1 Name of Medicine
Sodium fluoride.
2 Qualitative and Quantitative Composition
Radpharm LLK Kit consists of sterile, pyrogen free ingredients which need reconstitution with sodium pertechnetate [99mTc] injection and mixing to produce technetium [99mTc] stannous colloid complex suitable for labelling white blood cells in whole blood.
Each Vial A (solution) and Vial B (lyophilised) contains the following active ingredient and excipient:
Vial A.
6 mL solution of 1 mg/mL sodium fluoride (active ingredient) in Water for Injections BP (excipient).
Vial B.
0.64 mg of stannous fluoride (excipient) as a lyophilised powder.
The product contains no preservatives.3 Pharmaceutical Form
Radpharm LLK is a composite kit consists of:
Vial A.
Clear concentrated liquid for Intravenous Injection in 10 mL vials.
Vial B.
Dry white lyophilised powder in multidose 8 mL vacuum sealed vials for intravenous injection.4.1 Therapeutic Indications
Technetium [99mTc] labelled leucocytes may be used to image acute inflammation or infection.
4.2 Dose and Method of Administration
Recommended intravenous dose for the normal adult is 400 to 600 MBq.
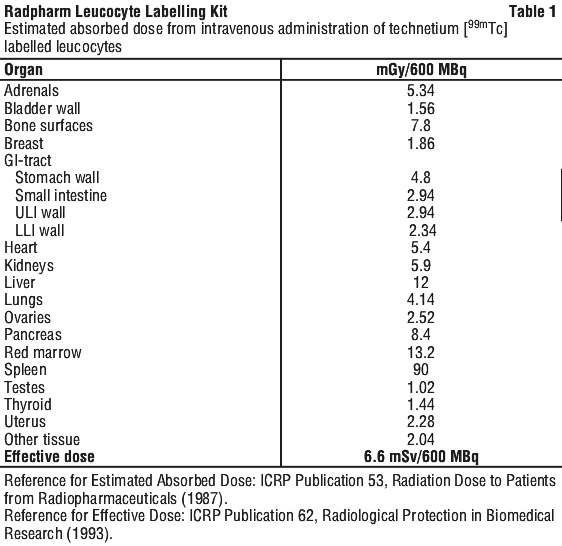
Radiation dosimetry.
See Table 1.
Heparin preparation.
Aseptically transfer 5 mL of heparin sodium (1000 units/mL) to 45 mL sodium chloride injection and mix. Final heparin sodium concentration is 100 units/mL.
Procedure.
Colloid preparation. Note.
If there is no vacuum in Vial B, discard and replace before delivering 5 mL from Vial A.
1. Draw 1.5 to 2 GBq sodium pertechnetate [99mTc] injection eluted from a technetium-99m generator into a 5 mL syringe and then draw sodium chloride injection to make a volume of 2.5 mL.
2. Draw 5 mL from Vial A into a syringe and transfer to Vial B. Mix for 20 seconds to dissolve.
3. Aseptically withdraw 1 to 2 mL of this solution into a 2.5 mL syringe and then transfer 0.5 mL via a 0.22 micrometer membrane filter into the syringe containing 2.5 mL sodium pertechnetate [99mTc] injection (step 1 Colloid preparation).
Note.
Filter has void volume of 0.5 mL.
4. Mix by slow rotation for 1 hour to produce ideal technetium [99mTc] stannous colloid integrity and size.
5. Use within 1 hour after mixing.
Summary.
1.5 to 2 GBq sodium pertechnetate [99mTc] injection to 2.5 mL with sodium chloride injection.
5 mL from Vial A ----> Vial B.
Mix to reconstitute for 20 seconds.
0.5 mL from Vial B (via 0.22 micrometer filter) ------> 2.5 mL sodium pertechnetate [99mTc] injection.
Mix by rotation for 1 hour.
After mixing use within 1 hour.
Leucocyte labelling procedure. 1. Draw 20 mL blood into syringe containing 100 units of heparin sodium.
2. Transfer 1.5 mL technetium [99mTc] stannous colloid (Step 4 Colloid Preparation) to 20 mL blood. Mix by rotation for 1 hour.
3. Transfer to sterile 50 mL centrifuge tube.
4. Centrifuge at 400 g (approx. 2000 rpm) for 5 minutes.
Note.
The buffy coat between plasma and red blood cells must be observed.
5. Remove plasma to 1 cm of buffy coat making sure not to disturb cells.
6. Add sufficient sodium chloride injection to replace plasma, mix by inversion and reinject blood.4.3 Contraindications
None known.
4.4 Special Warnings and Precautions for Use
Clinical.
As there is significant liver/spleen uptake of technetium [99mTc] labelled leucocytes and residual technetium [99mTc] stannous colloid, determination of sites causing fever of unknown origin is not recommended.
General.
Radiopharmaceuticals should only be used by physicians who are qualified by specific training in the safe use and handling of radionuclides.
The contents of the Vial A and B are intended only for use in the preparation of technetium [99mTc] labelled leucocytes.
The radioactivity of the dose should be checked with a suitable instrument immediately prior to administration.
Use in the elderly.
No data available.
Paediatric use.
No data available.
Effects on laboratory tests.
No data available.4.5 Interactions with Other Medicines and Other Forms of Interactions
None known.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
No data available.
(Category C)
Technetium-99m radiopharmaceuticals should only be given to a pregnant woman if in the judgement of the treating physician the expected benefits outweigh the potential hazards.
Technetium-99m is excreted in human milk. It is recommended that interruption to breast feeding is necessary after the administration of technetium [99mTc] labelled leucocytes for a period of not less than 12 hours and contact with the baby should be restricted to 5 hours in 24 hours.4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
For each patient, exposure to ionising radiation must be justifiable on the basis of likely benefit. The activity administered must be such that the resulting dose is as low as reasonably achievable bearing in mind the need to obtain the intended diagnostic or therapeutic result.
Exposure to ionising radiation is linked with cancer induction and a potential for development of hereditary defects. For diagnostic nuclear medicine investigations the current evidence suggests that these adverse effects will occur with low frequency because of the low radiation doses incurred.
For most diagnostic investigations using a nuclear medicine procedure the radiation dose delivered (EDE) is less than 20 mSv. Higher doses may be justified in some clinical circumstances.
Hypersensitivity reactions have been reported with technetium [99mTc] preparations.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.4.9 Overdose
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.2 Pharmacokinetic Properties
Technetium [99mTc] labelled leucocytes radiolabels neutrophils and monocytes by phagocytic engulfment of the radiocolloid. The radiocolloid is administered to autologous whole blood, rotated and incubated at room temperature for 1 hour, with a resultant mean labelling efficiency of 85.2% (neutrophils 62.6% and monocytes 22.6%).
5.3 Preclinical Safety Data
Genotoxicity.
No data available.
Carcinogenicity.
No data available.6 Pharmaceutical Particulars
6.1 List of Excipients
See Section 2 Qualitative and Quantitative Composition.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life of the Radpharm LLK composite kit can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the vial and carton packaging.
After slow rotation for 1 hour (step 4 in Colloid preparation) the technetium [99mTc] stannous colloid is stable at room temperature for 1 hour.
6.4 Special Precautions for Storage
Vial A and Vial B must be stored at 2°C to 8°C (Refrigerate. Do not freeze).
6.5 Nature and Contents of Container
Radpharm LLK composite kit is supplied in Vial A and Vial B.
a) Vial A is supplied as a carton of 5 sterile, pyrogen free 10 mL vials glass Type 1 clear vials with grey chlorobutyl non-lyophilisation stopper and aluminium seal with dark grey flip off.
b) Vial B is supplied as a carton of 5 sterile, pyrogen free, vacuum sealed 8 mL Type 1 coloured glass vials with 1888 grey chlorobutyl lyophilisation stopper and aluminium seal with light grey flip off.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or radioactive waste material should be disposed off in accordance with Code for the disposal of radioactive wastes by the user which is published on the Australian Radiation Protection and Nuclear Safety Agency (ARPANSA) website as Radiation Protection Series (RPS C-6).
6.7 Physicochemical Properties
Chemical structure.
 Chemical Formula: FNa.
Chemical Formula: FNa.
CAS number.
7681-49-4.7 Medicine Schedule (Poisons Standard)
Unscheduled.
Summary Table of Changes




 Chemical Formula: FNa.
Chemical Formula: FNa.