surgery.
If you become pregnant while taking this medicine, tell your doctor immediately.
Keep all of your doctor's appointments so that your progress can be checked.
Things you must not do
Do not take IKOTAB to treat any other complaints unless your doctor tells you to.
Do not give your medicine to anyone else, even if they have the same condition as you.
Do not stop taking your medicine or lower the dosage without checking with your doctor. If possible, your doctor may gradually reduce the amount you take each day before stopping this medicine completely.
Things to be careful of
Be careful driving or operating machinery until you know how IKOTAB affects you. This medicine may cause dizziness or light-headedness in some people. If you have any of these symptoms, do not drive, operate machinery or do anything else that could be dangerous.
Be careful when drinking alcohol while you are taking this medicine. IKOTAB may increase the effects of alcohol.
If you feel light-headed, dizzy or faint when getting out of bed or standing up, get up slowly. Standing up slowly, especially when you get up from bed or chairs, will help your body get used to the change in position and blood pressure. If this problem continues or gets worse, talk to your doctor.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking IKOTAB.
This medicine helps most people with angina, but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor or pharmacist if you notice any of the following and they worry you:
- headache
Headaches usually occur when you begin to take IKOTAB, and generally do not last long. - dizziness and light headedness, especially when getting up from a sitting or lying down position
- tiredness, drowsiness
- cough
- nausea, vomiting, indigestion
- diarrhoea
- constipation
- stomach ache
- flushing, sweating
- loss of appetite, weight loss
- fever
- leg, neck, back, chest or muscular pain, pain in the arm or general pain
- trouble sleeping
- nervousness
- depression
- itching
- double vision
- nose bleed
- skin abscess
Tell your doctor as soon as possible if you notice any of the following:
- high blood pressure
- fast or irregular heart beats
- swelling of the face, hands, ankles or feet
- difficulty in breathing or shortness of breath
- tingling or numbness of the hands or feet
- rash
- ringing or other persistent noise in the ears
- persistent mouth ulcers or genital, anal or skin ulcers
- dark bowel motions and/or bloody diarrhoea
- inflammation of the bowel wall (fever, vomiting and stomach pain or discomfort)
- high potassium levels in the blood
- nerve paralysis
Tell your doctor immediately, or go to Accident and Emergency at your nearest hospital if you notice any of the following:
- allergic type reactions e.g. skin rash, itching and difficulty breathing, wheezing or coughing.
You may need urgent medical attention or hospitalisation.
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Other side effects not listed above may also occur in some people.
After using IKOTAB
Storage
Keep your tablets in the pack until it is time to take them. If you take the tablets out of the pack they may not keep well.
Keep your tablets in a cool dry place where the temperature stays below 25°C.
Do not store IKOTAB or any other medicine in the bathroom or near a sink. Do not leave it on a window sill or in the car. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
Discard this medicine 30 days after opening the blister strip.
If your doctor tells you to stop taking this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Product description
What it looks like
IKOTAB 10 mg tablets are round and white scored on one side and marked '10' on the other side.
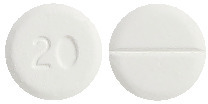
IKOTAB 20 mg tablets are round and white scored on one side and bearing the inscription '20' on the other side.
They are available in blister packs of 60 tablets. Each blister strip contains a desiccant.
Ingredients
IKOTAB contains 10 mg or 20 mg of nicorandil as the active ingredient.
The tablets also contain the following inactive ingredients:
- mannitol
- stearic acid
- croscarmellose sodium
- pregelatinised maize starch
This medicine does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
Distributor
IKOTAB is distributed in Australia by:
Alphapharm Pty Ltd
Level 1, 30 The Bond
30-34 Hickson Road
Millers Point NSW 2000
www.mylan.com.au
This leaflet was prepared in April 2021.
10 mg: AUST R 218690
20 mg: AUST R 218689
ikotab_cmi\apr21/00
Published by MIMS May 2021



 Chemical name: N-(2-hydroxyethyl)-nicotinamide nitrate (ester).
Chemical name: N-(2-hydroxyethyl)-nicotinamide nitrate (ester).