What is this leaflet?
This leaflet answers some of the common questions people ask about PENTHROX® (methoxyflurane). It does not contain all the information known about PENTHROX®.
It does not take the place of talking to your healthcare professional (i.e., doctor, dentist, pharmacist, nurse, etc.).
All medicines have risks and benefits. Your healthcare professional has weighed the risks of you being given PENTHROX® against the benefits they expect it will have for you.
If you have any concerns about being given this medicine, ask your healthcare professional.
Keep this leaflet in a safe place. You may need to read it again.
What PENTHROX® is used for
PENTHROX® is a medicine which is used to reduce pain.
It is inhaled through the PENTHROX® INHALER.
Pain relief should start after 6-10 breaths. PENTHROX® is intended to reduce the severity of pain, rather than completely eliminate it.
PENTHROX® belongs to a family of medicines called inhalation anaesthetics. At the recommended dose, PENTHROX® provides pain relief without producing anaesthesia.
Ask your healthcare professional if you have any questions about why PENTHROX® has been prescribed for you.
Before you are given PENTHROX®
When you must not be given it
You must not be given PENTHROX® if you have an allergy to methoxyflurane, other inhalation anaesthetics or any of the ingredients listed at the end of this leaflet.
Symptoms of an allergic reaction may include:
- Shortness of breath, wheezing or difficultly to breathe
- Swelling of the face, lips, tongue or other parts of the body
- Rash, itching or hives on the skin
You must not be given PENTHROX® if you have, or are suspected of having, an inherited tendency for a condition called malignant hyperthermia. This is a condition where, when you or a related family member has been given an anaesthetic, symptoms such as a very high fever, fast, irregular heartbeat, muscle spasms and breathing problems have occurred.
You must not be given PENTHROX® if you have heart disease, kidney disease or reduced function of your kidneys, difficulty breathing or head injury.
If you are not sure whether you should be given PENTHROX®, talk to your healthcare professional.
Before you are given it
PENTHROX® should only be used if the package is undamaged and the expiry date marked on the bottle has not passed.
Tell your healthcare professional if you have allergies to:
- Any other medicines
- Any other substances such as foods, preservatives or dyes
- Any ingredients listed at the end of this information leaflet
Tell your healthcare professional if you are pregnant or intending to become pregnant. Your healthcare professional will discuss the possible risks and benefits of being given PENTHROX® during pregnancy.
Tell your healthcare professional if you are breast-feeding or intending to breast-feed. Your healthcare professional will discuss the possible risks and benefits of being given PENTHROX® during breast-feeding.
Tell your healthcare professional if you have, or have had, any medical conditions, especially the following:
- Kidney problems
- Liver problems
Tell your healthcare professional immediately if you experience any breathing problems.
Respiratory depression, with symptoms such as too slow and shallow breathing or other difficulties in breathing, has been reported in association with treatment with PENTHROX®.
If you have not told your healthcare professional about any of the above, tell them before you are given PENTHROX®. You may still be able to use PENTHROX®, but your healthcare professional will need to assess the risks against the potential benefits.
Taking other medicines
Tell your healthcare professional if you are taking any other medicines, including medicines that you buy without a prescription at the chemist, supermarket or health food shop.
Some medicines and PENTHROX® may interfere with each other. Your healthcare professional needs to know if you are taking any of these medicines to accurately assess the risks and benefits of administering PENTHROX®. These include:
- Isoniazid to treat tuberculosis
- Barbiturates, such as phenobarbital to treat epilepsy
- Rifampicin to treat infection
- Medicines, or illegal drugs, that have a dampening effect on the nervous system such as narcotics.
- Antibiotics or other medicines that may harm the kidney such as tetracycline, gentamicin, kanamycin, colistin, polymyxin B, cephaloridine or, amphotericin B
- Intravenous adrenaline
- β-blockers to treat hypertension
Your doctor may have more information on medicines to be careful with around the time you receive PENTHROX®.
How PENTHROX® is given
How much is given
One bottle of PENTHROX® (3 mL) to be used initially. Additional bottle(s) may be used if required. The maximum recommended dosage is 6 mL of PENTHROX® per day and 15 mL per week. PENTHROX® should not be used on consecutive days. You should not inhale more than the maximum dose because PENTHROX® may damage your kidneys.
How the PENTHROX® Inhaler is given
- Your healthcare professional will prepare the PENTHROX® Inhaler (with or without the optional Activated Carbon (AC) Chamber), and place wrist loop over your wrist.
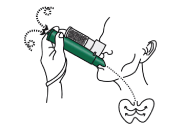
- Breathe in through the mouthpiece of the PENTHROX® Inhaler to obtain pain relief. Your healthcare professional will show you how if you are unsure. Accustom yourself to the fruity smell of the medicine by inhaling gently for the first few breaths. You must breathe out through the PENTHROX® Inhaler when the AC Chamber is attached for the AC Chamber to adsorb any exhaled methoxyflurane. After the first few breaths, breathe normally through the PENTHROX® Inhaler. Pain relief should commence after approximately 6-10 consecutive breaths.
After the initial 6-10 breaths, you can inhale PENTHROX® continuously or intermittently as instructed by your healthcare professional. For intermittent dosing, a top-up of 6 breaths may be given before each of the more painful parts of a procedure.
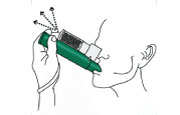
- If you need stronger pain relief, cover the dilutor hole on the PENTHROX® Inhaler or on the AC Chamber with your finger during use. Your healthcare professional will show you where the dilutor hole is.
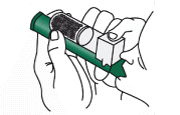
- You do not need to breathe in through the PENTHROX® Inhaler all of the time. Your healthcare professional will encourage you to take breaks from the PENTHROX® Inhaler as this will increase the duration of use.
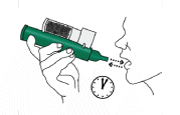
How long is it given for
Continue using your medicine until your healthcare professional tells you to stop or when you have inhaled the maximum recommended dose.
One 3 mL bottle of PENTHROX® provides approximately 20-25 minutes of pain relief when inhaled continuously. A second 3 mL bottle of PENTHROX® can be given to extend the period of pain relief to approximately 50-55 minutes when inhaled continuously. Intermittent inhalation will increase the time of analgesia.
How is it given
PENTHROX® is poured into the base of the PENTHROX® Inhaler by the healthcare professional and is absorbed into the wick. You will inhale PENTHROX® either directly from the PENTHROX® Inhaler.
Overdose
The healthcare professional giving you PENTHROX® will be experienced in its use, so it is extremely unlikely that you will be given too much. The dose of PENTHROX® is limited by the amount contained in each bottle.
You should not use more than 6 mL in one day and not more than 15 mL in one week. Administration of consecutive days is not recommended. If the maximum dose is exceeded PENTHROX® may cause irreversible damage to your kidneys.
Immediately contact your healthcare professional or the Poisons Information Centre (telephone 13 11 26) for advice, or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have been given too much PENTHROX®. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
While you are being given PENTHROX®
Things you must do
You should breathe in through the mouthpiece, initially ensuring that the “dilutor” hole of the PENTHROX® Inhaler is not covered.
Accustom yourself to the characteristic fruity smell of the PENTHROX® by inhaling gently for the first few breaths through the PENTHROX® Inhaler. You must breathe out through the PENTHROX® Inhaler, if an AC Chamber is attached.
If further relief is required you may cover the “dilutor” hole with your finger for a higher inhaled concentration of PENTHROX®.
Use PENTHROX® intermittently as required to provide pain relief.
Things you must not do
Do not give PENTHROX® to anyone else, even if they have the same condition as you.
Do not drive or operate machinery until you know how PENTHROX® affects you.
PENTHROX® may cause drowsiness or dizziness in some people and therefore may affect alertness.
Make sure you know how you react to PENTHROX® before you drive a car, operate machinery, or do anything else that could be dangerous if you are drowsy, dizzy or not alert.
Things that may be helpful
You are in control of the level of your pain relief by directly inhaling PENTHROX® from the PENTHROX® Inhaler.
The aim of PENTHROX® is to relieve pain until you feel comfortable. Relief will commence after approximately 6-10 breaths. Relief will continue for several minutes after ceasing use of PENTHROX®.
Side Effects
Tell your healthcare professional as soon as possible if you do not feel well after you have been given PENTHROX®.
PENTHROX® is well tolerated, but it may occasionally have unwanted side effects. All medicines can have side effects. Sometimes they are serious, but most of the time they are not. You may need medical treatment if you have some of the side effects.
Ask your healthcare professional to answer any questions you may have.
Other side effects not listed below may occur in some patients.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
If you are taking PENTHROX® for Trauma and associated pain
Tell your healthcare professional if you notice any of the following side effects and they worry you.
PENTHROX® may cause:
- Feeling sick or nauseous
- Dry mouth
- Coughing (usually in the first few breaths)
- Vomiting
- Dizziness
- Loss of memory
- Headache
- Migraine
- Drowsiness
- Low blood pressure
- Feeling drunk
- Toothache
- Flu-like symptoms, such as high temperature, sore throat, runny nose, cough and chills
- Viral infection
- Nose and throat inflammation
- Fall
- Joint sprain
- Increase in blood enzyme levels, including alanine aminotransferase, aspartate aminotransferase and blood lactate dehydrogenase
- Painful menstrual periods
- Pain in the mouth and throat
- Rash
- Back pain
- Difficulty in speaking
If you require PENTHROX® for surgical procedures
Tell your healthcare professional if you notice any of the following side effects and they worry you.
PENTHROX® may cause:
- Dizziness
- Feeling of extreme happiness
- Feeling sick or nauseous
- Sweating
- Taste disturbance or loss of taste
- Flushing
- High blood pressure
- Feeling anxious
- Depression
- Numbness or weakness of the arms and legs
- Drowsiness
- Vomiting
- Confusion
These lists include the more common side effects of PENTHROX®. They are usually mild and only last a short time.
Contact your doctor immediately if:
- You experience any symptoms of liver problems, such as loss of appetite, nausea, vomiting, jaundice (yellowing of the skin and/or eyes), dark coloured urine, pale coloured stools, pain/ache or sensitivity to touch in your right abdominal area (below your ribs)
- You experience any symptoms of kidney problems such as reduced or excessive urination or swelling of feet or lower legs.
- You experience too slow and shallow breathing or other difficulties in breathing (symptoms of respiratory depression)
Tell your healthcare professional if you notice anything else that is making you feel unwell.
Other sides effects not listed above may also occur in some people. Some of these side effects (for examples changes to blood enzyme levels) can only be found when your doctor does tests from time to time to check your progress.
After being given PENTHROX® (methoxyflurane)
Storage
PENTHROX® should be carefully stored below 30°C in its original container.
Disposal
Your healthcare professional will dispose of any excess PENTHROX® liquid and the PENTHROX® INHALER in the appropriate way.
Product Description
What it looks like
PENTHROX® is a clear, almost colourless liquid with a characteristic fruity smell that becomes a vapour or gas when it is used with the PENTHROX® INHALER.
PENTHROX® (methoxyflurane) is supplied in the following presentations:
a) Pack of ten 3 mL bottles,
b) Combination Pack containing one 3 mL bottle, one PENTHROX® Inhaler and Activated Carbon (AC) Chamber,
c) Combination Pack (Starter Pack) containing one 3 mL bottle, one PENTHROX® Inhaler and Activated Carbon (AC) Chamber,
d) Single Combination Pack containing ten 3 mL bottles and ten PENTHROX® Inhalers
e) Double Combination Pack containing two 3 mL bottles, one PENTHROX® Inhaler and Activated Carbon (AC) Chamber (Pack of ten)
f) Combination Pack containing one 1.5 mL bottle, one PENTHROX® Inhaler and Activated Carbon (AC) Chamber.
g) Single Combination Pack containing ten 1.5 mL bottles and ten PENTHROX® Inhalers
Not all packs may be marketed
Ingredients
Active Ingredient:
- Methoxyflurane 99.9%
There is a small amount (approximately 0.01% Butylated Hydroxy Toluene) of stabilising agent in PENTHROX®.
Manufacturer and Sponsor
Medical Developments International Limited
4 Caribbean Drive
Scoresby VIC 3179 Australia
Australia
Tel: +61 3 9547 1888
This leaflet was revised in October 2023
Australian Registration Number:
AUST R 43144
Published by MIMS November 2023

 In listings below, are adverse reactions (adverse effects that are related to the treatment) which occurred at a rate lower than in Table 1. They are listed by system organ class and frequency (common ≥ 1/100 to < 1/10; uncommon ≥ 1/1,000 to < 1/100; and rare ≥ 1/10,000 to < 1/1,000).
In listings below, are adverse reactions (adverse effects that are related to the treatment) which occurred at a rate lower than in Table 1. They are listed by system organ class and frequency (common ≥ 1/100 to < 1/10; uncommon ≥ 1/1,000 to < 1/100; and rare ≥ 1/10,000 to < 1/1,000).
 Methoxyflurane is stable and does not decompose in contact with soda lime. An antioxidant, butylated hydroxytoluene (0.01% w/w) is added to ensure stability on standing. As polyvinyl chloride plastics are extracted by methoxyflurane, contact should be avoided. Methoxyflurane does not extract polyethylene plastics, polypropylene plastics, fluorinated hydrocarbon plastics or nylon.
Methoxyflurane is stable and does not decompose in contact with soda lime. An antioxidant, butylated hydroxytoluene (0.01% w/w) is added to ensure stability on standing. As polyvinyl chloride plastics are extracted by methoxyflurane, contact should be avoided. Methoxyflurane does not extract polyethylene plastics, polypropylene plastics, fluorinated hydrocarbon plastics or nylon.