1 Name of Medicine
Isoprenaline hydrochloride.
2 Qualitative and Quantitative Composition
Isoprenaline Macure injection solution contains 1 mg of isoprenaline hydrochloride in 5 mL (1:5000).
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Clear, colourless or pale yellow solution for injection.
4.1 Therapeutic Indications
For mild or transient episodes of heart block that do not require electric shock or pacemaker therapy.
For serious episodes of heart block and Adams-Stokes attacks (except when caused by ventricular tachycardia or fibrillation). (See Section 4.3 Contraindications.)
For use in cardiac arrest until electric shock or pacemaker therapy, the treatments of choice, are available. (See Section 4.3 Contraindications.)
For bronchospasm occurring during anaesthesia.
As an adjunct to fluid and electrolyte replacement therapy and the use of other drugs and procedures in the treatment of hypovolaemic and septic shock, low cardiac output (hypoperfusion) states, congestive heart failure and cardiogenic shock. (See Section 4.4 Special Warnings and Precautions for Use.)
4.3 Contraindications
Use of isoprenaline hydrochloride is contraindicated in patients with tachyarrhythmias; tachycardia or heart block caused by digitalis intoxication; ventricular arrhythmias which require inotropic therapy; recent myocardial infarction; angina pectoris; hypersensitivity to isoprenaline or to any of the excipients in Section 6.1 List of Excipients.
4.4 Special Warnings and Precautions for Use
Isoprenaline hydrochloride infusions may produce an increase in myocardial work and oxygen consumption. These effects may be detrimental to myocardial metabolism and functioning in patients in cardiogenic shock secondary to coronary artery occlusion and myocardial infarction.
In a few patients, presumably with organic disease of the A-V node and its branches, isoprenaline hydrochloride has been reported, paradoxically, to precipitate Adams-Stokes seizures during normal sinus rhythm or transient heart block.
Adequate filling of the intravascular compartment by suitable volume expanders is of primary importance in most cases of shock, and should precede the administration of isoprenaline. In patients with normal cardiac function, determination of central venous pressure is a reliable guide during volume replacement. If evidence of hypoperfusion persists after adequate volume replacement, isoprenaline hydrochloride may be given.
In addition to the routine monitoring of systemic blood pressure, heart rate, urine flow, and electrocardiograph, the response to therapy should also be monitored by frequent determinations of the central venous pressure and blood gases. Patients in shock should be closely observed during isoprenaline hydrochloride administration. If the heart rate exceeds 110 beats per minute, it may be advisable to decrease the infusion rate or temporarily discontinue the infusion. Determinations of cardiac output and circulation time may also be helpful. Doses of isoprenaline hydrochloride sufficient to increase the heart rate to more than 130 beats per minute may induce ventricular arrhythmia. If the cardiac rate increases sharply, patients with angina pectoris may experience anginal pain until the cardiac rate decreases.
If ventricular hyperexcitability (extrasystoles, polymorphic extrasystoles or sustained ventricular tachycardia) should occur, the dosage should be reduced and the electrocardiogram monitored.
Appropriate measures should be taken to ensure adequate ventilation. Careful attention should be paid to acid-base balance and to the correction of electrolyte disturbances.
In cases of shock associated with bacteraemia, suitable antimicrobial therapy is, of course, imperative.
There are case reports of occasional fatal cardiac dysrhythmia and myocardial necrosis at autopsy as a result of intravenous isoprenaline. ECG changes and serum CPK-MB level elevation consistent with transient myocardial ischaemia and abnormal echocardiographic findings suggestive of myocardial dysfunction have been documented with the use of intravenous isoprenaline hydrochloride infusion for the treatment of severe asthma exacerbations in children. Care should be taken to ensure that oxygen is always administered during isoprenaline infusions in patients with asthma. Heart rate, blood pressure, arrhythmias and evidence of myocardial ischaemia by ECG should be monitored. Arterial blood gases should also be monitored carefully and PaO2 maintained above 60 torr. Where the ECG suggests myocardial ischaemia, cardiac enzymes including cardiac specific CPK-MB isoenzyme levels should be determined.
The dosage of isoprenaline hydrochloride should be carefully adjusted in patients with cardiovascular disorders (particularly coronary insufficiency, ischaemic heart disease, hypertension and arrhythmias), diabetes or hyperthyroidism. Administration of the medicinal product should be avoided in cases of uncontrolled hyperthyroidism.
Caution when used on patients under the effect of digitalis (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Caution in cases of convulsive disorders.
Caution when using in patients sensitive to sympathomimetic amines or who respond to sympathomimetic amines in an unusual manner.
Use in the elderly.
The dosage of isoprenaline hydrochloride should be carefully adjusted, particularly in the elderly and in patients with coronary insufficiency, ischaemic heart disease, hypertension, diabetes or hyperthyroidism, and in patients sensitive to sympathomimetic amines.
Paediatric use.
Dosage has not been established in children. (See Section 4.2 Dose and Method of Administration.)
Effects on laboratory tests.
No data available.4.5 Interactions with Other Medicines and Other Forms of Interactions
Isoprenaline hydrochloride should not be given simultaneously with adrenaline (epinephrine) or digitalis because both drugs are direct cardiac stimulants and their combined effects may induce serious arrhythmias. The drugs may, however, be administered alternately, provided a proper interval has elapsed between doses.
Isoprenaline hydrochloride should be used with caution, if at all, when potent inhalational anaesthetics such as halothane and cyclopropane are employed, because of their potential to sensitise the myocardium to the effects of sympathomimetic amines.
Isoprenaline should not be used with chlorpromazine or monoamine oxidase inhibitors since the effects of isoprenaline may be magnified.
Doxapram and MAOIs may cause a risk of severe hypertension. Hypertension may occur because of the high vasopressor effect of sympathomimetic vasoconstrictors (e.g. oxytocin).
Caution should be maintained when using continuous intravenous isoprenaline hydrochloride infusions in conjunction with intravenous methyl xanthines (aminophylline, theophylline) and intravenous corticosteroids. The use of isoprenaline hydrochloride with aminophylline and corticosteroids may be additive in cardiotoxic properties and can lead to myocardial necrosis and death. Severe cardiac symptoms of sympathetic overactivation, i.e. hypertension, tachycardia, arrhythmias, seizures, myocardial ischaemia, and fatal myocardial necrosis, have been reported.
Isoprenaline toxicity increases when administered at the same time as other cardiotonics or drugs stimulating the central nervous system (such as sympathomimetics or thyroid hormone products).
Isoprenaline may worsen cardiovascular side effects of tricyclic antidepressants such as imipramine.
The simultaneous administration of isoprenaline and drugs combined with sulphates, such as salicylamide, may exacerbate the pharmacological effects of isoprenaline.
Administration of entacapone may enhance the effect of isoprenaline.
Isoprenaline hydrochloride may increase the risk of ergotism, if given together with ergotamine.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
No data available.
(Category A)
Drugs which have been taken by a large number of pregnant women of childbearing age without any proven increase in the frequency of malformation or other direct or indirect harmful effects on the foetus having been observed.
There has been no clinical evidence of teratogenic effects attributable to isoprenaline hydrochloride in more than 25 years' use of the drug. However, before administration of any drug to pregnant women or lactating women, or women of childbearing potential, the expected benefit of the drug should be carefully weighed against the possible risk to the mother or child.
It is unknown whether isoprenaline hydrochloride is excreted into breast milk. Caution should be exercised in administering to a nursing mother.4.7 Effects on Ability to Drive and Use Machines
No specific studies have been conducted to assess the direct effect of Isoprenaline Macure on the ability to drive and use machines. However, adverse effects of isoprenaline hydrochloride include dizziness which could affect the ability to drive or use machines. See Section 4.8 Adverse Effects (Undesirable Effects).
4.8 Adverse Effects (Undesirable Effects)
Serious effects to isoprenaline hydrochloride are infrequent. The following effects, however, have been reported:
CNS.
Nervousness, headache, dizziness, restlessness, tension, fear of excitement and, rarely, tinnitus, light headedness and asthenia.
Cardiovascular.
Tachycardia, palpitations, angina, Adams-Stokes attacks, hypertension, hypotension, ventricular arrhythmias, tachyarrhythmias and pulmonary oedema. In patients with acute myocardial infarction, isoprenaline may increase the ischaemic injury to the myocardium.
Other.
Hot flashes, flushing of the skin, sweating, mild tremors, weakness and, rarely, nausea and vomiting.
These effects disappear quickly and usually do not require discontinuation of treatment with isoprenaline hydrochloride. No cumulative effects have been reported. Pulmonary oedema has been reported in a patient extremely intolerant of all sympathomimetic drugs.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.4.9 Overdose
The acute toxicity of isoprenaline hydrochloride in animals is much less than that of adrenaline. Excessive doses in animals or humans can cause a striking drop in blood pressure, and repeated large doses in animals may result in cardiac enlargement and focal myocarditis.
In cases of accidental overdosage, as evidenced mainly by tachycardia or other arrhythmias, palpitations, angina, hypotension or hypertension, reduce rate of administration or discontinue isoprenaline hydrochloride until the patient's condition stabilises. Blood pressure, pulse, respiration and ECG should be monitored.
Very cautious use of a non-selective beta receptor antagonist should be considered if symptoms are very severe, but close monitoring of airway function would be essential. It is not known whether isoprenaline hydrochloride is dialysable.
The oral LD50 of isoprenaline hydrochloride in mice is 3,850 mg/kg ± 1,190 mg/kg of pure drug in solution.
For information on the management of overdose, contact the Poisons Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
Isoprenaline hydrochloride acts primarily on the heart, and on the smooth muscle of bronchi, skeletal muscle vasculature and gastrointestinal tract.
Isoprenaline hydrochloride increases cardiac output due to its positive inotropic and chronotropic actions and by increasing venous return. With usual therapeutic doses, the increase in cardiac output is generally sufficient to maintain or increase systolic blood pressure. Intravenous infusion of Isoprenaline Macure also lowers peripheral vascular resistance. The diastolic pressure, therefore, may be expected to fall in normal individuals. Thus the mean pressure may be reduced. The rate of discharge of cardiac pacemakers is increased with isoprenaline hydrochloride.
Isoprenaline hydrochloride relaxes most smooth muscle, the most pronounced effect being on bronchial and gastrointestinal smooth muscle. It produces marked relaxation in the smaller bronchi and may even dilate the trachea and main bronchi past the resting diameter.
Clinical trials.
No data available.
5.2 Pharmacokinetic Properties
Absorption.
The half-life of isoprenaline hydrochloride is brief, lasting only a few minutes following intravenous administration and up to 2 hours after subcutaneous administration.
Metabolism.
Isoprenaline is metabolised by catechol-ortho-methyl transferase, primarily in the liver. The major metabolite after intravenous administration is 3-O-methylisoprenaline, which is reported to have weak beta-adrenergic blocking activity, and its conjugates.
Excretion.
The metabolites are excreted through the kidneys.
5.3 Preclinical Safety Data
Genotoxicity.
No data available.
Carcinogenicity.
No data available.6 Pharmaceutical Particulars
6.1 List of Excipients
Sodium chloride, disodium edetate, sodium citrate dihydrate, citric acid monohydrate, water for injections, sodium hydroxide (for pH adjustment), hydrochloric acid (for pH adjustment).
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine. Isoprenaline Macure can be mixed with sodium chloride 9 mg/mL (0.9 %) solution for injection or glucose 50 mg/mL (5 %) solution for injection.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store refrigerated (2°C - 8°C).
It is recommended that, to reduce microbiological contamination hazards, the diluted solutions should be prepared immediately prior to use and infusion commenced as soon as practicable after preparation of the mixture. Keep diluted solution at 25°C for not more than 24 hours. The diluted infusion solution should be used within 24 hours and any residue discarded.
6.5 Nature and Contents of Container
Isoprenaline hydrochloride injection 1 mg/5 mL clear, Type I amber glass ampoules: packaged into cartons containing 5 x 5 mL ampoules.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure.
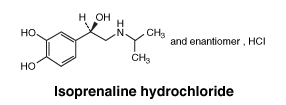
CAS number.
51-30-9.7 Medicine Schedule (Poisons Standard)
Schedule 4 (Prescription Only Medicine).
Summary Table of Changes






