1 Name of Medicine
Sevoflurane.
2 Qualitative and Quantitative Composition
Sevoflurane is a nonflammable and nonexplosive liquid administered by vaporisation. Sevorane is a clear, colourless, stable liquid. At least 300 ppm of water is present to provide protection from environmental Lewis acids. No other additives or chemical stabilisers are used.
It is nonpungent.
The chemical name is fluoromethyl 2,2,2-trifluoro-1-(trifluoromethyl)-ethyl ether.
Some physical constants of the compound are: Molecular weight: 200.05. Specific gravity at 20°C: 1.520-1.525. Boiling point at 760 mmHg: 58.6°C. Vapour pressure: 157 mmHg at 20°C; 197 mmHg at 25°C; 317 mmHg at 36°C. Distribution partition coefficients at 37°C: blood/gas 0.63-0.69; water/gas 0.36; olive oil/gas 47.2-53.9; brain/gas 1.15. Mean component/gas partition coefficient at 25°C: conductive rubber 14.0; butyl rubber 7.7; polyvinyl chloride 17.4; polyethylene 1.3.
3 Pharmaceutical Form
Sevorane (sevoflurane) is an inhalation anaesthetic, packaged in 100 mL* and 250 mL amber-coloured plastic bottles.
(* Presentation not currently marketed).
4.1 Therapeutic Indications
Sevorane may be used for induction and maintenance of general anaesthesia in adult and paediatric patients undergoing surgery.
4.2 Dose and Method of Administration
The concentration of sevoflurane being delivered from a vaporiser during anaesthesia should be known. This may be accomplished by using a vaporiser calibrated specifically for sevoflurane.
Premedication.
Premedication should be selected according to the need of the individual patient, and at the discretion of the anaesthetist.
Induction.
Dosage should be individualised and titrated to the desired effect according to the patient's age and clinical status. A short acting barbiturate or other intravenous induction agent may be administered followed by inhalation of sevoflurane. Induction with sevoflurane may be achieved in oxygen or in combination with oxygen-nitrous oxide mixtures. In adults inspired concentrations of up to 5% sevoflurane usually produce surgical anaesthesia in less than 2 minutes. In children inspired concentrations of up to 7% sevoflurane usually produce surgical anaesthesia in less than 2 minutes.
Maintenance.
Surgical levels of anaesthesia may be sustained with concentrations of 0.5-3% sevoflurane with or without the concomitant use of nitrous oxide (see Table 1).
Elderly.
As with other inhalation agents, lesser concentrations of sevoflurane are normally required to maintain anaesthesia.
The minimum alveolar concentration (MAC) is the concentration at which 50% of the population tested does not move in response to a single stimulus of skin incision. MAC equivalents for sevoflurane for various age groups are summarised in Table 1.

Emergence.
Emergence times are generally short following sevoflurane anaesthesia. Therefore, patients may require postoperative pain relief earlier.
Renal or hepatic impairment.
Sevoflurane did not exacerbate pre-existing renal or hepatic impairment in clinical studies. However, caution is recommended when using Sevoflurane in patients with renal insufficiency (see Section 4.4 Special Warnings and Precautions for Use).4.3 Contraindications
Sevoflurane should not be used in patients with known sensitivity to sevoflurane or to other halogenated agents (e.g. history of hepatotoxicity, usually including elevated liver enzymes, fever, leukocytosis and/or eosinophilia temporally related to anaesthesia with one of these agents) or with known or suspected genetic susceptibility to malignant hyperthermia.
The use of sevoflurane in anaesthesia apparatus employing rebreathing circuits which contain Baralyme is contraindicated. (See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
4.4 Special Warnings and Precautions for Use
Sevoflurane may cause respiratory depression, which may be augmented by narcotic premedication or other agents causing respiratory depression. Respiration should be supervised and if necessary, assisted.
Sevoflurane should be administered only by persons trained in the administration of general anaesthesia. Facilities for maintenance of a patent airway, artificial ventilation and oxygen enrichment and circulatory resuscitation must be immediately available.
The concentration of sevoflurane being delivered from a vaporizer must be known exactly. As volatile anaesthetics differ in their physical properties, only vaporizers specifically calibrated for sevoflurane must be used. The administration of general anaesthesia must be individualized based on the patient's response. Hypotension and respiratory depression increase as anaesthesia is deepened.
Isolated reports of QT prolongation, very rarely associated with torsades de pointes (in exceptional cases, fatal), have been received. Caution should be exercised when administering sevoflurane to susceptible patients.
Isolated cases of ventricular arrhythmia were reported in paediatric patients with Pompe's disease.
Caution should be exercised in administering general anaesthesia, including sevoflurane, to patients with mitochondrial disorders.
During maintenance of anaesthesia, increasing the concentration of sevoflurane produces dose dependent decreases in blood pressure. An excessive decrease in blood pressure may be related to depth of anaesthesia and in such instances may be corrected by decreasing the inspired concentration of sevoflurane.
As with all anaesthetics, maintenance of haemodynamic stability is important to the avoidance of myocardial ischaemia in patients with coronary artery disease.
The recovery from general anaesthesia should be assessed carefully before patients are discharged from the postanaesthesia care unit.
Replacement of desiccated CO2 absorbents.
Rare cases of extreme heat, smoke, and/or spontaneous fire in the anaesthesia machine have been reported during sevoflurane use in conjunction with the use of desiccated CO2 absorbent, specifically those containing potassium hydroxide (e.g. Baralyme). An unusually delayed rise or unexpected decline of inspired sevoflurane concentration compared to the vaporizer setting may be associated with excessive heating of the CO2 absorbent canister.
An exothermic reaction, enhanced sevoflurane degradation, and production of degradation products can occur when the CO2 absorbent becomes desiccated, such as after an extended period of dry gas flow through the CO2 absorbent canisters. Sevoflurane degradants (methanol, formaldehyde, carbon monoxide, and Compounds A, B, C, and D) were observed in the respiratory circuit of an experimental anaesthesia machine using desiccated CO2 absorbents and maximum sevoflurane concentrations (8%) for extended periods of time (= 2 hours). Concentrations of formaldehyde observed at the anaesthesia respiratory circuit (using sodium hydroxide containing absorbents) were consistent with levels known to cause mild respiratory irritation. The clinical relevance of the degradants observed under this extreme experimental model is unknown.
When a clinician suspects that the CO2 absorbent may be desiccated, it should be replaced before administration of sevoflurane. The colour indicator of most CO2 absorbents does not necessarily change as a result of desiccation. Therefore, the lack of significant colour change should not be taken as an assurance of adequate hydration. CO2 absorbents should be replaced routinely regardless of the state of the colour indicator.
Compound A.
The production of degradants in the anaesthesia circuit results from the extraction of the acidic proton in the presence of a strong base (KOH and/or NaOH) forming an alkene (Compound A) from sevoflurane, similar to formation of 2-bromo-2-chloro-1,1-difluoroethylene (BCDFE) from halothane. Baralyme causes more production of Compound A than does soda lime. Laboratory simulations have shown that the concentration of these degradants is inversely correlated with the fresh gas flow rate (see Figure 1).
At a fresh gas flow rate of 1 L/min, mean maximum concentrations of Compound A in the anaesthesia circuit in clinical settings are approximately 20 ppm (0.002%) with soda lime and 30 ppm (0.003%) with Baralyme in adult patients; mean maximum concentrations in paediatric patients with soda lime are about half those found in adults. The highest concentration observed in a single patient with Baralyme was 61 ppm (0.0061%) and 32 ppm (0.0032%) with soda lime. The concentrations of Compound A, measured in the anaesthesia circuit when sevoflurane is used clinically are not known to be deleterious to humans.
 Sevoflurane produces low levels of Compound A (pentafluoroisopropenyl fluoromethyl ether (PIFE)) and trace amounts of Compound B (pentafluoromethoxy isopropyl fluoromethyl ether (PMFE)), when in direct contact with CO2 absorbents. Levels of Compound A increase with an increase in canister temperature; increase in anaesthetic concentration, decrease in gas flow rate and increase more with the use of Baralyme rather than soda lime. Although Compound A is a dose dependent nephrotoxin in rats, the mechanism of this renal toxicity is unknown and has not been established in humans. While a level of Compound A exposure at which clinical nephrotoxicity might be expected to occur has not been established, it is prudent to consider all of the factors leading to Compound A exposure in humans, especially duration of exposure, fresh gas flow rate and concentration of sevoflurane. During sevoflurane anaesthesia the clinician should adjust inspired concentration and fresh gas flow rate to minimise exposure to Compound A. Because of limited clinical experience with sevoflurane in low flow systems, fresh gas flow rates below 2 L/min in a circle absorber system are not recommended.
Sevoflurane produces low levels of Compound A (pentafluoroisopropenyl fluoromethyl ether (PIFE)) and trace amounts of Compound B (pentafluoromethoxy isopropyl fluoromethyl ether (PMFE)), when in direct contact with CO2 absorbents. Levels of Compound A increase with an increase in canister temperature; increase in anaesthetic concentration, decrease in gas flow rate and increase more with the use of Baralyme rather than soda lime. Although Compound A is a dose dependent nephrotoxin in rats, the mechanism of this renal toxicity is unknown and has not been established in humans. While a level of Compound A exposure at which clinical nephrotoxicity might be expected to occur has not been established, it is prudent to consider all of the factors leading to Compound A exposure in humans, especially duration of exposure, fresh gas flow rate and concentration of sevoflurane. During sevoflurane anaesthesia the clinician should adjust inspired concentration and fresh gas flow rate to minimise exposure to Compound A. Because of limited clinical experience with sevoflurane in low flow systems, fresh gas flow rates below 2 L/min in a circle absorber system are not recommended.
Malignant hyperthermia.
In susceptible individuals, potent inhalation anaesthetic agents including sevoflurane, may trigger a skeletal muscle hypermetabolic state leading to high oxygen demand and the clinical syndrome known as malignant hyperthermia. The clinical syndrome is signalled by hypercapnia, and may include muscle rigidity, tachycardia, tachypnoea, cyanosis, arrhythmias, and/or unstable blood pressure. Some of these nonspecific signs may also appear during light anaesthesia, acute hypoxia, hypercapnia and hypovolaemia.
In clinical trials, one case of malignant hyperthermia was reported in 3220 exposures (incidence 0.03%). The patient responded to dantrolene sodium, and subsequent muscle biopsy confirmed the patient's susceptibility to this condition. In addition, there have been postmarketing reports of malignant hyperthermia. Some of these reports have been fatal. Sevoflurane has been shown to trigger malignant hyperthermia in genetically susceptible pigs.
Treatment of malignant hyperthermia includes discontinuation of triggering agents (e.g. sevoflurane), administration of intravenous dantrolene sodium (consult product information for intravenous dantrolene sodium for additional information on patient management), and application of supportive therapy. Such therapy includes vigorous efforts to restore body temperature to normal, respiratory and circulatory support as indicated, and management of electrolyte fluid acid base abnormalities. Renal failure may appear later, and urine flow should be monitored and sustained if possible.
Hyperkalaemic cardiac arrest in paediatric patients.
Use of inhaled anaesthetic agents has been associated with rare increases in serum potassium levels that have resulted in cardiac arrhythmias and death in paediatric patients during the postoperative period. Patients with latent as well as overt neuromuscular disease, particularly Duchenne muscular dystrophy, appear to be most vulnerable. Concomitant use of succinylcholine has been associated with most, but not all, of these cases. These patients also experienced significant elevations in serum creatine kinase levels and, in some cases, changes in urine consistent with myoglobinuria. Despite the similarity in presentation to malignant hyperthermia, none of these patients exhibited signs or symptoms of muscle rigidity or hypermetabolic state. Early and aggressive intervention to treat the hyperkalaemia and resistant arrhythmias is recommended, as is subsequent evaluation for latent neuromuscular disease.
Seizures.
Rare cases of seizures have been reported in association with sevoflurane use (see Section 4.4 Special Warnings and Precautions for Use, Paediatric use; Section 4.8 Adverse Effects (Undesirable Effects)).
Use in renal impairment.
Because clinical experience in administering sevoflurane in patients with renal insufficiencies (creatinine > 1.5 mg/dL) is limited (n = 21), its safety in these patients has not been fully established. Limited pharmacology data in these patients appear to suggest that the half-life of sevoflurane may be increased. The clinical significance is unknown at this time. Therefore due to limited clinical experience sevoflurane should be used with caution in patients with renal insufficiency.
Use in hepatic impairment.
In a limited number of patients with mild to moderate hepatic impairment (n = 16), the hepatic function was not affected by sevoflurane. The safety of sevoflurane in patients with severe hepatic impairment has not yet been demonstrated; therefore, sevoflurane should be used with caution in these patients.
Very rare cases of mild, moderate and severe postoperative hepatic dysfunction or hepatitis with or without jaundice have been reported from postmarketing experiences.
Clinical judgment should be exercised when sevoflurane is used in patients with underlying hepatic conditions or under treatment with drugs known to cause hepatic dysfunction (see Section 4.8 Adverse Effects (Undesirable Effects)).
It has been reported that previous exposure to halogenated hydrocarbon anaesthetics, especially if the interval is less than 3 months, may increase the potential for hepatic injury.
Use in the elderly.
Fluoride concentrations have been measured after single, extended, and repeat exposure to sevoflurane in normal surgical and special patient populations, and pharmacokinetic parameters were determined. Compared with healthy individuals, the fluoride ion half-life was not affected in elderly patients.
Paediatric use.
The use of sevoflurane has been associated with seizures. Many of these have occurred in children and young adults starting from 2 months of age, most of whom had no predisposing risk factors. Clinical judgment should be exercised when using sevoflurane in patients who may be at risk for seizures. (See Section 4.8 Adverse Effects (Undesirable Effects)).
Some published studies in children have observed cognitive deficits after repeated or prolonged exposures to anaesthetic agents early in life. These studies have substantial limitations, and it is not clear if the observed effects are due to the anaesthetic/analgesic/sedation drug administration or other factors such as the surgery or underlying illness.
Published animal studies of some anaesthetic/analgesic/sedation drugs that are NMDA antagonists or GABAergic agonists have reported adverse effects on brain development in early life and late pregnancy (see Section 5.3 Preclinical Safety Data). The clinical significance of these nonclinical findings is yet to be determined.
With inhalation or infusion of such drugs, exposure is longer than the period of inhalation or infusion. Depending on the drug and patient characteristics, as well as dosage, the elimination phase may be prolonged relative to the period of administration.
Effects on laboratory tests.
Occasional cases of transient changes in hepatic function tests and isolated examples of mild impairment of renal concentrating ability have been reported.4.5 Interactions with Other Medicines and Other Forms of Interactions
Beta-sympathomimetic agents like isoprenaline and alpha and beta-sympathomimetic agents like adrenaline and noradrenaline should be used with caution during sevoflurane narcosis, due to a potential risk of ventricular arrhythmia.
There is a risk of crisis during the operation in patients undergoing treatment with nonselective MAO-inhibitors. It is generally recommended that treatment should be stopped 2 weeks prior to surgery.
Sevoflurane may lead to marked hypotension in patients treated with calcium antagonists, in particular dihydropyridine derivates.
Caution should be exercised when calcium antagonists are used concomitantly with inhalation anaesthetics due to the risk of additive negative inotropic effect.
Concomitant use of succinylcholine with inhaled anaesthetic agents has been associated with rare increases in serum potassium levels that have resulted in cardiac arrhythmias and death in paediatric patients during the postoperative period.
Sevoflurane has been shown to be safe and effective when administered concurrently with a wide variety of agents commonly encountered in surgical situations such as central nervous system agents, autonomic drugs, skeletal muscle relaxants, anti-infective agents including aminoglycosides, hormones and synthetic substitutes, blood derivatives and cardiovascular drugs.
Preclinical data suggest that the defluorination of sevoflurane by hepatic enzymes, and hence the production of fluoride, may be increased by agents such as alcohol, isoniazid and barbiturates.
Benzodiazepines and opioids.
Benzodiazepines and opioids are expected to decrease the MAC of sevoflurane in the same manner as with other inhalational anaesthetics. Sevoflurane administration is compatible with benzodiazepines and opioids as commonly used in anaesthetic practice.
Inducers of CYP2E1.
Medicinal products and compounds that increase the activity of cytochrome P450 isoenzyme CYP2E1, such as isoniazid and alcohol, may increase the metabolism of sevoflurane and lead to significant increases in plasma fluoride concentrations (see Section 5.2 Pharmacokinetic Properties).
Nitrous oxide.
As with other halogenated volatile anaesthetics, the MAC of sevoflurane is decreased when administered in combination with nitrous oxide. Using 50% N2O, the MAC equivalent is reduced approximately 50% in adult and approximately 25% in paediatric patients (see Section 4.2 Dose and Method of Administration).
Neuromuscular blocking agents.
As with other inhalational anaesthetic agents, sevoflurane affects both the intensity and duration of neuromuscular blockade by nondepolarising muscle relaxants.
Among nondepolarising agents, vecuronium, pancuronium and atracurium interactions have been studied. The requirements for nondepolarising muscle relaxants: (1) for endotracheal intubation, do not reduce the dose of nondepolarising muscle relaxants, (2) during maintenance of anaesthesia, the dose of nondepolarising muscle relaxants is likely to be reduced compared to that during N2O/ opioid anaesthesia. The dosage adjustments for these muscle relaxants when administered with sevoflurane are similar to those required with isoflurane. Administration of supplemental doses of muscle relaxants should be guided by the response to nerve stimulation.
Dosage reduction of neuromuscular blocking agents during induction of anaesthesia may result in delayed onset of conditions suitable for endotracheal intubation or inadequate muscle relaxation because potentiation of neuromuscular blocking agents is observed a few minutes after the beginning of sevoflurane administration.
When used to supplement alfentanil N2O anaesthesia, sevoflurane potentiates neuromuscular block induced with pancuronium, vecuronium or atracurium.
The effect of sevoflurane on suxamethonium chloride and the duration of depolarising neuromuscular blockade has not been studied.
There is an increased incidence of hypotension and chills occurring with the combination of sevoflurane and alfentanil.4.6 Fertility, Pregnancy and Lactation
Effects on fertility.
Potential effects of sevoflurane on male and female fertility have not been adequately investigated. In rats, after repeated administration of anaesthetic doses, there were suggestions of reduced fertility. The significance of these studies for humans is not known.
Reproduction studies have been performed in rats and rabbits at doses up to 2.2% and 1.8% respectively and have revealed no evidence of teratogenicity due to sevoflurane. However, teratogenic potential has not been adequately investigated in rabbits. The significance of these studies for humans is not known.
(Category B2)
There are no adequate and well controlled studies in pregnant women. Sevoflurane should be used during pregnancy only if clearly needed.
The safety of sevoflurane has been demonstrated in a clinical trial of anaesthesia for caesarean section. The safety of sevoflurane in labour and delivery has not been demonstrated.
Sevoflurane, like other inhalational agents, has relaxant effects on the uterus with the potential risk for uterine bleeding. Clinical judgment should be observed when using sevoflurane during obstetric anaesthesia.
Published animal studies of some anaesthetic/analgesic/sedation drugs that are NMDA antagonists or GABAergic agonists have reported adverse effects on brain development in early life and late pregnancy.
It is not known whether sevoflurane or its metabolites is excreted in human milk. Due to the absence of documented experience, women should be advised to skip breastfeeding for 48 hours after administration of sevoflurane and discard milk produced during this period.4.7 Effects on Ability to Drive and Use Machines
Although recovery of consciousness following sevoflurane administration generally occurs within minutes, the impact on intellectual function for two or three days following anaesthesia has not been studied. As with other anaesthetics, small changes in moods may persist for several days following administration.
Patients should be advised that performance of activities requiring mental alertness, such as operating a motor vehicle or hazardous machinery, may be impaired for some time after general anaesthesia.
4.8 Adverse Effects (Undesirable Effects)
As with all potent inhaled anaesthetics, sevoflurane may cause dose dependent cardiorespiratory depression. Most adverse events are mild or moderate in severity and transient in duration. Nausea, vomiting and delirium have been observed in the postoperative period, which may be due to the inhalational anaesthetic, other agents administered intraoperatively or postoperatively or the patient's response to the surgical procedure.
In clinical trials involving 2906 patients the incidence of cardiovascular adverse events was reported as less than 1%. The cardiovascular events reported were as follows: arrhythmia, ventricular extrasystoles, supraventricular extrasystoles, complete AV block, QT prolongation associated with Torsade, bigeminy, inverted T wave, atrial fibrillation, atrial arrhythmia, second degree heart block, S-T depressed.
Adverse event data are derived from reference controlled clinical trials in 2906 patients exposed to sevoflurane including 2069 adults and 837 children. Adverse events are listed by body system in order of decreasing frequency.
Adverse events during the induction period (from onset of anaesthesia by mask induction to surgical incision).
Adults (n = 118). Common (> 1% and < 10%). Cardiovascular.
Bradycardia 5%, hypotension 4%, tachycardia 2%.
Nervous system.
Agitation 7%.
Respiratory disorder.
Laryngospasm 8%, airway obstruction 8%, breathholding 5%, cough increased 5%.
Paediatric patients (n = 507). Very common (≥ 10%). Nervous system.
Agitation 15%.
Common (> 1% and < 10%). Cardiovascular.
Tachycardia 6%, hypotension 4%.
Digestive system.
Increased salivation 2%.
Respiratory system.
Breathholding 5%, cough increased 5%, laryngospasm 3%, apnoea 2%.
Adverse events during maintenance and emergence periods.
(All patients n = 2906). Very common (≥ 10%). Digestive system.
Nausea 25%, vomiting 18%.
Cardiovascular system.
Hypotension 11%.
Respiratory system.
Cough increased 11%.
Common (< 1% and < 10%). Body as a whole.
Shivering 6%, hypothermia 1%, movement 1%, fever 1%, headache 1%.
Cardiovascular system.
Bradycardia 5%, hypertension 2%, tachycardia 2%.
Nervous system.
Somnolence 9%, agitation 9%, dizziness 4%, increased salivation 4%.
Respiratory system.
Breathholding 2%, laryngospasm 2%.
Adverse events, postmarketing.
As with other anaesthetic agents:
cases of dystonic movement with spontaneous resolution have been reported in children receiving sevoflurane for induction of anaesthesia with an uncertain relationship to sevoflurane;
seizure-like activity (described as convulsions, seizures, tonic clonic movements and twitching) may occur on very rare occasions following sevoflurane administration. Reported events were of short duration and there was no evidence of any abnormality during emergence from anaesthesia or in the postoperative period.
Rare reports of postoperative hepatitis exist. In addition, there have been rare postmarketing reports of hepatic failure and hepatic necrosis associated with the use of potent volatile anaesthetic agents, including sevoflurane. However, the actual incidence and relationship of sevoflurane to these events cannot be established with certainty.
Rare reports of hypersensitivity (including contact dermatitis, rash, dyspnoea, wheezing, chest discomfort, swelling face, or anaphylactic reaction) have been received, particularly in association with long-term occupational exposure to inhaled anaesthetic agents, including sevoflurane.
Very rare events of acute renal failure have been reported with an uncertain relationship to sevoflurane.
Rare events of malignant hyperthermia (see Section 4.3 Contraindications; Section 4.4 Special Warnings and Precautions for Use) and allergic reactions, such as rash, urticaria, pruritus, bronchospasm, anaphylactic or anaphylactoid reactions have been reported (see Section 4.3 Contraindications).
There have been very rare postmarketing reports of cardiac arrest in the setting of sevoflurane use.
Reporting suspected adverse effects.
Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at http://www.tga.gov.au/reporting-problems.4.9 Overdose
In the event of overdosage, the following action should be taken. Discontinue administration of sevoflurane, maintain a patent airway, initiate assisted or controlled ventilation with oxygen and maintain adequate cardiovascular function.
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action.
Sevoflurane has been demonstrated to be a fast acting, nonirritating agent in a variety of animal species including man. Administration has been associated with a smooth, rapid loss of consciousness during inhalation induction and a rapid recovery following discontinuation of anaesthesia.
As with other halogenated agents, minimum alveolar concentration (MAC) decreases with age and with the addition of nitrous oxide (see Section 4.2 Dose and Method of Administration).
Induction is accomplished with a minimum of excitement or of signs of upper respiratory irritation, no evidence of excessive secretions within the tracheobronchial tree and no central nervous system stimulation. The times for induction and recovery were reduced in paediatric patients who received sevoflurane in clinical studies.
Clinical trials.
Some of the recovery variables evaluated during the sevoflurane clinical program are summarised in Tables 2, 3 and 4.


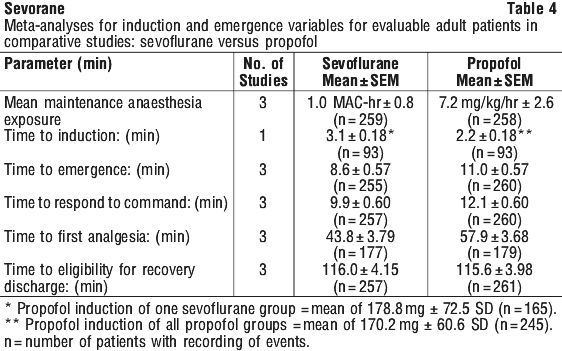
Cardiovascular effects.
Sevoflurane was studied in 14 healthy volunteers (18-35 years old) comparing sevoflurane-O2 (Sevo/O2) to sevoflurane-N2O/O2 (Sevo/N2O/O2) during 7 hours of anaesthesia. During controlled ventilation, haemodynamic parameters measured are shown in Figures 2-5.



 Sevoflurane is a dose related cardiac depressant. It does not produce increases in heart rate at doses less than 2 MAC.
Sevoflurane is a dose related cardiac depressant. It does not produce increases in heart rate at doses less than 2 MAC.
A study investigating the adrenaline induced arrhythmogenic effect of sevoflurane versus isoflurane in adult patients undergoing transsphenoidal hypophysectomy demonstrated that the threshold dose of adrenaline (i.e. the dose at which the first sign of arrhythmia was observed) producing multiple ventricular arrhythmias was 5 microgram/kg with both sevoflurane and isoflurane. Consequently, the interaction of sevoflurane with adrenaline appears to be equal to that seen with isoflurane.
Cardiovascular surgery/ coronary artery bypass graft (CABG) surgery.
Sevoflurane was compared to isoflurane as an adjunct with opioids in a multicentre study of 273 patients undergoing CABG surgery. The average MAC dose was 0.49 for sevoflurane and 0.53 for isoflurane. No statistical differences were observed between the two treatment groups with respect to incidence (sevoflurane 7%, isoflurane 11%) and duration (sevoflurane approx. 18 minutes, isoflurane approx. 17 minutes) of ischaemic events, number of patients with diagnosis of myocardial infarction (sevoflurane 8%, isoflurane 10%), time to haemodynamic stability (sevoflurane approx. 5 hours, isoflurane approx. 6 hours), or use of cardioactive drugs (sevoflurane 53%, isoflurane 47%).
Noncardiac surgery patients at risk for myocardial ischaemia.
Sevoflurane-N2O was compared to isoflurane-N2O for maintenance of anaesthesia in a multicentre study of 214 patients who were at mild to moderate risk for myocardial ischaemia who underwent elective noncardiac surgery. The average MAC dose was 0.49 for both drugs. No statistical differences were observed between the treatment groups for the incidence of any haemodynamic variation (tachycardia, bradycardia, hypertension, hypotension, and ischaemia without haemodynamic abnormality). No statistical differences were observed between the two regimens with respect to intraoperative incidence of myocardial ischaemia (sevoflurane 6%, isoflurane 3%) or postoperative incidence of ischaemic events (sevoflurane 10%, isoflurane 16%). No statistical differences were observed between the treatment groups for the incidence of study drug related adverse experiences by body system or by COSTART term (sevoflurane 60%, isoflurane 61%). There was one death in the sevoflurane group while four deaths occurred in the isoflurane group. None of these deaths were considered by the investigator to be drug related.
Paediatric anaesthesia.
The concentration of sevoflurane required for maintenance of general anaesthesia is age dependent (see Section 4.2 Dose and Method of Administration). An overall incidence of bradycardia (more than 20 beats/min less than normal) is lower for sevoflurane (3%) than for halothane (7%). Emergence times for sevoflurane are faster than with halothane (12 vs 19 minutes, respectively). A higher incidence of agitation occurs with sevoflurane (208/837 patients or 25%) when compared with halothane (114/661 patients or 17%).
Neurosurgery.
Three studies compared sevoflurane to isoflurane for maintenance of anaesthesia during neurosurgical procedures. In a study of 20 patients, there was no difference between sevoflurane and isoflurane with regard to recovery from anaesthesia. In two studies, a total of 22 patients with intracranial pressure (ICP) monitors received either sevoflurane or isoflurane. There was no difference between sevoflurane and isoflurane with regard to ICP response to inhalation of 0.5, 1.0 and 1.5 MAC inspired concentrations of volatile agent during N2O/O2/fentanyl anaesthesia. During progressive hyperventilation from PaCO2 = 40 to PaCO2 = 30, ICP response to hypocarbia was preserved with sevoflurane at both 0.5 and 1.0 MAC concentrations. In patients at risk for elevations of ICP, sevoflurane should be administered cautiously in conjunction with ICP reducing manoeuvers such as hyperventilation.
Caesarean section.
Sevoflurane (n = 29) was compared to isoflurane (n = 27) in ASA class I or II patients for the maintenance of anaesthesia during caesarean section. Newborn evaluations and recovery events were recorded. With both anaesthetics, Apgar scores averaged 8 and 9 at 1 and 5 minutes, respectively.
Use of sevoflurane as part of general anaesthesia for elective caesarean section produced no untoward effects in mother or neonate. Sevoflurane and isoflurane demonstrated equivalent recovery characteristics. There was no difference between sevoflurane and isoflurane with regard to the effect on the newborn, as assessed by Apgar score and neurological and adaptive capacity score (average = 29.5). The safety of sevoflurane in labour and vaginal delivery has not been evaluated.
5.2 Pharmacokinetic Properties
The low solubility of sevoflurane in blood would suggest that alveolar concentrations should rapidly increase upon induction and rapidly decrease upon cessation of the inhaled agent. This was confirmed in a clinical study where inspired and end tidal concentrations (FI and FA) were measured. The FA/FI (wash in) value at 30 minutes for sevoflurane was 0.85. The FA/FAO (wash out) value at 5 minutes was 0.15 where FAO is the last alveolar concentration measured immediately before discontinuance of the anaesthetic. See Figures 6 and 7.

 Yasuda N, Lockhart S, Eger El ll, et al: Comparison of kinetics of sevoflurane and isoflurane in humans. Anesth Analg 72: 316, 1991.
Yasuda N, Lockhart S, Eger El ll, et al: Comparison of kinetics of sevoflurane and isoflurane in humans. Anesth Analg 72: 316, 1991.
The rapid pulmonary elimination of sevoflurane minimises the amount of anaesthetic available for metabolism. In humans, approximately 5% sevoflurane absorbed is metabolised by cytochrome P450 2E1 to hexafluoroisopropanol (HFIP), with release of inorganic fluoride and carbon dioxide (or a one carbon fragment). Once formed, HFIP is rapidly conjugated with glucuronic acid and eliminated. No other metabolic pathways for sevoflurane have been identified. It is the only fluorinated volatile anaesthetic that is not metabolised to trifluoracetic acid.
Cytochrome P450 2E1 is the principal isoform identified for sevoflurane metabolism and this may be induced by chronic exposure to isoniazid and ethanol. This is similar to the metabolism of isoflurane and enflurane and is distinct from that of methoxyflurane which is metabolised via a variety of cytochrome P450 isoforms (Figure 8).
 Approximately 7% of patients/ volunteers evaluated for inorganic fluoride concentration in Abbott clinical studies had fluoride levels > 50 micromole (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Approximately 7% of patients/ volunteers evaluated for inorganic fluoride concentration in Abbott clinical studies had fluoride levels > 50 micromole (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Pharmacokinetics of fluoride ion.
Fluoride ion concentrations are influenced by the duration of anaesthesia, the concentration of sevoflurane administered, and the composition of the anaesthetic gas mixture. In studies where anaesthesia was maintained purely with sevoflurane for periods ranging from 1 to 6 hours, peak fluoride concentrations ranged between 12 micromole and 90 micromole. As shown in Figure 9, peak concentrations occur within 2 hours of the end of anaesthesia and are less than 25 micromole (475 nanogram/mL) for the majority of the population after 10 hours. The half-life is in the range of 15-23 hours.
It has been reported that following administration of methoxyflurane, serum inorganic fluoride concentrations > 50 micromole were correlated with the development of vasopressin resistant, polyuric renal failure. Inadequate data exist to evaluate the nephrotoxicity of elevated fluoride concentrations with sevoflurane. Isolated examples of mild impairment of concentrating ability have been reported. In clinical trials with sevoflurane, there were no reports of toxicity with elevated fluoride ion levels. Based on animal and human studies this methoxyflurane derived threshold does not appear valid for sevoflurane, perhaps due to sevoflurane's rapid pulmonary elimination, difference in cytochrome P450 isoforms involved in metabolism, low level of metabolism and lower area under the curve (see Figure 8).

Fluoride concentrations after repeat exposure and in special populations.
Fluoride concentrations have been measured after single, extended, and repeat exposure to sevoflurane in normal surgical and special patient populations, and pharmacokinetic parameters were determined.
Compared with healthy individuals, the fluoride ion half-life was prolonged in patients with renal impairment, but not in the elderly. A study in 8 patients with hepatic impairment suggests a slight prolongation of the half-life. The mean half-life in patients with renal impairment averaged approximately 33 hours (range 21-61 hours) as compared to a mean of approximately 21 hours (range 10-48 hours) in normal healthy individuals. The mean half-life in the elderly (greater than 65 years) approximated 24 hours (range 18-72 hours). The mean half-life in individuals with hepatic impairment was 23 hours (range 16-47 hours). Mean maximal fluoride values (Cmax) determined in individual studies of special populations are displayed below. Obesity is a risk factor contributing to elevated inorganic fluoride concentrations. See Table 5.

5.3 Preclinical Safety Data
Compound A has been shown to be nephrotoxic in rats after exposures that have varied in duration from one to three hours. No histopathologic change was seen at a concentration of up to 270 ppm for one hour. Sporadic single cell necrosis of proximal tubule cells has been reported at a concentration of 114 ppm after a 3 hour exposure to Compound A in rats. The LC50 reported at 1 hour is 1050-1090 ppm (male-female) and, at 3 hours, 350-490 ppm (male-female).
Published studies in pregnant and juvenile animals suggest that the use of anaesthetic/analgesic and sedation drugs that block NMDA receptors and/or potentiate GABA activity during the period of rapid brain growth or synaptogenesis may result in neuronal and oligodendrocyte cell loss in the developing brain and alterations in synaptic morphology and neurogenesis when used for longer than 3 hours. These studies included anaesthetic agents from a variety of drug classes.
Genotoxicity.
No mutagenic effect was noted in the Ames test and no chromosomal aberrations were induced in cultured mammalian cells.
Carcinogenicity.
Studies on carcinogenesis have not been performed.6 Pharmaceutical Particulars
6.1 List of Excipients
See Section 2 Qualitative and Quantitative Composition.
6.2 Incompatibilities
Sevoflurane is not corrosive to stainless steel, brass, aluminium, nickel plated brass, chrome plated brass, or copper beryllium alloy.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 30°C.
Sevoflurane is stable when stored under normal room lighting conditions. No discernible degradation occurs in the presence of strong acids or heat. In the absence of a suitable inhibitor (such as water used in Sevorane), sevoflurane can be degraded by Lewis acids (e.g. oxides of common metals such as iron and aluminium) to give hexafluoroisopropyl alcohol, formaldehyde, hydrogen fluoride and other degradants. Through a separate mechanism, degradation in the clinical setting has been observed through direct contact with CO2 absorbents (soda lime and Baralyme), producing pentafluoroisopropenyl fluoromethyl ether (PIFE, C4H2F6O), a haloalkene derivative also known as Compound A, and trace amounts of pentafluoromethoxy isopropyl fluoromethyl ether (PMFE, C5H6F6O), also known as Compound B. See Figure 10.
 Sevoflurane degradation in soda lime has been shown to increase with temperature. Since the reaction of carbon dioxide with absorbents is exothermic, this temperature increase will be determined by quantities of CO2 absorbed, which in turn will depend on fresh gas flow in the anaesthesia circle system, metabolic status of the patient, and ventilation. The relationship of temperature produced by varying levels of CO2 and Compound A production is illustrated in the above in vitro simulation where CO2 was added to a circle absorber system (see Figure 10).
Sevoflurane degradation in soda lime has been shown to increase with temperature. Since the reaction of carbon dioxide with absorbents is exothermic, this temperature increase will be determined by quantities of CO2 absorbed, which in turn will depend on fresh gas flow in the anaesthesia circle system, metabolic status of the patient, and ventilation. The relationship of temperature produced by varying levels of CO2 and Compound A production is illustrated in the above in vitro simulation where CO2 was added to a circle absorber system (see Figure 10).
6.5 Nature and Contents of Container
Sevorane (sevoflurane) is packaged in 100 mL* and 250 mL amber-coloured plastic bottles.
* Not currently marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure.

CAS number.
28523-86-6.7 Medicine Schedule (Poisons Standard)
Schedule 4- Prescription only Medicine.
Summary Table of Changes



 Sevoflurane produces low levels of Compound A (pentafluoroisopropenyl fluoromethyl ether (PIFE)) and trace amounts of Compound B (pentafluoromethoxy isopropyl fluoromethyl ether (PMFE)), when in direct contact with CO2 absorbents. Levels of Compound A increase with an increase in canister temperature; increase in anaesthetic concentration, decrease in gas flow rate and increase more with the use of Baralyme rather than soda lime. Although Compound A is a dose dependent nephrotoxin in rats, the mechanism of this renal toxicity is unknown and has not been established in humans. While a level of Compound A exposure at which clinical nephrotoxicity might be expected to occur has not been established, it is prudent to consider all of the factors leading to Compound A exposure in humans, especially duration of exposure, fresh gas flow rate and concentration of sevoflurane. During sevoflurane anaesthesia the clinician should adjust inspired concentration and fresh gas flow rate to minimise exposure to Compound A. Because of limited clinical experience with sevoflurane in low flow systems, fresh gas flow rates below 2 L/min in a circle absorber system are not recommended.
Sevoflurane produces low levels of Compound A (pentafluoroisopropenyl fluoromethyl ether (PIFE)) and trace amounts of Compound B (pentafluoromethoxy isopropyl fluoromethyl ether (PMFE)), when in direct contact with CO2 absorbents. Levels of Compound A increase with an increase in canister temperature; increase in anaesthetic concentration, decrease in gas flow rate and increase more with the use of Baralyme rather than soda lime. Although Compound A is a dose dependent nephrotoxin in rats, the mechanism of this renal toxicity is unknown and has not been established in humans. While a level of Compound A exposure at which clinical nephrotoxicity might be expected to occur has not been established, it is prudent to consider all of the factors leading to Compound A exposure in humans, especially duration of exposure, fresh gas flow rate and concentration of sevoflurane. During sevoflurane anaesthesia the clinician should adjust inspired concentration and fresh gas flow rate to minimise exposure to Compound A. Because of limited clinical experience with sevoflurane in low flow systems, fresh gas flow rates below 2 L/min in a circle absorber system are not recommended.





 Sevoflurane is a dose related cardiac depressant. It does not produce increases in heart rate at doses less than 2 MAC.
Sevoflurane is a dose related cardiac depressant. It does not produce increases in heart rate at doses less than 2 MAC.
 Yasuda N, Lockhart S, Eger El ll, et al: Comparison of kinetics of sevoflurane and isoflurane in humans. Anesth Analg 72: 316, 1991.
Yasuda N, Lockhart S, Eger El ll, et al: Comparison of kinetics of sevoflurane and isoflurane in humans. Anesth Analg 72: 316, 1991. Approximately 7% of patients/ volunteers evaluated for inorganic fluoride concentration in Abbott clinical studies had fluoride levels > 50 micromole (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Approximately 7% of patients/ volunteers evaluated for inorganic fluoride concentration in Abbott clinical studies had fluoride levels > 50 micromole (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).

 Sevoflurane degradation in soda lime has been shown to increase with temperature. Since the reaction of carbon dioxide with absorbents is exothermic, this temperature increase will be determined by quantities of CO2 absorbed, which in turn will depend on fresh gas flow in the anaesthesia circle system, metabolic status of the patient, and ventilation. The relationship of temperature produced by varying levels of CO2 and Compound A production is illustrated in the above in vitro simulation where CO2 was added to a circle absorber system (see Figure 10).
Sevoflurane degradation in soda lime has been shown to increase with temperature. Since the reaction of carbon dioxide with absorbents is exothermic, this temperature increase will be determined by quantities of CO2 absorbed, which in turn will depend on fresh gas flow in the anaesthesia circle system, metabolic status of the patient, and ventilation. The relationship of temperature produced by varying levels of CO2 and Compound A production is illustrated in the above in vitro simulation where CO2 was added to a circle absorber system (see Figure 10).
