What is in this leaflet
This leaflet answers some of the common questions people ask about SEROQUEL XR. It does not contain all the available information.
It does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor will have weighed the risks of you taking it against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What SEROQUEL XR is used for
SEROQUEL XR helps to correct chemical imbalances in the brain. It is used to treat conditions such as:
- Bipolar disorder, an illness of in which there are sustained mood swings either up (mania) or down (depression). During mania, patients experience episodes of overactivity, elation or irritability. During depression, patients may feel depressed or guilty, lack energy, lose their appetite and have trouble sleeping.
- Recurrent major depressive disorder, an illness where depression is longer lasting and/ or more severe than the "low moods" everyone has from time to time due to the stress of everyday life. It is thought to be caused by a chemical imbalance in parts of the brain. This imbalance affects your whole body and can cause emotional and physical symptoms such as feeling low in spirit, loss of interest in activities, being unable to enjoy life, poor appetite or overeating, disturbed sleep, often waking up early, loss of sex drive, lack of energy and feeling guilty over nothing.
- Generalised anxiety disorder, where patients have excessive anxiety and worry.
- Schizophrenia, an illness with disturbances in thinking, feelings and behaviour.
SEROQUEL XR belongs to a group of medicines called antipsychotics.
Ask your doctor if you have any questions about why SEROQUEL XR has been prescribed for you. Your doctor may have prescribed this medicine for another reason.
This medicine is only available with a doctor's prescription.
You may find it helpful to tell a friend or relative that you are suffering from these symptoms, and ask them to read this leaflet. You might ask them to tell you if they think your symptoms are getting worse, or if they are worried about any other changes in your behaviour.
SEROQUEL XR is not addictive.
Before you take it
When you must not take it
Do not take SEROQUEL XR if you have an allergy to:
- quetiapine, the active ingredient in SEROQUEL and SEROQUEL XR
- any of the other ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include shortness of breath, wheezing or difficulty breathing; swelling of the face, lips, tongue or other parts of the body; rash, itching or hives on the skin or you may feel faint.
SEROQUEL XR is not recommended for use in children. There is not enough information on its effects in children.
SEROQUEL XR, as with other antipsychotic medicines, is recommended for use with caution in the elderly and is not approved for treatment of dementia and behavioural disturbances. In clinical studies with this group of medicines for the treatment of dementia and behavioural disturbances in the elderly, have suggested an increased risk of cardiovascular adverse events including stroke, and increased mortality risk for elderly patients has been reported.
Do not take it after the use by (expiry) date printed on the pack.
Do not take it if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking SEROQUEL XR talk to your doctor or pharmacist.
Before you start to take it
Tell your doctor if you have any allergies to:
- any other medicines
- any other substances such as foods, dyes or preservatives
Tell your doctor or pharmacist if you have, or have had, any medical conditions, especially the following:
- heart or blood vessel problems or a family history of heart or blood vessel problems including low blood pressure, stroke, problems with your circulation or any condition that affects blood flow to the brain, problems with the way your heart beats or a history of heart attack
- liver problems
- diabetes or a family history of diabetes. Patients with diabetes or who have a higher chance of diabetes should have their blood sugar checked before and during treatment with SEROQUEL XR.
- epilepsy (seizures or fits)
- dementia or related behavioural disorders (especially in elderly patients)
- low white blood cell count
- sleep apnoea - a condition where you stop breathing for short periods during your normal nightly sleep
- urinary retention (a condition where you can't completely empty your bladder)
- an enlarged prostate
- a blockage in your intestines
- increased pressure inside your eyes or glaucoma
- history of alcohol or drug abuse
Tell your doctor or mental health professional if you have any mental/mood changes or suicidal thoughts. Depression and other mental illnesses can increase the risk of suicide. It is important to discuss all the risks of treating depression and mental illness as well as the risks of not treating it. You should discuss all treatment choices with your doctor, not just the use of antidepressants.
Patients (and caregivers of patients) need to monitor for any worsening of their condition and/or the emergence of thoughts of suicide or suicidal behaviour or thoughts of harming themselves and to seek medical advice immediately if these symptoms present.
Do not take SEROQUEL XR if you are pregnant or breastfeeding unless your doctor says so. Ask your doctor about the risks and benefits involved. It is not known if it is safe for you to take it while you are pregnant.
Neonates exposed to antipsychotic drugs (including quetiapine) may experience agitation, hypertonia (high level muscle tone), hypotonia (decreased muscle tone), tremor, somnolence, respiratory distress and feeding disorder following delivery (extrapyramidal neurological disturbances and/or withdrawal symptoms). These complications have varied in severity; while in some cases symptoms have been self-limited, in other cases neonates have required additional medical treatment or monitoring.
However, if you need to take it during your pregnancy, the doctor will discuss the risks and benefits of taking it with you.
It is recommended that you do not breastfeed while taking it, as it may pass into breast milk.
Before your doctor starts you on SEROQUEL XR your doctor may want to take some tests (eg blood tests, blood pressure, weight or height measurements). These tests may help to prevent side effects.
Tell your doctor if you are lactose intolerant. SEROQUEL XR tablets contain lactose.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and SEROQUEL XR may interfere with each other, these include:
- phenytoin or carbamazepine - medicines for epilepsy
- medicines for high blood pressure (including diuretics or fluid tablets) or heart conditions
- lorazepam - a medicine used to help you sleep
- medicines used to treat anxiety, depression, mood swings, attention deficit hyperactivity disorder (ADHD) or other mood disorders
- medicines for fungal infections such as ketoconazole
- some antibiotics such as rifampicin and erythromycin
- thioridazine - an antipsychotic medicine
- medicines used to treat Parkinson's disease
- stimulants such as amphetamines
- glucocorticoids - medicines used to treat inflammation
- medicines for Human Immunodeficiency Virus (HIV)
- medicines that have anticholinergic (muscarinic) effects
These medicines may be affected by SEROQUEL XR, or may affect how well it works. You may need different amounts of your medicine or you may need to take different medicines. Your doctor will advise you.
Your doctor and pharmacist have more information about medicines to be careful with or avoid while taking SEROQUEL XR.
If you have not told your doctor about any of these things, tell them before you take any SEROQUEL XR.
How to take it
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
If you do not understand the instructions on the pack ask your doctor or pharmacist for help.
How to take it
Swallow your SEROQUEL XR tablets whole with a full glass of water. Do not split, chew or crush the tablets. If you split, chew or crush the tablets they will not work properly.
How much to take
Your doctor will tell you how many tablets you will need to take each day and how long you need to take it. This depends on your condition and whether or not you are taking any other medicines.
SEROQUEL XR is usually started as a low dose that will be increased by your doctor. Your doctor will recommend a dose especially for you. This will depend on various factors including your age, condition being treated, other medical conditions (eg liver problems), other medicines you are taking and how you may react to SEROQUEL XR.
Your doctor will monitor your condition and may change your dose depending on how you respond to it. Your doctor will use the lowest dose for the least amount of time to keep you well.
Your doctor may have switched your treatment from SEROQUEL tablets to SEROQUEL XR tablets. Your doctor will generally prescribe you a once daily dose of SEROQUEL XR, which is equivalent to your total daily dose of SEROQUEL tablets. Your doctor will tell you how many tablets you will need to take each day.
When to take it
SEROQUEL XR should be taken once a day, at approximately the same time each day. Taking your tablets at the same time each day will have the best effect. It will also help you remember when to take the tablets.
It should be taken without food.
How long to take it
Continue taking the tablets for as long as your doctor tells you.
SEROQUEL XR helps control your condition, but does not cure it. Therefore you must take it every day.
Do not stop taking it unless your doctor tells you to - even if you feel better.
If you forget to take it
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to. Otherwise, take it as soon as you remember, and then go back to taking your medicine as you would normally.
Do not take a double dose to make up for the dose that you missed.
If you are not sure what to do, ask your doctor or pharmacist.
If you have trouble remembering when to take your medicine, ask your pharmacist for some hints.
If you take too much (overdose)
Immediately telephone your doctor or the Poisons Information Centre (13 11 26) for advice, or go to Accident and Emergency at your nearest hospital if you think that you or anyone else may have taken too much SEROQUEL XR. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
If you take too many SEROQUEL XR tablets you may feel drowsy, sleepy, dizzy or have fast heart beats.
SEROQUEL XR overdose may lead to gastric bezoar (tightly packed partially digested material in stomach) formation.
Patients with pre-existing severe cardiovascular disease may be at an increased risk of the effects of overdose.
There were cases reported of QT prolongation (abnormal electrocardiogram) with overdose.
There have been very rare reports of overdose of quetiapine alone resulting in death or coma.
While you are taking it
Things you must do
Tell any other doctors, dentists, and pharmacists who are treating you that you are taking it.
If you are about to be started on any new medicines, tell your doctor, dentist or pharmacist that you are taking it.
Tell your doctor or mental health professional immediately, or go to the nearest hospital, if you have any of the following suicidal thoughts or other mental/mood changes:
- thoughts or talk of death or suicide
- thoughts or talk of self-harm or harm to others
- any recent attempts of self-harm
- increase in aggressive behaviour, irritability or agitation
- worsening of depression
Occasionally, the symptoms of depression may include thoughts of suicide or self-harm. These symptoms may continue or get worse during the early stages of treatment until the effect of the medicine becomes apparent. All mentions of suicide or violence must be taken seriously.
If you plan to have surgery that needs a general anaesthetic, tell your doctor or dentist that you are taking it.
If you become pregnant while taking it, tell your doctor immediately.
If you need to have any medical tests (including urine drug screening) while you are taking it, tell your doctor. It may affect the results of some tests.
Be sure to keep all of your doctor's appointments so that your progress can be checked. Your doctor will check your progress and may want to take some tests (eg blood tests, blood pressure, weight or height measurements) from time to time. These tests may help to prevent side effects.
Things you must not do
Do not stop taking it, or change the dosage, even if you are feeling better, without checking with your doctor. If you stop taking it suddenly, your condition may worsen or your chance of getting an unwanted side effect may increase. To prevent this, your doctor may gradually reduce the amount of SEROQUEL XR you take each day before stopping completely.
Do not take it to treat any other complaints unless your doctor tells you to.
Do not give this medicine to anyone else, even if their symptoms seem similar or they have the same condition as you.
Do not take any medicines that cause drowsiness while you are taking it, unless recommended by your doctor.
Things to be careful of
Be careful driving or operating machinery until you know how SEROQUEL XR affects you. It can make some people dizzy or sleepy. Make sure you know how you react to it before you drive a car, operate machinery or do anything else that could be dangerous if you are dizzy or sleepy.
If it makes you feel light-headed, dizzy or faint, be careful when getting up from a sitting or lying position. Standing up slowly, especially when you get up from bed or chairs, will help your body get used to the change in position and blood pressure. If this problem continues or gets worse, talk to your doctor.
Be careful when drinking alcohol while you are taking it. Combining SEROQUEL XR and alcohol can make you more sleepy or dizzy. Your doctor may suggest you avoid alcohol while you are being treated with it.
Avoid getting over-heated or dehydrated - do not over-exercise, in hot weather stay inside in a cool place, stay out of the sun, do not wear too much or heavy clothing, drink plenty of water. Keep warm in cool weather. SEROQUEL XR may affect the way your body reacts to temperature changes.
Avoid drinking large quantities of grapefruit juice. This medicine may be affected by grapefruit juice. Talk to your doctor or pharmacist if you have any concerns.
Talk to your doctor or pharmacist about these things if you think they may bother you.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking it.
All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects. Some side effects may be related to the dose of SEROQUEL XR or may be more likely to occur during long term treatment. Therefore, it is important that you tell your doctor as soon as possible if you notice anything that is making you feel unwell, even if you think the problems are not connected with this medicine. Your doctor may then decide to adjust your dose or use a different medicine.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor if you notice any of the following and they worry you:
- feeling sleepy
- weight gain, increased appetite
- dry mouth
- upset stomach, constipation, indigestion, vomiting (mainly in elderly or children)
- feeling weak
- swelling of the hands, ankles or feet
- runny or stuffy nose (particularly in children)
- blurred vision
- abnormal dreams, nightmares
- irritability
- confusion
- shortness of breath, difficulty in breathing and/or tightness in the chest
- fast or irregular heartbeats (palpitations)
- muscle pain or swelling or weakness
- headache
- insomnia
- diarrhoea
These side effects are usually mild. Some of these side effects may go away after a while.
Tell your doctor as soon as possible if you notice the following:
- difficulty swallowing
- falling, feeling dizzy or faint on standing up
- flat and red skin lesions or substantial hemorrhages under the skin (purpura)
- difficulty in speaking
- rapid heart beat
- symptoms of high sugar levels in the blood (including passing large amounts of urine, excessive thirst, increase in appetite with a loss of weight, feeling tired, drowsy, weak, depressed, irritable and generally unwell)
- breast enlargement, unusual secretion of breast milk
- cutaneous vasculitis, with skin symptoms such as lesions, including palpable purpura (discoloration of skin, raised and can be felt), petechiae (tiny spots of bleeding under the skin), urticaria, ulcers, livedo reticularis (a type of skin disorder), and nodules.
These are serious side effects. You may need medical attention.
If any of the following happen, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- abnormal muscle movements, including difficulty starting muscle movements, shaking, restlessness or muscle stiffness without pain.
- worm-like movements of the tongue or other uncontrolled movements of the tongue, mouth, cheeks or jaw which may progress to the arms and legs (a disorder called ‘tardive dyskinesia)
- a sudden increase in body temperature, with sweating, or a fast heart beat
- bleeding or bruising more easily than normal
- very marked drowsiness
- reduced consciousness
- fits (seizures)
- long-lasting and painful erections
- fainting (particularly in children)
- widespread skin rash that may include blistering or peeling of the skin, often accompanied by flu like symptoms, fever, swelling of the face and/or swollen lymph nodes (painful, warm, or red lump under your skin - often under your chin, on your neck, groin, armpit or behind your ear). These symptoms may also be associated with changes in your blood (eg white blood cell increase, as sometimes seen in allergic reactions) or liver function. These are some of the symptoms of potentially life-threatening conditions called Stevens-Johnson Syndrome (SJS), toxic epidermal necrolysis (TEN) and drug reaction with eosinophilia and systemic symptoms (DRESS).
- severe allergic reaction (may include severe difficulty in breathing, shock, swelling of the face, lips, tongue or other parts of the body, skin rash, hayfever, or you may feel faint)
- signs of frequent infections such as fever, chills, sore throat or mouth ulcers
- severe upper stomach pain, often with nausea and vomiting (particularly in patients with other risk factors such as gallstones, alcohol consumption and/or increased levels of certain fats within the blood). These are symptoms of pancreatitis.
- Combination of fever, very marked drowsiness, muscle stiffness, marked increase in blood pressure or heartbeats and reduced consciousness (a disorder called "neuroleptic malignant syndrome").
These are very serious side effects. Stop using SEROQUEL XR if you develop these symptoms. You may need urgent medical attention or hospitalisation.
Occasionally, SEROQUEL XR may be associated with changes in your liver function or blood (eg blood fat levels such as cholesterol or triglyceride, blood sugar levels, blood pressure, thyroid hormone levels, white blood cells). These can only be found when your doctor does tests from time to time to check your progress.
Other side effects not listed here may occur in some patients. Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
After taking it
Storage
Keep your tablets in the blister pack until it is time to take them. If you take the tablets out of the blister pack they will not keep well.
Keep it in a cool dry place where the temperature stays below 30°C.
Do not store it or any other medicine in the bathroom or near a sink. Do not leave it in the car or on a window sill. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop taking it or the tablets have passed their expiry date, ask your pharmacist what to do with any that are left over.
Product description
What SEROQUEL XR looks like
SEROQUEL XR tablets are capsuleshaped and are embossed with "XR" and the strength on one side, and plain on the other. Tablet colouring is as follows:
- 50 mg - peach
- 150 mg - white
- 200 mg - yellow
- 300 mg - pale yellow
- 400 mg - white
All strengths are available in packs of 10 or 60 tablets.
Ingredients
Each SEROQUEL XR tablet contains quetiapine fumarate as the active ingredient equivalent to quetiapine 50 mg, 150 mg, 200 mg, 300 mg or 400 mg.
Other ingredients include:
- Microcrystalline cellulose (E460)
- Sodium citrate dihydrate
- Lactose monohydrate
- Magnesium stearate (E572)
- Hypromellose
- Macrogol 400
- Titanium dioxide (E171)
- Iron oxide red CI77491 (E172 - 50 mg only)
- Iron oxide yellow CI77492 (E172 - 50 mg, 200 mg and 300 mg)
SEROQUEL XR tablets do not contain gluten or sucrose.
Supplier
Luye Pharma Australia Pty Ltd
ABN 56 637 287 80
Level 3, 160 Sussex Street
SYDNEY NSW 2000
Telephone: +61 8 7079 0504
[email protected]
This leaflet was prepared on 15 November 2022
SEROQUEL XR Australian Registration Numbers:
50 mg - AUST R 138917
150 mg - AUST R 153883
200 mg - AUST R 138920
300 mg - AUST R 138921
400 mg - AUST R 138922
SEROQUEL XR is a registered trademark of the AstraZeneca group of companies
©AstraZeneca, 2020
Published by MIMS January 2023




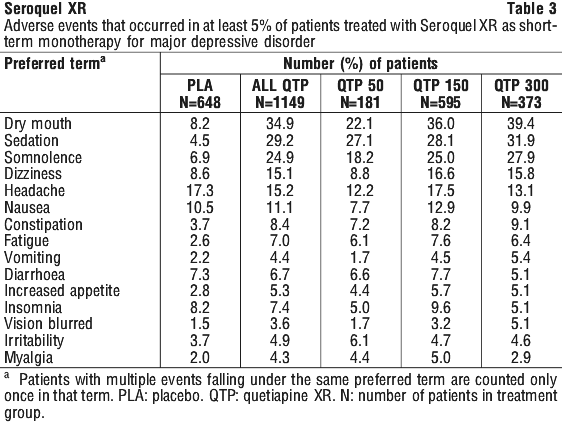 The treatment emergent adverse events that occurred during adjunct therapy (up to 6 weeks) of MDD in at least 5% of patients treated with Seroquel XR in placebo controlled trials are listed in Table 4 regardless of causality.
The treatment emergent adverse events that occurred during adjunct therapy (up to 6 weeks) of MDD in at least 5% of patients treated with Seroquel XR in placebo controlled trials are listed in Table 4 regardless of causality. The pattern of adverse events in the elderly population treated with Seroquel XR (short-term monotherapy) was similar to that seen in younger patients, with somnolence, headache, dry mouth and dizziness predominating.
The pattern of adverse events in the elderly population treated with Seroquel XR (short-term monotherapy) was similar to that seen in younger patients, with somnolence, headache, dry mouth and dizziness predominating.




 Very rare cases of cataract have been reported in the post-marketing data, but no causal link between these reports and quetiapine has been established.
Very rare cases of cataract have been reported in the post-marketing data, but no causal link between these reports and quetiapine has been established.

 Maintenance treatment with Seroquel was superior to placebo in increasing the time to recurrence of a depressive or a manic event (see Table 11). Patients on Seroquel also had a lower risk of experiencing a depressive or a manic event prior to week 28 and week 52 compared to patients on placebo (see Table 12).
Maintenance treatment with Seroquel was superior to placebo in increasing the time to recurrence of a depressive or a manic event (see Table 11). Patients on Seroquel also had a lower risk of experiencing a depressive or a manic event prior to week 28 and week 52 compared to patients on placebo (see Table 12).

 The safety and efficacy of quetiapine 300 mg and 600 mg once daily for the treatment of bipolar depression was established in 4 similarly designed placebo controlled clinical trials (n = 2461) over 8 weeks with 2 of these studies assessing maintenance of effect for up to 52 weeks. In all 4 studies quetiapine doses of 300 mg/day and 600 mg/day demonstrated clinical and statistical superiority to placebo in the treatment of depression at 8 weeks. The magnitude of the antidepressant effect was also supported by the secondary outcome variables. Alleviation of anxiety symptoms by quetiapine in all 4 studies was confirmed by a statistically superior Hamilton Rating Scale for Anxiety (HAM-A) total score change from baseline compared to placebo. Efficacy was demonstrated to be independent of bipolar I or II diagnosis, rapid cycling course, gender, age or ethnicity.
The safety and efficacy of quetiapine 300 mg and 600 mg once daily for the treatment of bipolar depression was established in 4 similarly designed placebo controlled clinical trials (n = 2461) over 8 weeks with 2 of these studies assessing maintenance of effect for up to 52 weeks. In all 4 studies quetiapine doses of 300 mg/day and 600 mg/day demonstrated clinical and statistical superiority to placebo in the treatment of depression at 8 weeks. The magnitude of the antidepressant effect was also supported by the secondary outcome variables. Alleviation of anxiety symptoms by quetiapine in all 4 studies was confirmed by a statistically superior Hamilton Rating Scale for Anxiety (HAM-A) total score change from baseline compared to placebo. Efficacy was demonstrated to be independent of bipolar I or II diagnosis, rapid cycling course, gender, age or ethnicity. Quetiapine patients also had a lower risk of experiencing a depressive event at weeks 26 and 52 compared to patients on placebo. The analysis of time to a depressive event mirrored the overall mood event results with patients on quetiapine having a 57% less risk of experiencing a depressive event compared with patients treated with placebo (HR 0.43, 95% CI 0.30, 0.62, p < 0.001). The risk of a depressive event for quetiapine versus placebo was reduced by 52% for the 300 mg dose and by 61% for the 600 mg dose.
Quetiapine patients also had a lower risk of experiencing a depressive event at weeks 26 and 52 compared to patients on placebo. The analysis of time to a depressive event mirrored the overall mood event results with patients on quetiapine having a 57% less risk of experiencing a depressive event compared with patients treated with placebo (HR 0.43, 95% CI 0.30, 0.62, p < 0.001). The risk of a depressive event for quetiapine versus placebo was reduced by 52% for the 300 mg dose and by 61% for the 600 mg dose. The proportion of patients showing ≥ 50% reduction in YMRS total score (responders) was statistically significantly higher for the Seroquel XR group compared to the placebo group at day 8 (week 1) and at the end of treatment. The proportion of patients showing a YMRS total score ≤ 12 (remission) was statistically significantly higher for the Seroquel XR group compared to the placebo group by day 8 (week 1) and at the end of treatment. The changes in CGI-BP-S and CGI-BP-I overall illness scores were statistically significant in favour of Seroquel XR at day 4 and at end of treatment.
The proportion of patients showing ≥ 50% reduction in YMRS total score (responders) was statistically significantly higher for the Seroquel XR group compared to the placebo group at day 8 (week 1) and at the end of treatment. The proportion of patients showing a YMRS total score ≤ 12 (remission) was statistically significantly higher for the Seroquel XR group compared to the placebo group by day 8 (week 1) and at the end of treatment. The changes in CGI-BP-S and CGI-BP-I overall illness scores were statistically significant in favour of Seroquel XR at day 4 and at end of treatment. The efficacy of Seroquel XR in the treatment of MDD was further demonstrated in two 6 week placebo controlled, fixed dose trials (n = 936) as combination therapy with an antidepressant in patients who had previously shown an inadequate response to at least one antidepressant. Seroquel XR 300 mg once daily in combination with ongoing antidepressant therapy was superior to antidepressant therapy alone in reduction of MADRS total score in both trials while Seroquel XR 150 mg was superior to antidepressant therapy alone in one study only. Improvement in depressive symptoms was seen at week 1 through end of study (week 6).
The efficacy of Seroquel XR in the treatment of MDD was further demonstrated in two 6 week placebo controlled, fixed dose trials (n = 936) as combination therapy with an antidepressant in patients who had previously shown an inadequate response to at least one antidepressant. Seroquel XR 300 mg once daily in combination with ongoing antidepressant therapy was superior to antidepressant therapy alone in reduction of MADRS total score in both trials while Seroquel XR 150 mg was superior to antidepressant therapy alone in one study only. Improvement in depressive symptoms was seen at week 1 through end of study (week 6).



