What NuvaRing contains:
Composition in Full
NuvaRing contains:
- active substances: etonogestrel (11.7 mg) and ethinylestradiol (2.7 mg);
- other substances: ethylene vinylacetate copolymer (a type of plastic that will not dissolve in the body): Evatane 28-25RG (proprietary ingredient 139830) and Evatane 1020VN3 (proprietary ingredient 140194)
- magnesium stearate.
Etonogestrel and ethinylestradiol are released from the ring at a rate of 0.120 mg/day and 0.015 mg/day respectively, each for 3 weeks.
1. WHAT NUVARING IS AND WHAT IT IS USED FOR
NuvaRing is a contraceptive vaginal ring used to prevent pregnancy. Each ring contains a small amount of two female sex hormones - etonogestrel and ethinylestradiol. The ring slowly releases these hormones into the blood circulation. Because of the low amount of hormones that is released, NuvaRing is considered a low-dose hormonal contraceptive. Since NuvaRing releases two different types of hormones it is a so-called combined hormonal contraceptive.
NuvaRing works just like a combined contraceptive pill (the Pill) but instead of taking a pill every day, the ring is used for 3 weeks in a row. NuvaRing releases two female sex hormones that prevent the release of an egg cell from the ovaries. If no egg is released you cannot become pregnant. An advantage of NuvaRing is that you do not have to remember to take a pill every day.
NuvaRing is very reliable, but as for all contraceptive methods, protection is never 100%. If NuvaRing is used according to the directions, your chance of getting pregnant is less than 0.7% per year. For comparison purposes, if combined oral contraceptives are used diligently, the chance of getting pregnant is expected to be about 0.1% and if progestogen only pills ("mini pills") are used about 0.3%. Your chance of getting pregnant increases if NuvaRing is not used exactly according to the directions.
2. WHAT YOU NEED TO KNOW BEFORE YOU USE NUVARING
General notes
In this leaflet, several situations are described where you should stop using NuvaRing, or where NuvaRing may be less reliable. In such situations you should not have intercourse or you should take extra non-hormonal contraceptive precautions such as using a male condom or another barrier method. Do not use rhythm or temperature methods. These methods can be unreliable because NuvaRing alters the monthly changes of the body temperature and of the cervical mucous.
NuvaRing, like other hormonal contraceptives, does not protect against HIV infection (AIDS) or any other sexually transmitted disease.
2.1 When you should not use NuvaRing
In some situations you should not use a combined hormonal contraceptive. Tell your doctor if any of the following conditions apply to you. Your doctor may then advise you to use a different (non-hormonal) method of birth control.
Do not use NuvaRing:
- If you have, or have ever had a disorder affecting the blood vessels. In particular, this applies to conditions relating to thrombosis. Thrombosis is the formation of a blood clot. This may occur in the blood vessels of the legs (deep vein thrombosis), the lungs (pulmonary embolism), the heart (heart attack), the brain (stroke), or other parts of the body;
- if you have ever had a heart attack, or a stroke, or if you have (or have ever had) a condition that may be a first sign of a heart attack (such as angina pectoris, or severe chest pain) or stroke (such as a transient ischaemic attack [a TIA - a slight temporary stroke]);
- if you have a serious risk factor, or several risk factors for developing a blood clot - see also in section 2.2 'Blood clots (Thrombosis)';
- if you have a disorder affecting the blood clotting, for instance protein C deficiency;
- if you have major surgery (e.g., an operation) and your ability to move around is limited for a long period of time (see in section 2.2 'Blood clots (Thrombosis)').
- if you have (had) a type of migraine called 'migraine with aura' Ask your doctor if you are unsure;
- if you have diabetes with damaged blood vessels;
- if you have (had) an inflammation of the pancreas (pancreatitis) associated with high levels of fat in your blood;
- If you have jaundice (yellowing of the skin) or if you have or ever had severe liver disease and your liver is not yet working normally;
- if you have any unexplained vaginal bleeding;
- if you are allergic to ethinylestradiol or etonogestrel, or any of the other ingredients of NuvaRing;
- If you have or have had cancer of the breast or the genital organs;
- If you have or have had a benign or malignant tumour in the liver;
- If you are pregnant or think you might be pregnant.
If any of these conditions appear for the first time while using NuvaRing, remove the ring immediately and contact your doctor. In the meantime, use non-hormonal contraceptive measures.
Do not use NuvaRing if you have hepatitis C and are taking the combination drug regimen ombitasvir/paritaprevir/ritonavir with or without dasabuvir and medicinal products including glecaprevir and pibrentasvir (see in section 2.2 'Other medicines and NuvaRing').
For possible signs of a blood clot see in section 2.2 'Blood Clots (Thrombosis)'.
2.2 Warnings and precautions
In some situations you need to take special care while using a combined hormonal contraceptive.
Talk to your doctor before using NuvaRing if any of the following conditions apply to you. Also if the condition develops or gets worse while you are using NuvaRing you must tell your doctor.
- if you breast-feed a baby. The use of a hormonal contraceptive containing an estrogen is generally not recommended until the nursing mother has completely weaned her child;
- if you have diabetes;
- if you are overweight;
- if you have high blood pressure;
- if you have a heart valve disorder or a certain heart rhythm disorder;
- if you have an inflammation of your veins (superficial phlebitis);
- if you have varicose veins;
- if anyone in your immediate family has had a thrombosis, a heart attack or a stroke;
- if you suffer from migraine;
- if a close relative has or has ever had breast cancer;
- if you have epilepsy (see in section 2.2 'Other Medicines and NuvaRing');
- if you or someone in your immediate family has or had high blood levels of fatty substances (cholesterol or triglycerides);
- if you have liver disease (for instance jaundice) or gallbladder disease (for instance gallstones);
- if you have Crohn's disease or ulcerative colitis (chronic inflammatory bowel disease);
- if you have SLE (systemic lupus erythematosus; a disease affecting your natural defence system);
- if you have HUS (haemolytic uraemic syndrome; a disorder of blood clotting causing failure of the kidneys);
- if you have sickle cell anaemia (an inherited disease of the red blood cells);
- if you have elevated levels of fat in the blood (hypertriglyceridemia) or a positive family history for this condition. Hypertriglyceridemia has been associated with an increased risk of developing pancreatitis (inflammation of the pancreas) in women using hormonal contraceptives.
- if you have an operation, or if your ability to move around is limited for a long time (see in section 2.2 'Blood Clots (Thrombosis)';
- if you have a condition that occurred for the first time or worsened during pregnancy or previous use of sex hormones, e.g. hearing loss, porphyria (a disease of the blood), herpes gestationis (skin rash with vesicles during pregnancy), Sydenham's chorea (a disease of the nerves in which sudden movements of the body occur); hereditary and acquired angioedema (you should see your doctor immediately if you experience symptoms of angioedema such as swollen face, tongue and/or throat and/or difficulty swallowing or hives, potentially with difficulty breathing). Products containing estrogens may cause or worsen the symptoms of hereditary and acquired angioedema.
- if you have (or have ever had) chloasma [yellowish-brown pigment patches, so called 'pregnancy patches', particularly on the face]; if so, avoid too much exposure to the sun or ultraviolet light;
- if you have a medical condition that makes it difficult to use NuvaRing - e.g. if you are constipated, have a prolapse of the uterine cervix or have pain during intercourse;
- if you have recently given birth you are at an increased risk of blood clots. You should ask your doctor how soon after delivery you can start using NuvaRing (see in section 2.2 'Blood clots (Thrombosis)');
- if you have (or have ever had) an allergic reaction while using NuvaRing, including swelling of the face, lips, tongue, and/or throat causing difficulty in breathing or swallowing (angioedema and/or anaphylaxis);
- if you have a history of toxic shock syndrome (TSS).
Even if none of the conditions listed above applies to you, it is sensible to see your doctor regularly for a medical check-up, e.g. once every year.
Blood clots (Thrombosis)
Blood clots in a vein
A blood clot in a vein (known as a 'venous thrombosis') can block the vein. This can happen in veins in the leg, the lung (a lung embolus), or other organs.
Using combined hormonal contraceptives, including NuvaRing, increases a woman's risk of developing a venous thrombosis compared with a woman not using any combined hormonal contraceptive. The risk of developing a blood clot in a vein is highest during the first year of using a combined hormonal contraceptive for the first time. The risk is also higher if you restart using a combined hormonal contraceptive (the same product or a different product) after a break of 4 weeks or more. The risk is not as high as the risk of developing a blood clot during pregnancy. The risk of getting a blood clot with NuvaRing is similar to the risk contraceptive pills.
If you use a combined hormonal contraceptive your risk of venous thrombosis increases further:
- the older you are;
- if one of your close relatives has had a blood clot in the leg, lung or other organ at a young age;
- if you are overweight;
- if you must have an operation, or if your ability to move around is limited for a long period of time because of any injury or illness, or you have your leg in a plaster cast.
If this applies to you, it is important to tell your doctor that you are using NuvaRing, as the treatment may have to be stopped. Your doctor may tell you to stop using your hormonal contraception several weeks before surgery or while you are less mobile. Your doctor will also tell you when you can start using NuvaRing again after you are able to move around. See also section 2.1 'When should you not use NuvaRing'.
- if you gave birth less than a few weeks ago.
Blood clots in an artery
A blood clot in an artery can cause serious problems. For example, a blood clot in an artery in the heart causes a heart attack, or in the brain causes a stroke. Extremely rarely blood clots can occur in the liver, gut, kidney or eye.
The use of a combined hormonal contraceptive has also been connected with an increased risk of clots in the arteries. This risk increases further:
- the older you are;
- if you smoke.
When using a combined hormonal contraceptive like NuvaRing you are strongly advised to stop smoking, especially if you are older than about 35 years;
- if you are overweight;
- if you have high blood pressure. If you develop high blood pressure while using NuvaRing, you may be told to stop using it;
- if a close relative has had a heart attack or stroke at a young age;
- if you have a high level of fat in your blood (cholesterol or triglycerides);
- if you have diabetes;
- if you get migraine;
- if you have a problem with your heart (valve disorder, disturbance of the rhythm).
Symptoms of blood clots
Remove NuvaRing and contact your doctor immediately if you notice possible signs of a blood clot, such as:
- unusual pain and/or swelling in one of your legs;
- severe pain in the chest which may reach the left arm;
- sudden breathlessness;
- sudden cough without an obvious cause;
- any unusual, severe or long-lasting headache or worsening of migraine;
- partial or complete blindness or double vision;
- difficulty in speaking or inability to speak;
- giddiness or fainting;
- weakness, strange feeling, or numbness in any part of your body.
Following a blood clot recovery is not always complete. Very occasionally serious permanent disabilities may occur or the blood clot may even be fatal.
Cancer
The information given below was obtained from studies of women who used combined oral hormonal contraceptives, such as the combined pill, and from an additional study that included both oral and non-oral hormonal contraceptives, such as NuvaRing.
In studies with the combined pill, breast cancer has been found slightly more often in women using combined pills, but it is not known whether this is caused by the treatment. For example, it may be that tumours are found more in women on combined pills because they are examined by the doctor more often. The increased occurrence of breast cancer becomes gradually less after stopping the combined pill, so that 10 years after stopping the extra risk has gone.
In the additional study that included both oral and non-oral hormonal contraceptives, such as NuvaRing, the occurrence of breast cancer was reported to increase the longer the women used the contraceptive. The difference in the reported risk of breast cancer between women who had never used the contraceptive and those who had used the contraceptive was small: 13 additional cases of breast cancer per 100,000 women-years.
It is important to regularly check your breasts and you should contact your doctor if you feel any lump. You should also tell your doctor if a close relative has, or ever had breast cancer (see section 2.2 Warnings and precautions).
In rare cases benign liver tumours and in even fewer cases, malignant liver tumours have been reported in pill users. Contact your doctor if you have unusual severe abdominal pain.
Chronic infection with Human Papilloma Virus (HPV) is the single most important risk factor for cervical cancer. HPV is a sexually transmitted infection. In women who use combined oral contraceptives for a long time the chance of getting cervical cancer may be slightly higher. This finding may not be caused by the Pill itself but may be related to sexual behaviour and other factors.
Other medicines and NuvaRing
Always tell the doctor who prescribes NuvaRing which medicines or herbal products you are already using, including medicines obtained without a prescription. Also tell any other doctor or dentist who prescribes another medicine (or the dispensing pharmacist) that you use NuvaRing.
Some medicines may cause particular problems when you are using combined hormonal contraceptives, such as NuvaRing.
- There are medicines that can make NuvaRing less effective in preventing pregnancy, or can cause unexpected bleeding. These include medicines used to treat:
- epilepsy (e.g. primidone, phenytoin, phenobarbital, carbamazepine, oxcarbamazepine, topiramate, felbamate);
- tuberculosis (e.g. rifampicin);
- HIV infection (e.g. ritonavir, nelfinavir, nevirapine, efavirenz);
- Hepatitis C virus infection (e.g. boceprevir, telaprevir)
- other infectious diseases (e.g. griseofulvin).
- high blood pressure in the blood vessels of the lungs (bosentan). - The herbal product St. John's wort may also stop NuvaRing from working properly. If you want to use herbal products containing St. John's wort while you are already using NuvaRing you should consult your doctor first.
- If you are taking medicines or herbal products that might make NuvaRing less effective, a barrier contraceptive method should also be used. Since the effect of another medicine on NuvaRing may last up to 28 days after stopping the medicine, it is necessary to use the additional barrier contraceptive method for that long. Note: Do not use NuvaRing with a diaphragm, cervical cap, or a female condom.
- NuvaRing may also interfere with the working of other medicines - such as ciclosporin and the anti-epileptic lamotrigine.
- Do not use NuvaRing if you have Hepatitis C and are taking the combination drug regimen ombitasvir/paritaprevir/ritonavir with or without dasabuvir as this may cause increases in liver function blood test results (increase in ALT liver enzyme). NuvaRing can be restarted approximately 2 weeks after completion of treatment with the combination drug regimen. See section 2.1 'When you should not use NuvaRing'.
- If you are taking other Hepatitis C drug combinations (such as glecaprevir/pibrentasvir) you may experience increased levels of the liver enzyme “alanine aminotransferase” (ALT) in the blood.
You can use tampons while using NuvaRing. Insert NuvaRing before inserting a tampon. You should be careful when removing a tampon to be sure that the ring is not accidentally pulled out. If the ring does come out, simply rinse the ring in cool to lukewarm water (do not use hot water) and immediately reinsert it.
Ring breakage has occurred when also using a vaginal product such as a lubricant or treatment for infection (see section 3.4 'What to do if...Your ring breaks').
Using spermicides or vaginal yeast products will not reduce the contraceptive efficacy of NuvaRing.
Laboratory tests
If you are having any blood or urinary test, tell your health care professional that you are using NuvaRing as it may affect the results of some tests.
Pregnancy
NuvaRing must not be used by women, who are pregnant, or who think they may be pregnant.
If you get pregnant while using NuvaRing you should remove the ring and contact your doctor.
If you want to stop NuvaRing because you want to get pregnant, see section 3.4 'What to do if…You want to stop using NuvaRing'.
Breastfeeding
NuvaRing is not usually recommended for use during breast-feeding. If you wish to use NuvaRing while breastfeeding, please seek the advice of your doctor.
Driving and using machines
NuvaRing is unlikely to affect your ability to drive or use machines.
More about hormonal contraceptives
Combined hormonal contraceptives, like NuvaRing, may also have non-contraceptive health benefits. Your periods may be lighter and shorter. As a result, the risk of anaemia may be lower. Your period pains may become less severe or may completely disappear. Your period may be more confined to the ring-free period when you use NuvaRing.
Furthermore, the following serious disorders have been reported to occur less frequently in users of hormonal contraceptives with 50 micrograms of ethinylestradiol ('high-dosed' pills) than in non-users. This may also be the case for NuvaRing but this has not been confirmed.
- Cancer of the endometrium (the lining of the womb)
- Cancer of the ovaries
- Benign breast disease
- Ovarian cysts
- Pelvic infections (pelvic inflammatory disease or PID)
- Ectopic pregnancy (pregnancy in which the embryo implants outside of the uterus)
3. HOW TO USE NUVARING?
You can insert and remove NuvaRing yourself. Your doctor will tell you when to start using NuvaRing for the first time. The vaginal ring must be inserted on the correct day in your monthly cycle (see section 3.3 'When to start with the first ring') and left in place for 3 consecutive weeks. Regularly check that NuvaRing is still in your vagina (for example, before and after intercourse) to ensure that you are protected from pregnancy. After the third week, you take NuvaRing out and have a one week break. You will usually have your monthly period during this ring-free interval.
While using NuvaRing, you should not use certain female barrier contraceptive methods such as a vaginal diaphragm, cervical cap, or female condom as your back-up method of birth control because NuvaRing may interfere with the correct placement and position of a diaphragm, cervical cap, or female condom.
3.1 How to insert and remove NuvaRing
- Before inserting the ring, check it is not out of date (see section 6 'How to store NuvaRing').
- Wash your hands before inserting or removing the ring.
- See Figures 1 - 5 below for details
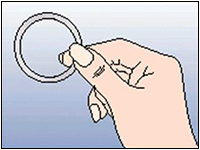
Figure 1: Take NuvaRing out of the sachet.
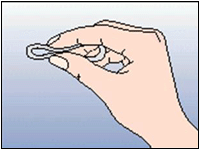
Figure 2: Hold the ring between your thumb and index finger, press the opposite sites together. Compress the ring.
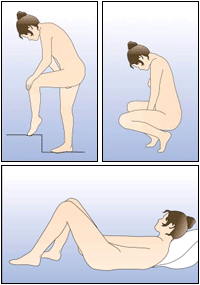
Figure 3: Choose a comfortable position to insert the ring, like standing with one leg up, squatting, or lying down.
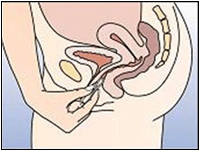
Figure 4a: Insert the ring into the vagina with one hand, if necessary the labia may be spread with the other.
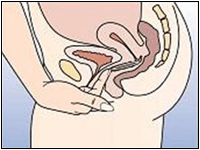
Figure 4b: Push the ring into the vagina until the ring feels comfortable. When NuvaRing is in place you should not feel anything. If you feel uncomfortable, gently change the position of the NuvaRing (e.g, push the ring a bit further into the vagina) until it is comfortable. The exact position of the ring inside the vagina is not important.
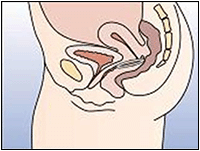
Figure 4c: Leave the ring in place for 3 weeks.
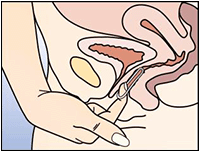
Figure 5: After 3 weeks, remove NuvaRing from the vagina. NuvaRing can be removed by hooking the index finger under the ring or by grasping the ring between the index and middle finger and pulling it out.
- Dispose of the used ring with the normal household waste, preferably inside the resealable sachet. Do not flush NuvaRing down the toilet.
3.2 Three weeks in, one week out
- Starting with the day you put it in, the vaginal ring must be left in place without interruption for 3 weeks.
- After 3 weeks you remove the ring on the same day of the week and at approximately the same time as it was put in. For example, if you put NuvaRing in on a Wednesday at about 22.00 h, you should remove the ring 3 weeks later, on Wednesday, at about 22.00 h.
- After you have removed the ring, you do not use a ring for 1 week. During this week a vaginal bleed should occur. Usually this starts 2-3 days after removal of NuvaRing.
- Start a new ring exactly after the 1 week interval (again on the same day of the week and approximately the same time), even if you have not stopped bleeding. If the new ring is inserted more than 3 hours too late, the protection from pregnancy may be reduced. Follow the instructions in section 3.4 'What to do if... You have forgotten to insert a new ring after the ring-free interval'.
If you use NuvaRing as described above, your vaginal bleed will take place every month on roughly the same days.
3.3 When to start with the first ring
- You have not used a hormonal contraceptive during the last month.
Insert the first NuvaRing on the first day of your natural cycle (i.e. the first day of your menstrual period). NuvaRing starts working straight away. You don't need to take any other contraceptive precautions.
You can also start NuvaRing between day 2 and day 5 of your cycle, but if you have sexual intercourse during the first 7 days of NuvaRing use make sure that you also use an additional contraceptive method (such as a male condom). You only have to follow this advice when you use NuvaRing for the first time. - You have used a combined Pill during the last month.
Start using NuvaRing at the latest the day following the tablet-free period of your present Pill. If your Pill pack also contains inactive tablets, start NuvaRing at the latest on the day after the last inactive tablet. If you are not sure which tablet this is, ask your doctor or pharmacist. Never extend the hormone-free interval of your current Pill pack beyond its recommended length.
If you have used the Pill consistently and correctly and if you are sure that you are not pregnant, you can also stop taking the Pill on any day of your current Pill pack and start using NuvaRing immediately. - You have used a transdermal patch during the last month.
Start using NuvaRing at the latest the day following your usual patch-free break. Never extend the patch-free break beyond its recommended length.
If you have used the patch consistently and correctly and if you are sure that you are not pregnant, you can also stop using the patch on any day and start using NuvaRing immediately. - You have used a minipill (progestagen-only pill) during the last month.
You can stop taking the minipill any day and start NuvaRing the next day, at the same time you would have normally taken your pill. But make sure you also use an additional contraceptive method (such as a male condom) for the first 7 days of ring use. - You have used an injectable or an implant or a progestagen-releasing intrauterine device (IUD) during the last month.
Start using NuvaRing when your next injection is due or on the day that your implant or your progestagen-releasing IUD is removed. But make sure you also use an additional contraceptive method (such as a male condom) for the first 7 days of ring use. - After having a baby.
If you have just had a baby, your doctor may tell you to wait until after your first normal period before you start using NuvaRing. Sometimes it is possible to start sooner. Your doctor will advise you. If you are breast-feeding and want to use NuvaRing, you should discuss this first with your doctor. - After a miscarriage or an abortion.
Your doctor will advise you. - When you have had irregular cycles or no bleeding
Your doctor will advise you.
3.4 What to do if…
You ring is accidentally expelled from the vagina
NuvaRing may accidentally be expelled from the vagina for example, if it has not been inserted properly, while removing a tampon, during sexual intercourse, during constipation, or if you have a prolapse of the womb. Therefore, it is a good habit to regularly check whether the ring is still in your vagina (for example, before and after intercourse).
Your ring has temporarily been out of the vagina
NuvaRing might still protect you from getting pregnant depending on how long it has been out of your vagina.
If the ring has been out of your vagina for:
- Less than 3 hours,
it will still protect you from pregnancy. You should rinse the ring with cold to lukewarm water (do not use hot water) and put the ring back in as soon as possible but only if the ring has been out of the vagina for less than 3 hours. - More than 3 hours during the 1st and 2nd week,
it may not protect you from pregnancy. You should rinse the ring with cold to lukewarm water (do not use hot water) and put the ring back in the vagina as soon as you remember, and leave the ring in place without interruption for at least 7 days. Use a male condom if you have sexual intercourse during these 7 days. If you are in your 1st week, and you had sexual intercourse during the past 7 days, there is a possibility you may be pregnant. In that case contact your doctor. - More than 3 hours in the 3rd week,
it may not protect you from pregnancy. You should discard that ring and choose between one of the following two options:
- Insert a new ring immediately:
This will start the next 3-week use period. You may not have your period, but breakthrough bleeding and spotting may occur.
- Do not insert the ring again.
Have your period first and insert a new ring no later than 7 days from the time the previous ring was removed or fell out. You should only choose this option if you have used NuvaRing continuously during the previous 7 days.
- An unknown amount of time,
you may not be protected from pregnancy. Perform a pregnancy test and consult your doctor prior to inserting a new ring.
Your ring breaks
Very rarely NuvaRing may break. A broken ring is unlikely to cause an overdose because the ring will not release a higher amount of contraceptive hormones. Vaginal injury associated with ring breakage has been reported.
If NuvaRing breaks, expulsion of the ring is likely to occur (see section 3.4 'What to do if…Your ring has temporarily been out of the vagina'). Therefore, if you notice that your NuvaRing has broken, discard that ring and replace it with a new ring as soon as possible.
You have inserted more than one ring/Overdose
There have been no reports of serious harmful effects due to an overdose of the hormones in NuvaRing. If you have accidentally inserted more than one ring, you may feel sick (nausea), or have vomiting or vaginal bleeding. Remove excess rings and contact your doctor if these symptoms persist.
You have forgotten to insert a new ring after the ring-free interval
If your ring-free interval was longer than 7 days, put a new ring in as soon as you remember. Use extra contraceptive precautions (such as a male condom) if you have sexual intercourse during the next 7 days. If you had sexual intercourse in the ring-free interval, there is a possibility you may be pregnant. In that case contact your doctor immediately. The longer the ring-free interval, the higher the risk that you have become pregnant.
You have forgotten to remove the ring
- If your ring has been left in place for between 3 and 4 weeks, it will still protect you from pregnancy. Have your regular ring-free interval of one week and subsequently insert a new ring.
- If your ring has been left in place for more than 4 weeks there is a possibility of becoming pregnant. Contact your doctor before you start with a new ring.
You have missed a menstrual period
- You have followed the instructions for NuvaRing
If you have missed a menstrual period but you followed the instructions for NuvaRing, and have not used other medicines it is very unlikely that you are pregnant. Continue to use NuvaRing as usual. If you miss your menstrual period twice in a row, however, you may be pregnant. Tell your doctor immediately. Do not start the next NuvaRing until your doctor has checked you are not pregnant. - If you have not followed the instructions for NuvaRing
If you have missed a menstrual period and you did not follow the instructions, and you do not have your expected period in the first normal ring-free interval, you may be pregnant. Contact your doctor before you start with a new NuvaRing.
You have unexpected bleeding
While using NuvaRing, some women have unexpected vaginal bleeding between menstrual periods. You may need to use sanitary protection. In any case, leave the ring in the vagina and continue to use the ring as normal. If the irregular bleeding continues becomes heavy or starts again, tell your doctor.
You want to change the first day of your menstrual period
If you follow the instructions for NuvaRing, your menstrual period (withdrawal bleed) will begin in the ring-free interval. If you want to change the day it starts, you can make the ring-free interval shorter (but never longer!). For example, if your ring-free interval begins on a Friday, you can change this to a Tuesday (3 days earlier). Simply insert your next ring 3 days earlier than usual.
If you make your ring-free interval very short (e.g. 3 days or less), you may not have your usual bleeding. You may have spotting (drops or flecks of blood) or breakthrough bleeding while using the next ring.
You want to delay your menstrual period
Delay of your menstrual period (withdrawal bleed) is possible by inserting a new ring immediately after removing the current ring, with no ring-free interval between rings.You can leave the new ring inserted for up to a maximum of 3 weeks. You may experience spotting (drops or flecks of blood) or breakthrough bleeding while using this new ring. When you want your period to begin, just remove the ring. Have your regular ring-free interval of one week and subsequently insert a new ring.
You want to stop using NuvaRing
You can stop using NuvaRing any time you want.
If you do not want to become pregnant, ask your doctor about other methods of birth control.
If you stop using NuvaRing because you want to get pregnant, you should wait until you have had a natural period before trying to conceive. This helps you calculate when the baby will be due.
4. WHEN SHOULD YOU CONTACT YOUR DOCTOR
Regular check-ups
When you are using NuvaRing, your doctor may tell you to return for regular check-ups. In general, you should have a check-up every year
Contact your doctor as soon as possible if:
- You notice any changes in your own health, especially involving any of the items mentioned in this leaflet (see also section 2.1 'When you should not use NuvaRing' and section 2.2 'Warnings and precautions'.
- Your ability to move around is limited for a long period of time or you are to have surgery. Tell your doctor at least four weeks in advance (see also section 2.2 'Blood clots (Thrombosis)').
- You feel a lump in your breast. This symptom may indicate breast cancer (see also section 2.2 'Cancer').
- You experience an allergic reaction, including hives, swelling of the face, lips, tongue, and/or throat causing difficulty in swallowing or potentially breathing (angioedema and/or anaphylaxis) (see also in section 2.2 'Warning and precautions').
- You have severe pain in your abdomen.
- You have unusual, heavy vaginal bleeding. This symptom may indicate cervical cancer.
- You are going to use other medications (see also in section 2.2 'Other medicines and NuvaRing').
- The ring was out of the vagina for longer than 3 hours in the first week of use and you had intercourse in the 7 days before.
- You have forgotten to insert a new ring after the ring-free interval of 7 days.
- You left NuvaRing in place for more than 4 weeks. Do not start the next ring until your doctor tells you.
- You missed your period twice in a row or suspect you are pregnant. Do not start the next ring until your doctor tells you.
- You have an urgent frequent burning, and/or painful urination, and cannot locate the ring in the vagina. These symptoms may indicate accidental placement of NuvaRing into the urinary bladder.
- If you locate the ring in your vagina, but are unable to remove it.
Remove NuvaRing and contact your doctor immediately if you notice possible signs of a blood clot. The symptoms are described in section 2.2 'Blood clots (Thrombosis) '.
5. POSSIBLE SIDE EFFECTS
Like all medicines, NuvaRing can cause side effects, although not everybody gets them.
Serious reactions seen with NuvaRing, as well as the related symptoms, are described in sections 2.2 'Blood clots (Thrombosis) ' and 'Cancer'. Please read these sections for additional information and consult your doctor if you suffer from any of these conditions or symptoms.
Users of NuvaRing have reported the following Common (affecting more than 1 in 100, but less than 1 in 10 women); and Uncommon (affecting more than 1 in 1000, but less than 1 in 100 women) side effects:
- abdominal pain, feeling sick (nausea)
- yeast infection of the vagina (such as 'thrush'); discomfort in the vagina due to the ring; genital itching; secretion from the vagina
- headache or migraine; depressive moods; lower sex drive
- breast pain; painful menstrual periods
- acne
- weight gain
- the ring falling out
- disturbed vision; dizziness
- swollen abdomen; vomiting, diarrhoea or constipation
- feeling tired, unwell or irritable; mood changes
- extra fluid in the body (oedema)
- bladder or urinary tract infection
- difficulty or pain when passing urine; strong desire or need to pass urine; passing urine more often
- problems during intercourse, including pain, bleeding or partner feeling the ring
- increased blood pressure
- increased appetite
- back pain; muscle spasms; pain on legs or arms
- less sensitive skin
- sore or larger breasts; fibrocystic breast disease (cysts in the breasts which may become swollen or painful)
- inflammation of the cervix; cervical polyps (growth in the cervix); rolling outward of the margin of the cervix (ectropion)
- genital secretion; changes to menstrual periods (e.g. periods can be heavy, long, irregular or stop altogether); pelvic discomfort; premenstrual syndrome; spasm of the uterus
- vaginal infection; burning feeling, smell, pain, discomfort or dryness in the vagina or vulva
- hair loss, eczema, itching, rash or hot flushes
- ring breakage.
Rare side effects
(affecting more than 1 in 10 000, but less than 1 in 1000 women)
- blood clot in a vein
- blood clot in an artery.
The following rare side effects have been reported in users of NuvaRing, but the frequency cannot be estimated from the available data: allergic reactions (hypersensitivity), including hives, swelling of the face, lips, tongue, and/or throat causing difficulty in breathing or swallowing (angioedema and/or anaphylaxis); symptoms of angioedema in patients who already have a (family) history of angioedema; vaginal injury associated with ring breakage; breast discharge; and penis discomfort of the partner (such as irritation, rash, itching).
If you get any side effects, talk to your doctor or pharmacist. This includes any side effects not listed in this leaflet.
6. PHARMACEUTICAL PARTICULARS OF NUVARING
Storage Instructions
Store your NuvaRing in the original sachet below 30°C.
Protect from light and freezing.
Do not use a NuvaRing if it was dispensed to you more than 4 months ago. The dispensing date is shown on the carton and sachet.
Do not use NuvaRing after the expiry date which is shown on the carton and sachet.
Do not use NuvaRing if you notice a colour change in the ring or any visible signs of deterioration.
Keep NuvaRing out of the reach and sight of children. If you discover that a child has been exposed to the hormones from NuvaRing, ask your doctor for advice.
What NuvaRing looks like and contents of the pack
NuvaRing is flexible, transparent, colourless to almost colourless and 54 mm wide.
Each ring is packed in a resealable sachet that is made of aluminium foil. The sachet is packed in a cardboard box together with this package leaflet. Each box contains 1 or 3 rings.
IF YOU HAVE ANY FURTHER QUESTIONS, PLEASE CONSULT YOUR DOCTOR OR PHARMACIST.
Sponsors
Organon Pharma Pty Ltd
Building A, 26 Talavera Road,
Macquarie Park NSW 2113
Australia
Date of Preparation
May 2023
AUST R 381186
S-CCPPI-OG8342A-RNG-112021
RCN 100002807-AU
Published by MIMS July 2023


 In studies required or sponsored by regulatory agencies, NuvaRing users had a risk of VTE similar to COC users (see Table 1 for adjusted hazard ratios). A large prospective, observational study, the Transatlantic Active Surveillance on Cardiovascular Safety of NuvaRing (TASC), investigated the risk of VTE for new users, switchers, and restarters of NuvaRing and COCs in a population that is representative of routine clinical users. The women were followed for 24 to 48 months. The results showed a similar risk of VTE among NuvaRing users (VTE incidence 8.3 per 10,000 WY; 95% CI: 5.0-12.9) and women using COCs (VTE incidence 9.2 per 10,000 WY; 95% CI: 6.0-13.5). For women using COCs, excluding desogestrel (DSG), gestodene (GSD) and drospirenone (DRSP), VTE incidence was 8.5 per 10,000 WY (95% CI: 4.5-14.6).
In studies required or sponsored by regulatory agencies, NuvaRing users had a risk of VTE similar to COC users (see Table 1 for adjusted hazard ratios). A large prospective, observational study, the Transatlantic Active Surveillance on Cardiovascular Safety of NuvaRing (TASC), investigated the risk of VTE for new users, switchers, and restarters of NuvaRing and COCs in a population that is representative of routine clinical users. The women were followed for 24 to 48 months. The results showed a similar risk of VTE among NuvaRing users (VTE incidence 8.3 per 10,000 WY; 95% CI: 5.0-12.9) and women using COCs (VTE incidence 9.2 per 10,000 WY; 95% CI: 6.0-13.5). For women using COCs, excluding desogestrel (DSG), gestodene (GSD) and drospirenone (DRSP), VTE incidence was 8.5 per 10,000 WY (95% CI: 4.5-14.6). Extremely rarely, thrombosis has been reported to occur in other blood vessels, e.g. hepatic, mesenteric, renal, cerebral or retinal veins and arteries, in CHC users.
Extremely rarely, thrombosis has been reported to occur in other blood vessels, e.g. hepatic, mesenteric, renal, cerebral or retinal veins and arteries, in CHC users.


 Chemical name: 19-nor-17α-pregna-1,3,5,(10)- trien-20-yne-3,17-diol.
Chemical name: 19-nor-17α-pregna-1,3,5,(10)- trien-20-yne-3,17-diol. Chemical name: (17α)-13-ethyl-17- hydroxy-11-methylene-18,19 dinorpregn-4-en-20-yn-3-one.
Chemical name: (17α)-13-ethyl-17- hydroxy-11-methylene-18,19 dinorpregn-4-en-20-yn-3-one.