What is in this leaflet
This leaflet answers some common questions about Voltaren tablets and suppositories. It does not contain all the available information. It does not take the place of talking to your doctor or pharmacist.
The information in this leaflet was last updated on the date listed on the final page. More recent information on the medicine may be available.
You should ensure that you speak to your pharmacist or doctor to obtain the most up to date information on the medicine. You can also download the most up to date leaflet from www.novartis.com.au. Those updates may contain important information about the medicine and its use of which you should be aware.
All medicines have risks and benefits. Your doctor has weighed the risks of you using this medicine against the benefits they expect it will provide.
If you have any concerns about this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What Voltaren is used for
Voltaren belongs to a group of medicines called non-steroidal anti-inflammatory drugs (NSAIDs), which are used to treat pain and reduce inflammation (swelling and redness).
Voltaren is used to treat:
- different types of arthritis including rheumatoid arthritis and osteoarthritis
- other painful conditions where swelling is a problem such as back pain, rheumatism, muscle strains, sprains and tendonitis (e.g. tennis elbow)
- menstrual cramps (period pain)
- relieve pain in children after they have had an operation.
It can relieve the symptoms of pain and inflammation but it will not cure your condition.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another purpose.
Voltaren is only available with a doctor's prescription. It is not addictive.
Voltaren suppositories should not be used in children under 12 months of age. Because of their strength, Voltaren 100mg suppositories are not suitable for children and adolescents.
There is not enough information to recommend the use of Voltaren tablets in children.
Before you use Voltaren
When you must not use it
Do not use Voltaren if you are allergic (hypersensitive) to:
- diclofenac (the active ingredient in Voltaren) or any of the other ingredients listed at the end of this leaflet
- other medicines containing diclofenac (e.g. Voltaren Rapid tablets, Voltaren Emulgel)
- aspirin
- ibuprofen
- any other NSAID
If you are not sure if you are taking any of the above medicines, ask your doctor or pharmacist.
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue, throat, and/or extremities (signs of angioedema)
- rash, itching or hives on the skin.
Many medicines used to treat headache, period pain and other aches and pains contain aspirin or NSAID medicines. If you are allergic to aspirin or NSAID medicines and you use Voltaren, these symptoms may be severe.
Do not use Voltaren if you have had any of the following medical conditions:
- a stomach or intestinal ulcer
- bleeding from the stomach or bowel (symptoms of which may include blood in your stools or black stools)
- kidney or liver problems
- severe heart failure
- heart bypass surgery
Do not use Voltaren suppositories if you suffer from inflammation of the rectum (back passage) or if your rectum is painful (sometimes with bleeding or discharge).
Do not use Voltaren during the first 6 months of pregnancy, except on doctor's advice. Do not use during the last three months of pregnancy. Use of this medicine during the last 3 months of pregnancy may affect your baby and may delay labour and birth.
Use of non-aspirin NSAIDs can increase the risk of miscarriage, particularly when taken close to the time of conception.
Do not use Voltaren after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. In that case, return it to your pharmacist.
Before you start to use it
Tell your doctor if you have any of the following health problems / medical conditions:
- established disease of the heart or blood vessels (also called cardiovascular disease, including uncontrolled high blood pressure, congestive heart failure, established ischemic heart disease, peripheral arterial disease or atherosclerotic cardiovascular disease), as treatment with Voltaren is generally not recommended
- established cardiovascular disease (see above) or significant risk factors such as high blood pressure, abnormally high levels of fat (cholesterol, triglycerides) in your blood, diabetes, or if you smoke, and your doctor decides to prescribe Voltaren, you must not increase the dose above 100 mg per day if you are treated for more than 4 weeks.
- a past history of ulcers (stomach or intestinal)
- gastrointestinal problems such as stomach ulcer, bleeding or black stools, or have experienced stomach discomfort or heartburn after taking anti-inflammatory medicines in the past
- diseases of the bowel or inflammation of the intestinal tract (Crohn's disease) or colon (ulcerative or ischemic colitis)
- past history of haemorrhoids (piles) or irritation of the rectum (back passage)
- liver or kidney problems
- a rare liver condition called porphyria
- bleeding disorders or other blood disorders (e.g. anaemia)
- asthma or any other chronic lung disease that causes difficulty in breathing
- hay fever (seasonal allergic rhinitis)
- repeated chest infections
- polyps in the nose
- diabetes
- dehydration (e.g. by sickness, diarrhoea, before or after recent major surgery
- swollen feet
Your doctor may want to take special precautions if you have any of the above conditions.
It is generally important to take the lowest dose of Voltaren that relieves your pain and/or swelling and for the shortest time possible in order to keep your risk for cardiovascular side effects as small as possible.
Tell your doctor if you are pregnant or trying to become pregnant. There is not enough information to recommend the use of Voltaren during the first 6 months of pregnancy and it must not be used during the last 3 months. Voltaren may also reduce fertility and affect your chances of becoming pregnant. Your doctor can discuss with you the risks and benefits involved.
Tell your doctor if you currently have an infection. If you use Voltaren while you have an infection, some of the signs of the infection such as pain, fever, swelling and redness may be hidden. You may think, mistakenly, that you are better or that the infection is not serious.
Tell your doctor if you are breast-feeding. Breast-feeding is not recommended while you are using this medicine. The active ingredient in Voltaren passes into breast milk and may affect your baby.
Tell your doctor if you are lactose intolerant. Voltaren tablets contain lactose.
Tell your doctor if you are allergic to any other medicines, foods, dyes or preservatives. Your doctor will want to know if you are prone to allergies, especially if you get skin reactions with redness, itching or rash.
Taking other medicines
Tell your doctor if you are taking any other medicines, including any that you buy without a prescription from a pharmacy, supermarket or health food shop.
Some medicines that are important to mention include:
- other anti-inflammatory medicines, e.g. aspirin, salicylates or ibuprofen
- warfarin or other "blood thinners" (medicines used to prevent blood clotting)
- digoxin (a medicine for heart problems)
- lithium or selective serotonin-reuptake inhibitors (SSRIs), a medicine used to treat some types of depression
- diuretics (medicines used to increase the amount of urine)
- ACE inhibitors or beta-blockers (medicines used to treat high blood pressure, heart conditions, glaucoma and migraine)
- prednisone, cortisone, or other corticosteroids (medicines used to provide relief for inflamed areas of the body)
- medicines (such as metformin) used to treat diabetes, except insulin
- methotrexate (a medicine used to treat arthritis and some cancers)
- cyclosporin, tacrolimus (a medicine used in patients who have received organ transplants)
- trimethoprim (a medicine used to prevent or treat urinary tract infections)
- some medicines used to treat infection (quinolone antibacterials)
- glucocorticoid medicines, used to treat arthritis
- sulfinpyrazone (a medicine used to treat gout)
- voriconazole (a medicine used to treat fungal infections)
- phenytoin (a medicine used to treat seizures)
- Rifampicin (an antibiotic medicine used to treat bacterial infections)
You may need to take different amounts of your medicines or to take different medicines while you are using Voltaren. Your doctor and pharmacist have more information.
If you have not told your doctor about any of these things, tell him/her before you start using this medicine.
How to use Voltaren
When to take it
Voltaren Tablets
It is recommended to take the tablets before meals or on an empty stomach. If they upset your stomach, you can take them with food or immediately after food. They will work more quickly if you take them on an empty stomach but they will still work if you have to take them with food to prevent stomach upset.
Voltaren suppositories
Use the suppositories at bedtime to relieve pain during the night and early morning stiffness; or to relieve pain after an operation.
How much Voltaren to take/use
Follow all directions given to you by your doctor and pharmacist carefully. These instructions may differ from the information contained in this leaflet.
If you do not understand the instructions on the label, ask your doctor or pharmacist for help.
There are different ways to take Voltaren tablets and suppositories, depending on your condition. Your doctor will tell you exactly how many tablets or suppositories to take.
Do not exceed the recommended dose.
To treat arthritis or other painful conditions
The usual starting dose of Voltaren tablets is 75mg to 150mg each day. After the early stages of treatment, it is usually possible to reduce the dose to 75mg to 100mg each day.
To treat menstrual cramps (period pain)
The tablets are usually taken during each period as soon as cramps begin and continued for a few days until the pain goes away.
The usual starting dose of Voltaren tablets is 50mg to 100mg each day, beginning as soon as cramps begin and continuing until the pain goes away, but for no longer than 3 days.
If necessary, the dose can be raised over several menstrual periods to a maximum of 200mg each day.
To treat post-operative pain in children
Your doctor will advise what strength and dose of Voltaren suppositories is suitable for your child.
How to take the tablets
Voltaren tablets are usually taken in 2 or 3 doses during the day.
Swallow the tablets whole with a full glass of water or other liquid. Do not chew them. The tablets have a special coating to keep them from dissolving until they have passed through the stomach into the bowel. Chewing the tablets would destroy the coating.
How to use Voltaren suppositories
Do not take suppositories by mouth.
When used in children, the strength of the Voltaren suppository used depends on the weight of the child. Your doctor will decide which strength is suitable for your child and how often it can be used.
If possible, go to the toilet and empty your bowels before using the suppository.
Follow these steps:
- Wash your hands thoroughly with soap and water.
- If the suppository feels soft, chill it before removing the wrapper by placing it in the fridge or holding it under cold water for a few minutes.
- Put on a disposable glove, if desired (available from a pharmacy).
- Remove the entire wrapper from the suppository.
- Moisten the suppository by dipping it briefly in cool water.
- Lie on your side and raise your knees to your chest.
- Push the suppository, blunt end first, gently into your rectum (back passage). Do not break the suppository.
- Remain lying down for a few minutes so that the suppository dissolves.
- Wash your hands again thoroughly.
Try not to go to the toilet to empty your bowels for at least one hour after using the suppository.
If you are not sure how to use a suppository, ask your pharmacist or doctor.
How long to take/use it
Do not use Voltaren for longer than your doctor says.
If you are using Voltaren for arthritis, it will not cure your disease but it should help to control pain and inflammation. It usually begins to work within a few hours but several weeks may pass before you feel the full effects of the medicine.
Voltaren suppositories should not be used for more than 3 days in children.
If you forget to take/use it
If it is almost time for your next dose (e.g. within 2 or 3 hours), skip the dose you missed and take the next dose when you are meant to.
Otherwise, take it as soon as you remember, and then go back to taking it as you would normally.
Do not take a double dose to make up for the one that you missed. This may increase the chance of you getting an unwanted side effect.
If you have trouble remembering when to take your medicine, ask your pharmacist for some hints.
If you take/use too much Voltaren (Overdose)
Immediately telephone your doctor or Poisons Information Centre (telephone 13 11 26), or go to Accident and Emergency at your nearest hospital if you think that you or anyone else may have used too much Voltaren. Do this even if there are no signs of discomfort or poisoning. Keep the telephone numbers for these places handy.
If you take too much Voltaren, you may experience:
- vomiting
- bleeding from the stomach or bowel
- diarrhoea
- dizziness
- ringing in the ears
- convulsions (fits)
While you are taking/ using Voltaren
Things you must do
If you take Voltaren for more than a few weeks, you should make sure to visit your doctor for regular check-ups to ensure that you are not suffering from unnoticed undesirable effects.
If you become pregnant whilst taking or using Voltaren, tell your doctor immediately. Your doctor can discuss with you the risks of using it while you are pregnant.
Be sure to keep all of your doctor's appointments so that your progress can be checked. Your doctor will periodically re-evaluate whether you should continue treatment with Voltaren, if you have established heart disease or significant risks for heart disease, especially in case you are treated for more than 4 weeks.
Your doctor may want to check your kidneys, liver and blood from time to time to help prevent unwanted side effects.
If, at any time while taking Voltaren you experience any signs or symptoms of problems with your heart or blood vessels such as chest pain, shortness of breath, weakness, or slurring of speech, contact your doctor immediately. These may be signs of cardiovascular toxicity.
If you are going to have surgery, make sure the surgeon and anaesthetist know that you are using Voltaren. NSAID medicines can slow down blood clotting and affect kidney function.
If you get an infection while using Voltaren, tell your doctor. This medicine may hide some of the signs of an infection (pain, fever, swelling, redness). You may think, mistakenly, that you are better or that the infection is not serious.
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are using Voltaren.
Tell any other doctor, dentist or pharmacist who treats you that you are using Voltaren.
Things you must not do
Do not take any of the following medicines while you are using Voltaren without first telling your doctor:
- aspirin (also called ASA or acetylsalicylic acid)
- other salicylates
- other medicines containing diclofenac (e.g. Voltaren Rapid tablets, Voltaren Emulgel)
- ibuprofen
- any other NSAID medicine
If you take these medicines together with Voltaren, they may cause unwanted side effects.
If you need to take something for headache or fever, it is usually okay to take paracetamol. If you are not sure, your doctor or pharmacist can advise you.
Do not stop any other forms of treatment for arthritis that your doctor has told you to follow. This medicine does not replace exercise or rest programs or the use of heat/cold treatments.
Do not give this medicine to anyone else, even if their condition seems similar to yours.
Do not use it to treat any other complaints unless your doctor tells you to.
Things to be careful of
Be careful driving, operating machinery or doing jobs that require you to be alert until you know how Voltaren affects you. This medicine may cause dizziness, drowsiness, spinning sensation (vertigo) or blurred vision in some people. If you have any of these symptoms, do not drive, use machines, or do anything else that could be dangerous.
Elderly patients should take the minimum number of tablets or suppositories that provides relief of symptoms. Elderly patients, especially those with a low body weight, may be more sensitive to the effects of Voltaren than other adults.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are using Voltaren.
All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical treatment if you get some of the side effects.
If you are over 65 years old, you should be especially careful while taking this medicine. Report any side effects promptly to your doctor. As people grow older, they are more likely to get side effects from medicines.
Do not be alarmed by these lists of possible side effects. You may not experience any of them.
Ask your doctor or pharmacist to answer any questions you may have.
Tell your doctor if you notice any of the following and they worry you:
- stomach upset including nausea (feeling sick), vomiting, indigestion, cramps, loss of appetite, wind
- heartburn or pain behind or below the breastbone (possible symptoms of an ulcer in the tube that carries food from the throat to the stomach)
- stomach or abdominal pain
- constipation, diarrhoea
- sore mouth or tongue
- altered taste sensation
- headache
- dizziness, spinning sensation
- drowsiness, disorientation, forgetfulness
- feeling depressed, anxious or irritable
- strange or disturbing thoughts or moods
- shakiness, sleeplessness, nightmares
- tingling or numbness of the hands or feet
- feeling of fast or irregular heart beat
- unusual weight gain or swelling of arms, hands, feet, ankles or legs due to fluid build-up
- symptoms of sunburn (such as redness, itching, swelling, blistering of the lips, eyes, mouth, and/or skin) that happen more quickly than normal
- skin inflammation with flaking or peeling
- vision disorders* (e.g. blurred or double vision)
- buzzing or ringing in the ears, difficulty hearing
- hypertension (high blood pressure)
- hair loss or thinning
- application site irritation, painful rectum or discomfort in the rectum (back passage) or worsening of haemorrhoids (piles) when using the suppositories
NSAIDs, including diclofenac, may be associated with increased risk of gastro-intestinal anastomotic leak. Close medical surveillance and caution are recommended when using this medicine after gastrointestinal surgery.
*If symptoms of vision disorders occur during treatment with Voltaren, contact your doctor as an eye examination may be considered to exclude other causes.
If any of the following signs appear, tell your doctor immediately or go to Accident and Emergency at your nearest hospital:
- red or purple skin (possible signs of blood vessel inflammation)
- severe pain or tenderness in the stomach, vomiting blood or material that looks like coffee grounds, bleeding from the back passage, black sticky bowel motions (stools) or bloody diarrhoea (possible stomach problems)
- rash, skin rash with blisters, itching or hives on the skin; swelling of the face, lips, mouth, tongue, throat, or other part of the body which may cause difficulty to swallow, low blood pressure (hypotension), fainting, shortness of breath (possible allergic reaction)
- wheezing, troubled breathing, or feelings of tightness in the chest (signs of asthma)
- yellowing of the skin and/or eyes (signs of hepatitis/liver failure)
- persistent nausea, loss of appetite, unusual tiredness, vomiting, pain in the upper right abdomen, dark urine or pale bowel motions (possible liver problems)
- constant "flu-like" symptoms including chills, fever, sore throat, aching joints, swollen glands, tiredness or lack of energy, bleeding or bruising more easily than normal (possible blood problem)
- painful red areas, large blisters, peeling of layers of skin, bleeding in the lips, eyes, mouth, nose or genitals, which may be accompanied by fever and chills, aching muscles and feeling generally unwell (possible serious skin reaction)
- signs of a possible effect on the brain, such as sudden and severe headache, stiff neck (signs of viral meningitis), severe nausea, dizziness, numbness, difficulty in speaking, paralysis (signs of cerebral attack), convulsions (fits)
- change in the colour or amount of urine passed, frequent need to urinate, burning feeling when passing urine, blood or excess of protein in the urine (possible kidney disorders)
- sudden and oppressive chest pain (which may be a sign of myocardial infarction or a heart attack)
- breathlessness, difficulty breathing when lying down, swelling of the feet or legs (signs of cardiac failure)
- Coincidental occurrence of chest pain and allergic reactions (signs of Kounis syndrome)
Tell your doctor if you notice anything else that is making you feel unwell. Some people may have other side effects not yet known or mentioned in this leaflet.
After using Voltaren
Storage
- Keep your medicine in the original container until it is time to use it.
- Store it in a cool dry place.
- Do not store Voltaren or any other medicine in the bathroom or near a sink.
- Do not leave it in the car or on window sills.
Keep the medicine where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop using Voltaren or the expiry date has passed, ask your pharmacist what to do with any medicine you have left over.
Product description
What it looks like
Voltaren tablets
Voltaren 25mg tablets are round, yellow, coated tablets marked "CG" on one side and "BZ" on the other side; blisters of 50.
Voltaren 50mg tablets are round, pale brown, coated tablets marked "CG" on one side and "GT" on the other side; blisters of 50.
Voltaren suppositories
Voltaren suppositories are yellowish-white, torpedo shaped suppositories. The 100mg strength is in packs of 20 and the lower strength suppositories are in packs of 10.
Ingredients
Voltaren tablets
Contain 25mg or 50mg diclofenac sodium as the active ingredient in gastro-resistant tablets.
The tablets also contain:
- silica colloidal anhydrous
- microcrystalline cellulose (E460)
- lactose
- magnesium stearate (E572)
- maize starch
- povidone (E1201)
- hypromellose (E463)
- iron oxide yellow CI77492 (E172)
- iron oxide red CI77491 (50mg tablet only) (E172)
- titanium dioxide (E171)
- sodium starch glycolate
- purified talc (E553b)
- macrogol 8000
- PEG-40 hydrogenated castor oil
- acrylates copolymer
Voltaren tablets do not contain sucrose, gluten, tartrazine or any other azo dyes.
Voltaren suppositories
Contain either 12.5mg, 25mg, 50mg or 100mg diclofenac sodium as the active ingredient in a triglyceride base.
Voltaren suppositories do not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
Sponsor
Voltaren is supplied in Australia by:
NOVARTIS Pharmaceuticals Australia Pty Limited
ABN 18 004 244 160
54 Waterloo Road
Macquarie Park NSW 2113
Telephone: 1800 671 203
®= Registered Trademark
This leaflet was prepared in October 2019.
Australian Registration Numbers:
25mg tablet blister AUST R 166496
50mg tablet blister AUST R 66880
12.5mg suppository AUST R 96797
25mg suppository AUST R 96810
50mg suppository AUST R 96811
100mg suppository AUST R 37582
(vlt030123c) based on PI (vlt030123i)
Published by MIMS February 2023






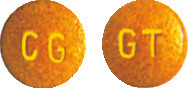
 Chemical name: sodium-[O-[(2,6-dichlorophenyl)-amino] phenyl]-acetate.
Chemical name: sodium-[O-[(2,6-dichlorophenyl)-amino] phenyl]-acetate.