1 Name of Medicine
Metoclopramide hydrochloride anhydrous.
2 Qualitative and Quantitative Composition
Chemical name: N-(diethyl-aminoethyl)-2-methoxy-4-amino-5-chlorbenzamide monohydrochloride monohydrate.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
5 mg tablets.
Metoclopramide-WGR film coated tablets containing metoclopramide hydrochloride 5 mg are white to off-white, circular, biconvex film-coated tablets plain on both sides.
10 mg tablets.
Metoclopramide-WGR film coated tablets containing metoclopramide hydrochloride 10 mg are white to off-white, circular, biconvex film-coated tablets with break line on both sides.4.1 Therapeutic Indications
Adults (20 years and over).
As an adjunct to X-ray examination of the stomach and duodenum.
To assist in intestinal intubation.
To control nausea and vomiting associated with the following conditions: intolerance to essential drugs possessing emetic properties; uraemia; radiation sickness; malignant disease; postoperative vomiting; labour; infectious diseases. There is no clear benefit in motion sickness or other labyrinth disturbances.
Metoclopramide has been found useful in the management of gastric retention after gastric surgery.
Metoclopramide may be useful in the treatment of diabetic gastroparesis of mild to moderate severity. Once control of diabetes has been established by diet and/or insulin, metoclopramide should be discontinued.
Young adults aged 15-19 years.
The use of Metoclopramide in young adults 15-19 years should be restricted to the following situations and only used as second line therapy:
Severe intractable vomiting of known cause;
Vomiting associated with radiotherapy and intolerance to cytotoxic drugs;
As an aid to gastrointestinal intubation.4.2 Dose and Method of Administration
Metoclopramide injection is unavailable in this brand, however this formulation is available in other brands. Information obtained from this formulation is included in the PI for prescriber information. Where correct dosing required this formulation, refer to the specific product information for these formulations for complete dosage and administration instructions.
Tablets should not be used in children less than 15 years.
Patients with normal renal and hepatic function.
The dosage recommendations given below should be strictly adhered to if side effects of the dystonic type are to be avoided. Total daily dosage of Metoclopramide-WGR Tablets, especially children and for young adults, should not normally exceed 0.5 mg/kg bodyweight with a maximum of 30 mg daily.
Metoclopramide should only be used after careful examination to avoid masking an underlying disorder, e.g. cerebral irritation. Maximum recommended treatment duration is 5 days in all age groups.
Medical indications.
Oral. Adults: 20 years and over.
10 mg three times daily.
Elderly patients.
As for adults. To avoid adverse reactions, adhere strictly to dosage recommendations and where prolonged therapy is considered necessary, patients should be regularly reviewed.
Young adults: 15-20 years.
5 to 10 mg three times daily, commencing at the lower dosage and used as second line therapy only.
Diagnostic indications.
A single dose of Metoclopramide-WGR Tablets may be given 5 to 10 minutes before the examination. Subject to bodyweight considerations, the following dosages are recommended:
Adults: 20 years and over.
10 to 20 mg.
Young adults: 15-19 years.
10 mg.
Patients with impaired renal and hepatic function: In patients with clinically significant degrees of renal or hepatic impairment, clearance of Metoclopramide-WGR Tablets is likely to be reduced. It is suggested that therapy be initiated at half the recommended dose. Subsequent dosage will depend on individual clinical response.4.3 Contraindications
Metoclopramide should not be used whenever stimulation of gastrointestinal motility might be dangerous, e.g. in the presence of gastrointestinal haemorrhage, mechanical obstruction, or perforation.
Phaeochromocytoma because the drug may cause a hypertensive crisis, probably due to release of catecholamines from the tumour. Such hypertensive crises may be controlled by phentolamine.
Known hypersensitivity or intolerance to the drug.
Porphyria.
Epilepsy as Metoclopramide-WGR may increase the frequency and severity of seizures.
Metoclopramide should not be administered to patients receiving other drugs which are likely to cause extrapyramidal reactions, since the frequency and severity of extrapyramidal reactions may be increased.
Metoclopramide tablets should not be used in children below 15 years of age.
4.4 Special Warnings and Precautions for Use
Persistent tardive dyskinesia.
Tardive dyskinesia may appear in some patients on long-term therapy or may appear after drug therapy has been discontinued. The risk appears to be greater in elderly patients on high dose therapy, especially females. The symptoms are persistent and can oftentimes appear to be irreversible. The syndrome is characterised by rhythmical involuntary movement of the tongue, face, mouth, or jaw (e.g. protrusion of tongue, puffing of cheeks, puckering of mouth, chewing movements). Sometimes these may be accompanied by involuntary movement of extremities. There is no known effective treatment for tardive dyskinesia, however, in some patient's symptoms may lessen or resolve after metoclopramide hydrochloride treatment is stopped. Antiparkinson agents usually do not alleviate the symptoms of this syndrome.
Although the risk of tardive dyskinesia with metoclopramide has not been extensively studied, one published study reported a tardive dyskinesia prevalence of 20% among patients treated for at least 3 months. Both the risk of developing the syndrome and the likelihood that it will become irreversible are believed to increase with the duration of treatment and the total cumulative dose.
Metoclopramide hydrochloride therapy should routinely be discontinued in patients who develop signs or symptoms of tardive dyskinesia. It has been suggested that fine vermicular movements of the tongue may be an early sign of the syndrome, and, if the medication is stopped at that time, the syndrome may not develop. Tardive dyskinesia may remit, partially or completely, within several weeks to months after metoclopramide is withdrawn. Metoclopramide itself, however, may suppress (or partially suppress) the signs of tardive dyskinesia, thereby masking the underlying disease process. The effect of this symptomatic suppression upon the long-term course of the syndrome is unknown. Therefore, metoclopramide should not be used for the symptomatic control of tardive dyskinesia.
Prolonged treatment (greater than 12 weeks) with metoclopramide should be avoided in all but rare cases where therapeutic benefit is thought to outweigh the risks to the patient of developing tardive dyskinesia.
Care should be exercised in patients being treated with other centrally active drugs.
Since extrapyramidal symptoms may occur with both metoclopramide hydrochloride and neuroleptics such as phenothiazines, care should be exercised in the event of both drugs being prescribed concurrently. (See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). The frequency and severity of seizures or extrapyramidal reactions may be increased in epileptic patients given Metoclopramide.
Dystonic reactions occur in approximately 1% of patients given metoclopramide hydrochloride. These occur more frequently in children and young adults and may occur after a single dose.
Neuroleptic Malignant Syndrome has been reported with metoclopramide hydrochloride in combination with neuroleptics as well as with metoclopramide hydrochloride monotherapy (see Section 4.8 Adverse Effects (Undesirable Effects)).
Prolactin levels.
Metoclopramide hydrochloride elevates prolactin levels, and the elevation persists during chronic administration (see Section 4.8 Adverse Effects (Undesirable Effects)). Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin dependent in vitro, a factor of potential importance if the prescription of metoclopramide hydrochloride is contemplated in a patient with previously detected breast cancer. Although disturbances such as galactorrhoea, amenorrhoea, gynaecomastia, and impotence have been reported with prolactin elevating drugs, the clinical significance of elevated serum prolactin levels is unknown for most patients. An increase in mammary neoplasms has been found in rodents after chronic administration of prolactin stimulating neuroleptic drugs. Neither clinical studies nor epidemiological studies conducted to date, however, have shown an association between chronic administration of these drugs and mammary tumorigenesis; the available evidence is too limited to be conclusive at this time.
Other.
Following operations such as pyloroplasty or gut anastomosis, metoclopramide hydrochloride therapy should be withheld for three or four days as vigorous muscular contractions may not help healing.
Special care should be taken in cases of severe renal insufficiency (see Section 4.2 Dose and Method of Administration).
The symptomatic relief provided by metoclopramide hydrochloride may delay recognition of serious disease. It should not be prescribed until diagnosis has been established and should not be substituted for appropriate investigation of the patient's symptoms.
If vomiting persists in a patient receiving metoclopramide hydrochloride, the patient should be reassessed to exclude the possibility of an underlying disorder e.g. cerebral irritation.
Patients should be cautioned about engaging in activities requiring mental alertness for a few hours after the drug has been administered.
Metoclopramide induced depression has been reported in patients without a prior history of depression. Metoclopramide should be given to patients with a prior history of depression only if the expected benefits outweigh the potential risks.
Metoclopramide should be used with caution in patients with hypertension as intravenously administered metoclopramide has been shown to release catecholamines.
Metoclopramide can exacerbate parkinsonian symptoms, therefore it should be used with caution, if at all, in patients with parkinsonian syndrome (see Section 4.8 Adverse Effects (Undesirable Effects)).
Identified precautions.
No data available.
Use in hepatic impairment.
In patients with clinically significant degrees of hepatic impairment, clearance of Metoclopramide is likely to be reduced (see Section 4.2 Dose and Method of Administration).
Use in renal impairment.
In patients with clinically significant degrees of renal impairment, clearance of Metoclopramide is likely to be reduced.
Special care should be taken in cases of severe renal insufficiency (see Section 4.2 Dose and Method of Administration).
Use in the elderly.
To avoid adverse reactions adhere strictly to dosage recommendations and where prolonged therapy is considered necessary, patients should be regularly reviewed (see Section 4.2 Dose and Method of Administration).
Paediatric use.
Metoclopramide tablets is contraindicated in children less than 15 years of age. Metoclopramide should not be given to children unless a clear indication has been established for its use, because of the higher incidence of adverse reactions in this age group.
Effects on laboratory tests.
No data available.4.5 Interactions with Other Medicines and Other Forms of Interactions
The effects of metoclopramide hydrochloride on gastrointestinal motility are antagonised by anticholinergic drugs and narcotic analgesics. Additive sedative effects can occur when metoclopramide hydrochloride is given with alcohol, sedatives, hypnotics, narcotics, or tranquillisers.
Since metoclopramide hydrochloride accelerates abnormally slow gastric and small bowel peristaltic activity, it may change absorption of orally administered drugs. The absorption of drugs from the small bowel may be accelerated (e.g. paracetamol, tetracycline, levodopa), whereas absorption of drugs from the stomach may be diminished (e.g. digoxin).
Metoclopramide may cause extrapyramidal symptoms in some patients. Therefore, when metoclopramide is used concomitantly with other drugs that are likely to cause extrapyramidal reactions (e.g. neuroleptics such as phenothiazines), caution should be exercised.
The decrease in gastric emptying time caused by metoclopramide may increase the bioavailability of cyclosporin. Monitoring of cyclosporin concentrations may be necessary.
When metoclopramide is given concurrently with suxamethonium the recovery time is prolonged.
Since metoclopramide influences the delivery of food to the intestine and thus the rate of its absorption, the administration of metoclopramide may result in poor diabetic control in some patients. Therefore, adjustment in, or timing of, insulin dosage may be necessary in insulin-controlled diabetics.
The finding that metoclopramide releases catecholamines in patients with essential hypertension suggests that it should be used cautiously, if at all, in patients receiving monoamine oxidase inhibitors.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
No data available.
(Category A)
Adequate human data on use during pregnancy are not available.
Adequate human data on use during lactation and adequate animal reproduction studies are not available.4.7 Effects on Ability to Drive and Use Machines
Patients should be cautioned about engaging in activities requiring mental alertness for a few hours after the drug has been administrated.
4.8 Adverse Effects (Undesirable Effects)
The most frequent adverse reactions to metoclopramide hydrochloride are restlessness, drowsiness, fatigue, and lassitude, which occur in approximately 10% of patients.
Less frequently, insomnia, headache, dizziness, nausea, or bowel disturbances may occur. Rare (less than 1 in 1,000) cases of acute depression have been reported. Anxiety or agitation may occur especially after rapid injection.
A single instance of supraventricular tachycardia following intramuscular administration has been reported. There have been very rare (less than 1 in 10,000) cases of abnormalities of cardiac conduction (such as bradycardia and heart block) in association with intravenous metoclopramide. Atrial fibrillation (AF), oedema, tachycardia and palpitations have been associated with the use of metoclopramide.
Although uncommon at normal dosage, various extrapyramidal reactions to metoclopramide hydrochloride, usually of the dystonic type, have been reported. Reactions include spasm of the facial muscles, trismus, rhythmic protrusion of the tongue, a bulbar type of speech, spasm of the extraocular muscles including oculogyric crises, unnatural positioning of the head and shoulders and opisthotonos. There may be a generalised increase in muscle tone. The majority of reactions occur within 36 hours of starting treatment and the effects usually disappear within 24 hours of withdrawal of the drug, however, close observation is required and in cases of more severe reactions, an antiparkinson drug such as benztropine or an anticholinergic antihistamine such as diphenhydramine should be given. A fatal dystonic reaction has been reported in a patient who received hexamethylmelamine, cisplatin and high dose metoclopramide. A fatal cardiorespiratory arrest has occurred in at least one patient with an acute dystonic reaction.
Tardive dyskinesia, which may be persistent, has been reported particularly in elderly patients undergoing long-term therapy with metoclopramide hydrochloride.
Very rare (less than 1 in 10,000) occurrences of the Neuroleptic Malignant Syndrome have been reported. This syndrome is potentially fatal and comprises hyperpyrexia, altered consciousness, muscle rigidity, autonomic instability and elevated levels of CPK and must be treated urgently (recognised treatments include dantrolene and bromocriptine). Metoclopramide hydrochloride should be stopped immediately if this syndrome occurs.
Parkinsonian symptoms, including tremor, rigidity, bradykinesia and akinesia, occur rarely in patients receiving metoclopramide but may be associated with usual or excessive doses or with decreased renal function.
There have been isolated reports of hypersensitivity reactions (such as urticaria, maculopapular rash) in patients receiving metoclopramide.
Methaemoglobinaemia has also been reported. There have been a few cases of neutropenia, leucopenia and agranulocytosis generally without clear cut relationship to metoclopramide.
Sulfhaemoglobinaemia in adults.
Hyperthermia has also been observed.
Raised serum prolactin levels have been observed during metoclopramide therapy; this effect is similar to that noted with many other compounds. Galactorrhoea and breast enlargement have also been observed during metoclopramide therapy.
Respiratory failure, secondary to dystonic reaction, acute asthmatic symptoms of wheezing and dyspnoea may occur.
Urinary incontinence and frequency, sexual dysfunction, priapism and muscle spasm may also occur.
Rarely, cases of hepatotoxicity, characterised by such findings as jaundice and altered liver function tests, when metoclopramide was administered with other drugs with known hepatotoxic potential.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.4.9 Overdose
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
Symptoms.
Overdose of metoclopramide may be expected to produce effects that are extensions of common adverse reactions: drowsiness, disorientation and extrapyramidal side effects. Very rarely AV block has been observed. Other reported effects associated with metoclopramide overdose have included feelings of anxiety or restlessness, headache, vertigo, nausea, vomiting, constipation, weakness, hypotension and xerostomia.
Management.
Management of overdosage consists of close observation and supportive therapy. Antiparkinson and antihistamine/anticholinergic drugs such as diphenhydramine hydrochloride have effectively controlled extrapyramidal reactions. Hemodialysis appears ineffective in removing metoclopramide. Similarly, continuous ambulatory peritoneal dialysis does not remove significant amounts of the drug.5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
Metoclopramide hydrochloride stimulates motility of the upper gastrointestinal tract without stimulating gastric, biliary, or pancreatic secretions.
Its mode of action is unclear. It seems to sensitise tissues to the action of acetylcholine. The effect of metoclopramide hydrochloride on motility is not dependent on intact vagal innervation, but it can be abolished by anticholinergic drugs.
Metoclopramide hydrochloride increases the tone and amplitude of gastric (especially antral) contractions, relaxes the pyloric sphincter and the duodenal bulb, and increases peristalsis of the duodenum and jejunum resulting in accelerated gastric emptying and intestinal transit. It increases the resting tone of the lower oesophageal sphincter. It has little, if any effect on the motility of the colon or gall bladder.
Metoclopramide hydrochloride has dopamine antagonist activity. Like the phenothiazines and related drugs, which are also dopamine antagonists, metoclopramide hydrochloride produces sedation and may produce extra-pyramidal reactions (see Section 4.4 Special Warnings and Precautions for Use).
Metoclopramide hydrochloride inhibits the central and peripheral effects of apomorphine, induces release of prolactin and causes a transient increase in circulating aldosterone levels.
Clinical trials.
No data available.
5.2 Pharmacokinetic Properties
Absorption.
The onset of pharmacological action is 1 to 3 minutes following an intravenous dose, 10 to 15 minutes following intramuscular administration, and 30 to 60 minutes following an oral dose; pharmacological effects persist for 1 to 2 hours.
There is marked variability in peak plasma concentrations of metoclopramide hydrochloride after oral administration, which appears to be due to interindividual differences in first-pass metabolism.
Distribution.
Plasma protein binding is 13% to 22%.
Metabolism.
80% of the drug is excreted in the urine in the first 24 hours, approximately half as the glucuronide and sulfate conjugates and half as unchanged drug.
Excretion.
Elimination half-life varies in different studies from 2.5 to 5 hours. Impaired renal function results in reduced clearance of metoclopramide hydrochloride and an increased half-life (15 hours).
5.3 Preclinical Safety Data
Genotoxicity.
No data available.
Carcinogenicity.
No data available.6 Pharmaceutical Particulars
6.1 List of Excipients
Metoclopramide-WGR tablets also contain the excipients microcrystalline cellulose, colloidal anhydrous silica, maize starch, stearic acid and pregelatinised maize starch. The coating for the tablets consists of hypromellose, macrogol 6000, titanium dioxide and purified talc.
See Section 2 Qualitative and Quantitative Composition.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Tablets should be stored below 25°C. Protect from light.
6.5 Nature and Contents of Container
Metoclopramide-WGR 10 mg and 5 mg tablets are packed in clear PVDC coated PVC/aluminium blister packs and are available in pack sizes of 10, 20, 25, 30, 50, 60 100, 125 or 150 tablets.
Metoclopramide-WGR 10 mg tablets are also available in 100's HDPE bottle pack with polypropylene child resistant closure and 500's tablets HDPE bottle pack with polypropylene screw cap.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure.
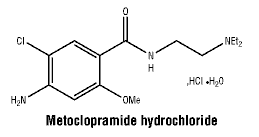 C14H22ClN3O2, HCl, H2O.
C14H22ClN3O2, HCl, H2O.
Chemical Name: N-(diethyl-aminoethyl)-2-methoxy-4-amino-5-chlorbenzamide monohydrochloride monohydrate.
Molecular weight: 354.3.
CAS number.
54143-57-6.7 Medicine Schedule (Poisons Standard)
S4 - Prescription only Medicines.
Summary Table of Changes



 C14H22ClN3O2, HCl, H2O.
C14H22ClN3O2, HCl, H2O.