What is in this leaflet
This leaflet answers some common questions about Telfast Decongestant.
It does not contain all the available information.
It does not take the place of talking to your pharmacist or doctor.
All medicines have risks and benefits. Your pharmacist or doctor has weighed the risks of you taking this medicine against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your pharmacist or doctor.
Keep this leaflet with the medicine. You may need to read it again.
What Telfast Decongestant is used for
Telfast Decongestant is used to relieve the symptoms of seasonal and perennial allergic rhinitis (including hayfever) with sinus/nasal congestion. Symptoms include:
- nasal and sinus congestion
- sneezing
- itchy, runny nose
- watery, itchy eyes
- itchy throat.
TELFAST Decongestant tablets contain a combination of two active ingredients, "fexofenadine" (an antihistamine) and "pseudoephedrine" (a decongestant).
Antihistamines help reduce allergic symptoms caused by a substance called histamine. Examples of these include: watery, itchy eyes, sneezing and runny nose.
Decongestants, like pseudoephedrine, work by reducing congestion in the upper respiratory tract, including the nose, nasal passages and sinuses, making it easier to breathe.
Your pharmacist or doctor may have given this medicine to you for another reason.
Ask your doctor or pharmacist if you have any questions about why this medicine has been recommended for you. Telfast Decongestant is only available from your pharmacist.
Before you take Telfast Decongestant
When you must not take it
Do not take this medicine if you are allergic to fexofenadine, pseudoephedrine, terfenadine or any of the other ingredients in Telfast Decongestant. These are listed at the end of this leaflet.
Some of the symptoms of an allergic reaction to Telfast Decongestant may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
Do not take Telfast Decongestant if you have:
- very high blood pressure
- severe coronary artery disease (heart disease caused by poor blood flow or narrowing of the blood vessels of the heart)
- narrow angle glaucoma
- urinary retention
- a sensitivity to adrenergic events (symptoms include insomnia, dizziness, weakness, tremor or irregular heart beat)
- or if you have taken monoamine oxidase inhibitors (medicines used to treat depression) in the last 14 days.
Do not take this medicine if you are pregnant or plan to become pregnant. This medicine is not recommended to be used during pregnancy. Your pharmacist or doctor will discuss the benefits and possible risks of taking the medicine during pregnancy.
Do not give this medicine to a child under the age of 12 years, unless your doctor has told you to do so.
If you are not sure whether you should start taking this medicine, talk to your pharmacist or doctor.
Do not use it after the expiry date (EXP) printed on the pack. If you take this medicine after the expiry date has passed, it may not work as well.
Do not use it if the packaging is damaged or shows signs of tampering.
Before you start to take it
Tell your pharmacist or doctor if you are allergic to any of the ingredients listed at the end of this leaflet.
Tell your pharmacist or doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your pharmacist or doctor if you are pregnant or intend to become pregnant. This medicine is not recommended to be used during pregnancy. Your pharmacist or doctor will discuss the risks and benefits of taking it if you are pregnant.
Tell your pharmacist or doctor if you are breastfeeding or planning to breastfeed. Small amounts of the drug pass into the breast milk. Your pharmacist or doctor will discuss the risks and benefits of taking it if you are breastfeeding or planning to breastfeed.
Tell your pharmacist or doctor if you have or have had any of the following medical conditions:
- high blood pressure
- hyperthyroidism (overactive thyroid gland)
- diabetes including diabetes mellitus
- heart disease and poor blood flow in the blood vessels of the heart
- glaucoma (high pressure in the eyes)
- prostate problems (including prostatic hypertrophy)
- liver or kidney disease
- hyperreactivity or sensitivity to ephedrine.
Tell your pharmacist or doctor if you plan to have surgery.
If you have not told your pharmacist or doctor about any of the above, tell them before you take this medicine.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you buy without a prescription from your pharmacy, supermarket or health food store.
Some medicines and Telfast Decongestant may interfere with each other. These include medicines used to treat:
- depression
- high blood pressure
- heart conditions
- urinary tract infections and bladder problems
- behavioural disorders
- congestion (phenylephrine)
and - appetite suppressants.
These medicines may be affected by Telfast Decongestant, or may affect how well it works. You may need to use different amounts of your medicine or you may need to take different medicines. Your pharmacist or doctor will advise you.
Your pharmacist or doctor has more information on medicines to be careful with or to avoid while taking this medicine.
How to take Telfast Decongestant
How much to take
Your pharmacist or doctor will tell you how much Telfast Decongestant you should take.
The recommended dose for adults and children over the age of 12 years, is one tablet 12 hourly.
Do not take more than the dose your pharmacist or doctor has directed.
Talk to your doctor or pharmacist if you are unsure what dose to take. The dosage directed by your pharmacist or doctor may be different to the recommended dose.
How to take it
Telfast Decongestant should be swallowed whole with a full glass of water, and be taken before a meal.
When to take it
Take the dose before a meal and ensure that you take the dose at about the same time each day.
If you forget to take it
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Otherwise, take it as soon as you remember, and then go back to taking it as you would normally.
Do not take a double dose to make up for the dose that you missed. This may increase the chance of you getting an unwanted side effect.
If you are not sure what to do, ask your pharmacist or doctor. If you have trouble remembering when to take your medicine, ask your pharmacist for some hints.
If you take too much (overdose)
Immediately telephone your doctor, or the Poisons Information Centre (telephone Australia 13 11 26), or go to Accident and Emergency at your nearest hospital, if you think you or anyone else may have taken too much Telfast Decongestant. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
While you are taking Telfast Decongestant
Things you must do
Talk to your pharmacist or doctor if your symptoms do not improve. Your pharmacist or doctor will assess your condition and decide if you should continue to take the medicine.
Tell all the doctors, dentists and pharmacists who are treating you that you are taking Telfast Decongestant.
If you are about to be started on any new medicine, tell your pharmacist or doctor that you are taking Telfast Decongestant.
If you plan to have surgery that needs a general anaesthetic, tell your doctor or dentist that you are taking this medicine.
If you become pregnant while you are taking this medicine, stop taking it and tell your pharmacist or doctor immediately.
Things you must not do
Do not take more than the recommended dose unless your pharmacist or doctor tells you to.
Do not give this medicine to anyone else, even if they have the same condition as you.
Do not take Telfast Decongestant to treat any other complaints unless your pharmacist or doctor tells you to.
Things to be careful of
Be careful driving or operating machinery until you know how this medicine affects you. This medicine may cause dizziness or light-headedness in some people, if this happens, do not drive or operate machinery. Make sure you know how you react to it before you drive a car, operate machinery, or do anything else that could be dangerous if you are dizzy.
Be careful if you are elderly, unwell or taking other medicines. Some people may experience side effects such as drowsiness, confusion, dizziness and unsteadiness, which may increase the risk of a fall.
Things to be careful of
After the active ingredient is absorbed into your body, you may see the empty tablet shell in your faeces (bowel motions). This is normal and does not affect the way Telfast Decongestant works.
Side Effects
Tell your pharmacist or doctor as soon as possible if you do not feel well while you are taking Telfast Decongestant. This medicine helps most people with allergic rhinitis (hayfever) and sinus/nasal congestion, but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects.
Ask your pharmacist or doctor to answer any questions you may have.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Tell your pharmacist or doctor if you notice any of the following and they worry you:
- headache
- nausea
- fatigue
- dry mouth
- anorexia
- drowsiness
- difficulty sleeping
- nervousness
- excitability
- restlessness
- dizziness
- fear or anxiety
- rapid heart beat
- tremor
- hallucinations.
The above list includes the more common side effects of your medicine. They are usually mild and short-lived.
Children and people over 65 years of age may have an increased chance of getting side effects.
Tell your pharmacist or doctor immediately, or go to Accident and Emergency at your nearest hospital if you notice any of the following:
- urine retention
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
The above list includes very serious side effects. If you have them, you may have had a serious allergic reaction to Telfast Decongestant. You may need urgent medical attention or hospitalisation. These side effects are very rare.
Other side effects not listed above may also occur in some patients. Tell your pharmacist or doctor if you notice anything else that is making you feel unwell.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
After taking Telfast Decongestant
Storage
Keep your tablets in the original pack until it is time to take them. If you take the tablets out of the box or blister pack they may not keep well.
Keep it in a cool, dry place where the temperature stays below 25 degrees C.
Do not store Telfast Decongestant or any other medicine in the bathroom or near a sink.
Do not leave it in the car or on window sills. Heat and dampness can destroy some medicines.
Keep it where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your pharmacist or doctor tells you to stop taking Telfast Decongestant, or it has passed its expiry date, ask your pharmacist what to do with any that are left over.
Product Description
What it looks like
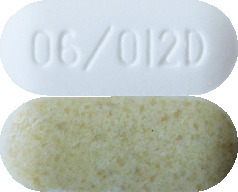
Telfast Decongestant tablets have two layers, are capsule shaped, film coated tablets. One half of the tablet is off white and the other half is tan in colour. The off white half of the tablet is marked with "06/012D".
Telfast Decongestant tablets are available in packs of 6 tablets.
Ingredients
Active Ingredient
Telfast Decongestant contains 60mg of fexofenadine hydrochloride and 120mg of pseudoephedrine hydrochloride as the active ingredients per tablet.
Inactive Ingredients
The tablets also contain:
- cellulose
- maize starch
- croscarmellose sodium
- magnesium stearate
- carnauba wax
- stearic acid
- silica
- opadry film coat.
Distributor
Telfast Decongestant is supplied in Australia by:
Aventis Pharma Pty Limited
27 Sirius Road
LANE COVE NSW 2066
Telfast Decongestant tablets:
AUST R 72552
This leaflet was prepared in November 2014.
® Registered Trademark
telfast-d-ccdsv6-cmiv3-03nov14
Published by MIMS May 2015

 The molecular formula is C32H39NO4.HCl and the molecular weight is 538.13.
The molecular formula is C32H39NO4.HCl and the molecular weight is 538.13. The molecular formula is C10H16ClNO and the molecular weight is 201.69.
The molecular formula is C10H16ClNO and the molecular weight is 201.69.