1 Name of Medicine
Nimodipine.
2 Qualitative and Quantitative Composition
Nimodipine is a yellow crystalline substance, practically insoluble in water.
Nimodipine is light sensitive but to a much lesser degree than nifedipine.
Nimodipine Juno is available as a 0.2 mg/mL concentrated intravenous infusion solution.
Excipients with known effect.
Ethanol.
For the full list of excipients, see Section 6.1 List of Excipients.3 Pharmaceutical Form
Nimodipine Juno concentrated intravenous infusion solution is presented as a clear slightly yellowish solution containing 10 mg nimodipine/50 mL and 10 g alcohol/50 mL in a glass vial.
4.1 Therapeutic Indications
Prophylaxis and treatment of ischaemic neurological deficits caused by cerebral vasospasm after subarachnoid haemorrhage following ruptured intracranial aneurysm, in patients who are in good neurological condition post-ictus, e.g. Hunt and Hess Grades I-III (see Section 5 Pharmacological Properties).
4.2 Dose and Method of Administration
Nimodipine tablet is unavailable in this brand however is available in other brands. Where correct dosing requires nimodipine tablet formulation, refer to the specific product information for this formulation for its complete dosage and administration instructions.
Dosage: Nimodipine Juno concentrated intravenous infusion solution.
For single use in one patient only. Discard any residue.
Continuous intravenous infusion.
Nimodipine Juno concentrated intravenous infusion solution must be administered by co-infusion via a three-way stopcock to the central catheter. The initial dosage is 5 mL Nimodipine Juno concentrated intravenous solution (= 1 mg nimodipine) per hour infused continuously for the first 2 hours (approximately 15 microgram/kg body weight/hr). Co-infusion solution must be administered at a rate of 20 mL per hour with this initial dosage. If this dosage is tolerated, particularly if there is no severe reduction in blood pressure, the dosage should then be increased to 10 mL Nimodipine Juno concentrated intravenous infusion solution per hour (= 2 mg nimodipine/h) (approximately 30 microgram/kg body weight/hr) with a corresponding increase in the rate of co-infusion solution to 40 mL per hour.
Patients whose body weights are distinctly below 70 kg or who have labile blood pressure can start with a dose of 2.5 mL Nimodipine Juno concentrated intravenous infusion solution/hr (= 0.5 mg nimodipine/h) with corresponding reduction in the rate of co-infusion and, if at all possible, the dosage should not be raised above 5 mL nimodipine concentrated intravenous infusion solution per hour. The treatment should be discontinued if necessary.
Intracisternal instillation.
Intracisternal instillation has been employed in uncontrolled trials in combination with IV/oral administration. A 1:19 ratio for dilution with Ringer's was tested in vitro with a very small risk of crystallisation. The dilute solution of nimodipine was used immediately after preparation. If the dilute solution is not used immediately, it should be discarded.
Patients with hepatic insufficiency may have substantially reduced clearance and approximately doubled plasma concentration; dosage should be reduced to 2.5 mL Nimodipine Juno concentrated intravenous infusion solution per hour and/or one nimodipine tablet (30 mg, available in other brands) every 4 hours in these patients.
In cases of severely disturbed kidney or liver function, particularly in cirrhosis of the liver, the effects and side effects, e.g. the reduction in blood pressure, may be more pronounced. In such cases the dose should, if necessary, be reduced in accordance with blood pressure monitoring and the ECG.
Administration: Nimodipine Juno concentrated intravenous infusion solution.
Nimodipine Juno concentrated intravenous infusion solution is administered as a continuous intravenous infusion via a central catheter using an infusion pump. A three-way stopcock should be used to connect the Nimodipine Juno polyethylene tube with the co-infusion line and the central catheter.
Only infusion pumps with polyethylene (PE) infusion tubing, polypropylene (PP) syringes and polyethylene or polypropylene extensions, taps, connectors may be used. Do not use polyvinylchloride (PVC) infusion tubing as nimodipine is adsorbed by the tubing.
Polyethylene or polyurethane catheters are to be used, only in conjunction with a polycarbonate stop-cock.
PVC Y-connector tubing must not be used and the rates of administration of recommended co-infusion solutions must be followed due to the possibility of crystal formation as seen in in vitro tests with Nimodipine Juno concentrated intravenous infusion solution at higher dilutions.
All infusion tubings must be changed every 24 hours.
Nimodipine Juno concentrated intravenous infusion solution should be co-infused with approximately 40 mL/h of any of the following infusion solutions which are compatible at the recommended 1 to 4 mixing ratio:
Sodium chloride intravenous infusion 0.9%, glucose intravenous infusion 5% (Glucose 5%), compound sodium lactate intravenous infusion solution (Hartmann's solution for injection/lactated Ringer's solution), lactated Ringer's solution with magnesium, Dextran 40, Mannitol (10%), hetastarch 6% (Poly (0-2-hydroxyethyl) starch 6%), Human albumin 5% or blood.
Nimodipine Juno concentrated intravenous infusion solution must not be mixed with any other drugs and must not be added to an infusion bag or bottle. Infusion solutions other than those recommended above should not be used. Nimodipine Juno concentrated intravenous infusion solution has a pH of 6.0-7.5.
Parenteral drug products should be inspected visually for particulate matter and colour change prior to administration. Any residual solution should not be kept for later use.
Nimodipine concentrated intravenous infusion solution is slightly light-sensitive. Its use in direct sunlight should be avoided. No special protective measures need be taken for up to 10 hours if Nimodipine Juno concentrated intravenous infusion solution is being administered in diffuse daylight or in artificial light.
Administration of Nimodipine Juno concentrated intravenous infusion solution should be continued during anaesthesia, surgery, and angiography.
Duration of administration.
Prophylaxis and treatment of ischaemic symptoms caused by vasospasm after subarachnoid haemorrhage should commence as soon as possible or within 4 days of the diagnosis of SAH and continue for at least 7 days up to a maximum of 14 days.
If during prophylactic administration of nimodipine, the source of the haemorrhage is treated surgically, intravenous treatment with nimodipine should be continued post-operatively for at least 5 days.
After the end of the infusion therapy, it is advisable to continue with oral administration (available in other brands).4.3 Contraindications
Nimodipine tablet is unavailable in this brand, however this dosage form is available in other brands. Contraindications, Special warnings and precautions for use, Interactions with other medicines and other forms of interactions, Fertility, pregnancy and lactation and Pharmacological properties information obtained using nimodipine tablet formulation is also included in the following sub-sections for prescriber information.
Nimodipine Juno concentrated intravenous infusion solution must not be used in cases of hypersensitivity to nimodipine or any of the excipients.
The use of nimodipine tablets (available in other brands) in combination with rifampicin is contraindicated as efficacy of nimodipine tablets may be significantly reduced when concomitantly administered with rifampicin (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
The concomitant use of oral nimodipine (available in other brands) and the antiepileptic drugs phenobarbital, phenytoin or carbamazepine is contraindicated as efficacy of nimodipine tablets may be significantly reduced (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
4.4 Special Warnings and Precautions for Use
Blood pressure.
Nimodipine has the haemodynamic effects expected of a calcium channel blocker although they are generally not marked at usual therapeutic doses. Blood pressure should be carefully monitored during treatment with nimodipine as a decrease in blood pressure has been reported in about 5% to 7% of SAH patients receiving oral nimodipine. Caution is required in patients with hypotension (systolic pressure lower than 100 mm Hg). The use of nimodipine is not generally recommended in patients taking antihypertensive drugs, including other calcium channel blockers, since it may potentiate the effects of these medications.
Simultaneous intravenous administration of β-blockers can lead to the mutual potentiation of negative inotropic effects and even to decompensated heart failure.
Please refer also to the section on Use in renal impairment.
In patients with unstable angina or within the first 4 weeks after acute myocardial infarction, physicians should consider the potential risk (e.g. reduced coronary artery perfusion and myocardial ischaemia) versus the benefit (e.g. improvement of brain perfusion).
Cerebral oedema or severely raised intracranial pressure.
Although treatment with nimodipine has not been shown to be associated with increases in intracranial pressure, cautious use and close monitoring is recommended in these cases when the water content of the brain tissue is elevated (generalised cerebral oedema).
Use in renal impairment.
There are insufficient data on patients with impaired renal function. However, patients with severe renal insufficiency should be carefully monitored with respect to any lowering of blood pressure when receiving nimodipine treatment.
Renal function should be closely monitored during intravenous nimodipine treatment in patients with known renal disease and/or receiving nephrotoxic drugs simultaneously (e.g. aminoglycosides, cephalosporins, frusemide). If deterioration is found discontinuation of the treatment should be considered.
Use in hepatic impairment.
The metabolism of nimodipine is decreased in patients with impaired hepatic function. Such patients should have their blood pressure and pulse rate monitored closely and should be given a lower dose (see Section 4.2 Dose and Method of Administration).
Elevations in one or more liver function test result, including elevated serum concentrations of LDH, alkaline phosphatase, or ALT (SGPT), have been reported in less than 1% of patients with SAH receiving oral nimodipine. Reversible increases in creatinine kinase (CK), creatinine phosphokinase (CPK), AST (SGOT), ALT (SGPT), gamma glutamyl transferase (GGT), gamma-glutamyltranspeptidase (GGTP), bilirubin and amylase also have been reported in patients receiving nimodipine, principally during intravenous administration of the drug. It has been suggested that such increases in liver function test results were caused by alcohol in the intravenous formulation rather than by the drug itself; however, in at least 2 studies, alcohol could not be detected in the blood of patients receiving an alcohol-containing nimodipine injection, and elevated transaminase concentrations also have been reported following oral administration of the drug in clinical studies.
Adverse hepatic effects reported in less than 1% of patients with SAH receiving oral nimodipine include hepatitis and jaundice.
Intestinal pseudo-obstruction and ileus.
Intestinal pseudo-obstruction (paralytic ileus) has been reported rarely. A causal relationship to nimodipine cannot be ruled out. In three cases, the condition responded to conservative management, but a fourth patient required surgical decompression of the extremely distended colon.
Alcohol content.
When treatment with Nimodipine Juno concentrated intravenous infusion solution is administered during pregnancy, the benefits and the potential risks must be carefully assessed according to the severity of the clinical situation.
Nimodipine Juno concentrated intravenous infusion solution contains 23.7% ethanol (alcohol), i.e. up to 50 g per daily dose (250 mL). This may be harmful for those suffering from alcoholism or impaired alcohol metabolism and should be taken into account in pregnant or breast feeding women, children, and high-risk groups such as patients with liver disease or epilepsy. The amount of alcohol in this product may alter the effects of other medicines (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Drugs altering the cytochrome P450 3A4 system.
Nimodipine is metabolised via the cytochrome P450 3A4 system. Drugs that are known to either inhibit or to induce this enzyme system may therefore alter the first pass or the clearance of nimodipine (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Drugs, which are known inhibitors of the cytochrome P450 3A4 system and therefore may lead to increased plasma concentrations of nimodipine are, e.g. macrolide antibiotics (e.g. erythromycin), anti-HIV protease inhibitors (e.g. ritonavir), azole antimycotics (e.g. ketoconazole), the antidepressants nefazodone and fluoxetine, quinupristin/dalfopristin, cimetidine, and valproic acid.
Upon co-administration with these drugs, blood pressure should be monitored and, if necessary, a reduction of the nimodipine dose should be considered.
Dermatologic effects.
Rash, requiring discontinuance of the drug in at least one case, and acne have been reported in less than 1% of patients with SAH receiving oral nimodipine. Pruritus, diaphoresis, and haematoma also have been reported in less than 1% of such patients.
Use in the elderly.
No data available.
Paediatric use.
Safety and effectiveness in children have not been established.
Effects on laboratory tests.
No data available.4.5 Interactions with Other Medicines and Other Forms of Interactions
Hypotensive agents.
In patients with elevated blood pressure who are receiving antihypertensive drugs, Nimodipine Juno can potentiate the blood-pressure-lowering effect of the concomitant medication. Blood pressure should be carefully monitored.
Drugs that affect nimodipine.
Nimodipine is metabolised via the cytochrome P450 3A4 system, located both in the intestinal mucosa and in the liver. Drugs that are known to either inhibit or to induce this enzyme system may therefore alter the first pass or the clearance of nimodipine.
The extent as well the duration of interactions should be taken into account when administering nimodipine together with the following drugs:
Rifampicin.
Rifampicin is expected to increase the rate of metabolism of Nimodipine Juno tablets due to enzyme induction, as experienced with other calcium antagonists such as nifedipine. Thus, the efficacy of Nimodipine Juno tablets may be significantly reduced when concomitantly administered with rifampicin. The use of nimodipine in combination with rifampicin is therefore contraindicated (see Section 4.3 Contraindications).
Anticonvulsants.
Few data are available on the interaction of nimodipine and anticonvulsant drugs. However, a study of epileptic patients receiving long-term treatment with the anticonvulsants carbamazepine, phenobarbitone or phenytoin, either alone or in combination, showed that plasma concentrations of nimodipine given as a single oral dose of 60 mg were markedly reduced (approx. 7 fold decrease in AUC and 8-10 fold in Cmax). This was due to the well-known enzyme inducing properties of these antiepileptic drugs, leading to a reduced oral bioavailability of nimodipine by enhanced first pass metabolism. This phenomenon has been reported for many high clearance drugs like nimodipine and also for other dihydropyridine calcium antagonists.
Thus, the concomitant administration of anticonvulsants and oral nimodipine is contraindicated in epileptic patients or patients on long-term/chronic anticonvulsant therapy, because the nimodipine serum concentration may be considerably lowered due to the induction of drug-metabolising enzymes (see Section 4.3 Contraindications).
A general guide concerning dose adjustments of nimodipine tablets is not possible because the extent of enzyme induction and changed capacity for nimodipine first pass metabolism may show large inter-individual differences.
Conversely, nimodipine plasma concentrations following administration of 60 mg single oral dose were increased (approx. 50%) in epileptic patients on long-term sodium valproate therapy. These patients may require smaller doses. The simultaneous administration of valproic acid can lead to an increase in the plasma nimodipine concentration (see Section 4.4 Special Warnings and Precautions for Use).
Effect of nimodipine on anticonvulsant therapy.
No effect was observed on the steady state plasma concentrations of the abovementioned anticonvulsants following the administration of a single oral 60 mg dose of nimodipine. Multiple dosing has not been investigated, but no effect of nimodipine on the bioavailability of these drugs is expected.
Upon co-administration with the following inhibitors of the cytochrome P450 3A4 system the blood pressure should be monitored and, if necessary, an adaptation in the nimodipine dose should be considered (see Section 4.2 Dose and Method of Administration).
Macrolide antibiotics (e.g. erythromycin).
No interaction studies have been carried out between nimodipine and macrolide antibiotics. Certain macrolide antibiotics are known to inhibit the cytochrome P450 3A4 system and the potential for drug interaction cannot be ruled out at this stage. Therefore, macrolide antibiotics should not be used in combination with nimodipine (see Section 4.4 Special Warnings and Precautions for Use). Azithromycin, although structurally related to the class of macrolide antibiotic, does not inhibit CYP3A4.
Anti-HIV protease inhibitors (e.g. ritonavir).
No formal studies have been performed to investigate the potential interaction between nimodipine and anti-HIV protease inhibitors. Drugs of this class have been reported to be potent inhibitors of the cytochrome P450 3A4 system. Therefore, the potential for a marked and clinically relevant increase in nimodipine plasma concentrations upon co-administration with these protease inhibitors cannot be excluded (see Section 4.4 Special Warnings and Precautions for Use).
Azole anti-mycotics (e.g. ketoconazole).
A formal interaction study investigating the potential of drug interaction between nimodipine and ketoconazole has not been performed. Azole anti-mycotics are known to inhibit the cytochrome P450 3A4 system, and various interactions have been reported for other dihydropyridine calcium antagonists. Therefore, when administered together with oral nimodipine, a substantial increase in systemic bioavailability of nimodipine due to a decreased first-pass metabolism cannot be excluded (see Section 4.4 Special Warnings and Precautions for Use).
Nefazodone.
No formal studies have been performed to investigate the potential interaction between nimodipine and nefazodone. This antidepressant drug has been reported to be a potent inhibitor of the cytochrome P450 3A4. Therefore, the potential for an increase in nimodipine plasma concentrations upon co-administration with nefazodone cannot be excluded (see Section 4.4 Special Warnings and Precautions for Use).
Fluoxetine.
The steady-state concomitant administration of nimodipine with the antidepressant fluoxetine led to about 50% higher nimodipine plasma concentrations. Fluoxetine exposure was markedly decreased, while its active metabolite norfluoxetine was not affected.
Nortryptyline.
The steady-state concomitant administration of nimodipine and nortryptyline led to a slight decrease in nimodipine exposure with unaffected nortryptyline plasma concentrations.
Quinupristin/dalfopristin.
Based on experience with the calcium-antagonist nifedipine, co-administration of quinupristin/dalfopristin may lead to increased plasma concentrations of nimodipine (see Section 4.4 Special Warnings and Precautions for Use).
Cimetidine.
A study in eight healthy volunteers has shown a 50% increase in mean peak nimodipine plasma concentrations and a 90% increase in the mean area under the curve, after a one-week course of cimetidine at 1,000 mg/day and nimodipine at 90 mg/day. This effect may be mediated by the known inhibition of hepatic cytochrome P-450 by cimetidine, which could decrease first-pass metabolism of nimodipine (see Section 4.4 Special Warnings and Precautions for Use).
Antineoplastic agents.
There is in vitro evidence that calcium-channel blocking agents, including nimodipine can enhance the cytotoxic effects of certain antineoplastic agents, e.g. doxorubicin, vincristine, but the clinical importance of these findings remains to be established.
Effects of nimodipine on other drugs.
Hypotensive agents.
Nimodipine may increase the blood pressure lowering effect of concomitantly applied antihypertensives, such as: diuretics, β-blockers, ACE inhibitors, A1-antagonists, other calcium antagonists, α-adrenergic blocking agents, PDE5 inhibitors, α-methyldopa.
However, if a combination of this type proves unavoidable particularly careful monitoring of the patient is necessary.
Zidovudine.
In a monkey study, simultaneous administration of zidovudine i.v. and nimodipine bolus i.v. resulted in a significantly higher AUC and significantly reduced distribution volume and clearance for zidovudine.
Other forms of interaction.
Because nimodipine concentrated intravenous infusion solution contains 23.7% (v/v) of ethanol, interactions with alcohol-incompatible medicines should be taken into consideration (see Section 4.4 Special Warnings and Precautions for Use).
Renal function can deteriorate if potentially nephrotoxic drugs are given simultaneously with Nimodipine Juno (see Section 4.4 Special Warnings and Precautions for Use).
Drug-food interaction.
Grapefruit juice.
Grapefruit juice inhibits the oxidative metabolism of dihydropyridines. Concomitant intake of grapefruit juice and nimodipine can result in increased plasma concentrations and prolonged action of nimodipine due to a decreased first pass metabolism or reduced clearance.
As a consequence, the blood pressure lowering effect may be increased. After intake of grapefruit juice this effect may last for at least 4 days after the last ingestion of grapefruit juice.
Ingestion of grapefruit/ grapefruit juice is therefore to be avoided while taking nimodipine.4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
No adverse effects on fertility were observed in male and female rats treated orally with nimodipine at 30 mg/kg/day (0.8 times the maximum recommended human dose on a mg/m2 body surface area basis). In single cases of in vitro fertilisation calcium channel blockers have been associated with reversible biochemical changes in the spermatozoa's head section that may result in impaired sperm function.
(Category C)
Animal studies have shown no consistent evidence of teratogenic activity in rats or rabbits at oral doses up to 100 mg and 30 mg/kg/day respectively (2.5- and 1.5-times the maximum recommended human dose on a mg/m2 body surface area basis), or at intravenous doses up to 0.5 mg/kg/day in both species (estimated relative exposure, 0.1-0.2). Nimodipine was embryotoxic in rats, causing reduced fetal weight from 30 mg/kg/day and resorption at 100 mg/kg/day when administered orally during organogenesis (estimated relative exposure, 0.8 and 2.5, respectively). No embryotoxicity occurred in rabbits at oral doses up to 10 mg/kg/day (estimated relative exposure, 0.5). Peri/postnatal studies in rats showed that oral doses of 30 mg/kg/day were associated with marginally higher incidences of skeletal variation, stunted fetuses and stillbirths. Nimodipine carries the potential to produce fetal hypoxia associated with maternal hypotension.
There are no adequate and well controlled studies in pregnant women to assess directly the effect on human fetuses. Nimodipine should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Nimodipine and its metabolites have been shown to appear in breast milk at concentrations of the same order of magnitude as corresponding maternal plasma concentrations. Nursing mothers are advised not to breast feed their babies when taking the drug.4.7 Effects on Ability to Drive and Use Machines
In principle the ability to drive and use machines can be impaired in connection with the possible occurrence of dizziness.
4.8 Adverse Effects (Undesirable Effects)
Adverse drug reactions (ADRs) based on clinical trials with nimodipine in the indication SAH sorted by CIOMS III categories of frequency (placebo-controlled studies: nimodipine N=703; placebo= 692; uncontrolled studies: nimodipine N=2496; status 31 Aug 2005) are listed below.
The frequencies of ADRs reported with nimodipine are summarised in Table 1. Within each frequency grouping, adverse effects are presented in order of decreasing seriousness. Frequencies are defined as: uncommon (≥ 1/1,000 to < 1/100); rare (≥ 1/10,000 to < 1/1,000).
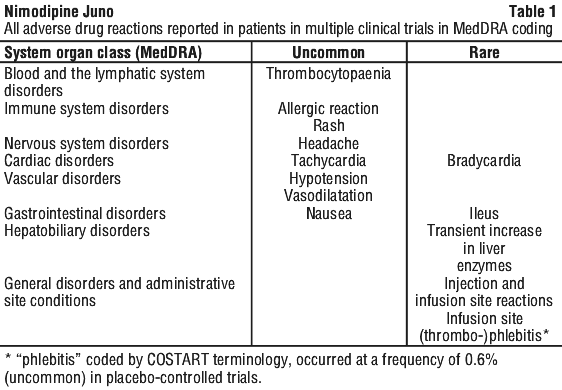
Post marketing adverse events.
Events described in MedDRA preferred terms:
Investigations/ vascular disorders.
hypotension.
Nervous system disorders.
headache.
Gastrointestinal.
nausea and vomiting.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at http://www.tga.gov.au/reporting-problems.4.9 Overdose
Symptoms.
Symptoms of acute overdosage to be anticipated are flushing, headache, marked lowering of the blood pressure, tachycardia or bradycardia, and (after oral administration) gastrointestinal complaints and nausea.
Treatment of overdosage.
In the event of acute overdosage, treatment with Nimodipine Juno must be discontinued immediately. Active cardiovascular support should include close monitoring of cardiac and respiratory function. Intravenous dopamine or noradrenaline may be helpful in restoring blood pressure. Since no specific antidote is known, subsequent treatment for other side effects should be governed by the most prominent symptoms. Since Nimodipine Juno is highly protein bound, dialysis is not likely to be of benefit.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
Nimodipine belongs to the class of pharmacological agents known as calcium channel blockers. Nimodipine is a calcium channel blocking agent belonging to the 1,4-dihydropyridine group. The mechanism(s) of nimodipine's clinical benefit in patients with subarachnoid haemorrhage has not been fully elucidated. Current evidence suggests that it may have a preferential cerebral vasodilator action and/or a direct effect involving prevention of calcium overload in neurons. It dilates the small resistance cerebral vessels and increases the cerebral blood flow, the increased perfusion being generally more pronounced in brain regions with preliminary damage and restricted circulation than in healthy regions. The improvement in cerebral circulation is particularly evident in patients with cerebral vasospasm after subarachnoid haemorrhage, particularly in Hunt and Hess grades I-III patients (see Table 2). Nimodipine produces significant reductions in ischaemic neurological deficits caused by vasospasm and in mortality.
 The contractile processes of the cerebral arterial smooth muscle cells are dependent upon calcium ions, which enter these cells during depolarisation as slow ionic transmembrane currents. Nimodipine binds to specific receptor sites in the central nervous system. It inhibits calcium ion transfer into these cells and inhibits contractions of vascular smooth muscle.
The contractile processes of the cerebral arterial smooth muscle cells are dependent upon calcium ions, which enter these cells during depolarisation as slow ionic transmembrane currents. Nimodipine binds to specific receptor sites in the central nervous system. It inhibits calcium ion transfer into these cells and inhibits contractions of vascular smooth muscle.
Clinical trials.
In animal experiments, nimodipine had a greater effect on cerebral arteries than on arteries elsewhere in the body. It is highly lipophilic, allowing it to cross the blood-brain barrier; concentrations of nimodipine as high as 12.5 nanogram/mL have been detected in the cerebrospinal fluid of nimodipine treated subarachnoid haemorrhage (SAH) patients.
Based on animal experiments, it was hoped that nimodipine would prevent cerebral arterial spasm in SAH patients. While clinical studies demonstrated a favourable effect by nimodipine on the severity of neurological deficits caused by cerebral vasospasm following SAH, there is no arteriographic evidence that the drug either prevents or relieves the spasm of these arteries. The actual mechanism of action in humans is, therefore, unknown.
5.2 Pharmacokinetic Properties
Absorption.
The orally administered active substance nimodipine is almost completely absorbed. The unchanged active substance and its early "first pass" metabolites are detected in plasma as little as 10-15 minutes after the ingestion of the tablet. Following multiple-dose oral administration (3 x 30 mg/day), the mean peak plasma concentrations (Cmax) are 7.3-43.2 nanogram/mL in elderly individuals, these being reached after 0.6-1.6 h (tmax). The peak plasma concentration and the area under the curve increase proportionally to the dose up to the highest dose under test (90 mg).
Using continuous infusions of 0.03 mg/kg/h, mean steady-state plasma concentrations of 17.6-26.6 nanogram/mL are achieved. After intravenous bolus injections, the plasma nimodipine concentrations fall biphasically with half-lives of 5-10 minutes and about 60 minutes. The distribution volume (Vss, 2-compartment model) for intravenous administration is calculated to be 0.9-1.6 L/kg body weight. The total (systemic) clearance is 0.6-1.9 L/h/kg. (See Figure 1.)
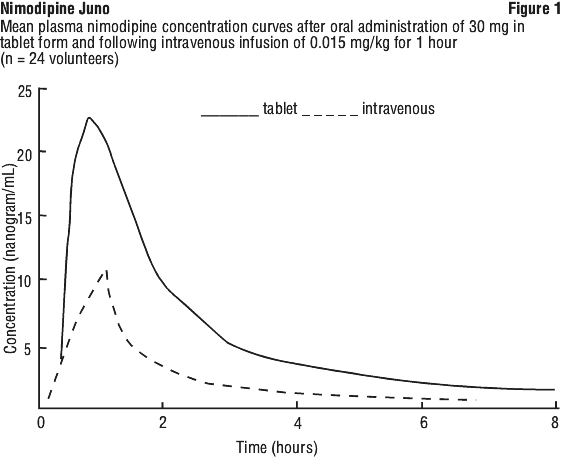 Nimodipine undergoes extensive first pass metabolism in the liver. The mean bioavailability of nimodipine tablets ranges from ± 3-12% in healthy individuals to 16% (range 3-30%) in patients with SAH.
Nimodipine undergoes extensive first pass metabolism in the liver. The mean bioavailability of nimodipine tablets ranges from ± 3-12% in healthy individuals to 16% (range 3-30%) in patients with SAH.
Bioavailability is significantly increased in patients with hepatic disease (e.g. cirrhosis) with Cmax approximately double that in normal patients which necessitates lowering the dose in this group of patients (see Section 4.2 Dose and Method of Administration).
The effects of a standard breakfast on the bioavailability of nimodipine tablets were investigated in two separate studies. From the results it was concluded that, although the rate of absorption is delayed as evidenced by the decrease in Cmax (of approx. 40%) and the increase of tmax (approx. 100%), the presence of food does not alter the extent of absorption of nimodipine tablets.
Distribution.
Studies in animals indicate that nimodipine is widely distributed into body tissues after oral or intravenous administration. Following intravenous administration in healthy individuals, nimodipine distributes rapidly into the central compartment with a half-life of approximately 67 minutes; the volume of distribution of the central compartment averaged 0.43 L/kg. The steady-state volume of distribution following intravenous administration has been reported to range from 0.94-2.3 L/kg. Plasma protein binding of unchanged nimodipine averages more than 95% and is independent of concentration over a range of 10 nanogram/mL to 10 microgram/mL.
Nimodipine appears to distribute to a limited extent into CSF. During intravenous infusion of nimodipine at a rate of 2 mg/hour for up to 14 days in patients with SAH, mean CSF and plasma concentrations of nimodipine averaged approximately 0.3 and 77 nanogram/mL, respectively. After oral administration of nimodipine 0.35 mg/kg every 4 hours for 3 weeks, mean CSF and plasma nimodipine concentrations were 0.77 and 6.9 nanogram/mL, respectively. However, concentrations as high as 12.5 nanogram/mL reportedly have been detected.
Nimodipine and/or its metabolites have been shown to appear in rat milk at concentrations much higher than in maternal plasma. Nimodipine itself has been shown to appear in human breast milk; the concentrations were lower than in maternal plasma.
Excretion.
Nimodipine concentrations appear to decline in a biphasic manner. The half-life (T½) was 1.21.8 hours after intravenous infusion; after oral administration, the elimination T½ was 5-10 hours and dose-independent. The elimination T½ from plasma of total radioactivity was 14 hours with 3H nimodipine.
No sign of accumulation was noted in patients receiving 40 mg nimodipine three times daily for 7 days.
Nimodipine is extensively metabolised in the liver via the cytochrome P450 3A4 system, with approximately 10%, or less than 1%, of an orally administered dose present in plasma or urine, respectively, as unchanged drug (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). All metabolites of nimodipine are either inactive or substantially less active than the parent drug.
Cumulative excretion of metabolites in urine is approximately 50% of the dose after 48 hours and 30% in faeces.
Plasma clearance of nimodipine varies considerably, averaging 0.84 L/kg per hour (range: 0.51-1.15 L/kg per hour) in healthy individuals and 1.18 L/kg per hour (range: 0.57-1.77 L/kg per hour) in patients with SAH. Clearance of nimodipine may be decreased substantially in patients with hepatic dysfunction.
Patients with renal impairment showed a substantial prolongation of nimodipine elimination half-life and a reduction in plasma clearance of the drug compared with healthy individuals. These findings may have been attributable in part to age related reductions in liver function in patients with renal impairment, who were substantially older (mean age 65.3 years) than healthy controls (mean age 25.2 years). An additional study in patients with different degrees of creatinine clearance suggests no systemic accumulation of the drug.
5.3 Preclinical Safety Data
Genotoxicity.
Nimodipine was not mutagenic when tested in bacteria (S. typhimurium strains TA98, TA100, TA1535 and TA1537) and yeast (Saccharomyces cerevisiae). Weak clastogenicity was observed in vitro in assays with Chinese Hamster ovary cells in the presence of metabolic activation, but chromosomal damage was not evident in vivo in either the mouse micronucleus test or the dominant lethal test.
Carcinogenicity.
Nimodipine was not tumorigenic in male and female mice treated with oral doses up to 546 and 774 mg/kg/day, respectively, for 21 months (estimated relative exposure, 7-10 based on mg/m2 body surface area). No treatment-related increase in the incidence of tumours was observed in rats administered oral doses of nimodipine of up to 91 mg/kg/day (males) or 121 mg/kg/day (females) for 2 years (estimated relative exposure, 2-3 based on mg/m2 body surface area).6 Pharmaceutical Particulars
6.1 List of Excipients
Nimodipine Juno concentrated intravenous infusion solution contains ethanol (200 mg/mL), macrogol 400, sodium citrate dihydrate, citric acid and water for injections as excipients.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Nimodipine Juno concentrated intravenous infusion solution has good stability, but is somewhat sensitive to light, and therefore must not be used in direct sunlight. The product should be stored in the manufacturer's light-protective glass bottle container within the cardboard carton. If appropriate, infusion pumps and tubing must be protected with opaque coverings, or black, brown, yellow or red infusion lines can be used. However, in diffuse daylight or artificial light, Nimodipine Juno concentrated intravenous infusion solution can be used for up to 10 hours without protection from light. Protect from freezing. Store below 25°C.
6.5 Nature and Contents of Container
Nimodipine Juno concentrated intravenous infusion solution.
Clear slightly yellowish solution containing 10 mg nimodipine/50 mL contained in a topaz glass vial with a grey rubber closure and sealed with a flip off top. Pack of 1 glass vial.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical name: Nimodipine is isopropyl (2-methoxyethyl) 1,4-dihydro-2,6-dimethyl-4- (3-nitrophenyl) -3,5-pyridine-dicarboxylate.
Chemical structure.

CAS number.
66085-59-4.
Molecular weight: 418.5.
Molecular formula: C21H26N2O7.7 Medicine Schedule (Poisons Standard)
Schedule 4 Prescription only Medicine.
Summary Table of Changes



 The contractile processes of the cerebral arterial smooth muscle cells are dependent upon calcium ions, which enter these cells during depolarisation as slow ionic transmembrane currents. Nimodipine binds to specific receptor sites in the central nervous system. It inhibits calcium ion transfer into these cells and inhibits contractions of vascular smooth muscle.
The contractile processes of the cerebral arterial smooth muscle cells are dependent upon calcium ions, which enter these cells during depolarisation as slow ionic transmembrane currents. Nimodipine binds to specific receptor sites in the central nervous system. It inhibits calcium ion transfer into these cells and inhibits contractions of vascular smooth muscle. Nimodipine undergoes extensive first pass metabolism in the liver. The mean bioavailability of nimodipine tablets ranges from ± 3-12% in healthy individuals to 16% (range 3-30%) in patients with SAH.
Nimodipine undergoes extensive first pass metabolism in the liver. The mean bioavailability of nimodipine tablets ranges from ± 3-12% in healthy individuals to 16% (range 3-30%) in patients with SAH.
