1 Name of Medicine
Tirzepatide.
2 Qualitative and Quantitative Composition
Single-dose vial and pre-filled pen (autoinjector).
Mounjaro tirzepatide 2.5 mg/0.5 mL solution for injection vial and pre-filled pen.
Each vial and pre-filled pen contains tirzepatide 2.5 mg in 0.5 mL solution.
Mounjaro tirzepatide 5 mg/0.5 mL solution for injection vial and pre-filled pen.
Each vial and pre-filled pen contains tirzepatide 5 mg in 0.5 mL solution.
Mounjaro tirzepatide 7.5 mg/0.5 mL solution for injection vial and pre-filled pen.
Each vial and pre-filled pen contains tirzepatide 7.5 mg in 0.5 mL solution.
Mounjaro tirzepatide 10 mg/0.5 mL solution for injection vial and pre-filled pen.
Each vial and pre-filled pen contains tirzepatide 10 mg in 0.5 mL solution.
Mounjaro tirzepatide 12.5 mg/0.5 mL solution for injection vial and pre-filled pen.
Each vial and pre-filled pen contains tirzepatide 12.5 mg in 0.5 mL solution.
Mounjaro tirzepatide 15 mg/0.5 mL solution for injection vial and pre-filled pen.
Each vial and pre-filled pen contains tirzepatide 15 mg in 0.5 mL solution.
Multiple-dose pre-filled pen (KwikPen).
Mounjaro KwikPen tirzepatide 4.17 mg/mL solution for injection multiple-dose pre-filled pen.
Each multiple-dose pre-filled pen delivers four 0.6 mL doses containing 2.5 mg tirzepatide.
Mounjaro KwikPen tirzepatide 8.33 mg/mL solution for injection multiple-dose pre-filled pen.
Each multiple-dose pre-filled pen delivers four 0.6 mL doses containing 5 mg tirzepatide.
Mounjaro KwikPen tirzepatide 12.5 mg/mL solution for injection multiple-dose pre-filled pen.
Each multiple-dose pre-filled pen delivers four 0.6 mL doses containing 7.5 mg tirzepatide.
Mounjaro KwikPen tirzepatide 16.67 mg/mL solution for injection multiple-dose pre-filled pen.
Each multiple-dose pre-filled pen delivers four 0.6 mL doses containing 10 mg tirzepatide.
Mounjaro KwikPen tirzepatide 20.83 mg/mL solution for injection multiple-dose pre-filled pen.
Each multiple-dose pre-filled pen delivers four 0.6 mL doses containing 12.5 mg tirzepatide.
Mounjaro KwikPen tirzepatide 25 mg/mL solution for injection multiple-dose pre-filled pen.
Each multiple-dose pre-filled pen delivers four 0.6 mL doses containing 15 mg tirzepatide.
For the full list of excipients, see Section 6.1 List of Excipients.3 Pharmaceutical Form
Solution for injection.
Mounjaro is a clear, colourless to slightly yellow, sterile solution for subcutaneous administration. The single dose vial and pre-filled pen are preservative-free. The multiple-dose pre-filled pen contains preservatives.
4.1 Therapeutic Indications
Type 2 diabetes mellitus.
Mounjaro is indicated for the treatment of adults with insufficiently controlled type 2 diabetes mellitus as an adjunct to diet and exercise as monotherapy when metformin is not tolerated or contraindicated; in addition to other medicinal products for the treatment of type 2 diabetes.
Chronic weight management.
Mounjaro is indicated as an adjunct to a reduced-calorie diet and increased physical activity for chronic weight management, including weight loss and weight maintenance, in adults with an initial body mass index (BMI) of:
≥ 30 kg/m2 (obesity) or
≥ 27 kg/m2 to < 30 kg/m2 (overweight) in the presence of at least one weight-related comorbid condition (e.g. hypertension, dyslipidaemia, obstructive sleep apnoea, cardiovascular disease, prediabetes or type 2 diabetes mellitus).
Obstructive sleep apnoea (OSA).
Mounjaro is indicated for the treatment of moderate to severe obstructive sleep apnoea in adults with obesity.4.2 Dose and Method of Administration
Use in adults (≥ 18 years).
The starting dose of tirzepatide is 2.5 mg once weekly.
After 4 weeks, increase the dose to 5 mg once weekly.
If needed, dose increases can be made in 2.5 mg increments after a minimum of 4 weeks on the current dose.
The recommended doses are 5 mg, 10 mg and 15 mg.
The 2.5 mg, 7.5 mg and 12.5 mg are not maintenance doses.
The maximum dose of tirzepatide is 15 mg once weekly.
Available doses are 2.5 mg, 5 mg, 7.5 mg, 10 mg, 12.5 mg and 15 mg. (See Section 2 Qualitative and Quantitative Composition.)
The Mounjaro KwikPen is a variable dosing device and there is potential for underdosing in patients if used incorrectly. Please refer to the Instructions for Use leaflet in the carton and ensure the dose knob on the Mounjaro KwikPen device is turned to the '1' icon to inject a full dose.
Self-monitoring of blood glucose is not needed to adjust the dose of tirzepatide.
When tirzepatide is added to existing metformin and/or sodium-glucose co-transporter 2 inhibitor (SGLT2i) therapy, the current dose of metformin and/or SGLT2i can be continued.
When tirzepatide is added to existing therapy of a sulfonylurea and/or insulin, a reduction in the dose of sulfonylurea or insulin may be considered to reduce the risk of hypoglycaemia. Blood glucose self-monitoring is necessary to adjust the dose of sulfonylurea and insulin. A stepwise approach to insulin reduction is recommended. (See Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects)).
Missed dose.
If a dose is missed, it should be administered as soon as possible.
If there are fewer than 3 days until the next regularly scheduled dose, skip the missed dose and administer the next dose on the regularly scheduled day. Patients can then resume their regular once weekly dosing schedule.
Changing the weekly dosing schedule.
The day of weekly administration can be changed, if necessary, as long as the time between two doses is at least 3 days (72 hours).
Special population.
Use in the elderly (≥ 65 years).
No dose adjustment is needed based on age.
Gender and body weight.
No dose adjustment is needed based on gender or body weight.
Race and ethnicity.
No dose adjustment is needed based on race and ethnicity.
Renal impairment.
No dose adjustment is needed in patients with renal impairment (including end-stage renal disease). Experience with the use of tirzepatide in patients with severe renal impairment and ESRD is limited. Caution should be exercised when treating these patients with tirzepatide.
Hepatic impairment.
No dose adjustment is needed in patients with hepatic impairment. Experience with the use of tirzepatide in patients with severe hepatic impairment is limited. Caution should be exercised when treating these patients with tirzepatide.
Paediatric population.
The safety and efficacy of tirzepatide in children aged less than 18 years have not yet been established. No data are available.
Method of administration.
Mounjaro can be injected at any time of the day, with or without meals.
Inject tirzepatide subcutaneously in the abdomen or thigh.
It is recommended to rotate injection sites with each dose.
Single-dose vial and pre-filled pen.
Preservative-free, for single use in one patient only.
Discard any residue.
Multiple-dose pre-filled pen.
For single-patient use only.4.3 Contraindications
Mounjaro is contraindicated in patients with known hypersensitivity to tirzepatide or any of the excipients listed in Section 6.1 List of Excipients.
4.4 Special Warnings and Precautions for Use
Mounjaro should not be used in patients with Type 1 diabetes mellitus or for the treatment of diabetic ketoacidosis.
Acute pancreatitis.
Tirzepatide has not been studied in patients with a history of pancreatitis and should be used in caution with these patients.
Acute pancreatitis has been reported in patients treated with tirzepatide.
Patients should be informed of the symptoms of acute pancreatitis. If pancreatitis is suspected, tirzepatide should be discontinued. If the diagnosis of pancreatitis is confirmed, tirzepatide should not be restarted. In the absence of other signs and symptoms of pancreatitis, elevations in pancreatic enzymes alone are not predictive of acute pancreatitis.
Hypoglycaemia in patients with type 2 diabetes mellitus.
Patients receiving tirzepatide in combination with an insulin secretagogue (for example, a sulfonylurea) or insulin may have an increased risk of hypoglycaemia. The risk of hypoglycaemia may be lowered by a reduction in the dose of the insulin secretagogue or insulin (see Section 4.2 Dose and Method of Administration; Section 4.8 Adverse Effects (Undesirable Effects)).
Gastrointestinal effects.
Tirzepatide has been associated with gastrointestinal adverse reactions, which include nausea, vomiting, and diarrhoea (see Section 4.8 Adverse Effects (Undesirable Effects)). These events may lead to dehydration, which could cause a deterioration in renal function, including acute renal failure.
Patients treated with tirzepatide should be advised of the potential risk of dehydration, particularly in relation to gastrointestinal adverse reactions and take precautions to avoid fluid depletion. Monitor renal function when initiating or escalating doses of Mounjaro in patients with renal impairment reporting severe gastrointestinal adverse reactions.
Severe gastrointestinal disease.
Tirzepatide has not been studied in patients with severe gastrointestinal disease, including severe gastroparesis, and should be used with caution in these patients. Events related to impaired gastric emptying, including severe gastroparesis, have been reported. Monitor and consider dose modification or discontinuation in patients who develop severe gastrointestinal symptoms while on treatment.
Malnutrition.
Events related to malnutrition have been reported, including severe, in patients receiving tirzepatide. Risks associated with malnutrition include, but are not limited to, vitamin and mineral deficiency, protein deficiency, and low body weight. Balanced nutritional support should be considered. Discontinuation should be considered for severe or persistent cases.
Diabetic retinopathy.
Rapid improvement in glucose control has been associated with a temporary worsening of diabetic retinopathy. Tirzepatide has not been studied in patients with non-proliferative diabetic retinopathy requiring acute therapy, proliferative diabetic retinopathy or diabetic macular oedema, and should be used with caution in these patients with appropriate monitoring.
Pulmonary aspiration.
Tirzepatide delays gastric emptying. Pulmonary aspiration has been reported in patients receiving long acting GLP-1 receptor agonists undergoing general anaesthesia or deep sedation. This should be considered prior to such procedures.
Psychiatric disorders.
Suicidal behaviour and ideation have been reported with GLP-1 receptor agonists. Monitor patients for the emergence or worsening of depression, suicidal thoughts or behaviours, and/or any unusual changes in mood or behaviour. Consider the benefits and risks for individual patients prior to initiating or continuing therapy in patients with suicidal thoughts or behaviours or have a history of suicidal attempts.
Congestive heart failure.
There is limited therapeutic experience in patients with congestive heart failure.
Benzyl alcohol.
Mounjaro KwikPen contains 5.4 mg benzyl alcohol in each 0.6 mL dose. Benzyl alcohol may cause allergic reactions.
Patients with hepatic or renal impairment should be informed of the potential risk of metabolic acidosis due to accumulation of benzyl alcohol over time.
Use in hepatic impairment.
No dose adjustment is needed in patients with hepatic impairment (see Section 5.2 Pharmacokinetic Properties). Experience with the use of tirzepatide in patients with severe hepatic impairment is limited. Caution should be exercised when treating these patients with tirzepatide.
Use in renal impairment.
No dose adjustment is needed in patients with renal impairment (including end-stage renal disease) (see Section 5.2 Pharmacokinetic Properties). Experience with the use of tirzepatide in patients with severe renal impairment and ESRD is limited. Caution should be exercised when treating these patients with tirzepatide.
Use in the elderly.
No dose adjustment is required based on age. Only very limited data are available from patients aged ≥ 85 years.
Paediatric use.
The safety and efficacy of tirzepatide in children aged less than 18 years have not yet been established. No data are available.
Effects on laboratory tests.
No information on the effect of tirzepatide on laboratory tests is available.4.5 Interactions with Other Medicines and Other Forms of Interactions
Tirzepatide delays gastric emptying and has the potential to affect the rate of absorption of concomitantly administered oral medications. This effect, resulting in decreased Cmax and a delayed tmax, is most pronounced at the time of tirzepatide treatment initiation.
Based on the results from a study with paracetamol, which was used as a model medicinal product to evaluate the effect of tirzepatide on gastric emptying, it is not anticipated that tirzepatide treatment will result in a clinically meaningful impact on orally administered drugs that do not have a narrow therapeutic index. However, it is recommended to monitor patients on oral medicinal products with a narrow therapeutic index (e.g. warfarin, digoxin), especially during the early phase of treatment with tirzepatide and following any dose increase. The risk of delayed effect should also be considered for any oral medicinal product for which a rapid onset of effect is important.
Oral contraceptives.
Administration of a combination oral contraceptive (0.035 mg ethinylestradiol plus 0.25 mg norgestimate) in the presence of a single dose of tirzepatide (5 mg) resulted in a reduction of oral contraceptive Cmax by 55 to 66%, with a 16 to 23% reduction in area under the curve (AUC) and a delay in tmax of 2.5 to 4.5 hours. This reduction in exposure after a single 5 mg dose of tirzepatide is not considered clinically relevant. Doses other than a single 5 mg dose of tirzepatide were not investigated in this interaction study.
The reduction in exposure described above may be significant in a setting with concomitant administration of medicines also affecting those exposures. Appropriate contraception methods (including non-oral contraceptives) should be discussed with the patient based on the patient's individual circumstances prior to commencing tirzepatide. Reduced efficacy of oral contraceptives cannot be excluded, it is therefore advised that patients using oral hormonal contraceptives switch to a non-oral contraceptive method or add a barrier method of contraception for 4 weeks after initiation and for 4 weeks after each dose escalation with Mounjaro.4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
The effect of tirzepatide on fertility in humans is unknown.
Tirzepatide did not affect fertility in male rats at doses up to 3 mg/kg/day, resulting in exposures 2 times the clinical AUC at the maximum recommended human dose (MRHD). In female rats, prolonged oestrus cycling and decreases in the mean numbers of corpora lutea, implantation sites, and viable embryos per litter was observed at subclinical exposures based on AUC at the MRHD.
(Category D)
There are no adequate and well-controlled studies of tirzepatide in pregnant women. Tirzepatide should not be used during pregnancy. Women of childbearing potential are advised to use contraception during treatment with tirzepatide (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). If a patient wishes to become pregnant or becomes pregnant, treatment with tirzepatide should be discontinued.
Studies in animals have shown reproductive toxicity when tirzepatide was administered during organogenesis. In pregnant rats, embryofetal toxicity (increased post-implantation loss, impaired growth and an increased incidence of fetal abnormalities) was observed at subclinical plasma exposures. All developmental effects occurred at maternally toxic doses. Exposures at the No Observed Adverse Effects Level (NOAEL) were subclinical and a direct effect of tirzepatide on the fetus cannot be excluded.
Following a single 5 mg dose, the concentration of tirzepatide in breastmilk was found to be undetectable to very low compared to plasma concentrations. As tirzepatide is an amino acid sequence, any low amount present in breastmilk is expected to be degraded and not orally absorbed as intact drug by the breastfed infant. Administer tirzepatide to nursing women only if the potential benefit to the mother justifies the potential risk to the infant. A risk to the newborns/ infants cannot be excluded.4.7 Effects on Ability to Drive and Use Machines
No studies on the effects on the ability to drive and use machines have been performed. When tirzepatide is used in combination with a sulfonylurea or insulin, patients should be advised to take precautions to avoid hypoglycaemia while driving and using machines (see Section 4.4 Special Warnings and Precautions for Use).
4.8 Adverse Effects (Undesirable Effects)
Summary of safety profile.
Type 2 diabetes mellitus.
In 7 completed phase 3 studies, 5,119 patients were exposed to tirzepatide alone or in combination with other glucose lowering medicinal products. The most frequently reported adverse reactions in clinical studies were gastrointestinal disorders, including nausea (very common), diarrhoea (very common), constipation (common) and vomiting (common), see Table 2. In general, these reactions were mostly mild or moderate in severity and occurred more often during dose escalation and decreased over time. (See Section 4.2 Dose and Method of Administration; Section 4.4 Special Warnings and Precautions for Use.)
Chronic weight management.
In 2 completed phase 3 studies, 2519 patients were exposed to tirzepatide. The most frequently reported adverse reactions were gastrointestinal disorders, including nausea (very common), diarrhoea (very common), constipation (very common), and vomiting (very common), see Table 3. In general, these reactions were mostly mild or moderate in severity and occurred more often during dose escalation and decreased over time (see Section 4.2 Dose and Method of Administration; Section 4.4 Special Warnings and Precautions for Use). Adverse drug reactions in the chronic weight management clinical trials were similar to those in the type 2 diabetes mellitus trials with the exception of the frequencies of abdominal pain (very common), constipation (very common) and vomiting (very common).
Obstructive sleep apnoea.
In 2 completed phase 3 studies, 233 patients were exposed to tirzepatide. The adverse reactions observed with Mounjaro maximum tolerated dose (10 mg or 15 mg) were consistent with those reported in the two pooled placebo controlled clinical trials for chronic weight management.
Tabulated list of adverse reactions.
The following related adverse reactions have been identified and are listed (see Table 1), as MedDRA preferred term by system organ class and in order of decreasing incidence (very common: ≥ 1/10; common: ≥ 1/100 to < 1/10; uncommon: ≥ 1/1,000 to < 1/100; rare: ≥ 1/10,000 to < 1/1,000; very rare: < 1/10,000) and not known (cannot be estimated from the available data). Within each incidence grouping, adverse reactions are presented in order of decreasing frequency. See Tables 2, 3 and 4.




Description of selected adverse reactions.
Gastrointestinal adverse reactions. In the placebo-controlled phase 3 studies, gastrointestinal disorders were dose-dependently increased for tirzepatide 5 mg (37.1%), 10 mg (39.6%) and 15 mg (43.6%) compared with placebo (20.4%). Nausea occurred in 12.2%, 15.4% and 18.3% versus 4.3% and diarrhoea in 11.8%, 13.3% and 16.2% versus 8.9% for tirzepatide 5 mg, 10 mg and 15 mg versus placebo. Gastrointestinal adverse reactions were mostly mild (74%) or moderate (23.3%) in severity. The incidence of nausea, vomiting, and diarrhoea was higher during the dose escalation period and decreased over time.
More subjects in the tirzepatide 5 mg (3.0%), 10 mg (5.4%) and 15 mg (6.6%) groups compared to the placebo group (0.4%) discontinued permanently due to the gastrointestinal event.
Hypoglycaemia. The risk of severe hypoglycaemia with tirzepatide is low. In clinical studies, 10 (0.20%) patients reported 12 episodes of severe hypoglycaemia. Of these 10 patients, 5 (0.10%) were on a background of insulin glargine or sulfonylurea who reported 1 episode each.
Clinically significant hypoglycaemia occurred in 10 to 14% (0.14 to 0.16 events/patient year) of patients when tirzepatide was added to sulfonylurea and in 14 to 19% (0.43 to 0.64 events/patient year) of patients when tirzepatide was added to basal insulin.
The rate of clinically significant hypoglycaemia when tirzepatide was used as monotherapy or when added to other oral antidiabetic medication was up to 0.03 events/patient year (see Table 1; see Section 4.2 Dose and Method of Administration; Section 4.4 Special Warnings and Precautions for Use; Section 5.1 Pharmacodynamic Properties).
Hypersensitivity reactions. Hypersensitivity reactions have been reported with tirzepatide in the pool of placebo-controlled trials, sometimes severe (e.g. urticaria and eczema); hypersensitivity reactions were reported in 3.2% of tirzepatide-treated patients compared to 1.7% of placebo-treated patients.
Immunogenicity. There was no evidence that the pharmacokinetic profile and efficacy were impacted by the development of anti-drug antibodies (ADA). More tirzepatide-treated patients who developed anti-tirzepatide antibodies experienced hypersensitivity reactions or injection site reactions than those who did not develop these antibodies.
Consistent with the potentially immunogenic properties of protein and peptide medicinal products, patients may develop antibodies following treatment with tirzepatide.
In Phase 3 clinical studies, approximately 51 - 65% of tirzepatide-treated patients developed ADA.
Of the overall tirzepatide-treated patients, up to 2.8% and up to 2.7% had neutralising antibodies against tirzepatide activity on the glucose-dependent insulinotropic polypeptide (GIP) and glucagon-like peptide-1 (GLP-1) receptors, respectively.
Up to 0.9% and 0.4% had neutralising antibodies against native GIP and GLP-1, respectively.
Heart rate. Type 2 diabetes mellitus.
In the placebo-controlled phase 3 studies, treatment with tirzepatide resulted in a maximum mean increase in heart rate of 3 to 5 beats per minute. The maximum mean increase in heart rate in placebo-treated patients was 1 beat per minute.
The incidence of patients who had a change of baseline heart rate of > 20 bpm for 2 or more consecutive visits was 2.1%, 3.8% and 2.9%, for tirzepatide 5 mg, 10 mg and 15 mg, respectively, compared with 2.1% for placebo.
Small mean increases in PR interval were observed with tirzepatide when compared to placebo (mean increase of 1.4 to 3.2 msec and mean decrease of 1.4 msec respectively). No difference in arrhythmia and cardiac conduction disorder treatment emergent events were observed between tirzepatide 5 mg, 10 mg, 15 mg and placebo (3.8%, 2.1%, 3.7% and 3% respectively).
Chronic weight management and obstructive sleep apnoea.
Treatment with tirzepatide resulted in a mean increase in heart rate of 3 beats per minute. There was a mean increase in heart rate of 0.1 beats per minute in placebo-treated patients.
Injection site reactions. In the placebo-controlled phase 3 studies, injection site reactions were increased for tirzepatide (3.2%) compared with placebo (0.4%).
Overall, in the phase 3 studies, the most common signs and symptoms of injection site reactions were erythema and pruritus. The maximum severity of injection site reactions for patients was mild (90%) or moderate (10%). No injection site reactions were serious.
Pancreatic enzymes. Type 2 diabetes mellitus.
In the placebo-controlled phase 3 studies, treatment with tirzepatide resulted in mean increases from baseline in pancreatic amylase of 33% to 38% and lipase of 31% to 42%. Placebo treated patients had an increase from baseline in amylase of 4% and no changes were observed in lipase.
Chronic weight management and obstructive sleep apnoea.
In the placebo-controlled phase 3 studies, treatment with tirzepatide resulted in mean increases from baseline in pancreatic amylase of 23% and lipase of 34%.
Postmarketing data.
The following adverse drug reactions are based on post marketing reports of tirzepatide:
Gastrointestinal disorders.
Intestinal obstruction including ileus.
Hepatobiliary disorders.
Acute gallbladder disease including cholelithiasis, cholecystitis, biliary colic and cholecystectomy: uncommon.
Immune system disorders.
Anaphylactic reaction and angioedema.
Nervous system disorders.
Dysaesthesia: uncommon (≥ 0.1% - < 1%).
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at http://www.tga.gov.au/reporting-problems.4.9 Overdose
In the event of overdose, appropriate supportive treatments should be initiated according to the patient's clinical signs and symptoms. A period of observation and treatment of these symptoms may be necessary, taking into account the half-life of tirzepatide (approximately 5 days).
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Pharmacotherapeutic group: drugs used in diabetes, blood glucose lowering drugs, excl. insulins.
ATC code: A10BX16.
Mechanism of action.
Tirzepatide is a long-acting GIP and GLP-1 receptor agonist. It is an amino acid sequence with a C20 fatty diacid moiety that enables albumin binding and prolongs half-life. Both receptors are present on the pancreatic α and β endocrine cells, brain, heart, vasculature, immune cells (leukocytes), gut and kidney. GIP receptors are also present on adipocytes.
Tirzepatide is selective to human GIP and GLP-1 receptors. Tirzepatide has high affinity to both the GIP and GLP-1 receptors. The activity of tirzepatide on the GIP receptor is similar to native GIP hormone. The activity of tirzepatide on the GLP-1 receptor is lower compared to native GLP-1 hormone. Tirzepatide is a biased agonist at the GLP-1 receptor with preferential signaling towards the activation of adenylyl cyclase as opposed to the recruitment of β-arrestin.
Pharmacodynamic effects.
Glycaemic control.
Tirzepatide improves glycaemic control by lowering fasting and postprandial glucose concentrations in patients with type 2 diabetes through several mechanisms.
Insulin secretion.
Tirzepatide increases β-cell glucose sensitivity. In a hyperglycaemic clamp study in patients with type 2 diabetes, tirzepatide was compared to placebo and the selective GLP-1 receptor agonist semaglutide 1 mg for insulin secretion. Tirzepatide 15 mg enhanced the first- and second-phase insulin secretion rate by 466% and 302% from baseline, respectively, in a glucose dependent manner. There was no change in first- and second-phase insulin secretion rate for placebo and the rates increased for semaglutide 1 mg by 298% and 223%, respectively.
Insulin sensitivity.
Tirzepatide 15 mg improved whole body insulin sensitivity by 63%, as measured by M-value, a measure of glucose tissue uptake using hyperinsulinemic euglycaemic clamp. The M-value was unchanged for placebo and increased in semaglutide 1 mg by 35%.
Tirzepatide lowers body weight in patients with type 2 diabetes, which may contribute to improvement in insulin sensitivity. Reduced food intake with tirzepatide contributes to body weight loss. Body weight reduction is mostly due to reduced fat mass.
Glucagon concentration.
Tirzepatide reduced the fasting and postprandial glucagon concentrations. Tirzepatide 15 mg reduced fasting glucagon concentration by 28% and glucagon AUC after a mixed meal by 43%, compared with no change for placebo, and decreases for semaglutide 1 mg in fasting glucagon by 22% and in glucagon AUC by 29%.
Gastric emptying.
Tirzepatide delays gastric emptying, with largest delay after the first dose and this effect diminishes over time. Slowing post-meal glucose absorption and can lead to a beneficial effect on postprandial glycaemia.
Energy intake.
In patients with type 2 diabetes, tirzepatide reduced food intake contributing to body weight loss. In pre-clinical rodent studies tirzepatide induced a preference to lower fat food.
Appetite regulation.
Tirzepatide regulates appetite and decreases food intake. Both the GIP and GLP-1 receptors are found in areas of the brain that are important for appetite regulation.
Animal studies show that tirzepatide distributes to and activates neurons in brain regions involved in regulation of appetite and food intake.
Body weight.
Tirzepatide reduces and controls body weight. GIP receptors are present on adipocytes. Studies in diet-induced obese mice show that tirzepatide modulates fat utilisation through the GIP receptor.
Clinical trials - clinical efficacy and safety.
Type 2 diabetes mellitus.
Glycaemic control and body weight.
The safety and efficacy of tirzepatide were evaluated in five (5) global randomised, controlled, phase 3 studies (SURPASS 1 to 5) assessing glycaemic efficacy as the primary objective involving 6,263 treated patients with type 2 diabetes (4,199 treated with tirzepatide). The secondary objectives included body weight, fasting serum glucose (FSG) and proportion of patients reaching target HbA1c. All five phase 3 studies assessed tirzepatide 5 mg, 10 mg and 15 mg. All patients treated with tirzepatide started with 2.5 mg for 4 weeks. Then the dose of tirzepatide was increased by 2.5 mg every 4 weeks until they reached their assigned dose.
Across all studies, treatment with tirzepatide demonstrated sustained, statistically significant and clinically meaningful reductions from baseline in HbA1c and body weight compared to either placebo or active control treatment (semaglutide, insulin degludec and insulin glargine) for up to 1 year. In 1 study these effects were sustained for up to 2 years. Results from the phase 3 studies are presented below based on the modified intent-to-treat (mITT) population consisting of all randomly assigned patients who were exposed to at least 1 dose of study treatment, excluding patients discontinuing study treatment due to inadvertent enrolment. The analysis aligned to the efficacy estimand for a longitudinal continuous variable employed a mixed model for repeated measurements.
SURPASS 1 - monotherapy. In a 40-week double blind placebo-controlled study (GPGK), 478 patients with inadequate glycaemic control with diet and exercise, were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or placebo. Patients had a mean age of 54 years and 52% were men. At baseline the patients had a mean duration of diabetes of 5 years and the mean BMI was 32 kg/m2. See Table 5 and Figure 1.

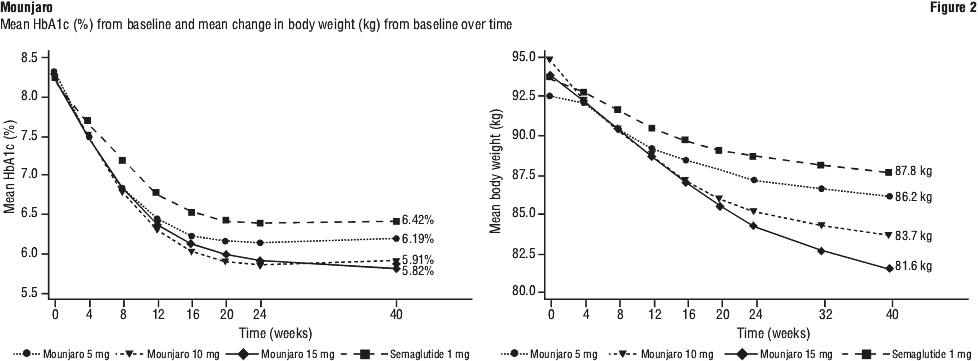
 SURPASS 2 - combination therapy with metformin. In a 40-week (GPGL) active-controlled open-label study, (double-blind with respect to tirzepatide dose assignment) 1,879 patients were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or semaglutide 1 mg once weekly, all in combination with metformin. Patients had a mean age of 57 years and 47% were men. At baseline the patients had a mean duration of diabetes of 9 years and the mean BMI was 34 kg/m2. See Table 6 and Figure 2.
SURPASS 2 - combination therapy with metformin. In a 40-week (GPGL) active-controlled open-label study, (double-blind with respect to tirzepatide dose assignment) 1,879 patients were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or semaglutide 1 mg once weekly, all in combination with metformin. Patients had a mean age of 57 years and 47% were men. At baseline the patients had a mean duration of diabetes of 9 years and the mean BMI was 34 kg/m2. See Table 6 and Figure 2.

 SURPASS 3 - combination therapy with metformin, with or without SGLT2i. In a 52-week active-controlled open-label study (GPGH), 1,444 patients were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or insulin degludec, all in combination with metformin and with or without a sodium-glucose co-transporter 2 inhibitor (SGLT2i). 32% of patients were using SGLT2i at baseline. At baseline the patients had a mean duration of diabetes of 8 years, a mean BMI of 34 kg/m2, a mean age of 57 years and 56% were men.
SURPASS 3 - combination therapy with metformin, with or without SGLT2i. In a 52-week active-controlled open-label study (GPGH), 1,444 patients were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or insulin degludec, all in combination with metformin and with or without a sodium-glucose co-transporter 2 inhibitor (SGLT2i). 32% of patients were using SGLT2i at baseline. At baseline the patients had a mean duration of diabetes of 8 years, a mean BMI of 34 kg/m2, a mean age of 57 years and 56% were men.
Patients treated with insulin degludec started at a dose of 10 U/day which was adjusted using an algorithm for a target fasting blood glucose of < 5 mmol/L. The mean dose of insulin degludec at week 52 was 49 units/day. See Table 7 and Figure 3.


Continuous glucose monitoring (CGM).
A subset of patients (N = 243) participated in an evaluation of the 24-hour glucose profiles captured with blinded CGM. At 52-weeks, patients treated with tirzepatide (10 mg and 15 mg pooled) spent significantly more time with glucose values in the euglycaemic range defined as 3.9 to 7.8 mmol/L compared to patients treated with insulin degludec, with 73% and 48% of the 24-hour period in range, respectively.
At 52-weeks patients in all 3 tirzepatide dose groups spent a greater proportion of the 24 hour period with blood glucose in the range of 3.9 to 10.0 mmol/L than patients treated with insulin degludec: tirzepatide (range), 84.9% to 91.2%; insulin degludec, 75.0%.
Liver fat content (LFC) and adipose tissue.
A subset of patients (N = 296) participated in an evaluation of LFC, visceral adipose tissue (VAT) and abdominal subcutaneous adipose tissue (ASAT) assessed through magnetic resonance imaging. At 52-weeks, patients treated with tirzepatide (10 mg and 15 mg pooled) demonstrated statistically significantly greater mean reductions in LFC compared to insulin degludec, -8.09% versus -3.38% respectively, from baselines of 15.67% and 16.58%. Patients treated with tirzepatide 5 mg, 10 mg and 15 mg had significantly greater reductions in volume of VAT (-1.10, -1.53 and -1.65 L respectively) and ASAT (-1.40, -2.25 and -2.05 L respectively) from overall baselines of 6.6 L and 10.4 L respectively at 52 weeks compared with an increase in the insulin degludec group (0.38 and 0.63 L).
SURPASS 4 - combination therapy with 1-3 oral antidiabetic medicinal products: metformin, sulfonylureas or SGLT2i. In an active-controlled open-label study of up to 104 weeks (primary endpoint at 52 weeks) (GPGM), 2,002 patients with type 2 diabetes and increased cardiovascular risk were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or insulin glargine once daily on a background of metformin (95%) and/or sulfonylureas (54%) and/or SGLT‑2i (25%). At baseline the patients had a mean duration of diabetes of 12 years, a mean BMI of 33 kg/m2, a mean age of 64 years and 63% were men. Patients treated with insulin glargine started at a dose of 10 U/day which was adjusted using an algorithm with a fasting blood glucose target of < 5.6 mmol/L. The mean dose of insulin glargine at week 52 was 44 units/day. See Table 8 and Figure 4.

 SURPASS 5 - combination therapy with titrated basal insulin, with or without metformin. In a 40-week double-blind placebo-controlled study (GPGI), 475 patients with inadequate glycaemic control using insulin glargine with or without metformin were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or placebo. Insulin glargine doses were adjusted utilising an algorithm with a fasting blood glucose target of < 5.6 mmol/L. At baseline the patients had a mean duration of diabetes of 13 years, a mean BMI of 33 kg/m2, a mean age of 61 years and 56% were men. The overall estimated median dose of insulin glargine at baseline was 34 units/day. The median dose of insulin glargine at week 40 was 38, 36, 29 and 59 units/day for tirzepatide 5 mg, 10 mg, 15 mg and placebo respectively. See Table 9 and Figure 5.
SURPASS 5 - combination therapy with titrated basal insulin, with or without metformin. In a 40-week double-blind placebo-controlled study (GPGI), 475 patients with inadequate glycaemic control using insulin glargine with or without metformin were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or placebo. Insulin glargine doses were adjusted utilising an algorithm with a fasting blood glucose target of < 5.6 mmol/L. At baseline the patients had a mean duration of diabetes of 13 years, a mean BMI of 33 kg/m2, a mean age of 61 years and 56% were men. The overall estimated median dose of insulin glargine at baseline was 34 units/day. The median dose of insulin glargine at week 40 was 38, 36, 29 and 59 units/day for tirzepatide 5 mg, 10 mg, 15 mg and placebo respectively. See Table 9 and Figure 5.


Cardiovascular evaluation.
Cardiovascular (CV) risk was assessed via a meta-analysis of patients with at least one adjudication confirmed major adverse cardiac event (MACE). The composite endpoint of MACE-4 included CV death, nonfatal myocardial infarction, non-fatal stroke, or hospitalisation for unstable angina.
In a primary meta-analysis of phase 2 and 3 registration studies, a total of 116 patients (tirzepatide: 60 [n = 4410]; all comparators: 56 [n = 2169]) experienced at least one adjudication confirmed MACE-4: The results showed that tirzepatide was not associated with excess risk for CV events compared with pooled comparators (HR: 0.81; CI: 0.52 to 1.26).
An additional analysis was conducted specifically for the SURPASS-4 study that enrolled patients with established CV disease. A total of 109 patients (tirzepatide: 47 [n=995]; insulin glargine: 62 [n=1000]) experienced at least one adjudication confirmed MACE-4: The results showed that tirzepatide was not associated with excess risk for CV events compared with insulin glargine (HR: 0.74; CI:0.51 to 1.08).
Blood pressure.
Treatment with tirzepatide resulted in a mean decrease in systolic and diastolic blood pressure of 6 to 9 mmHg and 3 to 4 mmHg, respectively. There was a mean decrease in systolic and diastolic blood pressure of 2 mmHg each in placebo-treated patients.
Other information.
Fasting serum glucose.
Treatment with tirzepatide resulted in significant reductions from baseline in FSG (changes from baseline to primary end point were -2.4 mmol/L to -3.8 mmol/L). Significant reductions from baseline in FSG could be observed as early as 2 weeks. The improvement in FSG was sustained through the longest study duration of 104 weeks.
Postprandial glucose.
Treatment with tirzepatide resulted in significant reductions in mean 2-hour post prandial glucose (mean of 3 main meals of the day) from baseline (changes from baseline to primary end point were -3.35 mmol/L to -4.85 mmol/L).
Pancreatic enzymes.
Treatment with tirzepatide resulted in an increase from baseline in pancreatic amylase of 33% to 38% and lipase of 31% to 42%. Placebo-treated patients had an increase from baseline in amylase of 4% and no changes were observed in lipase. In the absence of other signs and symptoms of acute pancreatitis, elevations in pancreatic enzymes alone are not predictive of acute pancreatitis.
Triglycerides.
Across SURPASS 1-5 trials, tirzepatide 5 mg, 10 mg and 15 mg resulted in reduction in serum triglyceride of 15 - 19%, 18 - 27% and 21 - 25% respectively.
In the 40-week trial versus semaglutide 1 mg, tirzepatide 5 mg, 10 mg and 15 mg resulted in 19%, 24% and 25% reduction in serum triglycerides levels respectively compared to 12% reduction with semaglutide 1 mg.
Proportion of patients reaching HbA1c < 5.7% without clinically significant hypoglycaemia.
In the 4 studies where tirzepatide was not combined with basal insulin, 93.6% to 100% of patients who achieved a normal glycaemia of HbA1c < 5.7%, at the primary endpoint visit with tirzepatide treatment did so without clinically significant hypoglycaemia. In Study SURPASS-5, 85.9% patients treated with tirzepatide who reached HbA1c < 5.7% did so without clinically significant hypoglycaemia.
Chronic weight management.
The safety and efficacy of tirzepatide for chronic weight management (weight reduction and maintenance) in combination with a reduced calorie intake and increased physical activity were evaluated in three randomised double-blinded, placebo-controlled phase 3 studies in patients with prediabetes or normoglycaemia, but without diabetes mellitus (SURMOUNT-1, SURMOUNT-3 and SURMOUNT-4) and in patients with diabetes mellitus (SURMOUNT2). SURMOUNT-1 included a total of 2539 patients (1896 randomised to treatment with tirzepatide), while a total of 938 patients (623 randomised to treatment with tirzepatide) were included in SURMOUNT-2. SURMOUNT-3 included a total of 806 participants (579 randomised to treatment), while a total of 783 participants were enrolled in the open-label tirzepatide lead-in period with 670 participants randomised to treatment in the double-blind period in SURMOUNT-4.
All patients treated with tirzepatide started with 2.5 mg for 4 weeks. Then the dose of tirzepatide was increased by 2.5 mg every 4 weeks until they reached their assigned dose.
In SURMOUNT-1, the dose of tirzepatide or matching placebo was escalated to 5 mg, 10 mg, or 15 mg subcutaneously once weekly during a 20-week period followed by the maintenance period.
In SURMOUNT-2, the dose of tirzepatide or matching placebo was escalated to 10 mg or 15 mg subcutaneously once weekly during a 20-week period followed by the maintenance period.
SURMOUNT-1. In a 72-week double blind placebo-controlled study, 2539 adult patients with obesity (BMI ≥ 30 kg/m2), or with overweight (BMI ≥ 27 kg/m2 to < 30 kg/m2) and at least one weight related comorbid condition, such as treated or untreated dyslipidaemia, hypertension, obstructive sleep apnoea, or cardiovascular disease, were randomised to tirzepatide 5 mg, 10 mg or 15 mg once weekly or placebo. Patients with type 2 diabetes mellitus were excluded. Patients had a mean age of 45 years and 67.5% were women. At baseline 40.6% of patients had prediabetes. Mean baseline body weight was 104.8 kg and mean BMI was 38 kg/m2. See Table 10.
 In SURMOUNT-1, pooled doses of tirzepatide 5 mg, 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-8.1 mmHg vs. -1.3 mmHg), diastolic blood pressure (-5.3 mmHg vs -1.0 mmHg), total cholesterol (-6.1% vs -1.2%), triglycerides (-27.6% vs. -6.3%), non-HDL (-11.4% vs. -1.8%), LDL (-6.8% vs -0.9%), HDL (7.9% vs. 0.2%), and HbA1c (-0.5% vs. -0.1% or -5.1 mmol/mol vs -0.8 mmol/mol). See Figure 6.
In SURMOUNT-1, pooled doses of tirzepatide 5 mg, 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-8.1 mmHg vs. -1.3 mmHg), diastolic blood pressure (-5.3 mmHg vs -1.0 mmHg), total cholesterol (-6.1% vs -1.2%), triglycerides (-27.6% vs. -6.3%), non-HDL (-11.4% vs. -1.8%), LDL (-6.8% vs -0.9%), HDL (7.9% vs. 0.2%), and HbA1c (-0.5% vs. -0.1% or -5.1 mmol/mol vs -0.8 mmol/mol). See Figure 6.
 Among the patients in SURMOUNT-1 with prediabetes at baseline (N = 1032), 95.3% patients treated with tirzepatide reverted to normoglycaemia at week 72, as compared with 61.9% of patients in the placebo group.
Among the patients in SURMOUNT-1 with prediabetes at baseline (N = 1032), 95.3% patients treated with tirzepatide reverted to normoglycaemia at week 72, as compared with 61.9% of patients in the placebo group.
SURMOUNT-2. In a 72-week double blind placebo-controlled study, 938 adult patients with BMI ≥ 27 kg/m2 and type 2 diabetes mellitus, were randomised to tirzepatide 10 mg or 15 mg once weekly or placebo. Patients had a mean age of 54 years and 50.7% were women. Mean baseline body weight was 100.7 kg and mean BMI was 36.1 kg/m2. See Table 11.
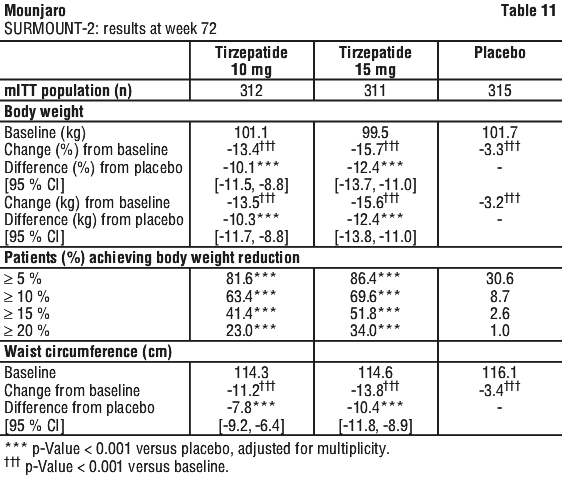 In SURMOUNT-2, pooled doses of tirzepatide 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-7.2 mmHg vs. -1.0 mmHg), diastolic blood pressure (-2.6 mmHg vs -0.2 mmHg), total cholesterol (-2.6% vs 2.1%), triglycerides (-28.7% vs. -5.8%), non-HDL (-6.7% vs. 2.3%), LDL (2.8% vs 6.3%), HDL (8.3% vs. 1.1%), and HbA1c (-2.2% vs. -0.2% or -23.9 mmol/mol vs -1.8 mmol/mol).
In SURMOUNT-2, pooled doses of tirzepatide 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-7.2 mmHg vs. -1.0 mmHg), diastolic blood pressure (-2.6 mmHg vs -0.2 mmHg), total cholesterol (-2.6% vs 2.1%), triglycerides (-28.7% vs. -5.8%), non-HDL (-6.7% vs. 2.3%), LDL (2.8% vs 6.3%), HDL (8.3% vs. 1.1%), and HbA1c (-2.2% vs. -0.2% or -23.9 mmol/mol vs -1.8 mmol/mol).
During the trial, treatment was permanently discontinued by 9.3% and 13.8% of patients randomised to tirzepatide 10 mg and 15 mg respectively compared to 14.9% randomised to placebo. See Figure 7.
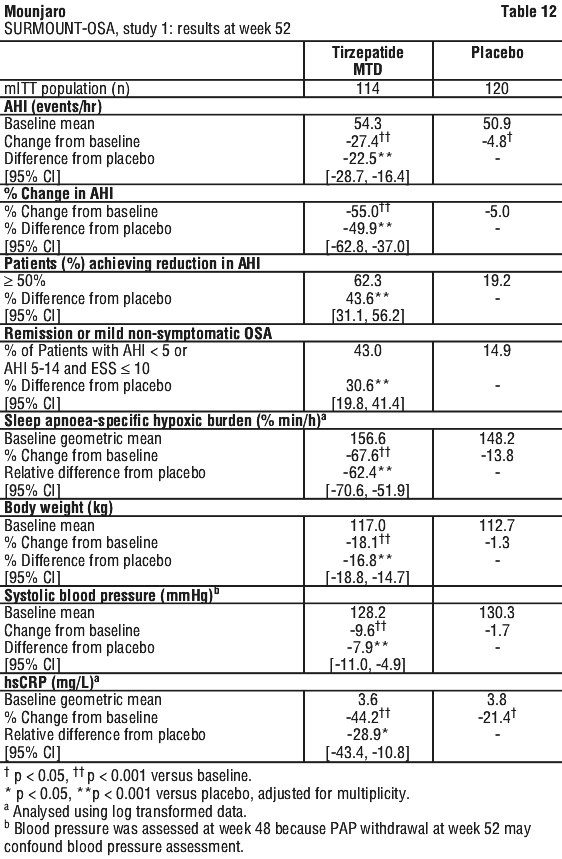
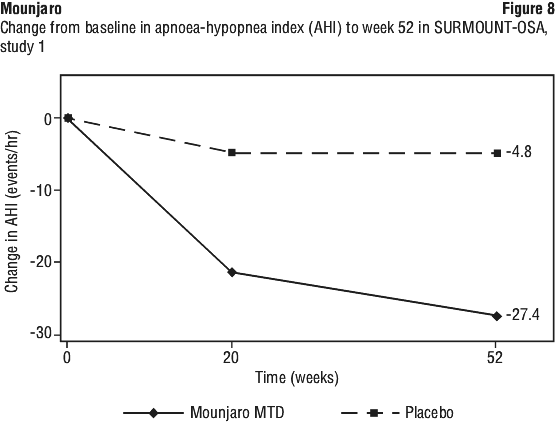
 SURMOUNT-3. In an 84-week study, 806 adult patients with obesity (BMI ≥ 30 kg/m2) or with overweight (BMI ≥ 27 kg/m2 to < 30 kg/m2) and at least one weight related comorbid condition, entered a 12-week intensive lifestyle intervention lead-in period consisting of a low-calorie diet (1200-1500 kcal/day), increased physical activity and frequent behavioural counselling. At the end of the 12-week lead-in period, 579 patients who achieved ≥ 5.0% weight reduction were randomised to tirzepatide maximum tolerated dose (MTD) of 10 mg or 15 mg once weekly or to placebo, for 72 weeks (double-blind phase). Patients were on a reduced-calorie diet and increased physical activity throughout the double-blind phase of the study. At randomisation patients had a mean age of 46 years and 63% were women. Mean BMI at randomisation was 35.9 kg/m2. See Table 12 and Figure 8.
SURMOUNT-3. In an 84-week study, 806 adult patients with obesity (BMI ≥ 30 kg/m2) or with overweight (BMI ≥ 27 kg/m2 to < 30 kg/m2) and at least one weight related comorbid condition, entered a 12-week intensive lifestyle intervention lead-in period consisting of a low-calorie diet (1200-1500 kcal/day), increased physical activity and frequent behavioural counselling. At the end of the 12-week lead-in period, 579 patients who achieved ≥ 5.0% weight reduction were randomised to tirzepatide maximum tolerated dose (MTD) of 10 mg or 15 mg once weekly or to placebo, for 72 weeks (double-blind phase). Patients were on a reduced-calorie diet and increased physical activity throughout the double-blind phase of the study. At randomisation patients had a mean age of 46 years and 63% were women. Mean BMI at randomisation was 35.9 kg/m2. See Table 12 and Figure 8.
 SURMOUNT-4. In an 88-week study, 783 adult patients with obesity (BMI ≥ 30 kg/m2) or with overweight (BMI ≥ 27 kg/m2 to < 30 kg/m2) and at least one weight related comorbid condition, were enrolled in a 36-week open label tirzepatide lead-in phase. At the start of lead-in period, the enrolled patients had a mean body weight of 107.0 kg and a mean BMI of 38.3 kg/m2. At the end of the lead-in period, 670 patients who achieved tirzepatide MTD of 10 mg or 15 mg dose were randomised to continue treatment with tirzepatide once weekly or to switch to placebo for 52 weeks (double-blind phase). Patients were counselled on a reduced calorie diet and increased physical activity throughout the trial. At randomisation (week 36), patients had a mean age of 49 years and 71% were women. Mean body weight at randomisation was 85.2 kg and mean BMI was 30.5 kg/m2.
SURMOUNT-4. In an 88-week study, 783 adult patients with obesity (BMI ≥ 30 kg/m2) or with overweight (BMI ≥ 27 kg/m2 to < 30 kg/m2) and at least one weight related comorbid condition, were enrolled in a 36-week open label tirzepatide lead-in phase. At the start of lead-in period, the enrolled patients had a mean body weight of 107.0 kg and a mean BMI of 38.3 kg/m2. At the end of the lead-in period, 670 patients who achieved tirzepatide MTD of 10 mg or 15 mg dose were randomised to continue treatment with tirzepatide once weekly or to switch to placebo for 52 weeks (double-blind phase). Patients were counselled on a reduced calorie diet and increased physical activity throughout the trial. At randomisation (week 36), patients had a mean age of 49 years and 71% were women. Mean body weight at randomisation was 85.2 kg and mean BMI was 30.5 kg/m2.
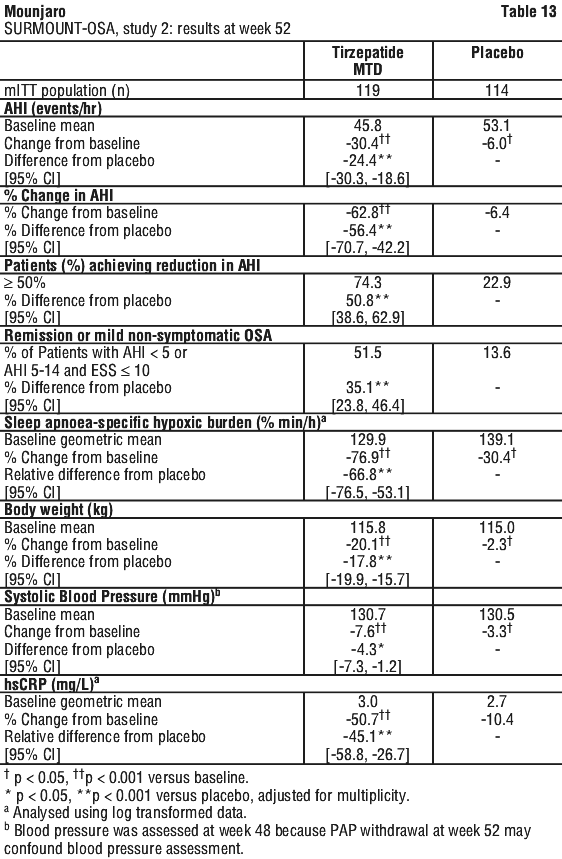
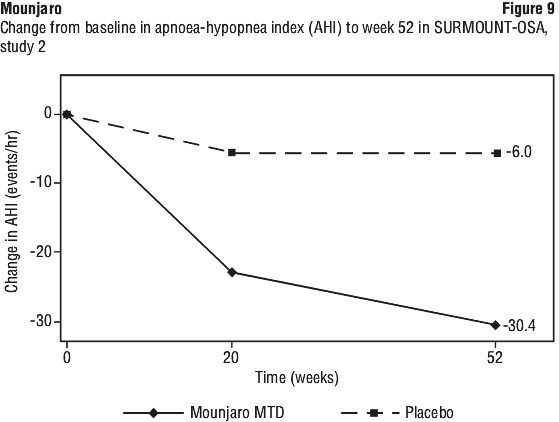
Patients who continued treatment with tirzepatide for an additional 52 weeks (up to 88 weeks in total) maintained and experienced further weigh loss after the initial weight reduction achieved during the 36-week lead-in phase. The weight reduction was superior and clinically meaningful compared to the placebo group, in which a substantial regain of body weight lost during the lead-in phase was observed (see Table 13 and Figure 9). Nevertheless, the observed mean body weight for placebo-treated patients was lower at week 88 than at the start of the lead-in phase (see Figure 9).
Risk of weight regain to > 95% of study baseline (week 0) weight at week 88.
Time to event analysis showed that continued tirzepatide treatment during the double-blind period reduced the risk of returning to greater than 95% body weight observed at week 0, for those who had already lost at least 5% since week 0 by approximately 99% compared with placebo (hazard ratio, 0.013 [95% CI, 0.004 to 0.046]; p < 0.001).
Cardiovascular evaluation.
An analysis was conducted for the SURMOUNT-1 study where a total of 14 patients (tirzepatide: 9 (0.47%) out of 1896; placebo: 5 (0.78%) out of 643) experienced at least one adjudication confirmed MACE. Percentages of patients with adjudication confirmed MACE were similar across placebo and tirzepatide groups.
Analysis was conducted for the SURMOUNT-2 study. A total of 11 patients (tirzepatide: 7 (1.12%) out of 623 placebo: 4 (1.27%) out of 315) experienced at least one adjudication confirmed MACE. Percentages of patients with adjudication confirmed MACE were similar across placebo and tirzepatide groups.
Blood pressure.
In SURMOUNT-1 treatment with tirzepatide resulted in a mean decrease in systolic and diastolic blood pressure of 8.1 mmHg and 5.3 mmHg, respectively. There was a mean decrease in systolic and diastolic blood pressure of 1.3 mmHg and 1.0 mmHg respectively in placebo treated patients.
In SURMOUNT-2 treatment with tirzepatide resulted in a mean decrease in systolic and diastolic blood pressure of 7.2 mmHg and 2.6 mmHg, respectively. There was a mean decrease in systolic and diastolic blood pressure of 1.0 mmHg and 0.2 mmHg respectively in placebo treated patients.
Other information.
Changes in body composition.
Changes in body composition were evaluated in a sub-study in SURMOUNT-1 using dual energy X-ray absorptiometry (DEXA). The results of the DEXA assessment showed that treatment with tirzepatide was accompanied by greater reduction in fat mass than in lean body mass leading to an improvement in body composition compared to placebo after 72 weeks. Furthermore, this reduction in total fat mass was accompanied by a reduction in visceral fat. These results suggest that most of the total weight loss was attributable to a reduction in fat tissue, including visceral fat.
Obstructive sleep apnoea.
The efficacy and safety of tirzepatide for the treatment of moderate to severe obstructive sleep apnoea (OSA), in combination with diet and exercise, in patients with obesity were evaluated in two randomised double-blinded, placebo-controlled phase 3 studies (SURMOUNT-OSA Study 1 and Study 2). A total of 469 adult patients with moderate to severe OSA and obesity (234 randomised to treatment with tirzepatide) were included in these studies. Patients with T2DM were excluded. Study 1 enrolled patients unable or unwilling to use Positive Airway Pressure (PAP) therapy. Study 2 enrolled patients on PAP therapy. All patients were treated with the maximum tolerated dose (MTD; 10 mg or 15 mg) of tirzepatide or placebo, once weekly for 52 weeks.
In both studies, treatment with tirzepatide demonstrated statistically significant and clinically meaningful reduction in the apnoea-hypopnoea index (AHI) compared with placebo. A reduction in AHI was observed with tirzepatide irrespective of age, sex, ethnicity, baseline BMI or baseline OSA severity. Greater proportions of patients treated with tirzepatide achieved remission or mild non-symptomatic OSA compared to placebo (see Table 14). Among tirzepatide treated patients, greater proportions of patients achieved at least 50% AHI reduction compared to placebo.
SURMOUNT-OSA, study 1. In a 52-week double-blind placebo-controlled study, 234 adult patients with moderate to severe OSA and obesity, were randomised to tirzepatide MTD of 10 mg or 15 mg once weekly, or to placebo, once weekly. Patients had a mean age of 48 years, 33% were female, 35% had moderate OSA, 63% had severe OSA, 65% had pre-diabetes, 76% had hypertension, 10% had cardiac disorders, and 81% had dyslipidemia. Patients had a mean Epworth Sleepiness Scale (ESS) of 10.6. See Table 14 and Figure 10.
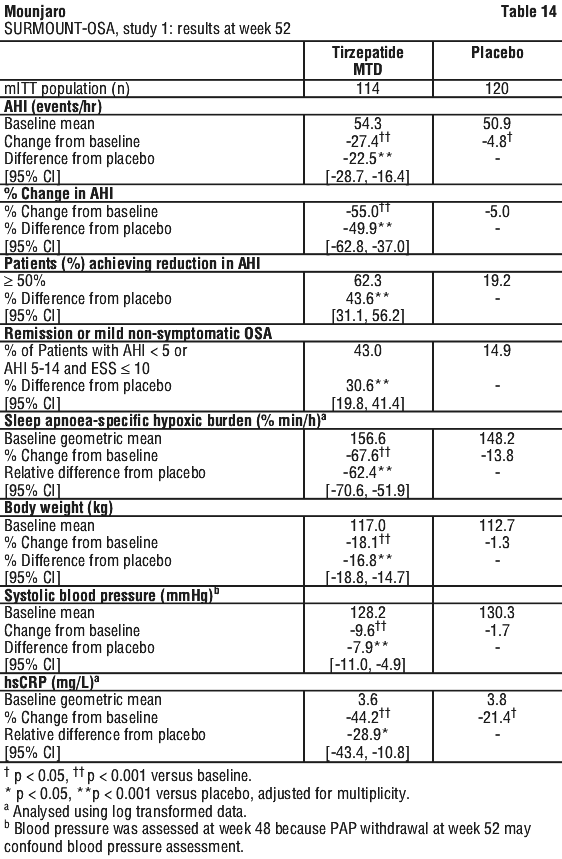
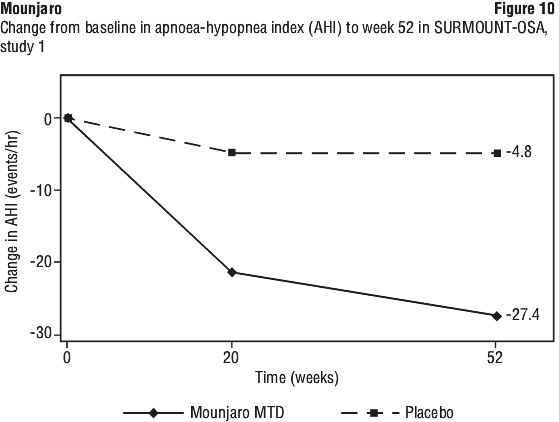 In SURMOUNT-OSA, study 1, tirzepatide MTD led to a significant improvement compared to placebo in diastolic blood pressure (-5.2 mmHg vs. -2.0 mmHg), triglycerides (-32.9% vs. -1.0%), non-HDL-C (-15.0% vs. -2.3%), HDL-C (10.6% vs. 3.1%), and fasting insulin (-44.2% vs. -4.7%).
In SURMOUNT-OSA, study 1, tirzepatide MTD led to a significant improvement compared to placebo in diastolic blood pressure (-5.2 mmHg vs. -2.0 mmHg), triglycerides (-32.9% vs. -1.0%), non-HDL-C (-15.0% vs. -2.3%), HDL-C (10.6% vs. 3.1%), and fasting insulin (-44.2% vs. -4.7%).
SURMOUNT-OSA, study 2. In a 52-week double-blind placebo-controlled study, 235 adult patients with moderate to severe OSA and obesity, were randomised to tirzepatide MTD of 10 mg or 15 mg once weekly or to placebo, once weekly. Patients had a mean age of 52 years, 28% were female, 31% had moderate OSA, 68% had severe OSA, 65% had pre-diabetes, 77% had hypertension, 11% had cardiac disorders, and 84% had dyslipidemia. Patients had a mean ESS of 10.2. See Table 15 and Figure 11.
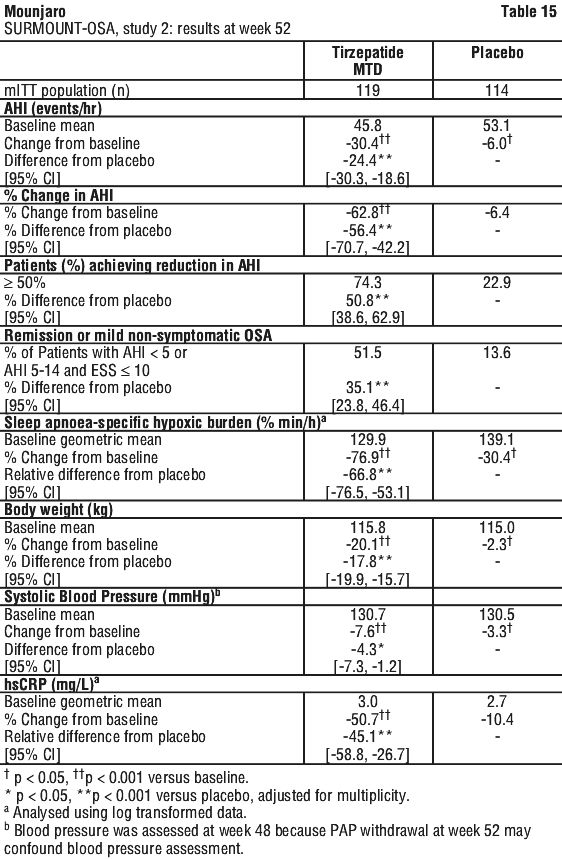
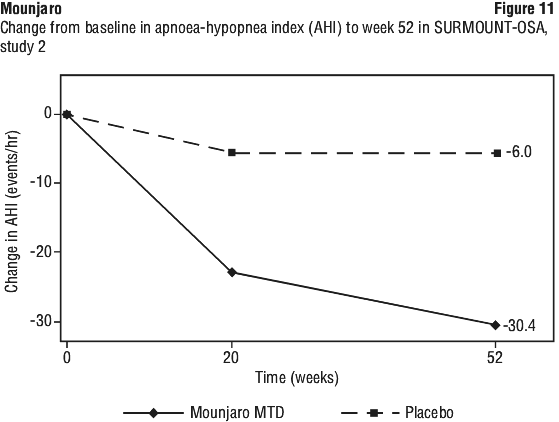 In SURMOUNT-OSA, study 2, tirzepatide MTD led to a significant improvement compared to placebo in triglycerides (-35.2% vs. -5.4%), non-HDL-C (-15.8% vs. -1.8%), HDL-C (15.0% vs. 4.5%), and fasting insulin (-48.5% vs. -5.6%).
In SURMOUNT-OSA, study 2, tirzepatide MTD led to a significant improvement compared to placebo in triglycerides (-35.2% vs. -5.4%), non-HDL-C (-15.8% vs. -1.8%), HDL-C (15.0% vs. 4.5%), and fasting insulin (-48.5% vs. -5.6%).
Improvement in sleep-related impairment and sleep disturbance.
Tirzepatide-treated patients, pooled across Studies 1 and 2, demonstrated statistically significant improvement in sleep-related impairment and sleep disturbance, as measured by the PROMIS sleep related impairment short form 8a (PROMIS SRI); t-scores (-7.3) versus placebo (-3.5) and PROMIS sleep disturbance short form 8b (PROMIS SD); t-scores (-5.8) versus placebo (-2.9), respectively. This trend was consistent in the individual studies. A significantly greater proportion of patients treated with tirzepatide reported a meaningful within-patient change compared to placebo in PROMIS SRI (Study 1: 44.4% vs 26.6%; Study 2: 39.1% v 23.1%) and PROMIS SD (Study 1: 35.8% vs 24.8%; Study 2: 46.1% vs 27.2%).
Cardiovascular evaluation.
In two placebo-controlled OSA phase 3 studies, one patient experienced at least one adjudication confirmed MACE (tirzepatide: 0 (n = 233); placebo: 1 (n = 234)).
Blood pressure.
In two placebo-controlled OSA phase 3 studies, treatment with tirzepatide resulted in a mean decrease in systolic and diastolic blood pressure of 9.0 mmHg and 3.8 mmHg, respectively. There was a mean decrease in systolic and diastolic blood pressure of 2.5 mmHg and 1.0 mmHg, respectively, in placebo treated patients.
Other information.
Triglycerides.
In two placebo-controlled OSA phase 3 studies (Study 1 and Study 2, respectively), treatment with tirzepatide MTD (10 mg or 15 mg) resulted in 32.9% and 35.2% reduction in serum triglyceride levels compared to 1.0% and 5.4% reduction with placebo.
Special populations.
In adult patients with type 2 diabetes, the efficacy of tirzepatide was not impacted by age, gender, race, ethnicity, region, or by baseline BMI, HbA1c, diabetes duration and level of renal function impairment.
In adult patients who are overweight or with obesity, treatment with tirzepatide produced a statistically significant reduction from baseline in body weight compared to placebo. A reduction in body weight was observed with tirzepatide irrespective of age, sex, race, ethnicity, baseline BMI, and glycaemic status.
The efficacy of tirzepatide for the treatment of moderate to severe OSA in patients with obesity was not impacted by age, sex, ethnicity, baseline BMI, or baseline OSA severity.
5.2 Pharmacokinetic Properties
Absorption.
Maximum concentration of tirzepatide is reached 8 to 72 hours post dose. Steady state exposure is achieved following 4 weeks of once weekly administration. Tirzepatide exposure increases in a dose proportional manner. Similar exposure was achieved with subcutaneous administration of tirzepatide in the abdomen, thigh, or upper arm. Absolute bioavailability of subcutaneous tirzepatide was 80%.
Distribution.
The mean apparent steady-state volume of distribution of tirzepatide following subcutaneous administration in patients with type 2 diabetes is approximately 10.3 L in patients with type 2 diabetes and 9.7 L in patients with obesity. Tirzepatide is highly bound to plasma albumin (99%).
Metabolism.
Tirzepatide is metabolised by proteolytic cleavage of the peptide backbone, beta-oxidation of the C20 fatty diacid moiety and amide hydrolysis.
Excretion.
The apparent population mean clearance of tirzepatide is approximately 0.06 L/h with an elimination half-life of approximately 5 days, enabling once weekly administration.
Tirzepatide is eliminated by metabolism. The primary excretion routes of tirzepatide metabolites are via urine and faeces. Intact tirzepatide is not observed in urine or faeces.
Special populations.
Age, gender, race, ethnicity, body weight.
Age, gender, race, ethnicity or body weight, do not have a clinically relevant effect on the pharmacokinetics (PK) of tirzepatide.
Renal impairment.
Renal impairment does not impact the PK of tirzepatide. The PK of tirzepatide after a single 5 mg dose was evaluated in patients with different degrees of renal impairment (mild, moderate, severe, ESRD) compared with subjects with normal renal function. This was also shown for patients with both type 2 diabetes mellitus and renal impairment based on data from clinical studies.
Hepatic impairment.
Hepatic impairment does not impact the PK of tirzepatide. The PK of tirzepatide after a single 5 mg dose was evaluated in patients with different degrees of hepatic impairment (mild, moderate, severe) compared with subjects with normal hepatic function.
Paediatric population.
Tirzepatide has not been studied in paediatric patients.
5.3 Preclinical Safety Data
Genotoxicity.
In an in vivo genotoxicity study (bone marrow micronucleus assay) there were no significant increase in micronuclei in polychromatic erythrocytes in bone marrow of male rats after single SC administration of up to 3 mg/kg tirzepatide. Based on the weight of evidence, tirzepatide is not considered genotoxic.
Carcinogenicity.
A 2-year carcinogenicity study was conducted with tirzepatide in male and female rats at doses of 0.15, 0.50, and 1.5 mg/kg (0.12, 0.36, and 1.02-fold the maximum recommended human dose (MRHD) based on area under the curve (AUC)) administered by subcutaneous injection twice weekly. Tirzepatide caused an increase in thyroid C-cell tumours (adenomas and carcinomas) at all doses compared to controls. The human relevance of these findings is currently unknown.
In a 6-month carcinogenicity study in rasH2 transgenic mice, tirzepatide at doses of 1, 3, and 10 mg/kg (up to 11-fold the MRHD based on AUC) administered by subcutaneous injection twice weekly did not produce increased incidences of thyroid C-cell hyperplasia or neoplasia at any dose.6 Pharmaceutical Particulars
6.1 List of Excipients
Single-dose vial and pre-filled pen (autoinjector).
Sodium chloride, dibasic sodium phosphate heptahydrate, hydrochloric acid, sodium hydroxide, water for injections.
Multiple-dose pre-filled pen (KwikPen).
Dibasic sodium phosphate heptahydrate, benzyl alcohol, glycerol, phenol, sodium chloride, hydrochloric acid, sodium hydroxide, water for injections.
6.2 Incompatibilities
Not applicable for subcutaneous single-dose product.
In the absence of compatibility studies this medicinal product must not be mixed with other medicinal products.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Single-dose vial and pre-filled pen (autoinjector).
Mounjaro vials and ready-to-use, single-use, pre-filled pens should be stored at 2°C to 8°C, refrigerated. Do not freeze. Do not shake. Store in original carton to protect from light.
In-use.
Mounjaro may be stored unrefrigerated for up to 21 days at temperatures not above 30°C.
Multiple-dose, pre-filled pen (KwikPen).
Mounjaro ready-to-use, multiple-dose, pre-filled pens should be stored at 2°C to 8°C, refrigerated. Do not freeze. Do not shake. Protect from light.
In-use.
Mounjaro may be stored unrefrigerated for up to 30 days at temperatures not above 30°C.
6.5 Nature and Contents of Container
Mounjaro is available in vials and as ready-to-use pre-filled pens.
Single-use vial.
The product is contained in a clear glass vial (Type I) with a bromobutyl elastomer stopper.
Trade packs of 1 vial and starter packs of 1 vial for the 2.5 mg/0.5 mL presentation.
Multiple-dose, pre-filled pen (KwikPen).
The product is contained in a clear glass cartridge (Type I) encased in a disposable multiple-dose pen.
Trade packs of 1 pre-filled pen and starter packs of 1 pre-filled pen for the 2.5 mg presentation.
No needles are included in the pack.
Single-use prefilled pen (autoinjector).
The product is contained in a glass syringe (Type I) encased in a disposable single-dose pen.
Trade packs of 2 or 4 pre-filled pens, and starter packs of 2 pre-filled pens for the 2.5 mg/0.5 mL presentation.
Not all pack sizes and presentations may be available.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure.
 Molecular weight: 4,813 daltons.
Molecular weight: 4,813 daltons.
CAS number.
2023788-19-2.7 Medicine Schedule (Poisons Standard)
S4 - Prescription Medicine.
Summary Table of Changes
















 In SURMOUNT-1, pooled doses of tirzepatide 5 mg, 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-8.1 mmHg vs. -1.3 mmHg), diastolic blood pressure (-5.3 mmHg vs -1.0 mmHg), total cholesterol (-6.1% vs -1.2%), triglycerides (-27.6% vs. -6.3%), non-HDL (-11.4% vs. -1.8%), LDL (-6.8% vs -0.9%), HDL (7.9% vs. 0.2%), and HbA1c (-0.5% vs. -0.1% or -5.1 mmol/mol vs -0.8 mmol/mol). See Figure 6.
In SURMOUNT-1, pooled doses of tirzepatide 5 mg, 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-8.1 mmHg vs. -1.3 mmHg), diastolic blood pressure (-5.3 mmHg vs -1.0 mmHg), total cholesterol (-6.1% vs -1.2%), triglycerides (-27.6% vs. -6.3%), non-HDL (-11.4% vs. -1.8%), LDL (-6.8% vs -0.9%), HDL (7.9% vs. 0.2%), and HbA1c (-0.5% vs. -0.1% or -5.1 mmol/mol vs -0.8 mmol/mol). See Figure 6. Among the patients in SURMOUNT-1 with prediabetes at baseline (N = 1032), 95.3% patients treated with tirzepatide reverted to normoglycaemia at week 72, as compared with 61.9% of patients in the placebo group.
Among the patients in SURMOUNT-1 with prediabetes at baseline (N = 1032), 95.3% patients treated with tirzepatide reverted to normoglycaemia at week 72, as compared with 61.9% of patients in the placebo group. In SURMOUNT-2, pooled doses of tirzepatide 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-7.2 mmHg vs. -1.0 mmHg), diastolic blood pressure (-2.6 mmHg vs -0.2 mmHg), total cholesterol (-2.6% vs 2.1%), triglycerides (-28.7% vs. -5.8%), non-HDL (-6.7% vs. 2.3%), LDL (2.8% vs 6.3%), HDL (8.3% vs. 1.1%), and HbA1c (-2.2% vs. -0.2% or -23.9 mmol/mol vs -1.8 mmol/mol).
In SURMOUNT-2, pooled doses of tirzepatide 10 mg and 15 mg led to a significant improvement compared to placebo in systolic blood pressure (-7.2 mmHg vs. -1.0 mmHg), diastolic blood pressure (-2.6 mmHg vs -0.2 mmHg), total cholesterol (-2.6% vs 2.1%), triglycerides (-28.7% vs. -5.8%), non-HDL (-6.7% vs. 2.3%), LDL (2.8% vs 6.3%), HDL (8.3% vs. 1.1%), and HbA1c (-2.2% vs. -0.2% or -23.9 mmol/mol vs -1.8 mmol/mol).





 In SURMOUNT-OSA, study 1, tirzepatide MTD led to a significant improvement compared to placebo in diastolic blood pressure (-5.2 mmHg vs. -2.0 mmHg), triglycerides (-32.9% vs. -1.0%), non-HDL-C (-15.0% vs. -2.3%), HDL-C (10.6% vs. 3.1%), and fasting insulin (-44.2% vs. -4.7%).
In SURMOUNT-OSA, study 1, tirzepatide MTD led to a significant improvement compared to placebo in diastolic blood pressure (-5.2 mmHg vs. -2.0 mmHg), triglycerides (-32.9% vs. -1.0%), non-HDL-C (-15.0% vs. -2.3%), HDL-C (10.6% vs. 3.1%), and fasting insulin (-44.2% vs. -4.7%).
 In SURMOUNT-OSA, study 2, tirzepatide MTD led to a significant improvement compared to placebo in triglycerides (-35.2% vs. -5.4%), non-HDL-C (-15.8% vs. -1.8%), HDL-C (15.0% vs. 4.5%), and fasting insulin (-48.5% vs. -5.6%).
In SURMOUNT-OSA, study 2, tirzepatide MTD led to a significant improvement compared to placebo in triglycerides (-35.2% vs. -5.4%), non-HDL-C (-15.8% vs. -1.8%), HDL-C (15.0% vs. 4.5%), and fasting insulin (-48.5% vs. -5.6%). Molecular weight: 4,813 daltons.
Molecular weight: 4,813 daltons.