How common is anxiety disorder?
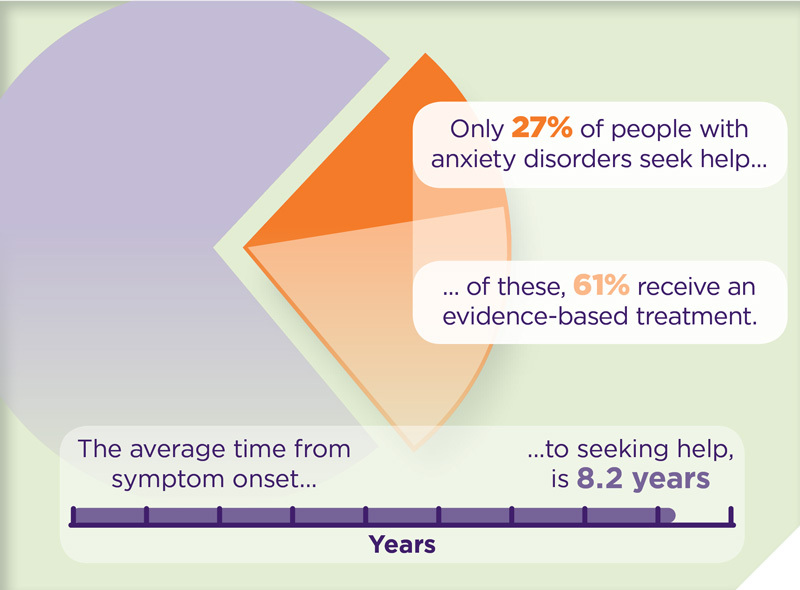
Around 14% of Australians aged 16–85 years are affected by anxiety disorders.1 However, only 27% of the people with an anxiety disordera seek help, and of these, 61% receive evidence-based treatment.2
Cognitive behavioural therapy (CBT; including validated online programs) and selective serotonin reuptake inhibitor (SSRI) medicines are effective for treating anxiety disorders, but it is important to adopt a shared decision-making approach, selecting and tailoring treatment in collaboration with each patient.
Being anxious is a normal response to situations in daily life, making us alert and improving our performance. Anxiety is classified as a disorder if the response:4
- occurs frequently over a long period of time (at least 6 months)
- is out of proportion to the triggering situation, and
- significantly affects everyday functioning.
People with anxiety disorders experience excessive worry and the urge to avoid situations that are the focus of this worry.5
aExcludes people with both anxiety and mood disorders.
Recognising specific anxiety disorders
Specific anxiety disorders have different presentations.5
- People with panic disorder experience sudden attacks of fear or anxiety, often with no obvious trigger, sometimes so severe that they think they may collapse or die.
- People with social anxiety disorder fear social settings and avoid situations where they may be subject to judgement or scrutinisation by others.
- Excessive worry over everyday things and being overly concerned about things that could go wrong is indicative of general anxiety disorder.
Patients may present with multiple anxiety disorders, and anxiety can also be comorbid with depression and other mental health conditions. Although the diagnosis of a specific anxiety disorder should guide treatment, recommended first-line treatments are effective for all anxiety disorders as well as for treating depression.5
Psychological or pharmacological treatment?
CBT and pharmacological treatment with an SSRI are first-line treatments for anxiety disorders. Both are similarly effective, and one out of every two people treated no longer satisfies the criteria for an anxiety disorder after treatment.5
CBT, delivered face-to-face or via the internet, is the psychological treatment with the best evidence of effectiveness for the treatment of anxiety.5 Other psychological treatments (with varying levels of evidence) are also sometimes used.
See Medicinewise News for more information on psychological treatments for anxiety disorders.
SSRIs are first-line pharmacological options for treating anxiety disorders. Serotonin-norepinephrine reuptake inhibitors (SNRIs) and then other medicines may be considered, if SSRIs have been properly trialled and have not been effective.5
The role of benzodiazepines and atypical antipsychotics such as quetiapine is limited because of their adverse safety profile.5
Treatment should be selected in consultation with the patient and choice should be based on efficacy, patient preference, accessibility, cost, tolerability and safety.5
References
- Australian Bureau of Statistics. National Survey of Mental Health and Wellbeing: Summary of Results. 2007 (accessed 14 September 2018).
- Harris MG, Hobbs MJ, Burgess PM, et al. Frequency and quality of mental health treatment for affective and anxiety disorders among Australian adults. Med J Aust 2015;202:185-9.
- Thompson A, Issakidis C, Hunt C. Delay to seek treatment for anxiety and mood disorders in an Australian clinical sample. Behav Change 2008;25:71-84.
- Craske MG, Stein MB. Anxiety. Lancet 2016;388:3048-59.
- Andrews G, Bell C, Boyce P, et al. Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for the treatment of panic disorder, social anxiety disorder, and generalised anxiety disorder. Aust NZ J Psychiatry 2018;52:1109-72.

