Measuring blood pressure
Blood pressure (BP) is dynamic. It can change according to time of day, after eating, or during and after physical activity. Health professionals should follow a best practice approach to minimise possible confounders and increase in-clinic accuracy. This may include using out-of-clinic measurements as well.
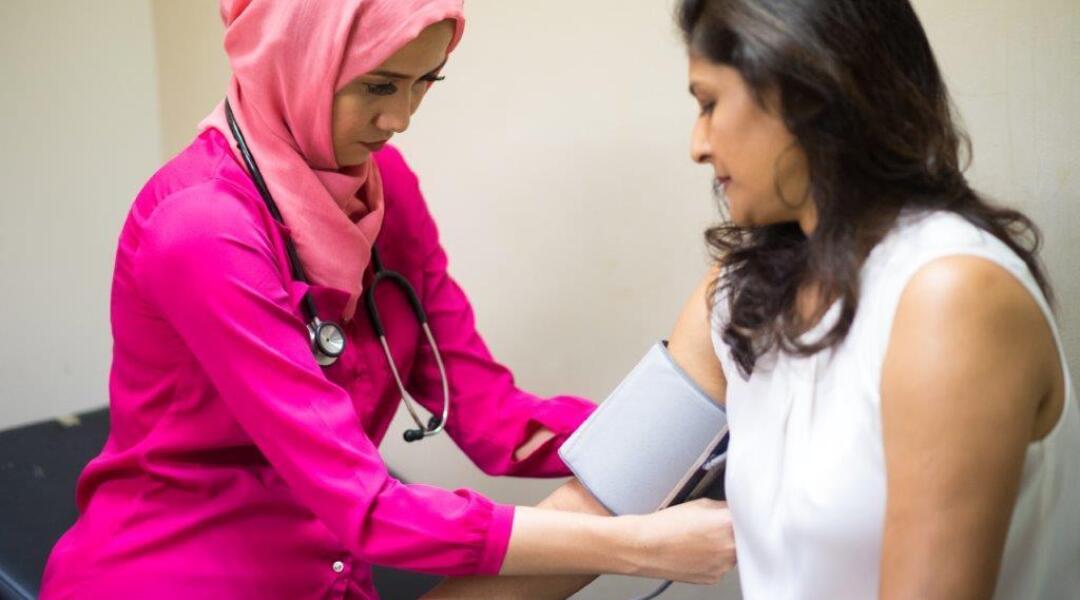
Best practice for in-clinic BP
In-clinic BP measurements are one of the cornerstones of general practice and a key contributor to the assessment of absolute cardiovascular risk.1,2 These values are also important for monitoring a patient's response to BP-lowering therapy.
However in-clinic readings are just a snapshot of an individual's blood pressure and may not accurately reflect a patients underlying BP due to a number of reasons, including:2,3
- inherent variability coupled with small number of BP readings
- poor technique due to common errors (eg, cuff over clothing, incorrect cuff size, device not calibrated)
- patterns of BP such as white coat hypertension, masked hypertension, nocturnal non-dipping.
Establishing a best practice routine for the in-clinic assessment of BP can help minimise confounders such as those described above and increase measurement accuracy.2,3
General principles for in-clinic BP measurements
In-clinic BP can be taken using a variety of methods:
- recording taken by the doctor
- recording taken by a health professional other than a doctor – this has been shown to reduce the white coat effect4
- automatic, non-observed recording by an automated oscillometric device in a seated patient who has been resting alone in a quiet room — this is considered ideal, and may also reduce the white-coat effect.1,2,5
All BP measuring devices should be serviced at least once per year.5
Multiple factors can affect the accuracy of an in-clinic BP measure and the magnitude of the mmHg discrepancy.6
| Technique-related factors (increase in mmHg SBP) | Patient-related factors (increase in mmHg SBP) |
|---|---|
| Cuff over clothing (5–50) | Talking or active listening (10) |
| Cuff too small (10) | Distended bladder (15) |
| Patient back unsupported (6–10) | Smoking or caffeine within 2 hours of measurement (6–20) |
| Patient arm unsupported – sitting (1–7) – standing (6–8) |
To measure in-clinic BP accurately, current guidelines recommend:5,7
- The patient be seated and relaxed – allow them a few minutes to sit quietly and calmly before measuring.
- Multiple measurements taken at different times – at least two measurements on each occasion, and repeated one week or more apart.
- Measuring BP on both arms at the first assessment – if there is a discrepancy of more than 5 mmHg, use the arm with the highest reading for all future readings
- Recording the result for systolic and diastolic BP – repeating the procedure after 30 seconds.
Average the readings. If the first two readings differ by more than 10 mmHg systolic or 6 mmHg diastolic, or if initial readings are high, have the patient rest quietly for 5 minutes then take several readings until consecutive readings do not vary by greater than these amounts.
For automated devices, three measurements should be obtained with the average of the second and third readings recorded.7
Limitations of in-clinic BP measurements
There are many cases where in-clinic measurement cannot accurately determine a person's average BP leading to an overestimation (and potentially over treatment) in some people and underestimation (and hence undertreatment) in others. Taking measurements outside of the clinic, through 24-hour ambulatory BP monitoring (ABPM) or home BP monitoring (HBPM) can help identify these cases and provide clarity around a person's true underlying BP.2,5,8
White coat hypertension
This condition affects around 13% of the population and occurs when a patient meets the threshold for high BP when measured in-clinic, but not when measured out-of-clinic.8 The effect may be more pronounced when BP is being taken by a doctor compared with a practice nurse or other health professional,1,9 and may be attenuated by using a validated automated device while the patient is alone in a quiet room.1
Masked hypertension
This condition also affects around 13% of the population and describes the situation where BP measurements taken in clinic are within 'normal' thresholds, but out-of-clinic measurements reveal elevated BP.8,9
Suspect masked hypertension in patients with known end-organ damage (ie, LVH, microalbuminuria, chronic kidney disease) and in-clinic BP readings that appear to be normal.5
Nocturnal non-dipping
Nocturnal non-dipping is a clinical condition that cannot be detected by in-clinic BP measurements or HBPM.
Nocturnal non-dipping is defined as a drop in BP of < 10% during sleep compared with daytime averages.9 This drop is small and in contrast to the reduction commonly seen in most people during sleep. People experiencing nocturnal non-dipping may have significant end organ damage, autonomic neuropathy or obstructive sleep apnoea.9
Measuring BP outside the clinic
- Out-of-clinic BP readings and treatment targets are often lower than those recorded in the clinic.
- Use of in-clinic measurement to guide management can lead both over- and under-treatment.
- Ambulatory (ABPM) and home (HBPM) blood pressure monitoring provide more reliable measures of BP that better predict CVD risk.
Numerous studies have confirmed the utility of out-of-clinic BP measurements such as 24-hour ambulatory BP monitoring (ABPM) or home BP monitoring (HBPM) as an adjunct to in-clinic recordings.1-3,9
These methods can detect patients with conditions that confound in-clinic measurements (ie white coat hypertension, masked hypertension), and there is substantial evidence that out-of-office measures give a better prediction of risk than in-clinic BP.2,8,10
Ambulatory blood pressure monitoring (ABPM)
In addition to confirming BP elevations and ongoing monitoring of patients being treated with BP lowering medicines,7,11 ABPM may also be useful for:5,7,9,12
- suspected white coat hypertension or masked hypertension
- suspected nocturnal hypertension or non-dipping
- tailoring BP lowering medicines
- measuring BP in patients with sleep apnoea
- identifying high BP resistant to appropriate treatment
- detecting high BP during early pregnancy
- identifying orthostatic hypotension (eg, syncope).
Home blood pressure monitoring (HBPM)
Australian guidelines currently endorse the use of HBPM5 and provide advice on how to ensure accuracy, but there is limited advice on how to implement home BP monitoring into practice.5,8,13
It has been suggested that self measurement with HBPM can help patients to better understand their high blood pressure, as it is generally an asymptomatic risk factor, and also see the effects positive lifestyle and medicines can have on BP readings.5
Ensuring accurate HBPM readings
To optimise the clinical value and accuracy of HBPM measurements:5
- ensure the device used is validated, serviced regularly and re-calibrated every 6 months
- provide practical instruction to the patient to ensure good self-measurement technique
- supply written instructions for reference at home
- follow-up reassessment to ensure correct technique
References
- Myers MG, Godwin M, Dawes M, et al. Measurement of blood pressure in the office: recognizing the problem and proposing the solution. Hypertension 2010;55:195–200. [Pubmed]
- Pickering TG, White WB, Giles TD, et al. When and how to use self (home) and ambulatory blood pressure monitoring. J Am Soc Hypertens 2010;4:56–61. [Pubmed]
- O'Callaghan CJ, Goh MY and Rong P. Hypertension - the difficult decisions. Aust Fam Physician 2013;42:376–9. [Pubmed]
- Clark CE, Horvath IA, Taylor RS, et al. Doctors record higher blood pressures than nurses: systematic review and meta-analysis. Br J Gen Pract 2014;64:e223–32. [Pubmed]
- National Heart Foundation of Australia. Guideline for the diagnosis and management of hypertension in adults - 2016. Melbourne: National Heart Foundation of Australia. 2016 (accessed 5 July 2021).
- Handler J. The importance of accurate blood pressure measurement. Perm J 2009;13:51–4. [Pubmed]
- Therapeutic Guidelines Limited. Blood pressure reduction. eTG complete [Internet]. Melbourne: 2018, amended March 2021 (accessed 5 July 2021).
- Mancia G, Fagard R, Narkiewicz K, et al. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J 2013;34:2159–219. [Pubmed]
- Head GA, McGrath BP, Mihailidou AS, et al. Ambulatory blood pressure monitoring in Australia: 2011 consensus position statement. J Hypertens 2012;30:253–66. [Pubmed]
- Ohkubo T, Imai Y, Tsuji I, et al. Home blood pressure measurement has a stronger predictive power for mortality than does screening blood pressure measurement: a population-based observation in Ohasama, Japan. J Hypertens 1998;16:971–5. [Pubmed]
- National Vascular Disease Prevention Alliance. Guidelines for the management of absolute cardiovascular disease risk. 2012. [Online]
- National Heart Foundation and High Blood Pressure Research Council of Australia Ambulatory Blood Pressure Monitoring Consensus Committee. Ambulatory blood pressure monitoring. Aust Fam Physician 2011;40:877–80. [Pubmed]
- Sharman JE, Howes FS, Head GA et al. Home blood pressure monitoring: Australian Expert Consensus Statement. J Hyperten 2015; 33: 1721-8(2015): 1721-8.
