What is in this leaflet
This leaflet answers some common questions about MINIRIN Injection.
It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you been given MINIRIN Injection against the benefits they expect it will have for you.
If you have any concerns about this medicine you will be given, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What MINIRIN Injection is given for
The active ingredient, desmopressin acetate in MINIRIN Injection is a synthetic version of a naturally occurring substance produced in the brain called vasopressin.
It has a number of different actions in the body including an action on the kidneys to reduce the amount of urine produced. This means that MINIRIN injection can be used for several different conditions including:
- cranial diabetes insipidus (CDI), large amounts of urine being produced day and night and constant thirst where intranasal administration is inconvenient
- as a diagnostic test to establish if the kidneys have the ability to concentrate urine in adults.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another reason.
This medicine is not addictive.
It is available only with a doctor's prescription.
This medicine is not expected to affect your ability to drive a car or operate machinery.
Before you are given MINIRIN Injection
When you must not be given it
MINIRIN Injection must not be given to you if you have an allergy to:
- any medicine containing desmopressin or any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include:
- shortness of breath, wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
You must not be given MINIRIN Injection if you:
- suffer from polydipsia (have excessive thirst and requiring increased fluid intake) or psychogenic polydipsia (psychologically-caused increased thirst and increased fluid intake
- have cardiac insufficiency (heart failure in which the heart is not able to pump enough blood throughout the body resulting in shortness of breath, swelling of feet or legs due to fluid build-up)
- have low levels of sodium in your bloodstream
- have SIADH (hormone secretion disorder where there is an overproduction of a hormone causing fluid retention, resulting in weakness, tiredness or confusion).
- have a history of a condition marked by severe pain in the chest, often also spreading to the shoulders, arms and neck, owing to an inadequate supply to the heart (angina pectoris).Have Von Willebrand disease type IIB (a Bleeding disorder).
Do not breast-feed if you are taking this medicine. MINIRIN Injection is not recommended while you are breast-feeding.
Do not give this medicine to a child under the age of 6 years. Safety and effectiveness in children younger than 6 years have not been established.
Do not take this medicine after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking this medicine, talk to your doctor.
Before it is given to you
Tell your doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any of the following medical conditions:
- a known allergy to anti-diuretic hormone (ADH)
- heart or blood vessel disease or any other disease for which you take diuretics (fluid tablets)
- low blood pressure
- cystic fibrosis or any other disease which causes fluid or salt imbalance
- any disease of the blood clotting cells
- serious problems with bladder function or with passing urine.
Tell your doctor if you are pregnant or plan to become pregnant or are breast-feeding.
MINIRIN Injection should only be given to a pregnant woman if it is needed. Your doctor can discuss with you the risks and benefits involved.
It is recommended that you do not breastfeed while given MINIRIN Injection.
If you have not told your doctor about any of the above, tell him/her before you will be given MINIRIN Injection.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and MINIRIN Injection may interfere with each other. These include:
- tricyclic antidepressants, which are medicines used to treat e.g. depression (such as clomipramine, imipramine, desipramine)
- selective serotonin reuptake inhibitors (SSRIs), which are medicines used to treat e.g. depression or anxiety (such as citalopram, paroxetine, sertraline)
- chlorpromazine, which is an anti-psychotic medicinal product used to treat e.g. schizophrenia
- carbamazepine, which is used to treat e.g. bipolar disorder and epilepsy
- antidiabetic medicinal products used for type II diabetes (medicines in the sulfonylurea group), particularly chlorpropamide
- medicines used to treat high blood pressure and some other conditions (ACE inhibitors or angiotensin receptor blockers e.g. enalapril, perindopril, irbesartan etc.)
- non-steroidal anti-inflammatory drugs (NSAIDs), which are medicinal products used for the treatment of pain and inflammation (e.g. aspirin and ibuprofen).
These medicines may be affected by MINIRIN Injection or may affect how well it works. You may need different amounts of your medicines, or you may need to take different medicines.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while you have been given this medicine.
How MINIRIN is given
MINIRIN may be given by injection into a muscle or into a vein (intravenously), depending on its use.
MINIRIN Injection is not intended for self-administration.
How much MINIRIN Injection you will be given
The dose of MINIRIN Injection prescribed by your doctor will vary depending on the condition being treated and your response to the treatment.
Cranial diabetes insipidus
The average daily dose for adults is 1 to 4 micrograms by injection. The dose for children will be up to 0.4 micrograms daily. The dose you receive will be adjusted to suit personal requirement. MINIRIN Injection is usually given in two doses each day. Sometimes a single daily dose is sufficient to control your condition.
Test the ability of the kidneys to concentrate urine
Adults will receive a single dose of up to 4 micrograms at any one time.
When MINIRIN Injection is given
Cranial diabetes insipidus
You will be given MINIRIN Injection at times specified by your doctor.
Test the ability of the kidneys to concentrate urine
Your doctor will advise you.
How long MINIRIN is given
Cranial diabetes insipidus
MINIRIN Injection can prevent or control the thirst and frequent urination associated with CDI. You will be less thirsty and urinate a smaller volume less often.
It is likely that you will need to be given MINIRIN Injection or other forms of MINIRIN for the rest of your life.
This medicine helps to control your condition, but does not cure it. It is important to keep taking your medicine even if you feel well.
Test the ability of the kidneys to concentrate urine
Your doctor will explain the details of the test.
What to expect
Individuals will vary greatly in their response to MINIRIN Injection and you may not feel any effect. You will receive regular monitoring to check on your body's response to MINIRIN Injection.
If you have a defect in your blood clotting cells, your skin bleeding time will be monitored before surgery to determine whether you are at high risk of blood loss.
If you are given too much (overdose)
It is unlikely that you will be given too much MINIRIN Injection.
Immediately telephone your doctor or the Poisons Information Centre (telephone 13 11 26) for advice, or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have taken too much MINIRIN Injection. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
Symptoms of an overdose may include confusion, drowsiness, continuing headache, nausea or vomiting, rapid weight gain due to a build-up of water in the body, or, in severe cases, convulsions.
The signs of overdosage can be treated by restoring your body's fluid balance, lowering the dose or giving MINIRIN Injection less often or it may be stopped completely.
While you are being given MINIRIN Injection
Things you must do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are being given MINIRIN Injection.
Tell all doctors, dentists and pharmacists who are treating you that you are being given MINIRIN Injection, especially if you are being started on any new medicines.
Tell your doctor immediately if you become pregnant while being given MINIRIN Injection. Your doctor can discuss with you the risks of using it while you are pregnant.
If you are going to have surgery, tell the surgeon or anaesthetist that you are being given this medicine. It may affect other medicines used during surgery.
If you are about to have any blood tests, tell your doctor that you are being given this medicine. It may interfere with the results of some tests.
Keep all of your doctor’s appointments so that your progress can be checked. Your doctor may do some tests from time to time to make sure the medicine is working and to prevent unwanted side effects.
Things you must not do
MINIRIN Injection should not be given to you to treat any other complaints unless your doctor tells you to do so.
Things to be careful of
Cranial diabetes insipidus
Carefully follow your doctor’s instruction about fluid intake. It is very important to keep your body water in balance, so that you do not let yourself get too thirsty or drink too much fluid.
Test the ability of the kidneys to concentrate urine
You must avoid drinking fluids from one hour before taking MINIRIN Injection until at least eight hours after administration of the spray. Over this period, drink no more than a few sips of water or other fluids. This is because a high fluid intake during this period can increase the chance that you will feel unwell (e.g. headache, nausea, dizziness).
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are being given MINIRIN Injection.
This medicine helps most people who are given it but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects.
If you are over 60 years of age you may have an increased chance of getting side effects.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor or pharmacist if you notice any of the following and they worry you:
- facial pressure or pain
- headache
- increased body temperature (fever)
- inflammation of the stomach and intestines
- stomach pain or nausea
- fatigue or tiredness.
The above list includes the more common side effects of your medicine. They are usually mild and short-lived.
Tell your doctor as soon as possible if you notice any of the following:
- emotional, behavioural or visual disturbances
- fast heart rate
- low blood pressure, feeling dizziness or lightheaded
- allergic reactions including skin rash or more general reactions.
The above list includes serious side effects which may require medical attention. Serious side effects are rare.
If you notice any of the following, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- confusion or drowsiness
- continuing headache
- nausea or vomiting
- rapid weight gain, which may be due to a build-up of water in the body
- convulsions, fitting and blackouts.
The above list includes very serious side effects. You may need urgent medical attention or hospitalisation. These side effects are very rare.
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
After MINIRIN Injection is given
Storage
MINIRIN Injection is usually stored in the hospital pharmacy or in the ward.
Keep MINIRIN Injection in a refrigerator at a temperature between 2°C and 8 °C. Do not freeze. Keep it in its original packaging and protect it from light. If you store the medicine out of its original packaging it may not keep well.
Do not store MINIRIN Injection, or any other medicine, in the bathroom or near a sink. Do not leave it on a window sill or in the car. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop taking this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Product description
What it looks like
MINIRIN Injection contains 4 micrograms of the active ingredient, desmopressin acetate, in 1mL solution. It is a clear colourless solution for injection packed in 1 mL ampoules. The ampoules are available in boxes of 10.
Ingredients
MINIRIN Injection also contains the inactive ingredients:
- sodium chloride
- hydrochloric acid (to adjust the pH)
- water for injections.
This medicine does not contain sucrose, gluten, tartrazine or any other azo dyes.
Sponsor
MINIRIN Injection is supplied in Australia by:
Ferring Pharmaceuticals Pty Ltd
Suite 2, Level 1, Building 1
20 Bridge Street
Pymble, NSW 2073
Australia.
AUST R 40689 - MINIRIN desmopressin acetate 4 microgram/1mL injection ampoule
This leaflet was prepared in December 2018.
#155-v5B.
MINIRIN and FERRING are registered trademarks of Ferring B.V.
Published by MIMS February 2019


 Rare post-marketing cases of deep vein thrombosis, cerebrovascular accident/disorder (stroke), cerebral thrombosis, pulmonary embolism, myocardial infarction, angina pectoris and chest pain have been reported in patients treated with desmopressin. Due to confounding factors and/or missing information, a causal relationship with Minirin/ Octostim Injections has not been established/ confirmed.
Rare post-marketing cases of deep vein thrombosis, cerebrovascular accident/disorder (stroke), cerebral thrombosis, pulmonary embolism, myocardial infarction, angina pectoris and chest pain have been reported in patients treated with desmopressin. Due to confounding factors and/or missing information, a causal relationship with Minirin/ Octostim Injections has not been established/ confirmed.
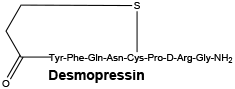 Synonyms of desmopressin: DDAVP.
Synonyms of desmopressin: DDAVP.