WHAT IS IN THIS LEAFLET
This leaflet answers some of the common questions about Progynova tablets. It does not contain all of the available information. It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks of you taking Progynova against the benefits they expect it will provide.
If you have any concerns about taking Progynova, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
WHAT PROGYNOVA IS USED FOR
Progynova provides hormone replacement therapy (HRT) for the treatment of menopausal complaints after the cessation of monthly bleeding, after surgical removal of the ovaries (oophorectomy) or due to radiotherapy. Progynova is only intended for short term use.
Progynova contains estradiol valerate, a precursor of the hormone estradiol. During menopause, the estradiol production of the ovaries declines. Although menopause is natural, it often causes distressing symptoms, which are connected with the gradual loss of the hormones produced by the ovaries.
Progynova replaces the hormone estradiol that the body no longer makes and prevents or relieves symptoms such as hot flushes, sweats, sleep disturbances, depressive moods, irritability, dizziness, headaches as well as vaginal dryness and burning.
If you have not had your uterus removed (hysterectomy) your doctor will prescribe another hormone progestogen to take with Progynova.
Progynova is not a contraceptive. It will not prevent you from falling pregnant.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another reason.
BEFORE YOU TAKE PROGYNOVA
When you must not take it
Do not take Progynova if you have an allergy to:
- estradiol valerate, the active ingredient in Progynova
- any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
Do not take Progynova if you have:
- undiagnosed vaginal bleeding
- breast cancer or a suspicion of breast cancer
- other tumours (including liver tumours) or a suspicion of other tumours
- severe liver disease including jaundice (yellowing of the skin and/or eyes)
- had a heart attack and/or stroke
- a history of or are at a high risk of a blood clot in the blood vessels of the legs (deep venous thrombosis) or the lungs (pulmonary embolism)
- high levels of fat in the blood (triglycerides)
- hearing loss caused by an abnormal bone growth in the ear (otosclerosis), which worsens during pregnancy
- severe diabetes
Do not take this medicine if you are pregnant. It may affect your developing baby if you take it during pregnancy.
Do not breast-feed if you are taking this medicine. The active ingredient in Progynova passes into breast milk and there is a possibility that your baby may be affected.
Do not take this medicine if you are under 18 years old.
Do not take this medicine after the expiry date printed on the pack and blister. The expiry date is printed on the carton and on each blister after “EXP” (e.g. 11 18 refers to November 2018). The expiry date refers to the last day of that month. If it has expired return it to your pharmacist for disposal.
Do not take this medicine if the packaging is torn or shows signs of tampering. If the packaging is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking this medicine, talk to your doctor.
Before you start to take it
Tell your doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if:
- you smoke
- you are overweight
- you or anyone in your immediate family has had blood clots (thrombosis)
- you have any hospitalisation, surgery or prolonged immobilisation
You have an increased risk of a blood clot if you have any of the above risk factors. In addition to these, there may be other risk factors. Talk to your doctor if you have any concerns.
Taking Progynova may also increase your risk of coronary heart disease. Tell your doctor if you experience chest pain or discomfort.
Taking Progynova may increase your risk of gall bladder disease. This is because estrogen stimulates the liver to remove more cholesterol from blood and divert it to the gall bladder.
Before starting Progynova, your doctor should conduct a thorough medical and gynaecological examination (including the breasts). Your doctor should conduct this examination periodically. If you have liver disease, your doctor will also conduct liver function tests from time to time. Your doctor will also note your family medical history and exclude pregnancy.
Tell your doctor if you have or have had any of the following:
- high blood pressure
- liver disease including jaundice (yellowing of the skin and/or eyes)
- thyroid disease and you are taking medication for it
- heart or kidney disease
- low calcium levels in the blood
- endometriosis (the presence of tissue of the lining of the womb in places in the body where it is not normally found)
- asthma
- diabetes
- epilepsy
- migraine
- porphyria (an inherited disease where the body cannot convert naturally occurring compounds into haem, which contains iron)
- systemic lupus erythematosus (SLE; a chronic inflammatory disease)
- an abnormal build-up of blood vessels in the liver (hepatic haemangioma)
- tumours in your womb or pituitary gland
- chloasma (yellow brown patches on the skin); if so, avoid too much exposure to the sun or ultraviolet radiation
- lumpy or painful breasts (benign breast disease)
- chorea minor (involuntary movement disorder)
- hereditary angioedema (repeated episodes of severe swelling)
Tell your doctor if you are 65 years or older when HRT is initiated. The reason is that there is limited evidence from clinical studies that hormonal treatment may increase the risk of significant loss of intellectual abilities such as memory capacity (dementia).
If HRT is used in the presence of any of the conditions listed above you will need to be kept under close observation. Your doctor can explain this to you. Therefore, if any of these apply to you, tell your doctor before starting to take Progynova.
HRT and cancer
Endometrial cancer
The risk of cancer of the lining of the womb (endometrial cancer) increases when estrogens are used alone for prolonged periods. Taking a progestogen in addition to the estrogen lowers the increased risk.
Please inform your doctor if you frequently have bleeding irregularities or persistent bleeding during the treatment with Progynova.
Breast cancer
Please inform your doctor if you have suffered from fibrocystic disease of the breasts (lumpy or painful breasts) or if you have first degree relatives (mother, sisters, daughters) who have had breast cancer.
Breast cancer has been diagnosed slightly more often in women who have used hormone replacement therapy (HRT) than in women of the same age who have never used HRT. The risk increases with duration of treatment. If you are concerned about this information you should discuss this with your doctor. It is recommended that yearly breast examinations are conducted and regular self-examination (monthly) should be carried out. HRT has been reported to result in an increased number of abnormal mammograms requiring further evaluation.
HRT increases the density of mammographic images. This may complicate the mammographic detection of breast cancer in some cases. Therefore your doctor may choose to use other breast cancer screening techniques as well.
Ovarian cancer
Some observational studies show a slightly increased overall risk of developing ovarian cancer in women who have used HRT compared to women who have never used HRT. In women currently using HRT, this risk was further increased. These associations have not been shown in all studies. There is no consistent evidence that the risk of developing ovarian cancer is related to the duration of use of HRT. However, the risk may be more relevant with long-term use (for several years).
Liver tumour
During or after the use of hormones such as those that are contained in Progynova, benign liver tumours have rarely occurred, and malignant liver tumours even more rarely. In isolated cases, bleeding has occurred from such tumours into the abdominal cavity. Although such events are rare, you should inform your doctor about any pain in your upper abdomen that does not disappear within a short time.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and Progynova may interfere with each other. These include:
- medicines to treat high blood pressure, chest pain and/or irregular heart beat such as ACE inhibitors, verapamil, diltiazem
- medicines used to treat epilepsy such as hydantoins, barbiturates, primidone, carbamazepine, oxcarbazepine, topiramate, felbamate
- rifampicin for the treatment of tuberculosis
- macrolide antibiotics (e.g. clarithromycin, erythromycin)
- herbal medicines containing St John’s Wort
- medicines used to treat HIV such as ritonavir or nevirapine
- some medicines used to treat Hepatitis C Virus (HCV) such as boceprevir, telaprevir
- medicines used to treat fungal infections such as ketoconazole, itraconazole, voriconazole, fluconazole
- grapefruit juice
- medicines used to treat pain and fever (e.g. paracetamol)
- medicines used to treat diabetes, such as insulin or other anti-diabetic medications
These medicines may be affected by Progynova or may affect how well it works. You may need different amounts of your medicines, or you may need to take different medicines.
If you are diabetic, your doctor may alter the dose of the diabetes medication.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while taking this medicine.
HOW TO TAKE PROGYNOVA
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
If you do not understand the instructions printed on the pharmacist label, ask your doctor or pharmacist for help.
How to take it
Take one tablet at the same time each day.
Taking it at the same time each day will have the best effect. It will also help you remember when to take it. It does not matter if you take this medicine before or after food.
When you have finished each blister foil start the next one on the following day. Never leave a break between blister foils unless your doctor has advised you to. Tablet taking should be continuous.
Swallow the tablets whole with a glass of water.
How long to take it
Progynova is only intended for short term use. Your doctor will advise you on how long to use Progynova. Your doctor will discuss the risks of long term treatment with HRT with you. Some recent studies have shown that women using HRT have a small increase in breast cancer risk. The risk increases with the length of HRT use.
HRT is associated with a small increase in the risk of developing breast cancer, heart attacks, strokes, blood clots, including clots in the lungs, and dementia. However, the evidence is inconclusive. On the other hand the risk of hip fractures and bowel cancer may be reduced. Your doctor can discuss these risks and benefits with you, taking into account your particular circumstances.
If you forget to take it
If you are less than 24 hours late take your tablet as soon as possible, and take the next one at the normal time. If you miss tablets for several days, irregular bleeding may occur.
If you take too much (overdose)
Immediately telephone your doctor or the Poisons Information Centre on 13 11 26 for advice, or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have taken too much Progynova.
Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
WHILE YOU ARE TAKING PROGYNOVA
Things you must do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking Progynova.
Tell any other doctors, dentists, and pharmacists who treat you that you are taking this medicine.
If you become pregnant while taking this medicine, tell your doctor immediately.
If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine. It may affect other medicines used during surgery.
The use of HRT may affect the results of certain laboratory tests. If you are about to have any blood tests, tell your doctor that you are taking this medicine. It may interfere with the results of some tests.
Stop taking it immediately if
You should stop treatment at once and consult your doctor if you have any of the following conditions:
- your very first attack of migraine (typically a throbbing headache and nausea preceded by visual disturbances)
- worsening of pre-existing migraine, any unusually frequent or unusually severe headaches
- sudden disturbances of vision or hearing
- swollen veins (phlebitis)
- itching of the whole body
- unusual upper abdominal pain that do not disappear within a short period of time.
If you get a blood clot while you are taking Progynova or there is a suspicion of this you should stop taking it immediately and contact your doctor. Warning signs to look out for are:
- coughing blood
- unusual pains or swelling of your arms or legs
- sudden shortness of breath
- fainting.
Progynova must also be stopped at once if you develop jaundice (yellowing of the skin and/or eyes). Tell your doctor immediately if either occurs.
Things you must not do
Do not take Progynova to treat any other complaints unless your doctor tells you to.
Do not give your medicine to anyone else, even if they have the same condition as you.
Do not stop taking your medicine without checking with your doctor. If you stop taking it suddenly, your condition may worsen or you may have unwanted side effects.
What to be careful of
Excess intake of alcohol during use of HRT has an influence on the treatment. Your doctor will advise you.
SIDE EFFECTS
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking Progynova.
All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
During the first few months of treatment you may experience some breast tenderness or enlargement. These symptoms are usually temporary and normally disappear with continued treatment. If they do not, contact your doctor.
The following symptoms have been reported in users of various oral HRT preparations:
- signs of allergy such as rash, swelling of the face, lips, mouth, throat or other parts of the body, shortness of breath, wheezing or trouble breathing
- changes in body weight
- feeling depressed and/or anxious
- changes in sexual drive
- visual disturbances such as partial or complete loss of vision, bulging eyes, double vision
- intolerance to contact lenses
- irregular heartbeat
- muscle cramps
- changes in vaginal bleeding pattern including spotting
- painful menstrual periods
- vaginal secretion
- premenstrual-like syndrome such as mood swings, bloating, breast swelling and tenderness
- breast pain
- indigestion
- nausea
- vomiting
- stomach pain
- increased appetite
- rash
- various skin disorders such as itching, hives, acne, excessive hairiness, hair loss or red, painful lumps
- headache
- migraine
- dizziness
- swelling of the hands, ankles or feet
- feeling tired
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Other side effects not listed above may also occur in some people.
Also tell your doctor if you have any of the symptoms listed under “While you are taking Progynova - stop taking it immediately”.
AFTER TAKING PROGYNOVA
Storage
Keep your tablets in the pack until it is time to take them. If you take the tablets out of the pack they may not keep well.
Keep your tablets in a cool dry place. Store your tablets as per directions on the carton.
Do not store it or any other medicine in the bathroom, near a sink, or on a window-sill.
Do not leave it in the car.
Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop taking this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Return any unused medicine to your pharmacist.
PRODUCT DESCRIPTION
What it looks like
Progynova (1 mg) are small round beige sugar coated tablets packaged in calendar blister strips containing 28 tablets.
Progynova (2 mg) are small round white sugar coated tablets packaged in calendar blister strips containing 28 tablets.
Each pack contains 2 blister strips.
Ingredients
Active ingredients per tablet:
- Progynova 1 – 1 mg estradiol valerate
- Progynova 2 – 2 mg estradiol valerate
Inactive ingredients per 1 mg tablet:
- lactose
- maize starch
- povidone
- purified talc
- magnesium stearate
- sucrose
- macrogol 6000
- calcium carbonate
- glycerol
- glycol montanate
- titanium dioxide
- iron oxide yellow
Inactive ingredients per 2 mg tablet:
- lactose
- maize starch
- povidone
- purified talc
- magnesium stearate
- sucrose
- macrogol 6000
- calcium carbonate
- glycol montanate
Suppliers
Bayer Australia Ltd
ABN 22 000 138 714
875 Pacific Highway
Pymble NSW 2073
Australian Registration Numbers
Progynova (1mg) - AUST R 10708
Progynova (2mg) - AUST R 323720
Date of preparation
December 2019
See TGA website (www.ebs.tga.gov.au) for latest Australian Consumer Medicine Information.
® Registered trademark of the Bayer group, Germany.
© Bayer Australia Ltd
All rights reserved.

Published by MIMS May 2021


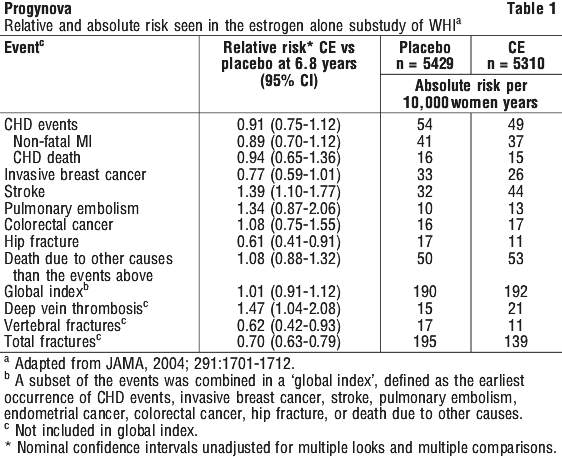 For those outcomes included in the WHI global index that reached statistical significance, the absolute excess risk per 10,000 women-years in the group treated with CE alone were 12 more strokes while the absolute risk reduction per 10,000 women-years was 6 fewer hip fractures. The absolute excess risk of events included in the global index was a nonsignificant 2 events per 10,000 women-years. There was no difference between the groups in terms of all cause mortality (see Section 4.4 Special Warnings and Precautions for Use).
For those outcomes included in the WHI global index that reached statistical significance, the absolute excess risk per 10,000 women-years in the group treated with CE alone were 12 more strokes while the absolute risk reduction per 10,000 women-years was 6 fewer hip fractures. The absolute excess risk of events included in the global index was a nonsignificant 2 events per 10,000 women-years. There was no difference between the groups in terms of all cause mortality (see Section 4.4 Special Warnings and Precautions for Use). For those outcomes included in the WHI global index, the absolute excess risks per 10,000 women-years in the group treated with CE/MPA were 7 more CHD events, 8 more strokes, 8 more PEs and 8 more invasive breast cancers, while the absolute risk reductions per 10,000 women-years were 6 fewer colorectal cancers and 5 fewer hip fractures. The absolute excess risk of events included in the global index was 19 per 10,000 women-years. There was no difference between the groups in terms of all cause mortality (see Section 4.4 Special Warnings and Precautions for Use).
For those outcomes included in the WHI global index, the absolute excess risks per 10,000 women-years in the group treated with CE/MPA were 7 more CHD events, 8 more strokes, 8 more PEs and 8 more invasive breast cancers, while the absolute risk reductions per 10,000 women-years were 6 fewer colorectal cancers and 5 fewer hip fractures. The absolute excess risk of events included in the global index was 19 per 10,000 women-years. There was no difference between the groups in terms of all cause mortality (see Section 4.4 Special Warnings and Precautions for Use). Chemical name: 1,3,5(10)-estratriene-3,17β-diol-17-valerate.
Chemical name: 1,3,5(10)-estratriene-3,17β-diol-17-valerate.