What is in this leaflet
This leaflet answers some common questions about this medicine. It does not contain all the available information. It does not take the place of talking to your doctor.
All medicines have risks and benefits. Your doctor has weighed the risks of you taking this medicine against the benefits they expect it will have for you.
If you have any concerns about taking this medicine, ask your doctor or pharmacist.
Keep this leaflet with the medicine. You may need to read it again.
What this medicine is used for
The name of your medicine is APO-Zolpidem. It contains the active ingredient, zolpidem tartrate.
Zolpidem is used to treat people with sleeping difficulties (insomnia). It works by binding to special sites in the brain which produce sleep.
Zolpidem must not be used for more than 4 weeks at a time.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed this medicine for another reason.
This medicine is available only with a doctor's prescription.
Use in children
Children or adolescents under the age of 18 must not take this medicine.
Before you take this medicine
When you must not take it
Do not take this medicine if you have an allergy to:
- any medicine containing zolpidem
- any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include:
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin
Do not take this medicine if you have:
- been drinking alcohol or you believe that you may have alcohol in your bloodstream.
- sleep apnoea (a condition where you temporarily stop breathing while you sleep).
- myasthenia gravis (a condition in which the muscles become weak and tire easily).
- severe liver problems
- sudden and/or severe lung problems
- previously experienced complex sleep behaviours after taking this medicine including sleepwalking, sleep-driving, and/or engaging in other activities while not fully awake.
Do not take this medicine if you are pregnant, suspect that you are pregnant or intend to become pregnant. Zolpidem may affect your developing baby if you take it during pregnancy.
Do not take this medicine if you are breastfeeding or plan to breastfeed. Zolpidem passes into breast milk and there is a possibility that your baby may be affected.
Do not take this medicine after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start taking this medicine, talk to your doctor.
Before you start to take it
Tell your doctor if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any of the following medical conditions:
- problems with your heart, liver, kidneys or lungs
- problems breathing or snoring often whilst sleeping
- epilepsy
- depression, schizophrenia or other mental illnesses
- addiction to alcohol, drugs or other medicines.
Tell your doctor if you are pregnant or plan to become pregnant or are breastfeeding. Do not take zolpidem whilst pregnant until you and your doctor have discussed the risks and benefits involved. The safety of taking zolpidem during pregnancy has not been established.
The use of zolpidem whilst breast-feeding is not recommended as it passes into breast milk.
If you have not told your doctor about any of the above, tell them before you start taking this medicine.
Taking other medicines
Tell your doctor or pharmacist if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and zolpidem may interfere with each other. These include:
- medicines to treat depression, anxiety and mental illness such as fluvoxamine
- medicines to treat epilepsy such as barbiturates (also used for sedation)
- pain relievers such as opioids
- muscle relaxants
- antihistamines
- St John's Wort (also known as Hypericum), a herbal remedy used to treat depression
- anaesthetics or any other medicines which may make you sleepy
- rifampicin or ciprofloxacin, medicines to treat infections
- ketoconazole, a medicine to treat antifungal infections.
These medicines may be affected by zolpidem or may affect how well it works i.e. by increasing drowsiness. This may affect your ability to drive a car or operate dangerous machinery. You may need different amounts of your medicines, or you may need to take different medicines.
Your doctor or pharmacist can tell you if you are taking any of these medicines. They may also have more information on medicines to be careful with or avoid while taking zolpidem.
Other interactions not listed above may also occur.
How to take this medicine
Follow carefully all directions given to you by your doctor. They may differ from the information in this leaflet.
If you do not understand any written instructions, ask your doctor or pharmacist for help.
How much to take
This will depend on your condition and whether you are taking any other medicines.
The usual adult dose of zolpidem is 10 mg.
If you are over 65 years of age or debilitated in any way, the usual dose is 5 mg at night.
If you have a liver problem, the usual dose is 5 mg.
Your doctor may have prescribed a different dose. The lowest effective daily dose should be used and must not exceed 10 mg.
How to take it
Swallow the tablets whole with a full glass of water unless your doctor has told you to take half a tablet.
Do not crush or chew the tablets.
When to take it
Zolpidem should only be taken when you are able to get a full night's sleep (7 to 8 hours) before you need to be active and alert again. It should be taken in one dose and not be readministered during the same night.
Take zolpidem immediately before you go to bed or while you are in bed, as it puts you to sleep quite quickly.
It also works more quickly if you take it on an empty stomach.
How long to take it for
Zolpidem should only be used for short periods (treatment should not exceed 4 weeks). Continuous longterm use is not recommended unless advised by your doctor.
If you forget to take it
If you forget to take zolpidem before you go to bed, and you wake up late in the night or very early in the morning, do not take it. If you take it later than normal, you may have trouble waking at your normal time.
Do not take a double dose to make up for missed doses. This may increase the chance of you experiencing side effects.
If you have trouble remembering to take your medicine, ask your pharmacist for some hints to help you remember.
If you take too much (overdose)
Immediately telephone your doctor or the Poisons Information Centre (telephone 13 11 26) for advice or go to Accident and Emergency at the nearest hospital, if you think that you or anyone else may have taken too much of this medicine. Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
If you take too much zolpidem your consciousness may be impaired (ranging from drowsiness to light coma) and can be fatal.
While you are taking this medicine
Things you must do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking this medicine.
Tell any other doctors, dentists, and pharmacists who treat you that you are taking this medicine.
If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine. It may affect other medicines used during surgery.
If you become pregnant while taking this medicine, tell your doctor immediately.
If you are about to have any blood tests, tell your doctor that you are taking this medicine. Zolpidem may interfere with the results of some tests.
If the tablets have not started to work after 7 to 14 days, go to your doctor to discuss what to do next.
Things you must not do
Do not give this medicine to anyone else, even if they have the same condition as you.
Do not take this medicine to treat any other condition unless your doctor tells you to.
Do not stop taking your medicine suddenly, or change the dosage, without first checking with your doctor. If you stop taking this medicine suddenly, there is a chance that your original symptoms of sleeplessness may become worse, or you get withdrawal symptoms such as muscle pain, sensitivity to light, touch or sound, headache, anxiety, tension, restlessness, confusion, strange thoughts, numbness, tingling, mood changes, irritability or, feeling not part of your body.
Do not drink alcohol before, during or immediately after taking this medicine. This can increase the risk of side effects.
Things to be careful of
Because zolpidem will make you sleepy or affect your alertness and response time, you should not operate dangerous machinery or drive motor vehicles for at least 8 hours after you take it. You should also be careful the next morning when you wake up. Make sure you know how you react to zolpidem before you drive a car or operate machinery. This is especially important if you drink alcohol or are taking other drugs that also make you drowsy, because they may make you even drowsier when taken with zolpidem.
Be careful if you are over the age of 65, unwell or debilitated in some way, or taking other medicines. You may be more sensitive to some of the side effects of zolpidem.
You must not have alcohol in your bloodstream while you are taking zolpidem. The effects of alcohol could be made worse while taking zolpidem.
Side effects
Tell your doctor as soon as possible if you do not feel well while you are taking zolpidem or if you have any questions or concerns.
All medicines can have side effects. Sometimes they are serious but most of the time they are not.
Do not be alarmed by the following lists of side effects. You may not experience any of them.
Tell your doctor if you notice any of the following and they worry you:
- drowsiness
- dizziness
- headache
- fatigue
- worsened insomnia
- nightmares
- hallucinations
- agitation
- temporary amnesia
- diarrhoea, nausea and vomiting
- abdominal pain
- muscle weakness
- sensation of pins and needles, or numbness
- infections of the nose throat and chest
- double or blurred vision
- change in appetite.
Tell your doctor as soon as possible if you notice any of the following. These may be serious side effects and you may need medical attention:
Unexpected changes in behaviour, such as anger, aggression or rage, worsened insomnia, nightmares, confusion, agitation, restlessness, irritability, stimulation, excitement, hallucinations, delusions, suicidal thoughts or attempts, and other forms of unwanted behaviour.
Alcohol can increase the risk of sleep walking and other related behaviours. These side effects can also occur without the presence of alcohol intake.
Although these side effects can occur at the dosage prescribed by your doctor, there is an increased risk of side effects if you take more than the recommended dose.
Some sleep medicines may cause short-term memory loss. When this occurs, a person may not remember what has happened for several hours after taking the medicine. This is usually not a problem since most people fall asleep after taking the medicine.
Dependence
Sleep medicines should, in most cases, be used only for short periods of time. If your sleep problems continue, consult your doctor.
Some sleep medicines can cause dependence, especially when they are used regularly for longer than a few weeks. People who have been dependent on alcohol or other drugs in the past may have a higher chance of becoming addicted to sleep medicines. If you have been addicted to alcohol or drugs in the past, it is important to tell your doctor before starting zolpidem.
If any of the following happen, stop taking this medicine and tell your doctor immediately, or go to Accident and Emergency at your nearest hospital:
- Sleep walking, driving motor vehicles and other unusual, and on some occasions, dangerous behaviours whilst apparently asleep. These have also included preparing and eating food, making phone calls or having sexual intercourse. People experiencing these effects have had no memory of the events
- symptoms of an allergic reaction including cough, shortness of breath, wheezing or difficulty breathing; swelling of the face, lips, tongue, throat or other parts of the body; rash, itching or hives on the skin.
These are very serious side effects. If you have them, you may need urgent medical attention or hospitalisation.
Withdrawal Symptoms
Sometimes when medicines are stopped suddenly, after being used for a long time, withdrawal symptoms may occur. Symptoms of withdrawal may include muscle pain, sensitivity to light, touch or sound, headache, anxiety, tension, restlessness, confusion, strange thoughts, numbness, tingling, mood changes, irritability or feeling not part of your body.
In some cases, your insomnia may appear worse for a short time which may be accompanied with other reactions including mood changes, anxiety and restlessness.
Let your doctor know if you have any problems when you stop taking zolpidem.
Tell your doctor or pharmacist if you notice anything that is making you feel unwell.
Other side effects not listed above may also occur in some people.
Storage and disposal
Storage
Keep your medicine in its original packaging until it is time to take it. If you take your medicine out of its original packaging it may not keep well.
Keep your medicine in a cool dry place where the temperature will stay below 30°C.
Do not store your medicine, or any other medicine, in the bathroom or near a sink. Do not leave it on a window sill or in the car. Heat and dampness can destroy some medicines.
Keep this medicine where children cannot reach it. A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Disposal
If your doctor tells you to stop taking this medicine or it has passed its expiry date, your pharmacist can dispose of the remaining medicine safely.
Product description
What APO-Zolpidem looks like
5 mg tablets: Pink, capsule-shaped, film-coated tablets, imprinted "APO" on one side and "ZOL 5" on the other side.
Packs of 7 and 14 tablets.
AUST R 127151. AUST R 127167.
10 mg tablets: White, modified oval, scored tablets, imprinted "APO" on one side and "1" European bisect "0"on the other side.
Packs of 7 and 14 tablets.
AUST R 127174. AUST R 127178.
* Not all strengths, pack types and/or pack sizes may be available.
Ingredients
Each tablet contains 5 or 10 mg of the active ingredient, zolpidem tartrate.
It also contains the following inactive ingredients:
- microcrystalline cellulose
- sodium starch glycollate
- magnesium stearate
- hypromellose
- hyprolose
- macrogol 8000
- titanium dioxide
- iron oxide red (CI77491) (5 mg only).
This medicine is gluten-free, lactose-free, sucrose-free, tartrazine-free and free of other azo dyes.
Sponsor
Apotex Pty Ltd
16 Giffnock Avenue
Macquarie Park NSW 2113
APO and APOTEX are registered trade marks of Apotex Inc.
This leaflet was last updated in: May 2020.
Published by MIMS July 2020


 Table 2 was derived from a pool of three placebo controlled long-term efficacy trials involving zolpidem (zolpidem tartrate). These trials involved patients with chronic insomnia who were treated for 28 to 35 nights with zolpidem at doses of 5, 10 or 15 mg. The table is limited to data from doses up to and including 10 mg, the highest dose recommended for use. The table includes only adverse events occurring at an incidence of at least 1% for zolpidem patients.
Table 2 was derived from a pool of three placebo controlled long-term efficacy trials involving zolpidem (zolpidem tartrate). These trials involved patients with chronic insomnia who were treated for 28 to 35 nights with zolpidem at doses of 5, 10 or 15 mg. The table is limited to data from doses up to and including 10 mg, the highest dose recommended for use. The table includes only adverse events occurring at an incidence of at least 1% for zolpidem patients.
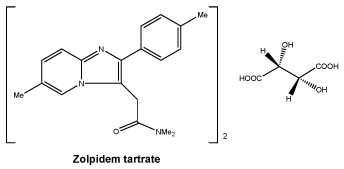 Chemical name: (bis[N,N-dimethyl-2-[6-methyl-2-(4-methylphenyl) imidazo[1,2-a]pyridin-3-yl]acetamide] (2R,3R)-2,3-dihydroxybutanedioate).
Chemical name: (bis[N,N-dimethyl-2-[6-methyl-2-(4-methylphenyl) imidazo[1,2-a]pyridin-3-yl]acetamide] (2R,3R)-2,3-dihydroxybutanedioate).